Category: Cardiology
Keywords: cocaine, cardiovascular, myocardial infarction (PubMed Search)
Posted: 5/1/2011 by Amal Mattu, MD
(Updated: 5/17/2026)
Click here to contact Amal Mattu, MD
Cocaine-associated MI occurs fairly early after acute cocaine use. 50% of MIs occur in patients prior to their arrival in the ED, and 24% of the total will occur within the first hour of cocaine use. If a patient has not ruled in by 12 hours post-arrival in the ED, it is extremely unlikely that the patient will rule in or suffer ACS-related complications from the cocaine....thus the concept behind using rapid rule out protocols in these patients.
The most important thing we as physicians can do for these patients is to strongly emphasize discontinuation of cocaine use and refer to rehab whenever possible. If the patient discontinues using cocaine, the prognosis for absence of subsequent cardiac events is excellent.
[thanks to Dr. Ellen Lemkin for her contribution to this pearl}
Schwartz BG. Cardiovascular effects of cocaine. Circulation 2011;122:2558-2569.
Category: Orthopedics
Keywords: Tendon Laceration (PubMed Search)
Posted: 4/30/2011 by Michael Bond, MD
Click here to contact Michael Bond, MD
Tendon Lacerations:
Hand lacerations need to be carefully explored in order to determine whether there is an associated tendon laceration. These can be be difficult to find unless a systematic approach is followed:
Future pearls will cover techniques on how to repair tendon lacerations. Stay tuned.
Category: Pediatrics
Posted: 4/22/2011 by Mimi Lu, MD
(Updated: 4/30/2011)
Click here to contact Mimi Lu, MD
You decided to intubate a child and wisely remembered that you should also follow with an NG/ OG after intubation to decompress the stomach. In order to avoid the blank stare when asked "what size"? Here's a nice mneumonic about Pediatric "tube" sizes... easy as 1-2-3-4!!! Please note ETT = endotracheal tube size.
So for example, a 4-year-old child would get intubated with a 5-0 ETT inserted to depth of 15 cm (3x ETT), a 10Fr NG/OG/foley (2x ETT), and a 20Fr chest tube (4x ETT).
Also, remember that you can use cuffed tubes in any child except neonates but the formula needs to be adjusted as follows: cuffed endotracheal tube ID (mm) = (age/4) + 3.5
Category: Toxicology
Keywords: glucose, dextrose, hypoglycemia (PubMed Search)
Posted: 4/28/2011 by Fermin Barrueto
(Updated: 5/17/2026)
Click here to contact Fermin Barrueto
Treating a patient with clinical hypoglycemia (neuroglycopenia if you want to sound cool) is with "1 amp of D50". Then some are starting D5 drips and D10 drips. Here is the actual breakdown of what you are giving:
1 amp of D50 = 50% dextrose = 50g/100mL = 25g x 4Kcal/g carbs = 100 calories bolus
1 L D5W at 100mL/hr = 5% Dextrose = 5g/100mL x 1L = 50g x (4Kcal/g) = 200 cal infusion of 20 cal/hr!
1 L D10W at 100mL/hr = 10%D= 10g/100mLx1L= 100g x (4Kcal/g)= 400 cal at infusion of 40 cal/hr!
Snickers Bar = 271 calories in one serving - most people will eat in 5 minutes = 54.2cal/min
Take home message is feed your patient once they are awake and alert. Much more effective.
Category: Neurology
Keywords: lumbar puncture, contraindications to lumbar puncture (PubMed Search)
Posted: 4/27/2011 by Aisha Liferidge, MD
(Updated: 5/17/2026)
Click here to contact Aisha Liferidge, MD
Contraindications to performing lumbar puncture (LP):
- INR > 1.4 or other coagulopathy
- Platelets < 50
- Infection at desired puncture site
- Obstructive / non-communicating hydrocephalus
- Intracranial mass
- High intracranial pressure (ICP) / papilledema (relative contraindication depending on etiology; especially a concern with intracranial mass lesion secondary to the increased risk of transtentorial or cerebellar herniation)
- Focal neurological symptoms/signs, decreased level of consciousness
- Partial / complete spinal block
- Acute spinal trauma
Category: Critical Care
Keywords: sepsis, shock, antimicrobials, combination, antibiotics (PubMed Search)
Posted: 4/26/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
A mortality benefit from combination antimicrobial therapy has not been clearly demonstrated in sepsis. However, when only the most severely-ill patients (i.e., septic shock) are considered in subgroup analysis, there appears to be a mortality benefit to using two antimicrobials against a suspected organism.
Combination antimicrobial therapy may reduce mortality through three mechanisms.
Always obtain appropriate cultures before initiating therapy. Although identification and susceptibility of the organism may take some time, eventually narrowing antimicrobial therapy to monotherapy in the ICU is still recommended.
Abad, C. Antimicrobial Therapy of Sepsis and Septic Shock: When are Two Drugs Better Than One? Crit Care Clinic 27 (2011) e1-e27.
Category: Visual Diagnosis
Posted: 4/25/2011 by Haney Mallemat, MD
(Updated: 5/17/2026)
Click here to contact Haney Mallemat, MD
Patient presents with the following X ray after yawning. Diagnosis?
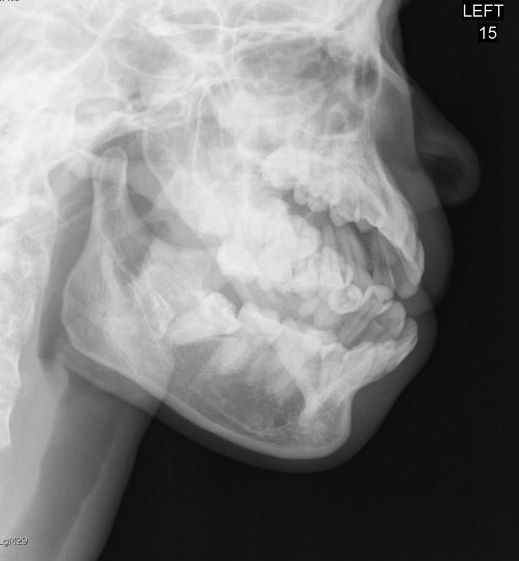
Diagnosis: Mandibular Dislocation
The link below demonstrates an interesting alternative to the traditional reduction method; prospective randomized trails are pending.
Thanks to Dr. George Kochman for the image and Dr. Christopher Doty (EM Program Director at SUNY Downstate / Kings County Hospital Center) for the video.
Category: Cardiology
Keywords: left bundle branch block, acute MI, electrocardiography (PubMed Search)
Posted: 4/24/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
Traditional teaching for many years has been that new or presumed new LBBB in patients with anginal type of symptoms should be treated as a STEMI, i.e. with immediate PCI or lytics. However, that teaching is based on poor evidence. Newer, increasing evidence is suggesting that new/presumed new LBBB in patients with anginal symptoms is actually not associated with acute MI any more often than when a patient has an old LBBB with those symptoms.
Probably the best management in patients with anginal type of symptoms and a new/presumed new LBBB is to contact the cardiologist on call and ask them for their preference in terms of treatment. Those patients are not necessarily definite AMIs.
1. Kontos MC, et al. Outcomes in patients with chronicity of left bundle-branch block with possible acute myocardial infarction. Am Heart J 2011;161:698-704.
2. Jain S, et al. Utility of left bundle branch block as a diagnostic criterion for acute myocardial infarction. Am J Cardiol 2011;107:1111-1116.
3. Chang AM, et al. Lack of association between left bundle-branch block and acute myocardial infarction in symptomatic ED patients. Am J Emerg Med 2009;27:916-921.
Category: Orthopedics
Keywords: Gout, pseudogout, NSAIDS, Steroids (PubMed Search)
Posted: 4/23/2011 by Brian Corwell, MD
(Updated: 5/17/2026)
Click here to contact Brian Corwell, MD
Gout treatment considerations
Treatment is directed to relieve pain and inflammation
NSAIDs, steroids and narcotics are the mainstays of treatment. All 3 should be used in combination.
Aspirin should be avoided as it may increase uric acid levels
Note: not in prevention doses (81mg) in treatment doses (325-650mg q4h)
NSAIDs and steroids take time to be effective. Provide appropriate analgesia with oral narcotic medication for short term relief
Don't forget the benefit of splinting a "hot" joint (the ankle or wrist for example)
NSAIDs: Use may be limited in the elderly and in those on coumadin or with peptic ulcer disease. 5-7 days of treatment is usually sufficient. Indomethacin is most commonly used (50 mg TID, which may be tapered to 25 mg TID after 3 days)
Steroids: Likely more effective than NSAIDs. Oral prednisolone is more effective than naproxen (1). Use prednisone 30-50 mg for 3-5 days without tapering (as we use for asthma). May be useful to supplement with NSAIDs on the tail end to prevent a rebound flare. If tapping the joint consider intraarticular steroids. If there is concern for medical noncompliance with oral steroids consider IM steroids (triamcinolone 60mg or methylprednisolone).
1) Janssens, The Lancet, 2008 May;371(1):1854-60.
2) Alloway, J Rheumatol. 1993 Jan;20(1):111-3.
Category: Toxicology
Keywords: ethanol, withdrawal (PubMed Search)
Posted: 4/21/2011 by Fermin Barrueto
(Updated: 5/17/2026)
Click here to contact Fermin Barrueto
The ability to determine whether or not a patient is an alcoholic or will go into alcohol withdrawal syndrome (AWS) is not amenable to a clinical decision rule though many attempts have been made. The strongest predictor that a patient can develop AWS is a positive family history of AWS. Some clinical and biochemical predictors are:
ALT >50 U/L
K <3.6
These two in one study have had an odds ratio of 9.0 and 5.7 respectively though specificity was quite low. Ethanol levels has also found to be contradictory. Being able to predict AWS does not currently seem plausible but the treatment of AWS should and can involve a clinical decision rule like CIWA-Ar which is a scoring system that takes into account N/V, tremor, sweats, anxiety, agitation, hallucinations, headache and sensorium. Take a look at the scoring system that is most validated and utilized for symptom triggered therapy - often considered the most effective treatment for alcohol withdrawal.
Rogers et al. Effect of disulfiram on adrenaergic function. Clin Pharmacol Ther 1979.
Category: Neurology
Keywords: opening pressure, lumbar puncture (PubMed Search)
Posted: 4/20/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Keywords: staphylococcal aureus, aminoglycoside, monotherapy, combination therapy (PubMed Search)
Posted: 4/19/2011 by Mike Winters, MBA, MD
(Updated: 5/17/2026)
Click here to contact Mike Winters, MBA, MD
Combination Antimicrobial Therapy for Gram (+) Bacteremia
Abad CL, Kumar A, Safdar N. Antimicrobial therapy of sepsis and septic shock - When are two drugs better than one? Crit Care Clin 2011;27:e1-e27.
Category: Cardiology
Keywords: dabigatran, anticoagulant, thrombin inhibitor (PubMed Search)
Posted: 4/17/2011 by Amal Mattu, MD
(Updated: 5/17/2026)
Click here to contact Amal Mattu, MD
Dabigatran is a new oral anticoagulant (direct thrombin inhibitor) which is being marketed as the new drug to replace warfarin in many cardiac patients. You'll hear much more about it in the coming year, but for now you should know the main advantage and disadvantage:
1. advantage: no need to check levels, e.g. INRs
2. disadvantage: no reversal agent; if a patient is actively bleeding, all you can do is to hold further doses and provide supportive therapy, e.g. tranfusions; hemodialysis is another option, but not ideal to place new dialysis catheters emergently in patients that are coagulopathic!
This second point, the disadvantage of having no reversal agent, is potentially a big issue, especially in older patients at risk for falls. Stay tuned for more information...
Category: Orthopedics
Keywords: Gout (PubMed Search)
Posted: 4/10/2011 by Brian Corwell, MD
(Updated: 4/16/2011)
Click here to contact Brian Corwell, MD
Gout Part 2
Man CY, Cheung IT, Cameron PA, Rainer TH. Comparison of oral prednisolone/paracetamol and oral indomethacin/paracetamol combination therapy in the treatment of acute gout like arthritis: a double-blind, randomized, controlled trial. Ann Emerg Med. 2007;49:670-677.
Category: Toxicology
Keywords: latex, allergy, kiwi, cross-reactivity (PubMed Search)
Posted: 4/13/2011 by Bryan Hayes, PharmD
(Updated: 4/14/2011)
Click here to contact Bryan Hayes, PharmD
Kiwi fruit and latex share several antigens in common. Thus, individuals who are allergic to either kiwi or latex may also suffer hypersensitivity reactions to the other material.
Murali MR, et al. Case 9-2011: A 37-year old man with flushing and hypotension. N Engl J Med 2011;364(12):1155-65.
Category: Neurology
Keywords: meningitis, prophylaxis, meningococcemia (PubMed Search)
Posted: 4/13/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Keywords: Vancomycin, Daptomycin, Linezolid, MRSA, gram positive, infections, sepsis, pneumonia (PubMed Search)
Posted: 4/12/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Vancomycin is often started empirically for gram-positive and MRSA coverage. Although effective and generally well-tolerated, emerging resistance and side-effect profiles limit its use in some patients. Two alternatives are Linezolid and Daptomycin.
Linezolid
Daptomycin
Alder, J. The Use of Daptomycin for Staphylococcus Aureus Infection in the Critical Care Medicine. Crit Care Clin 24(2008); 349-363.
Category: Visual Diagnosis
Posted: 4/10/2011 by Haney Mallemat, MD
(Updated: 4/11/2011)
Click here to contact Haney Mallemat, MD
60 y/o male transferred from local rehab facility c/o abdominal pain.
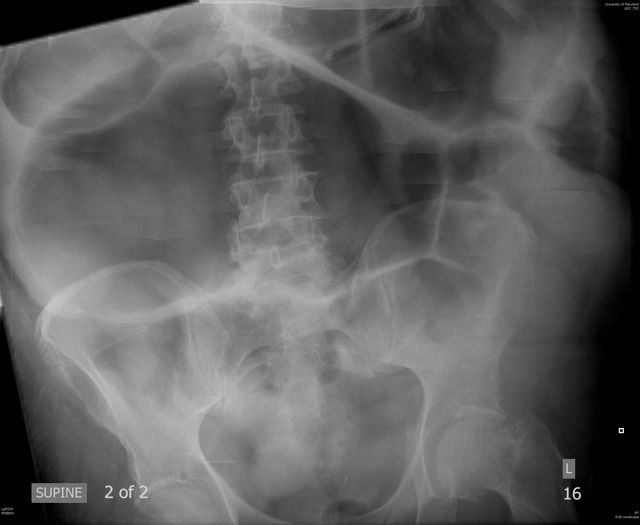
Ogilvie's syndrome / Acute colonic pseudo-obstruction (ACPO)
Syndrome of decreased GI motility believed to be an autonomic imbalance (specifically, parasympathetic suppression) predominantly in the cecum and right colon. ACPO is also commonly due to narcotic overuse / abuse.
Differential diagnosis:
Abdominal XR:
Treatment:
Fazel A, Verne GN. New solutions to an old problem: Acute colonic pseudo-obstruction. JClin Gastroenterol 2005; Vol 39(1): 17-20.
Ozkurt H, Yilmaz F, et al. Acute colonic pseudo-obstruction (Ogilvie's syndrome): radiologic diagnosis and medical treatment with neostigmine. Report of 4 cases. Am J of Emer Med 2009; Vol 27: 757.e1 - 757e4.
Category: Geriatrics
Keywords: geriatrics, polypharmacy, elderly (PubMed Search)
Posted: 4/10/2011 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
We already know that polypharmacy is a big issue in the elderly, but here are a few key points to keep in mind:
1. Adverse drug effects are responsible for 11% of ED visits in the elderly.
2. Almost 50% of all adverse drug effects in the elderly are accounted for by only 3 drug classes:
a. oral anticoagulant or antiplatelet agents
b. antidiabetic agents
c. agents with narrow therapeutic index (e.g. digoxin and phenytoin)
3. 1/3 of all adverse-effect-induced ED visits are accounted for by warfarin, insulin, and digoxin.
4. Up to 20% of new prescriptions given to elderly ED patients represents a potential drug interaction.
The bottom line here is very simple--scrutinize that medication list and any new prescriptions in the elderly patient!
Samaras N, Chevalley T, Samaras D, et al. Older patients in the emergency department: a review. Ann Emerg Med 2010;56:261-269.
Category: Orthopedics
Keywords: Knee Dislocation, Prosthetic (PubMed Search)
Posted: 4/9/2011 by Michael Bond, MD
(Updated: 5/17/2026)
Click here to contact Michael Bond, MD
Knee dislocations are uncommon, and prosthetic knee dislocations even rarer. Some general facts about prosthetic knee dislocations are:
Wang CJ, Wang HE. Dislocation of total knee arthroplasty: a report of 6 cases with 2 patterns of instability. Acta Orthop Scand 1997;68:282-285.
Stiehl JB, Komistek RD, Dennis DA, et al. Fluoroscopic analysis of kinematics after posterior-cruciate-retaining knee arthroplasty. J Bone Joint Surg Br 1995;77:884-889.
