Category: EMS
Keywords: HEMS, pediatric trauma (PubMed Search)
Posted: 5/15/2026 by Jenny Guyther, MD
(Updated: 5/21/2026)
Click here to contact Jenny Guyther, MD
Previous pediatric studies have shown that 1) air transport has shown improved outcomes compared to matched ground transports but 2) air transport may be overutilized.
This was a multicenter retrospective study using the Pediatric Emergency Care Applied Research Network Registry from 2012-2021 looking at pediatric patients transported to the ED by helicopter. This registry does not differentiate between field transports and interfacility transfers. The study looked to identify patients who were discharged from the ED or had a hospital stay < 48 hours. 7722 patients were included with a median age of 5.9 years. 20% of these patients were discharged from the ED. Among those admitted, over half were discharged within 48 hours. Patients who were discharged from the ED were found to have triage < ESI 1, missing a systolic blood pressure or temperature. Tachycardia, tachypnea, hypertension and abnormal temperature were associated with a lower rate of ED discharge.
Bottom line: Additional research is needed to identify patients who may be more appropriate for ground transport or when transport is not needed (or could be replaced with telemedicine).
Naik V, Bhardwaj P, Ramgopal S. Rapid Discharge Following Air Transport in Children. Prehosp Emerg Care. 2025 Jul 23:1-8. doi: 10.1080/10903127.2025.2531074. Epub ahead of print. PMID: 40643375.
Category: Critical Care
Keywords: Pulmonary embolism, massive PE, submassive PE, RV failure, cardiogenic shock, guidelines (PubMed Search)
Posted: 5/19/2026 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
Not all patients with an acute PE will be crashing and critically ill, but it seemed worthwhile to remind everyone that there are new guidelines and recommendations from AHA/ACC/ACCP/ACEP/CHEST/SCAI/SHM/SIR/SVM/SVN/XYZLMNOP about the management of patients with acute pulmonary embolism in the 2026 AHA/ACC Joint Committee statement. A few key takeaways, with highlights for the sicker PE patients:
Highlights for the sicker PE patients, i.e. Categories C+:
For a great breakdown and further discussion of the new guidelines, I recommend checking out the Life in the Fast Lane blogpost here.


Creager MA et al. 2026 AHA/ACC/ACCP/ACEP/CHEST/SCAI/SHM/SIR/SVM/SVN Guideline for the Evaluation and Management of Acute Pulmonary Embolism in Adults: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2026 Mar 24;153(12):e977-e1051.
Category: Administration
Posted: 5/13/2026 by Kevin Semelrath, MD
(Updated: 5/17/2026)
Click here to contact Kevin Semelrath, MD
This is a small qualitative study that focused on barriers to care and how to overcome them when dealing with patients with dementia, who are primarily Spanish speaking. The authors found to big themes that patients and caretakers thought would improve their care:
1- use of a certified translator, either telephonically or in person, eased social dynamics in communication
2- those same translators tended to only be used in an episodic manner- during HPI, exlaining results or discharge planning. But the patients and caretakers would prefer to have access to them in the “in between” periods so that it would be a more patient centered experience
A. N.Chary, V.Lara, S.Yoon, et al., “Communicating Across Languages: Experiences of Spanish-Speaking People With Dementia and Care Partners in the Emergency Department,” Academic Emergency Medicine33, no. 3 (2026): e70198, https://doi.org/10.1111/acem.70198.
Category: Trauma
Keywords: Removal, motorcycle helmet (PubMed Search)
Posted: 5/17/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
Here are two techniques to remove a helmet from an injured motorcyclist. The first uses a cast saw to bivalve the helmet. A link for a video is also provided.
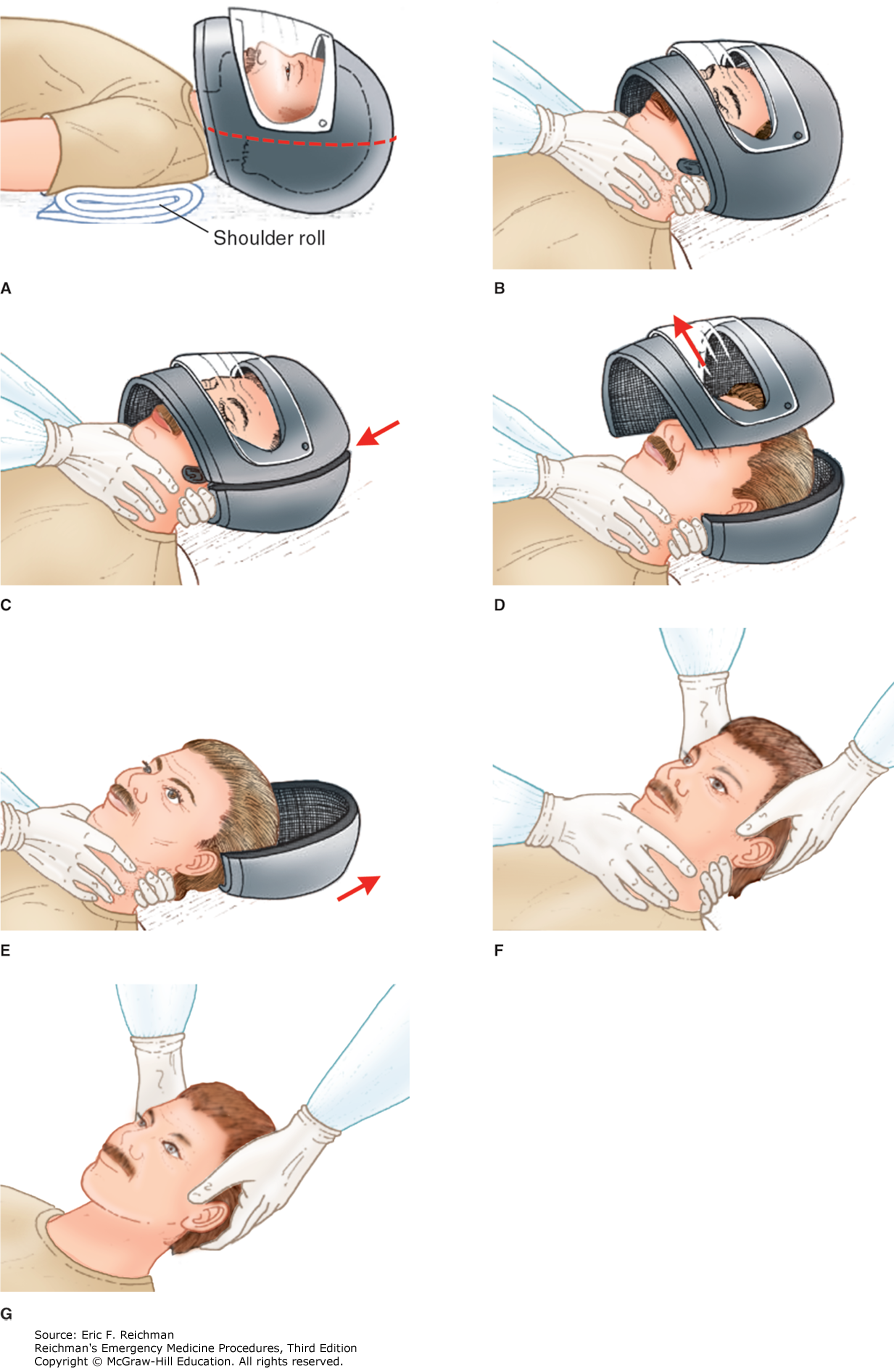
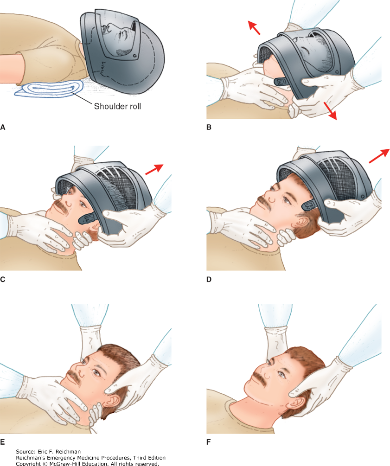
Category: Pediatrics
Keywords: CPR, ILCOR, PALS, VF, defibrillation (PubMed Search)
Posted: 5/15/2026 by Jenny Guyther, MD
(Updated: 5/22/2026)
Click here to contact Jenny Guyther, MD
US and International guidelines differ on the initial defibrillation dose in pediatric patients. International, European, Australian and New Zealand guidelines had recommend an initial dose of 4 J/kg for the initial and all subsequent doses while the American Heart Association recommends an initial dose of 2-4J/kg (with 2 J/kg in the teaching algorithms) with subsequent shocks being at least at 4J/kg and no greater than 10 J/kg. More recently, ILCOR suggested an initial dose of 2-4 J/kg.
This was a systemic review of 7 observational studies, mostly involving in hospital pediatric cardiac arrests. Outcomes of termination of VF/pVT, ROSC and survival to hospital discharged were examined in relation to the initial J/kg dose that was used compared to initial doses of 2 J/kg. Outcomes were neither better or worse with doses < 1.5 J/kg or > 2.5 J/kg. Additional research is needed as this certainty of this evidence was considered “very low.”
Acworth J, Del Castillo J, Tiwari LK, Atkins D, de Caen A, Bansal A, Couto TB, Katzenschlager S, Kleinman M, Lopez-Herce J, Morgan RW, Myburgh M, Nadkarni V, Tijssen JA, Scholefield BR; International Liaison Committee on Resuscitation Paediatric Life Support Task Force. Energy doses for paediatric defibrillation in cardiac arrest: systematic review and meta-analysis. Resusc Plus. 2025 May 26;24:100991. doi: 10.1016/j.resplu.2025.100991. PMID: 40524976; PMCID: PMC12169708.
Category: Obstetrics & Gynecology
Keywords: contraception, reproductive care (PubMed Search)
Posted: 5/14/2026 by Ashley Martinelli
(Updated: 5/15/2026)
Click here to contact Ashley Martinelli
Access to reproductive care is being limited across the country, and the rate of undesired pregnancies is rising.
Discussing contraception preferences in the Emergency Department can support patients as well as and reduce the morbidity and mortality associated with an undesired pregnancy. Simply asking patients of childbearing age: "Are you interested in discussing pregnancy prevention?" can bridge a gap in access to reliable care. Easy and accessible tools can be used on shift to assist with appropriate initiation.
On Shift Tools:
Contraception Initiation • Clinical Resources • FemInEM
www.bedsider.org -Patient friendly comparisons of contraception options
Quick Start Contraception Care in the ED - Bridge to Treatment - ED oriented flow diagram
Cline L, Downey K, Rashid Y, et al. When Prevention is an Emergency: The Imperative of Contraception Initiation in the Emergency Department. J Emerg Med 2026; 85:177-182.
https://doi.org/10.1016/j.jemermed.2026.02.038.
(https://www.sciencedirect.com/science/article/pii/S0736467926000697)
Category: Gastrointestional
Keywords: Lower GI Bleeding (PubMed Search)
Posted: 5/13/2026 by Neeraja Murali, DO, MPH
Click here to contact Neeraja Murali, DO, MPH
Lower GI bleed is a common reason for ED visits. This study aimed to validate a scoring system to identify low-risk LGIB pts who could be safely discharged from the ED.
The SHA2PE score incorporates characteristics and data that are commonly collected on patients with this complaint; readers can click through to see the scoring system. A score of less than or equal to 1 helps identify patients suitable for outpatient management, with a NPV of 98.3% (95% CI [97.2-99.1]) for predicting the need for hospitalization and acute intervention. However, the findings should be interpreted with caution given the relatively low prevalence of interventions within the study population.
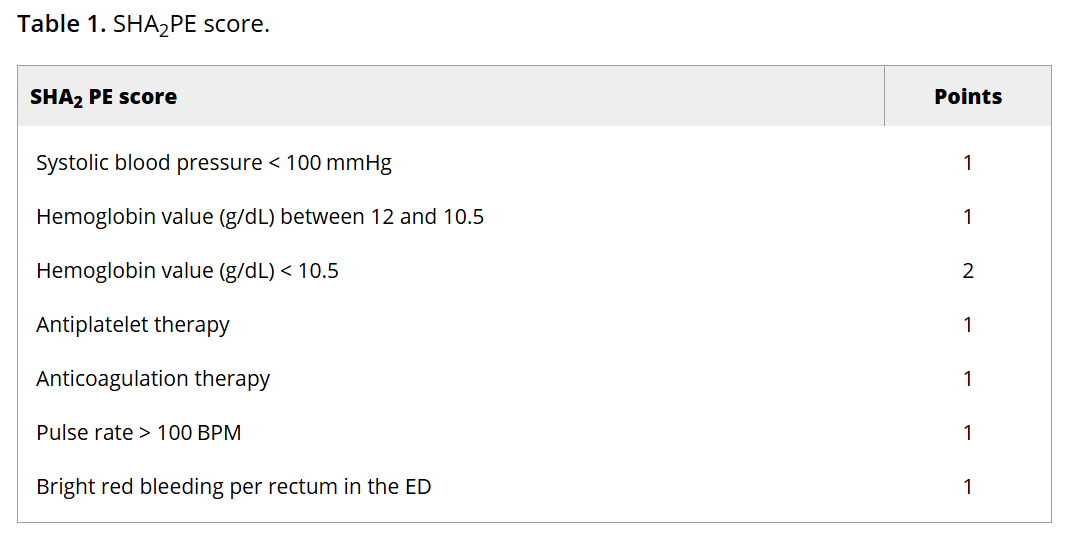
Ahmad AI, El Sabagh A, Zhang J, et al. External Validation of SHA2PE Score: A Score to Predict Low-Risk Lower Gastrointestinal Bleeding in the Emergency Department. Gastroenterol Res Pract. 2025;2025:5657404. Published 2025 Jan 3. doi:10.1155/grp/5657404
Category: Critical Care
Keywords: ventilator associated pneumonia, intubation, stroke, brain injury, antibiotics (PubMed Search)
Posted: 5/12/2026 by Jessica Downing, MD
Click here to contact Jessica Downing, MD
Should we give a dose of antibiotics after intubating to reduce risk of VAP down the line? A multicenter RCT conducted in 2024 - the PROPHY-VAP Trial - found that a single dose of 2g ceftriaxone administered within 12 hours of intubation reduced VAP within the first week of hospitalization for patients intubated for airway protection due to TBI, stroke or SAH, with a VAP rate of 14% in the CTX group vs 32% in the VAP group (HR 0.60; 95% CI 0.38-0.95).
Click the link below for details and additional discussion
Details:
Background: prior studies have investigated different antibiotic regimens in different groups. In 2023, the AMIKIHAL trial suggested that a 3d course of inhaled amikacin would reduce 28d risk of VAP among patients ventilated for >3d (not just neuro patients). In 2022, the SuDDICU trial suggested that “selective decontamination of the digestive tract” with a combination of IV abx, oral suspension of antibiotics, and topical abx to the oropharynx and buccal mucosa suggested a lower risk of in-hospital mortality in Baysian meta-analysis (though not in the primary study statistics). In 2005, the ANTHARTIC trial suggested a lower rate of VAP with a 2 days course of amoxicillin-clavulanate among patients admitted after OHCA.
Closing Thoughts: Together, these studies suggest that there may be a role for an early and short course of antibiotics for preventing VAP in a few patient populations. A single dose of CTX is easier and more benign than prior suggested regimens, and based on the available data, seems to offer benefit with minimal risk.
Dahyot-Fizelier C, Lasocki S, Kerforne T et al. Ceftriaxone to prevent early ventilator-associated pneumonia in patients with acute brain injury: a multicentre, randomised, double-blind, placebo-controlled, assessor-masked superiority trial. The Lancet Respiratory Medicine, 2024; 12, 375-385
Additional References
Category: Trauma
Keywords: Dementia trauma independent living (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/10/2026)
Click here to contact Robert Flint, MD
In 290 trauma patients diagnosed with dementia prior to injury, when compared to 3000 patients over age 65 without dementia and similar injury severity score, the dementia patients had a much higher rate of discharge to an institution instead of back to home living. This was particularly true of older women.
Cohen JE, Montoya MA, Thompson A, Sanchez SE, Hwabejire J, Anderson GA, Salim A, Herrera-Escobar JP. Functional Decline and Loss of Independence After Traumatic Injury in Older Adults With Dementia. J Am Geriatr Soc. 2026 Feb;74(2):438-446. doi: 10.1111/jgs.70242. Epub 2025 Dec 14. PMID: 41392016
Category: Orthopedics
Posted: 5/9/2026 by Brian Corwell, MD
(Updated: 5/22/2026)
Click here to contact Brian Corwell, MD
How much do you trust your plain film in the evaluation of elderly patients with traumatic hip pain?
A 2020 meta-analysis involving 3000 elderly patients investigated radiographically occult hip fractures.
The rate of surgical hip fracture was reported in each study.
MRI was used as the reference standard.
Mean age, 76.8 years ± 6.0.
The frequency of radiographically occult surgical hip fracture was 39% (1110 of 2835 patients)
The frequency of occult fracture was higher in 3 groups of patients:
Aged at least 80 years
Those with an equivocal radiographic report
Those with a history of trauma
Haj-Mirzaian A,et al. Use of Advanced Imaging for Radiographically Occult Hip Fracture in Elderly Patients: A Systematic Review and Meta-Analysis. Radiology. 2020 Sep;296(3):521-531.
Category: Pediatrics
Keywords: pediatrics, hypocalcemia, calcium, seizures, electrolytes (PubMed Search)
Posted: 5/8/2026 by Kathleen Stephanos, MD
(Updated: 5/22/2026)
Click here to contact Kathleen Stephanos, MD
BOTTOM LINE: It is critical to recognize and treat symptomatic hypocalcemia in pediatric patients.
Pediatric hypocalcemia has a variety of causes that should be considered. In the neonate congenital causes should be on the differential.
Parathyroid hormone levels should be checked on all patients along with magnesium levels and ionized calcium.
An ECG should also be obtained for prolonged QTc.
Management is guided by acute symptoms (tetany, seizures, cramping, etc.) or other signs of critical illness (sepsis, trauma, etc.) in conjunction with low ionized calcium levels.
For symptomatic patients give 20 mg/kg of elemental calcium IV over a 10–20 min period
For asymptomatic patient oral calcium supplements are typically given.
Failure to recognize concomitant hypomagnesemia may result in hypocalcemia that is resistant to treatment.
Disposition: Those children receiving IV calcium should be admitted with every 4-to-6-hour calcium levels and typically require ICU level admission. Children being monitored with oral supplementation can often be observed on a pediatric floor presuming there are no ECG abnormalities.
Zieg J, Ghose S, Raina R. Electrolyte disorders related emergencies in children. BMC Nephrol. 2024 Aug 30;25(1):282. doi: 10.1186/s12882-024-03725-5. PMID: 39215244; PMCID: PMC11363364.
Category: Geriatrics
Keywords: Readmission, dementia, paramedic, home health (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/7/2026)
Click here to contact Robert Flint, MD
This article describes a paramedic run community health initiative to assist people with dementia transition to home after an ED visit. They describe:
“Persons living with dementia (PLWD) frequently use the emergency department (ED) for unscheduled care and experience significant challenges during the ED-to-home transition.
The Community Paramedic-led Transitions Intervention (CPTI) is a structured, coaching-based program delivered by community paramedics that includes a home visit and follow-up calls to support PLWD and care partners during the 30?days after ED discharge.”
Could your ED use a program like this to prevent readmissions?
M. J.Morales, S.Ricketts, C. R.Grudzen, et al., “Bridging the Gap Between the ED and Home: The Community Paramedic-Led Transitions Intervention for Persons Living With Dementia,” Journal of the American Geriatrics Society (2026): 1–10, https://doi.org/10.1111/jgs.70403.
Category: Toxicology
Keywords: Salicylate toxicity, cerebral glucopenia, sodium bicarbonate, hemodialysis (PubMed Search)
Posted: 5/6/2026 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
Bottom Line: Multiple modalities of intervention may be needed to combat various aspects of salicylate toxicity. These include gastric decontamination, fluid hydration, dextrose admiinistration, aggressive serum alkalinization, establishment of normokalemia and hemodialysis. Intubation and chemical restraint should be avoided if possible.
Gastric decontamination: is recommended in those with acute toxicity if there are no contraindications (e.g., inability to protect the airway or refractory vomiting) as salicylate GI pill concretions can occur. Activated charcoal, 1 g/kg orally up to 100 g, is recommended. Salicylates can form gastric bezoars and cause delayed peak levels and toxicity.
Fluid resuscitation: should be addressed early in treatment course as patients can be volume depleted from multiple sources of fluid loss as much as 2-4 liters which worsens toxicity. D5W with 3 amps of sodium bicarbonate is the preferred fluid to treat volume depletion, hypoglycemia, and acidosis.
Dextrose: Hyperglycemia may present early due to increased cortisol levels, but hypoglycemia can follow and is common as oxidative phosphorylation is impaired and even with normal serum glucose levels cerebral glucopenia. A trial of IV dextrose bolus (0.5-1 g/kg) and/or infusion is recommended with mild encephalopathy
Aggressive serum alkalinization: is integral to management. This typically includes a bolus of 1-2 mEq/kg of hypertonic sodium bicarbonate followed by an infusion of isotonic sodium bicarbonate (150 mEq added to 1 L of 5% dextrose in water). Serum pH adjustment to a goal of 7.50-7.55 will decrease the volume of distribution of salicylate: salicylate will shift out of the tissues and into the serum. Urinary alkalinization aimed to achieve a urine pH >7.5 is a secondary goal. Frequent serial salicylate levels and blood gas determinations (2-4 hours) are necessary and should be correlated with clinical manifestations.
Normokalemia: is important as urinary alkalinization cannot be achieved if hypokalemia is present. Initial supplementation of potassium (40-60 mEq), addition of potassium (40-60 mEq) to the bicarbonate infusion, and additional administrations in response to therapy and level monitoring is recommended.
Hemodialysis: is necessary and lifesaving in cases with severely high serum salicylate concentrations, refractory acidemia or severe electrolyte disturbance, cerebral edema, altered mental status, renal failure, hypoxia from pulmonary edema, standard therapies not producing an adequate response, and specific serum concentrations. Early consultation with nephrology can expedite treatment.
Intubation or any chemical restraint should be avoided: as sedation and paralysis may result in further decrease in pH, due to hypercarbia from hypoventilation. This results in shifting salicylate to it’s uncharged state which can easily pass into tissues, further worsening toxicity and CNS and myocardial dysfunction. Non-invasive ventilation, such as a high-flow nasal cannula, may reduce the work of breathing. If intubation is necessary hyperventilation to reduce CO2 and bolus of intravenous bicarbonate
Salicylate Toxicity. Palmer B, Clegg D. New Egland Journal of Medicine. 2020;382(26). 2544-2555. DOI: 10.1056/NEJMra2010852
Hospitalizations for acute salicylate intoxication in the United States. Thongprayoon C, Petnak T, Kaewput W, et al. J Clin Med. 2020;9:2638. doi: 10.3390/jcm9082638.
Acute Salicylate Toxicity: A Narrative Review for Emergency Clinicians. Sidlak AM, Spadaro A, et.al, Cureus. 2025 Sep 2;17(9): e91505. doi: 10.7759/cureus.91505
Category: Trauma
Keywords: Rib fractures, geriatric, pain control (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
A retrospective study looking at use of transdermal Buprenorphine in older trauma patients with rib fractures found a good safety profile (less naloxone use) and less overall opioid use however no change in overall length of stay or mortality. Adding this to your multimodal pain strategy in older patients with rib fractures seems like a reasonable plan.
ournal of the American Geriatrics SocietyEarly View
CLINICAL INVESTIGATION
Iva Neupane, Brian Mikolasko, Charles A. Adams Jr, Joao Filipe Goncalves Monteiro, Nadia Mujahid, Linda Girouard, Jessica Arabi, Ashna Rajan, Audrea Bose, Stephanie Lueckel, Lynn McNicoll, Stefan Gravenstein
First published: 16 April 2026
Category: Geriatrics
Keywords: Constipation geriatric complex (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
A narrative review of literature involving older patients and constipation found:
“Major contributing factors include physical inactivity, sarcopenia, dehydration, inappropriate defecation posture, and polypharmacy, particularly opioids and anticholinergic agents. Importantly, these factors interact through the brain–gut–microbiota axis, contributing not only to gastrointestinal dysfunction but also to systemic outcomes such as frailty, cognitive decline, and increased healthcare burden, thereby supporting a multidimensional disease framework.”
It isn’t as simple as adding a laxative.
Mimura S, Morishita A, Kitaoka A, Sasaki K, Tai H, Yano R, Nakahara M, Oura K, Tadokoro T, Fujita K, et al. Constipation in Older Adults: Pathophysiology, Clinical Impact, and Management Strategies. Geriatrics. 2026; 11(2):47. https://doi.org/10.3390/geriatrics11020047
Category: Geriatrics
Keywords: Prescribing cascade (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 4/30/2026)
Click here to contact Robert Flint, MD
The article outlines how instead of looking at medications as the cause of symptoms, we often add more medications to treat the medication induced symptoms. Here is an example of how we get to polypharmacy in older patients
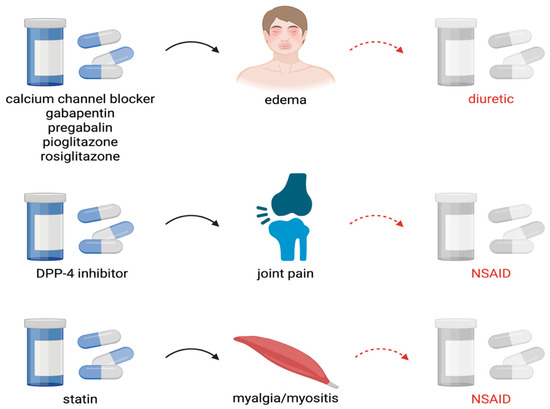
Bry?a A, Woro? J, Miedziaszczyk M, Lorkowska-Zawicka B, Bujak-Gi?ycka B, Orzechowski D, Po?etek P, Pa?ys W. Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity. Geriatrics. 2026; 11(2):37. https://doi.org/10.3390/geriatrics11020037
Category: Trauma
Keywords: Body armor, blunt injury, BABT (PubMed Search)
Posted: 4/26/2026 by Robert Flint, MD
(Updated: 5/22/2026)
Click here to contact Robert Flint, MD
Body armor/ bullet resistant vests used by law enforcement are designed to stop penetration by handgun rounds. These rounds have less velocity than rifle rounds. When caring for someone who has been shot while wearing body armor, verify no penetration has occurred and then look for blunt injuries such as rib fractures, liver injuries, pneumothorax, cardiac contusion, vertebral injury, etc. Behind Armor Blunt Trauma (BABT) is the technical term for injuries caused by the transfer of kinetic energy that occurs when these vests are struck.
Volume 49, Issue 7, July 2018, Pages 1251-1257
Author links open overlay panelRosalind M. Jennings a, Chris Malbon b, Fiona Brock a, Stuart Harrisson c, Debra J. Carr b
Category: Trauma
Keywords: trauma, chronic pain, (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/23/2026)
Click here to contact Robert Flint, MD
This narrative review of the trauma literature looking at chronic pain after trauma found:
Kussé M, Hans G, Saldien V, Wildemeersch D. Chronic pain following major trauma: Prevalence, predictive models, and risk factors across common injury types. Trauma. 2026;0(0). doi:10.1177/14604086251404750
Category: Administration
Posted: 4/21/2026 by Steve Schenkel, MD, MPP
(Updated: 4/22/2026)
Click here to contact Steve Schenkel, MD, MPP
Ambient Artificial Intelligence based scribes that create visit notes based on the conversation in the room during patient evaluation may save documentation time and reduce total time in the health record but may not perform as well as human scribes in some circumstances, at least for pediatric patient charts.
Two side-by-side reports in the May Annals of Emergency Medicine portray related but slightly different pictures of ambient scribing.
Preiksaitis et al found that the offer of an ambient AI scribing system led to some adoption more for lower acuity visits. AI use led to shorter notes, shorter electronic health record time, and about one minute less documentation time per chart. Morey et al compared human and AI scribes and found that human scribes were associated with similar note lengths and metrics for adult patients and somewhat higher quality charts in pediatric patients. An associated editorial argues that AI charting may offer a moment of culture change. (I am one of the authors of the editorial.)
Preiksaitis C, Alvarez A, Winkel M, et al. Ambient Artificial Intelligence Scribe Adoption and Documentation Time in the Emergency Department. Annals of Emergency Medicine, 2026; 87, 569-574.
Morey J, Jones D, Walker L, et al. Ambient Artificial Intelligence Versus Human Scribes in the Emergency Department. Annals of Emergency Medicine, 2025; 87, 561-568.
Schriger D, Schenkel S. Can Ambient Charting Fix Emergency Medicine? Annals of Emergency Medicine, 2026; 87, 575-577.
Category: Critical Care
Keywords: Oxygenation, ARDS, P:F Ratio, S:F Ratio, Hypoxia, Mechanical Ventilation (PubMed Search)
Posted: 4/21/2026 by Mark Sutherland, MD
(Updated: 5/22/2026)
Click here to contact Mark Sutherland, MD
PaO2 to FiO2 (P:F) ratios, are often considered the gold standard in critical care for assessing the degree of oxygen-refractory hypoxia in various pathologies, particularly ARDS. P:F does have some limitations, including not accounting for the PEEP, but probably the most limiting is that it requires collecting an ABG, which is invasive and not always feasible or a top priority when resuscitating a critically ill hypoxic patient. On the other hand, SpO2 (pulse ox saturation) is routinely available, and of course the FiO2 should be known, so many have suggested perhaps using an SpO2 to FiO2 (S:F) ratio instead. But how S:F maps to P:F and how well they correlate is not fully known. Chaudhuri et al recently conducted a meta-analysis, published in Critical Care Medicine this month, which reviewed the literature on this.
Bottom Line: Yes, S:F ratios correlate well with P:F ratios, especially when the SpO2 is less than 97%, but you can't just substitute the S:F for P:F, you have to use one of the accepted formulas. See additional info on the website for the actual formula to apply and how a given S:F translates to P:F.
The authors identified 4 particularly high performing formulas from well-done studies. One was logarithmic, and two were non-linear, making the math hard, so the best is probably the linear one (correlation coefficient was 0.89, which is quite good). It is:
SF = 64 + 0.84 x PF
Usually you have the SF and want to figure out the PF, so rearranging to solve for PF (to save you all the trouble):
PF = (SF - 64) / 0.84
Since we usually care about P:F < 300 (mild ARDS), < 200 (moderate ARDS), and < 100 (severe ARDS), here are the S:F mappings for those P:Fs to make things super simple:
If P:F is 300 then S:F is 315
If P:F is 200 then S:F is 235
If P:F is 100 then S:F is148
And 150 is another P:F that is important since we often consider proning and/or paralysis under this level. That would equate to an S:F of 190 using this formula.
Don't forget! The SpO2 is expressed as a percentage, and FiO2 as a decimal. So for example, for a patient with a sat of 97% on RA (21% FiO2):
97 / 0.21 = 461 would be their S:F.
Chaudhuri D, Lazarte J, Shah K, Pitre T, Pekkarinen PT, Sendagire C, Martin GS, Jung C, Laffey JG, Rochwerg B; Sequential Organ Failure Assessment (SOFA)-2 study group. Approaches to Converting Sp o2 /F io2 Ratio to Pa o2 /F io2 Ratio for Assessment of Respiratory Failure in Critically Ill Patients: A Systematic Review. Crit Care Med. 2026 Apr 1;54(4):950-959. doi: 10.1097/CCM.0000000000007018. Epub 2026 Jan 2. PMID: 41493393.
