Category: Trauma
Keywords: Dementia trauma independent living (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/10/2026)
Click here to contact Robert Flint, MD
In 290 trauma patients diagnosed with dementia prior to injury, when compared to 3000 patients over age 65 without dementia and similar injury severity score, the dementia patients had a much higher rate of discharge to an institution instead of back to home living. This was particularly true of older women.
Cohen JE, Montoya MA, Thompson A, Sanchez SE, Hwabejire J, Anderson GA, Salim A, Herrera-Escobar JP. Functional Decline and Loss of Independence After Traumatic Injury in Older Adults With Dementia. J Am Geriatr Soc. 2026 Feb;74(2):438-446. doi: 10.1111/jgs.70242. Epub 2025 Dec 14. PMID: 41392016
Category: Geriatrics
Keywords: Readmission, dementia, paramedic, home health (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/7/2026)
Click here to contact Robert Flint, MD
This article describes a paramedic run community health initiative to assist people with dementia transition to home after an ED visit. They describe:
“Persons living with dementia (PLWD) frequently use the emergency department (ED) for unscheduled care and experience significant challenges during the ED-to-home transition.
The Community Paramedic-led Transitions Intervention (CPTI) is a structured, coaching-based program delivered by community paramedics that includes a home visit and follow-up calls to support PLWD and care partners during the 30?days after ED discharge.”
Could your ED use a program like this to prevent readmissions?
M. J.Morales, S.Ricketts, C. R.Grudzen, et al., “Bridging the Gap Between the ED and Home: The Community Paramedic-Led Transitions Intervention for Persons Living With Dementia,” Journal of the American Geriatrics Society (2026): 1–10, https://doi.org/10.1111/jgs.70403.
Category: Trauma
Keywords: Rib fractures, geriatric, pain control (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/3/2026)
Click here to contact Robert Flint, MD
A retrospective study looking at use of transdermal Buprenorphine in older trauma patients with rib fractures found a good safety profile (less naloxone use) and less overall opioid use however no change in overall length of stay or mortality. Adding this to your multimodal pain strategy in older patients with rib fractures seems like a reasonable plan.
ournal of the American Geriatrics SocietyEarly View
CLINICAL INVESTIGATION
Iva Neupane, Brian Mikolasko, Charles A. Adams Jr, Joao Filipe Goncalves Monteiro, Nadia Mujahid, Linda Girouard, Jessica Arabi, Ashna Rajan, Audrea Bose, Stephanie Lueckel, Lynn McNicoll, Stefan Gravenstein
First published: 16 April 2026
Category: Geriatrics
Keywords: Constipation geriatric complex (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 5/2/2026)
Click here to contact Robert Flint, MD
A narrative review of literature involving older patients and constipation found:
“Major contributing factors include physical inactivity, sarcopenia, dehydration, inappropriate defecation posture, and polypharmacy, particularly opioids and anticholinergic agents. Importantly, these factors interact through the brain–gut–microbiota axis, contributing not only to gastrointestinal dysfunction but also to systemic outcomes such as frailty, cognitive decline, and increased healthcare burden, thereby supporting a multidimensional disease framework.”
It isn’t as simple as adding a laxative.
Mimura S, Morishita A, Kitaoka A, Sasaki K, Tai H, Yano R, Nakahara M, Oura K, Tadokoro T, Fujita K, et al. Constipation in Older Adults: Pathophysiology, Clinical Impact, and Management Strategies. Geriatrics. 2026; 11(2):47. https://doi.org/10.3390/geriatrics11020047
Category: Geriatrics
Keywords: Prescribing cascade (PubMed Search)
Posted: 4/28/2026 by Robert Flint, MD
(Updated: 4/30/2026)
Click here to contact Robert Flint, MD
The article outlines how instead of looking at medications as the cause of symptoms, we often add more medications to treat the medication induced symptoms. Here is an example of how we get to polypharmacy in older patients
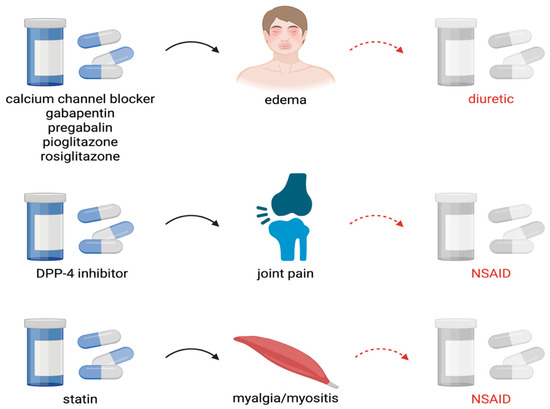
Bry?a A, Woro? J, Miedziaszczyk M, Lorkowska-Zawicka B, Bujak-Gi?ycka B, Orzechowski D, Po?etek P, Pa?ys W. Prescribing Cascade as a Therapeutic Error: A Danger for Geriatric Patients with Multimorbidity. Geriatrics. 2026; 11(2):37. https://doi.org/10.3390/geriatrics11020037
Category: Trauma
Keywords: Body armor, blunt injury, BABT (PubMed Search)
Posted: 4/26/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Body armor/ bullet resistant vests used by law enforcement are designed to stop penetration by handgun rounds. These rounds have less velocity than rifle rounds. When caring for someone who has been shot while wearing body armor, verify no penetration has occurred and then look for blunt injuries such as rib fractures, liver injuries, pneumothorax, cardiac contusion, vertebral injury, etc. Behind Armor Blunt Trauma (BABT) is the technical term for injuries caused by the transfer of kinetic energy that occurs when these vests are struck.
Volume 49, Issue 7, July 2018, Pages 1251-1257
Author links open overlay panelRosalind M. Jennings a, Chris Malbon b, Fiona Brock a, Stuart Harrisson c, Debra J. Carr b
Category: Trauma
Keywords: trauma, chronic pain, (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/23/2026)
Click here to contact Robert Flint, MD
This narrative review of the trauma literature looking at chronic pain after trauma found:
Kussé M, Hans G, Saldien V, Wildemeersch D. Chronic pain following major trauma: Prevalence, predictive models, and risk factors across common injury types. Trauma. 2026;0(0). doi:10.1177/14604086251404750
Category: Trauma
Keywords: obesity, trauma, mortality, organ failure, sepsis, ARDS (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/18/2026)
Click here to contact Robert Flint, MD
This German retrospective review of 1500 level one trauma center patients (ICU level or ISS over 9) found obesity was an independent predictor of ARDS, multisystem organ failure, and sepsis but not pneumonia or mortality.
Erdle, B., Mangold, J., Kalbhenn, J. et al. BMI is independently associated with ARDS, sepsis and multiorgan failure after major trauma—results of a high-volume retrospective observational cohort study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01603-7
Category: EMS
Keywords: prehospital, EMS, ultrasound (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/12/2026)
Click here to contact Robert Flint, MD
This German retrospective study compared the prehospital use of ultrasound by trained paramedics and compared their findings to in-hospital diagnosis and image results. The authors found:
“Diagnostic accuracy, defined as the concordance between prehospital POCUS-based working diagnoses and final in-hospital diagnoses, was particularly strong for lung ultrasound (pneumothorax, pulmonary edema, pneumonia and pleural effusion; sensitivity 91.7%, specificity 100%) and eFAST (sensitivity 100%, specificity 96.5%), while for the abdominal ultrasound examinations, the specificity was 70% and sensitivity was 71.43%.”
This study sets the stage for future prospective work looking at prehospital US use by paramedics.
Boehm, A., Bexten, T., Stanley, M. et al. Feasibility and diagnostic accuracy of paramedic-performed prehospital point-of-care ultrasound: a retrospective observational study. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01595-4
Category: Trauma
Keywords: trauma, treatment disparity, gender (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/8/2026)
Click here to contact Robert Flint, MD
This systematic literature review looking at gender differences in trauma care reveals:
Ghika-Nanchen, A., Marzorati, L., Merra, A. et al. Sex and gender bias in major trauma care: a scoping review. Scand J Trauma Resusc Emerg Med (2026). https://doi.org/10.1186/s13049-026-01596-3
Category: Geriatrics
Keywords: prehospital, geriatric, education (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 4/5/2026)
Click here to contact Robert Flint, MD
A modified 2 round Delphi study was used to create 57 learning objectives in geriatric care for European prehospital providers. Based on in-hospital learning objectives and literature, these experts came up with what appears to be a very reasonable and helpful list of education objectives for pre-hospital providers that could easily apply to emergency medicine learners as a whole. Here is their table:
https://link.springer.com/article/10.1186/s13049-026-01550-3/tables/3
Krohn, JN., Barrett, J., Heeren, P. et al. A European paramedic curriculum for geriatric emergency medicine developed via a modified Delphi technique. Scand J Trauma Resusc Emerg Med 34, 14 (2026). https://doi.org/10.1186/s13049-026-01550-3
Category: Trauma
Keywords: splenic injury, geriatrics, mortality (PubMed Search)
Posted: 4/4/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
In this retrospective cohort study looking at splenic injury management and outcomes in the UK, patients over age 65 had much higher mortality and were more often managed conservatively (vs splenectomy or embolization) despite having a lower splenic injury grade and lower overall injury severity score compared to those under 65. Many factors are possible here including frailty, reluctance to intervene in older patients, and lower mechanism of injury bias away from evaluation and management.
Jenkins P, Anton B, Blair G, et al. Traumatic splenic injury in the elderly population: Does management choice affect outcome? Trauma. 2026;0(0). doi:10.1177/14604086261430458
Category: Trauma
Keywords: Cervical immobilization, collar rigid, soft (PubMed Search)
Posted: 4/2/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Looking at trauma patients evaluated at a major trauma center before and after EMS switched from semi-rigid to soft cervical collars for immobilization found no difference in adverse outcomes. Add this to the mounting evidence that our current practice of spinal immobilization may not offer any benefit.
JACEP Open 2024;5:e13239. https://doi.org/10.1002/emp2.13239
Category: Trauma
Keywords: Shock, bradycardia, Hemoperitoneum, hypotension, (PubMed Search)
Posted: 3/29/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Bradycardia accompanying hypotension can be found in spinal cord injury (loss of autonomic reflex), beta blocker and calcium channel blocker overdose, intrinsic cardiac electrophysiologic derangement, and, often forgotten, intrabdominal hemorrhage. In the appropriate setting (blunt trauma, ruptured ectopic pregnancy), bradycardic hypotensive patients should be considered the same as tachycardic hypotensive patients and get a work up and treatment focused on Hemoperitoneum.
Category: Geriatrics
Posted: 3/26/2026 by Robert Flint, MD
Click here to contact Robert Flint, MD
Using a database of 300,000 patients and applying a predictive measure for mortality, these authors found that patients over 66 with a high likelihood of 6 month mortality at the time of presentation were more likely to be admitted to an ICU when they presented to an ED. The authors conclude there is much work to be done regarding discussion of goals of care based on this information.
Adeyemi O, Hill J, Siman N, Goldfeld KS, Cuthel AM, Grudzen CR. Acute Care Use and Prognosis in Older Adults Presenting to the Emergency Department. J Pain Symptom Manage. 2025;69(6):559-568. doi:10.1016/j.jpainsymman.2025.01.006
Category: Trauma
Keywords: Whole blood, trauma center level (PubMed Search)
Posted: 3/22/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Looking at a national database, this study concluded the use of low titer O whole blood during trauma resuscitations was increasing at level one centers but not at level 2 and 3 centers. Is this a representation of the national blood supply as whole blood is harder to stock? We need to understand this trend to assure equal and appropriate care to trauma patients across the country.
LETTER TO THE EDITOR
Steven G. Schauer, Mark H. Yazer
First published: 01 February 2026
Category: Trauma
Keywords: Trauma, geriatric, undertriage (PubMed Search)
Posted: 3/15/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Another study, this one from New Zealand, showing older trauma patients with similar injury severity score had less trauma team activations and higher mortality.
M.Nonis, A.McCombie, C.Wakeman, J.Geddes, and L. R.Joyce, “The Effect of Increasing Age on Outcomes in Major Trauma: A Retrospective Cohort Study,” Emergency Medicine Australasia38, no. 1 (2026): e70226, https://doi.org/10.1111/1742-6723.70226.
Category: Infectious Disease
Keywords: vasculitis, IgA, drug induced (PubMed Search)
Posted: 3/8/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This case report reminds us that vasculitis is an inflammatory process that attacks blood vessels leading to organ dysfunction. The etiology can be a hypersensitivity reaction (think drugs) or an IgA mediated process secondary to infection (Strep or Mycoplasma). In this case, concomitate use of NSAIDS (very common etiology of hypersensitivity) and Mycoplasma lead to vasculitis. Treatment ranges from supportive care, to steroids to immunosuppressive agents such as azathioprine.
Elaine Yu, Akousa Osei-Tutu, Rachna Subramony,
Small Vessel Vasculitis from Mycoplasma Infection and Concurrent Topical Nonsteroidal Anti-Inflammatory Drug (NSAID) Medication,
The Journal of Emergency Medicine,
Volume 82,
2026,
Pages 88-93,
ISSN 0736-4679,
https://doi.org/10.1016/j.jemermed.2025.12.003.
Category: Pharmacology & Therapeutics
Keywords: Drug reaction. (PubMed Search)
Posted: 3/5/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Of 925 ED headache patients in this meta analysis comparing extrapyramidal side effects of bolus vs. continuous infusion of metoclopremide the majority of the reactions occurred in the bolus group.
Ryuta Onodera, Yusuke Ito, Takahiro Itaya, Yoshie Yamada, Taku Iwami, Yusuke Ogawa,
Extrapyramidal symptoms and effectiveness of continuous vs bolus intravenous metoclopramide: A systematic review and meta-analysis,
The American Journal of Emergency Medicine,
Volume 103,
2026,
Pages 36-44,
ISSN 0735-6757,
https://doi.org/10.1016/j.ajem.2026.01.051.
Category: Trauma
Keywords: Ketamine, pain control, trauma (PubMed Search)
Posted: 3/1/2026 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
When compared to saline(!) trauma patients with a high injury severity score who received ketamine via pca for pain control had better quality of life indicators at 1,3, and 6 months post injury.
Trevino, C. , Carver, T. , Tomas, C. , Larson, C. , Mantz-Wichman, M. , Peppard, W. & deRoon-Cassini, T. (2026). Acute traumatic pain treatment with ketamine decreased PTSD and anxiety symptoms 6 months post hospital discharge. Journal of Trauma and Acute Care Surgery, 100 (2), 215-220. doi: 10.1097/TA.0000000000004835.
