Category: Toxicology
Keywords: Factor Xa inhibitor, reversal agent, adexanet alfa, andexxa (PubMed Search)
Posted: 5/4/2018 by Hong Kim, MD
(Updated: 5/11/2018)
Click here to contact Hong Kim, MD
On May 3, the FDA approved adexanet alfa, the reversal agent for factor Xa inhibitors - apixaban and rivaroxaban. It received both U.S. Orphan Drug and FDA Breakthrough Therapy designations.
Unlike indarucizumab (a monoclonal antibody fragment) to reverse dabigatran (direct thrombin inhibitor) associated bleeding, adexanet alfa is a recombinant modified human factor Xa decoy protein.
A phase 3 study showed that adexanet alfa decreased the anti-factor Xa activity of rivaroxaban by 92% from baseline and by 94% in apixaban treated participants.
ANNEXA-4 study involving participants with acute major bleeding (GI and intracranial) showed a significant decrease in the anti-factor Xa activity after the bolus dose of adexanet alfa and "effective" hemostasis was noted in 79% of the participants at 12 hours post infusion.
Andexanet alfa is expected to become available in June 2018.
Category: Neurology
Keywords: Intracerebral hemorrhage, ICH, hematoma expansion, prediction score, BAT score (PubMed Search)
Posted: 5/9/2018 by WanTsu Wendy Chang, MD
(Updated: 5/19/2026)
Click here to contact WanTsu Wendy Chang, MD
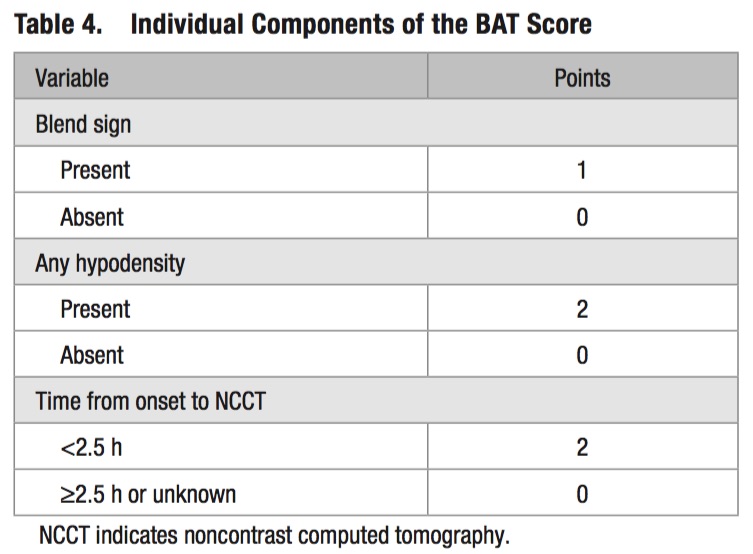
Morotti A, Dowlatshahi D, Boulouis G, et al. Predicting intracerebral hemorrhage expansion with noncontrast computed tomography: The BAT score. Stroke 2018;49(5):1163-9.
Follow me on Twitter @EM_NCC
Category: Geriatrics
Keywords: pneumonia, infection, delirium, atypical (PubMed Search)
Posted: 5/6/2018 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
- Half of elderly patients presenting with pneumonia will manifest signs of delirium
- Tachypnea is the most reliable and earliest vital sign abnormality
- Classic symptoms are not often helpful at predicting severity of illness
- Symptoms are unreliable
- Cough (63-84%)
- Dyspnea (58-74%)
- Fever by history (53-60%)
- Fever at arrival (12-32%)
- Pleuritic chest pain (8-32%)
- Sputum (30-65%)
Caterino JM. Evaluation and management of geriatric infections in the emergency department. Emerg Med Clin N Am 2008;26:319-343.
Category: Pediatrics
Keywords: supination with flexion, hyperpronation (PubMed Search)
Posted: 5/4/2018 by Sarah Kleist, MD
Click here to contact Sarah Kleist, MD
Nursemaid’s elbow is a common pediatric injury with peak incidence occurring between two and three years of age. It is a condition that typically arises from a sudden upward pull of the arm as an axial traction is placed on the forearm, and the radius is pulled through the annular ligament, resulting in subluxation of the radial head. Over the years, various maneuvers have been attempted, but the two most common are supination with flexion and hyperpronation. A 2017 Cochrane meta-analysis analyzed 8 trials specifically comparing supination with flexion versus hyperpronation. Data from those trials suggested that hyperpronation resulted in less failures at ?rst attempt than the supination-?exion, and although there was limited data, there was no obvious difference in adverse events or pain between the two techniques.
Bottom Line: There is likely a lower risk of failure with first attempt reduction with hyperpronation than with supination-flexion for nursemaid’s elbow.
References:
1. Schutzman SA, Teach S. Upper-extremity impairment in young children. Ann Emerg Med. 1995;26:474-479.
2. Hart GM. Subluxation of the head of the radius in young children. J Am Med Assoc. 1959;169:1734-1736.
3. Vitello S, Dvorkin R, Sattler S, Levy D, Ung L. Epidemiology of Nursemaid’s Elbow. Western Journal of Emergency Medicine, Vol 15, Iss 4, Pp 554-557 (2014). 2014:554.
4. Macias CG, Bothner J, Wiebe R. A comparison of supination/flexion to hyperpronation in the reduction of radial head subluxations. Pediatrics. 1998;102:e10-e10.
5. Bexkens R, Washburn FJ, Eygendaal D, van den Bekerom M,P.J., Oh LS. Effectiveness of reduction maneuvers in the treatment of nursemaid's elbow: A systematic review and meta-analysis. Am J Emerg Med. 2016;34.
6. Krul M, van der Wouden J,C., van Suijlekom-Smit LW, Koes BW. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database Syst Rev. 2009:CD007759.
7. Krul M, van der Wouden JC, van Suijlekom-Smit LW, Koes BW. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database Syst Rev. 2012.
8. Krul M. Manipulative interventions for reducing pulled elbow in young children. Cochrane Database of Systematic Reviews. 2017.
Category: Toxicology
Keywords: Intralipid Emulsion (PubMed Search)
Posted: 5/3/2018 by Kathy Prybys, MD
Click here to contact Kathy Prybys, MD
Despite initial excitement for the use of intravenous lipid emulsion (ILE) therapy as an antidote for serious poisonings due to lipohphilic drugs there remains an absence of evidence combined with an incomplete understanding of its efficacy, mechanisms of action, safety, and analytical interferences to recommend its use except in a few clinical scenarios.
The lipid emulsion workgroup performed a comprehensive analysis of four systematic reviews and based recommendations from consensus of expert panelists from the American Academy of Clinical Toxicology, the European Association of Poison Centres and Clinical Toxicologists, the American College of Medical Toxicology, the Asia Pacific Association of Medical Toxicology, the American Association of Poison Control Centers, and the Canadian Association of Poison Control Centers. Toxins evaluated had to have a minimum of three human cases reported in the literature.They concluded that ILE could be indicated for the following clinical situations:
The Bottom Line:
The use of Intravenous Lipid Emulsion in severe poisoning is recommended only for a few poisoning scenarios and was based on very low quality of evidence, and consideration of risks and benefits, adverse effects, laboratory interferences as well as related costs and resources.
Evidence-based recommendations on the use of intravenous lipid emulsion therapy in poisoning. Goseslin S. Hoegeberg L, Hoffman R, et al. Clinical Toxicology, 54:10, 899-923.
What are the adverse effects associated with the combined use of intravenous lipid emulsion therapy and extracorporeal membrane oxygenation in the poisoned patient? Hwee MD, Lee RH, et al. Clinical Toxicology, 53:3, 145-150.
Intravenous Lipid Emulsion Therapy and VA-ECMO rescue therapy for Massive Venlafaxine and Clonazepam Overdose. Thomas A, Ovakim D, et al. J Clin Toxicol 2017 7: 368.
Category: Critical Care
Posted: 5/1/2018 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
DOACs and the Critically Ill
Stensballe J, Moller MH. Ten things ICU specialists need to know about direct oral anticoagulants (DOACs). Intensive Care Med. 2018: epub ahead of print.
Category: Orthopedics
Keywords: Pregnancy, sports medicine (PubMed Search)
Posted: 4/28/2018 by Brian Corwell, MD
(Updated: 5/19/2026)
Click here to contact Brian Corwell, MD
Exercise talking points for the pregnant patient
(from ACSM 2017 Consesnsus statement)
Exercise throughout pregnancy is generally safe but should be monitored
No evidence of higher rates of preterm or prolonged labor, or deliveries that require induction or episiotomy
No evidence of negative effect on APGAR scores
Other benefits:
Avoidance of excessive weight gain, improved balance, and decreased back pain
Improved well-being, energy levels, and sleep patterns
Improved labor symptoms and facilitation of post-partum recovery
Lower risk of C-section
Reduced risk of having a large for gestational age (LGA) or small for gestational age (SGA) infant
Risks include environmental exposure, dehydration, hypoxia, and uterine trauma:
High impact or high-strain physical activity during the fetal implantation phase may lead to slightly higher risk of miscarriage
Sports with high risk of trauma last in pregnancy could result in placental abruption
Scuba diving is contraindicated because the fetus is not protected from decompression problems
Limit use of sauna or hot tub to fewer than ten minutes or omit altogether
Female athlete issues for the Team Physician: A consensus statement- 2017 Update
American College of Sports Medicine, 2018
Category: Toxicology
Keywords: fentanyl overdose, observation period (PubMed Search)
Posted: 4/26/2018 by Hong Kim, MD
Click here to contact Hong Kim, MD
Non-pharmaceutical fentanyl (NPF) is a major contributor to opioid overdoses and overdose fatality. In certain urban areas such as Vancouver, over 80% of heroin samples contain NPF. For isolated heroin overdose ED patients, they can be safely discharged after brief observation period (~2 hours). However, “safe” observation time for fentanyl is unknown.
Recently, a retrospective study evaluating the safe observation period in 1009 suspected (uncomplicated) fentanyl overdose ED visits (827 unique patients).
Results:
In the field:
In the ED:
Conclusion:
Scheuermeyer FX et al. Safety of a brief emergency department observation protocol for patients with presumed fentanyl overdose. Ann Emerg Med 2018 (PMID: 29530654)
Category: Critical Care
Keywords: acute hypoxic respiratory failure, intubation, noninvasive positive pressure ventilation, high flow nasal cannula, BiPAP, vapotherm (PubMed Search)
Posted: 4/25/2018 by Kami Windsor, MD
Click here to contact Kami Windsor, MD
ED physicians frequently utilize modailities such as noninvasive positive pressure ventilation (NIV) and high flow nasal cannula (HFNC) to support and potentially avoid intubation in patients presenting with acute hypoxic respiratory failure. Unfortunately, failure of these measures, resulting in "delayed" intubation, has been associated with increased mortality.1,2
A recent post-hoc analysis of data from a multicenter randomized controlled trial evaluated 310 patients with acute hypoxic respiratory failure managed with supplemental O2 by regular nasal cannula, HFNC, or NIV.3
The following factors were predictive of eventual intubation in the different groups:
Of note, 45% of the 310 patients eventually required intubation, and these patients in general had a higher initial respiratory rate and lower PaO2 at presentation, and were more likely to have bilateral infiltrates on CXR.
Bottom Line: Reevaluate your patients frequently. If RR remains high, P:F ratio remains low, or patient respiratory effort/work of breathing is not alleviated by noninvasive measures, consider pulling the trigger on intubation earlier.
Category: Pediatrics
Keywords: Infant fever, lumbar puncture, risks, ultrasound (PubMed Search)
Posted: 4/20/2018 by Jenny Guyther, MD
(Updated: 5/19/2026)
Click here to contact Jenny Guyther, MD
Unsuccessful lumbar punctures (LP) may lead to epidural hematoma (EH) formation at the site of needle insertion which may affect subsequent attempts and lead to no success or a grossly bloody sample. There is no standard definition of a traumatic LP based on CSF red blood cell counts. Gross blood may also be obtained by interrupting the vascular structures outside the spinal canal which would not result in EH formation.
This was a prospective study of children younger than 6 months who had an LP at a single children’s hospital. Post LP ultrasounds were completed by the investigating team and interpreted by a pediatric radiologist. 74 patients were included in the study. 31% of the patients had evidence of a post LP EH. 17% fully effaced the thecal sac which would likely preclude future success at that anatomic site. 25% of patients where the clinician did not feel there was a traumatic attempt had evidence of an EH.The study was not powered to determine the risk factors for EH formation. The study also did not look at any other consequences to EH.
Key points: Point of care ultrasound to evaluate EH and bleeding at the failed LP site my provide useful information for a location of subsequent attempts. Also US to evaluate for bleeding in the spinal canal may help with interpretation of the CSF when a large number of red blood cells are present.
Kusulas MP, Eutsler EP, DePiero AD. Bedside Ultrasound for the Evaluation of Epidural Hematoma After Infant Lumbar Puncture. Pediatric Emergency Care. Epub ahead of print. Feb 2018.
Category: Toxicology
Posted: 4/19/2018 by Kathy Prybys, MD
(Updated: 4/20/2018)
Click here to contact Kathy Prybys, MD
Bradycardias caused by poisoning are due to the toxin's effects on cardiovascular receptors and cellular channels and transport mechanisms and are often refractory to standard ACLS drugs. The most common drug classes responsible for bradycardias are calcium channel and beta blockers and digoxin (cardiac glycosides). Sodium channel blockers, clonidine, and opiates also can cause bradycardias. Antidotes are as follows:
** ILE is recommended only in life threatening poisonings where other accepted therapies have been use first or in cardiac arrest clinical scenarios.
Toxic Bradycardias in the Critically Ill Poisoned Patient. Givens M. Emergency Medicine International. Vol 2012.
The safety of high-dose insulin euglycaemia therapy in toxin-induced cardiac toxicity.Page CB, Ryan NM, et al. Clin Toxicol. 2017 Oct 26:1-6
Category: Critical Care
Posted: 4/18/2018 by Ashley Menne, MD
(Updated: 5/19/2026)
Click here to contact Ashley Menne, MD
Linezolid, an antimicrobial agent in the oxazolidinone class, often used to cover MRSA and/or VRE, is a reversible MAOI that increases the risk of serotonin syndrome, particularly when administered with other serotonergic agents.
In 2011, the US FDA issued a warning against concomitant use of Linezolid and other serotonergic agents, particularly SSRIs and SNRIs. When use of linezolid is absolutely indicated, an appropriate washout period prior to initiation was recommended.
Based on published reports and retrospective reviews, the incidence of linezolid-associated serotonin toxicity is between 0.54% and 18.2%.
A study published in the Journal of Clinical Psychopharmacology in Oct 2017 examined the incidence of serotonin syndrome with combined use of linezolid and SSRIs/SNRIs compared with linezolid alone and though there was a trend toward increased incidence in patients on SSRI/SNRIs, the authors were unable to find a statistically significant difference.
Several flaws:
-Study was retrospective
-Incidence of serotonin syndrome in both groups was very low: 1/87 (1.1%) in Linezolid + SSRI/SNRI group compared to 1/261 (0.4%) in Linezolid alone group.
-Patients in “Linezolid alone” group were not on SSRIs or SNRIs, but were allowed to be on other serotonergic medications.
Despite this study, there are many (>30) case reports of Linezolid-associated serotonin syndrome in patients taking other serotonergic agents.
Cyproheptadine (the “antidote”) is an H1 antagonist and nonspecific serotonin antagonist. A single case study published in 2016, reported successful use of cyproheptadine for prophylaxis against serotonin toxicity in a patient with schizophrenia, depression, and severe osteomyelitis requiring treatment with linezolid while on fluoxetine.
Bottom Line:
Risk of linezolid-associated serotonin syndrome may be lower than previously thought, however, it is still not recommended for use in patients taking concomitant serotonergic agents without an appropriate washout period.
In case of resistant infection with no other antibiotic treatment options, the risks and benefits of concomitant administration must be weighed seriously and providers must familiarize themselves with and be vigilant in watching for signs/symptoms of serotonin toxicity.
In situations where use of linezolid is unavoidable in patients on concomitant serotonergic agents, prophylactic cyproheptadine may be considered.
Karkow DC, Kauer JF, Ernst EJ. Incidence of Serotonin Syndrome With Combined Use of Linezolid and Serotonin Reuptake Inhibitors Compared With Linezolid Monotherapy. J Clin Psychopharmacol. 2017;37(5):518-523. doi:10.1097/JCP.0000000000000751.
Deardorff OG, Khan T, Kulkarni G, Doisy R, Loehr C. Serotonin Syndrome: Prophylactic Treatment With Cyproheptadine. Prim Care Companion CNS Disord. 2016;18(4). doi:10.4088/PCC.16br01966.
Woytowish MR, Maynor LM. Clinical Relevance of Linezolid-Associated Serotonin Toxicity. Ann Pharmacother. 2013;47(3):388-397. doi:10.1345/aph.1R386.
Ramsey TD, Lau TT, Ensom MH. Serotonergic and Adrenergic Drug Interactions Associated with Linezolid: A Critical Review and Practical Management Approach. Ann Pharmacother. 2013;47(4):543-560. doi:10.1345/aph.1R604.
Category: Orthopedics
Keywords: Stress fracture, amenorrhea (PubMed Search)
Posted: 4/14/2018 by Brian Corwell, MD
(Updated: 5/19/2026)
Click here to contact Brian Corwell, MD
Energy availability considers the amount of remaining energy for metabolic processes based on calories takin in with eating and calories burned through exercise or both.
Menstrual dysfunction occurs as a result of low energy availability causing decreased GnRH inhibition and ovarian suppression and decreased estrogen.
Low bone mineral density occurs due to amenorrhea and decreased energy availability. Estrogen limits bone resorption (stimulates calcitonin and renal calcium retention).
This is very important for young girls as by age 12 they have 83% of their total BMD & 95% two years after menarche.
If you see an athlete in the ED with one component of the triad, inquire about the other two. A 15yo athlete with a stress fracture may not realize that her disordered eating, excessive exercise or amenorrhea may by contributing factors and may benefit from follow up with PCP, dietitian, Gyn, etc.
Category: Toxicology
Keywords: clonidine toxicity, high-dose naloxone (PubMed Search)
Posted: 3/18/2018 by Hong Kim, MD
(Updated: 5/19/2026)
Click here to contact Hong Kim, MD
Clonidine, (central alpha-2 receptor agonist) can produce opioid-like toxidrome in addition to its cardiac effects (bradycardia and hypotension). Previous studies have shown that naloxone has variable (~40%) success in reversing CNS/respiratory depression and cardiac effect.
A recent retrospective study (n=51) of pediatric poisoning showed that administration of 5 to 10 mg had improved reversal of clonidine toxicity.
Total of 51 somnolent patients: 5- 10 mg of naloxone reversed 40 patients
There was no adverse effect from naloxone administration.
Repeat administration of naloxone was required in some patients.
Bottom line
Seger DL, Loden JK. Naloxone resersal of clonidine toxicity: dose, dose, dose. Clin Toxicol (Phila) 2018 Mar 16:1-7. doi: 10.1080/15563650.2018.1450986. [Epub ahead of print]
Category: Misc
Keywords: dental pain, ibuprofen, acetaminophen (PubMed Search)
Posted: 4/6/2018 by Michael Bond, MD
Click here to contact Michael Bond, MD
Category: Toxicology
Keywords: adulterated synthetic cannabinoid, elevated INR, brodifacoum (PubMed Search)
Posted: 4/4/2018 by Hong Kim, MD
Click here to contact Hong Kim, MD
In the past couple of weeks, there have been reports from Illinois about patients using adulterated synthetic cannabinoids, resulting in elevated INR and bleeding. To date, there are approximately 70 cases including 3 fatalities. Brodifacoum, a long-acting vitamin K mediated anticoagulant (similar to warfarin) has been identified in 10 cases. Brodifacoum is frequently used as rodenticide.
This week, Maryland Poison Center received our first notification of a patient with bleeding and elevated INR due to suspected adulterated synthetic cannabinoid use.
When evaluating our patient population:
Patient management of suspected cases:
Patient can be discharged when INR < 2 is achieved with oral vitamine K regimen only (without recent FFP infusion).
Review of published cases highlights that most patients are started on a median doses of 100 mg/day (range: 15 - 600 mg) and stabilize on a PO regimen of 50-100 mg/day. Prolonged PO vitamin K course of 2 – 3 months or longer should be anticipated.
Pease call the Maryland Poison Center at 1-800-222-1222 as we are working with the Maryland Department of Health and CDC to track these cases.
Gunja N, Coggins A, Bidny S. Management of intentional superwarfarin poisoning with long-term vitamin K and brodifacoum levels. Clinical Toxicology. 2011;49(5):385-390. doi:10.3109/15563650.2011.587126.
Category: Critical Care
Posted: 4/3/2018 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Acute on Chronic Liver Failure
Fuhrmann V, Whitehouse T, Wendon J. The ten tips to manage critically ill patients with acute-on-chronic liver failure. Intensive Care Med. 2018.
Category: Geriatrics
Keywords: palliative, advance directive, end-of-life (PubMed Search)
Posted: 4/1/2018 by Danya Khoujah, MBBS
(Updated: 5/19/2026)
Click here to contact Danya Khoujah, MBBS
25% of U.S. health care spending goes to the 6% of people who die every year. ICUs account for 20% of all health care costs. A new study has shown that patients with POLST (Physician Orders for Life-Sustaining Treatments) forms are less likely to receive unwanted life sustaining treatments when compared to patients with traditional Do-Not-Resuscitate orders (http://www.ohsu.edu/polst/). Using the POLST did not impact the degree of comfort care received for symptom management and helped individuals make more informed choices about the type and level of end-of-life care they wish to receive.
Category: Critical Care
Keywords: sepsis (PubMed Search)
Posted: 3/31/2018 by Ashley Martinelli
(Updated: 5/19/2026)
Click here to contact Ashley Martinelli
Bottom Line: Implement sepsis protocols as soon as sepsis is suspected prior to the end of the 3 hour treatment window.
Category: Pediatrics
Posted: 3/30/2018 by Rose Chasm, MD
(Updated: 5/19/2026)
Click here to contact Rose Chasm, MD
