Category: Neurology
Keywords: lumbar puncture, seizure, febrile seizure (PubMed Search)
Posted: 2/23/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
-- 6 to 12 months > "strongly consider" LP
-- 12 to 18 months > "consider" LP
-- 18 months and up > LP not routinely necessary; may consider after clinical assessment
-- Any infant/child with recent antibiotic treatment plus SFS > "strongly consider" LP
Category: Critical Care
Posted: 2/22/2011 by Mike Winters, MBA, MD
(Updated: 5/19/2026)
Click here to contact Mike Winters, MBA, MD
Hemodynamic Monitoring in the Ventilated Patient
Magder S. Hemodynamic monitoring in the mechanically ventilated patient. Curr Opin Crit Care 2011;17:36-42.
Category: Visual Diagnosis
Posted: 2/21/2011 by Rob Rogers, MD
Click here to contact Rob Rogers, MD
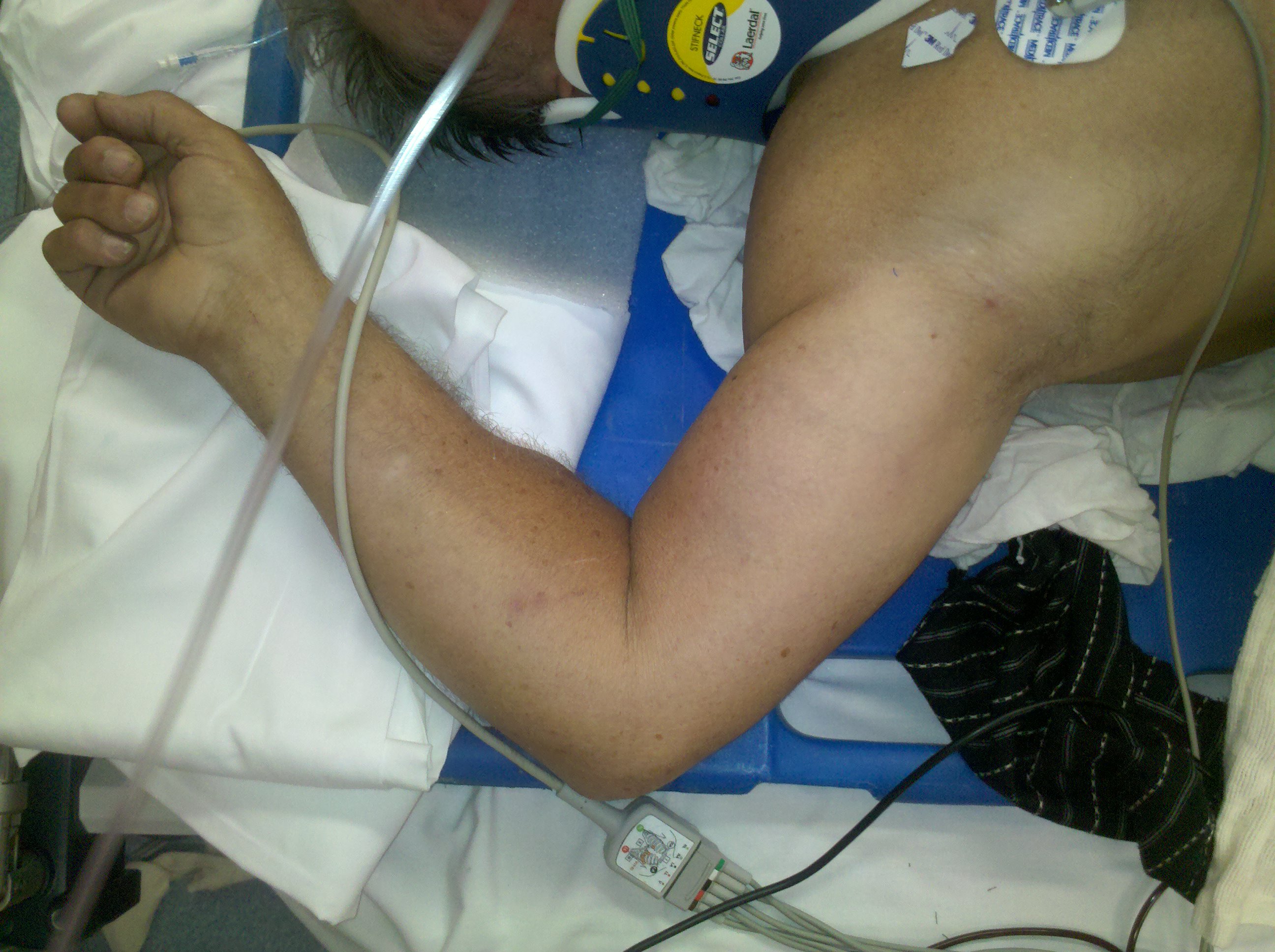
Luxatio Erecta-inferior glenohumeral dislocation
A rare shoulder dislocation caused by a hyperabduction injury to the arm.
Category: Cardiology
Keywords: bradycardia, bradydysrhythmia, digoxin, hyperkalemia (PubMed Search)
Posted: 2/20/2011 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
[Here's a nice simple pearl from Jeff Tabas, MD (Prof of EM at UCSF).]
3 causes of bradycardia to consider when the rhythm is not clearly sinus bradycardia:
1. Junctional bradycardia
2. Hyperkalemia
3. Digoxin toxicity
Category: Orthopedics
Keywords: radius, fracture, treatment (PubMed Search)
Posted: 2/19/2011 by Michael Bond, MD
Click here to contact Michael Bond, MD
Distal Radius Fractures
Typically distal radius fractures are treated with closed reduction and splinting in the ED, followed by operative repair. This is done because it is felt that patients will have the best functional outcomes if the bones are restored to their normal anatomic alignment. However, two studies published in 2010 suggest differently.
The study by Neidenbach showed that after one year there was no difference in functional outcomes between patients that were just splinted in the ED in the position the fracture was found versus those that had closed reduction with splinting.
The second study by Ego showed that there was no difference in outcomes between those that underwent conservative treatment with closed reduction and splinting versus those that underwent operative repair.
The take home point from these studies for the EM physician is that most distal radius fractures can be splinted in the position found with them following up with an orthopaedist. There is probably little advantage to performing a closed reduction in the ED knowing that this procedure can use a lot of valuable time and resources.
Neidenbach P, Audige L, Wilhelmi-Mock M, Hanson B, De Boer P. The efficacy of closed reduction in displaced distal radius fractures. Injury. 2010;41(6):592-598.
Egol KA, Walsh M, Romo-Cardoso S, Dorsky S, Paksima N. Distal radial fractures in the elderly: operative compared with nonoperative treatment. J Bone Joint Surg Am. 2010;92(9):1851-1857.
Category: Toxicology
Keywords: THC, marijuana (PubMed Search)
Posted: 2/18/2011 by Fermin Barrueto
(Updated: 5/19/2026)
Click here to contact Fermin Barrueto
Sold under the name of K2, Spice. Patients exposed to this will present with dry mouth, paranoia, tachycardia, hallucinations but will resolved rather quickly over several hours. Observation in the ED and supportive care is usually all that is needed. A little history about synthetic marijuana:
Category: Neurology
Keywords: ketamine, conscious sedation, procedural sedation (PubMed Search)
Posted: 2/16/2011 by Aisha Liferidge, MD
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Keywords: Pulmonary embolism, PE, echocardiography, ultrasound, hemodynamics, McConnell sign, right ventricle (PubMed Search)
Posted: 2/15/2011 by Haney Mallemat, MD
(Updated: 5/19/2026)
Click here to contact Haney Mallemat, MD
Casazza F., et al. Regional right ventricular dysfunction in acute pulmonary embolism and right ventricular infarction.Eur J Echocardiography 2005 Jan; 6(1): 11-4.
Category: Trauma
Keywords: blunt trauma, pneumothorax, CXR supine, ultrasound, seashore, stratasphere (PubMed Search)
Posted: 2/14/2011 by Haney Mallemat, MD
(Updated: 8/28/2014)
Click here to contact Haney Mallemat, MD
(Please note the prior version of this pearl was incorrect with respect to the images referenced. This version is corrected.)
Patient s/p blunt chest trauma. CXR (image 1) vs. lung ultrasound (image 2), do you see any inconsistencies?
Lung ultrasound in traumatic pneumothorax: The "Stratosphere Sign"
Written by Dr. Michael Allison.
For advanced sonographers:
1. Blaivas, M. et al. A prospective comparison of supine chest radiography and bedside ultrasound for the diagnosis of traumatic pneumothorax. Academic Emergency Med. 2005 Sep;12(9):844-9.
2. Lichtenstein D et al. Ultrasound diagnosis of occult pneumothorax. Crit Care Med. 2005 June;33(6): 1231-8.
Category: Cardiology
Keywords: syncope, near-syncope, pre-syncope (PubMed Search)
Posted: 2/13/2011 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
Is there a difference in the workup, etiologies, or prognosis between patients with syncope vs. near-syncope? Traditional teaching indicates that there is no difference, but that doesn't necessarily reflect common practice. Physicians sometimes are a bit less concerned about patients with near-syncope vs. patients with true, full-blown syncope; and many syncope studies exclude patients with near-syncope.
Grossman and colleagues recently published a useful reminder that patients with syncope and near-syncope have a similar 30-day rate of adverse outcome. However, they have a lower admission rate, reflecting the lower level of concern physicians have in their evaluation. Be wary of those patients with near-syncope. Don't be reassured just because they didn't hit the floor...yet!
Grossman SA, Babineau M, Burke L, et al. Do outcomes of near syncope parallel syncope? Amer J Emerg Med 2010 (article currently in press)
Category: Pediatrics
Keywords: head CT, trauma, pediatrics, head injury (PubMed Search)
Posted: 2/11/2011 by Adam Friedlander, MD
(Updated: 5/19/2026)
Click here to contact Adam Friedlander, MD
Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study.Lancet2009;374:1160-
Category: Toxicology
Keywords: dose-response, paracelsus (PubMed Search)
Posted: 1/26/2011 by Bryan Hayes, PharmD
(Updated: 2/10/2011)
Click here to contact Bryan Hayes, PharmD
Many consider Paracelsus (1493–1541) as the father of modern toxicology.
The introduction of the dose–response concept might have been his most important contribution to toxicology, meaning that everything is toxic at the right dose (even oxygen and water).
Category: Neurology
Keywords: IV tPA, stroke, alteplase (PubMed Search)
Posted: 2/9/2011 by Aisha Liferidge, MD
(Updated: 5/19/2026)
Click here to contact Aisha Liferidge, MD
-- Age > 80 years old
-- NIH Stroke Scale > 25
-- History of combination of previous stroke and diabetes
-- On anticoagulation medication, regardless of INR
Category: Critical Care
Posted: 2/8/2011 by Mike Winters, MBA, MD
(Updated: 5/19/2026)
Click here to contact Mike Winters, MBA, MD
Acute LV Dysfunction in the Critically Ill
Chockalingam A, Mehra A, Dorairajan S, et al. Acute left ventricular dysfunction in the critically ill. Chest 2010; 138:198-207
Category: Airway Management
Keywords: teaching, NEJM, app (PubMed Search)
Posted: 2/7/2011 by Rob Rogers, MD
(Updated: 5/19/2026)
Click here to contact Rob Rogers, MD
Great resource for teaching in the emergency department....
Here is a great new app that you can use when teaching residents and students in the ED. It's the NEJM app. Great pics, videos, audio, procedures, and articles. And, it's FREE.

Just go to the App store and search "NEJM"
Category: Cardiology
Keywords: hyperkalemia, digoxin, calcium (PubMed Search)
Posted: 2/6/2011 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
For those that listen to EmedHome's EM Cast, you may have already heard this but I thought it's worth sharing with everyone else:
Many of us learned in our training that you should never give calcium to a hyperkalemic patient that is on digoxin or has digoxin toxicity. However, there's a paucity of data to support this contention. Here's one more article suggesting that calcium in the presence of digoxin or dig-toxicity may, in fact, be okay.
Levine and colleagues retrospectively evaluated 161 patients with digoxin toxicity, of whom 23 patients received calcium for hyperkalemia. None of the patients developed significant dysrhythmias in the first hour after calcium, and there was no increase in mortality rate.
Though not definitive, this is further support for treating hyperkalemia with calcium even in the presence of digoxin toxicity.
Levine M, Nikkanen H, Pallin DJ. The effects of intravenous calcium in patients with digoxin toxicity. J Emerg Med 2011;40:41-46.
Category: Pharmacology & Therapeutics
Keywords: iohexol, iodixanol, radio contrast media, immediate hypersensitivity reactions (PubMed Search)
Posted: 2/5/2011 by Bryan Hayes, PharmD
Click here to contact Bryan Hayes, PharmD
Many patients report an allergy to iodinated RCM, sometimes adding to the complexity of diagnostic decision making. Here are a few pearls to help:
Bottom line: Despite the lack of cross reactivity with shellfish/iodine allergies AND the very low risk associated with today’s low osmolality agents, premedication is still indicated in patient’s with a history of IHR to RCM.
Category: Pediatrics
Keywords: head CT, trauma, pediatrics, head injury (PubMed Search)
Posted: 2/4/2011 by Adam Friedlander, MD
Click here to contact Adam Friedlander, MD
Head injuries in children under 2yo are stress provoking, particularly with regard to when you should be getting a head CT. Luckily, a large (42,412 children, 10,718 <2yo) multi-center trial exists to guide your behavior.
Category: Toxicology
Keywords: Methemoglobinemia,methylene blue (PubMed Search)
Posted: 2/3/2011 by Ellen Lemkin, MD, PharmD
(Updated: 5/19/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Category: Neurology
Keywords: stroke, seizure (PubMed Search)
Posted: 2/3/2011 by Aisha Liferidge, MD
(Updated: 5/19/2026)
Click here to contact Aisha Liferidge, MD
