Category: Orthopedics
Keywords: diabetes, exercise, weight loss (PubMed Search)
Posted: 2/13/2021 by Brian Corwell, MD
(Updated: 5/17/2026)
Click here to contact Brian Corwell, MD
What time of day is best for exercise to achieve weight loss goals?
Working out in the morning has traditionally held the edge, especially if done on an empty stomach.
Upon walking, elevated levels of cortisol and GH will aid in fat metabolism.
Switching to a morning workout may also decrease appetite throughout the day.
Morning exercise may also induce significant circadian phase?shifting effects. Patients report feeling more alert in the morning and get more tired at night. This may “force” people to get increased rest as poor sleep quality and duration has been associated with weight gain.
Moderate intensity aerobic exercise has been shown to cause immediate mood improvement and mental productivity. These effects can last up to 12 hours and may be a simple aid to combat job stress.
However, a recent small study looked at this question with a group of men at high risk for Type 2 diabetes.
Those that exercised in the morning had better blood sugar control and lost more abdominal fat than those who exercised in the morning.
Study: 32 adult males (58 ± 7 years) at risk for or diagnosed with type 2 diabetes performed 12 weeks of supervised exercise training either:
In the morning (8.00–10.00 a.m., N = 12) OR
In the afternoon (3.00–6.00 p.m., N = 20)
Test: Graded cycling test with ECG monitoring until exhaustion
Results: Compared to those who trained in the morning, participants who trained in the afternoon experienced superior beneficial effects of exercise training on peripheral insulin sensitivity, insulin?mediated suppression of adipose tissue lipolysis, fasting plasma glucose levels, exercise performance and fat mass.
Conclusion: Metabolically compromised patients may benefit from shifting their exercise routine to the afternoon from the morning. Ultimately, any exercise is great in this population, but this study may be worth sharing to your patients.
Mancilla R, Brouwers B, Schrauwen-Hinderling VB, Hesselink MKC, Hoeks J, Schrauwen P. Exercise training elicits superior metabolic effects when performed in the afternoon compared to morning in metabolically compromised humans. Physiol Rep. 2021 Jan;8(24):e14669.
Category: Critical Care
Keywords: Oxygenation, Mechanical Ventilation, Critical Care (PubMed Search)
Posted: 2/9/2021 by Mark Sutherland, MD
Click here to contact Mark Sutherland, MD
Optimal oxygenation targets and the possible, theoretical, benefits of hyperoxygenating critically ill patients have long been points of controversy. Multiple studies have suggested harm in pursuing aggressive hyperoxygenation amongst critical patients with various conditions ranging from myocardial infarction to sepsis to neurologic conditions. In addition, oxygen toxicity is a known mechanism causing ARDS.
The HOT-ICU trial adds to the list of arguments against hyperoxygenation, by looking at 2928 ICU patients on high levels of supplemental oxygen and targeting a paO2 of 60 mm Hg (low oxygen group) vs paO2 of 90 mm Hg (high oxygen group). There was no difference in mortality, or other significant difference in outcomes.
Bottom Line: A lower paO2 goal of 60 (correlates to an O2 sat of 90%) is noninferior to a higher paO2 goal of 90 (O2 sat of approximately 96%). When titrating oxygen, targeting a pulse ox of 90-96% is reasonable in critically ill patients. Be sure to include an upper limit on the sat goal, beware an O2 sat of 100%, and titrate down supplemental oxygen when the spO2 is above goal, as the paO2 may be dangerously high.
Schjørring OL, Klitgaard TL, Perner A, Wetterslev J, Lange T, Siegemund M, Bäcklund M, Keus F, Laake JH, Morgan M, Thormar KM, Rosborg SA, Bisgaard J, Erntgaard AES, Lynnerup AH, Pedersen RL, Crescioli E, Gielstrup TC, Behzadi MT, Poulsen LM, Estrup S, Laigaard JP, Andersen C, Mortensen CB, Brand BA, White J, Jarnvig IL, Møller MH, Quist L, Bestle MH, Schønemann-Lund M, Kamper MK, Hindborg M, Hollinger A, Gebhard CE, Zellweger N, Meyhoff CS, Hjort M, Bech LK, Grøfte T, Bundgaard H, Østergaard LHM, Thyø MA, Hildebrandt T, Uslu B, Sølling CG, Møller-Nielsen N, Brøchner AC, Borup M, Okkonen M, Dieperink W, Pedersen UG, Andreasen AS, Buus L, Aslam TN, Winding RR, Schefold JC, Thorup SB, Iversen SA, Engstrøm J, Kjær MN, Rasmussen BS; HOT-ICU Investigators. Lower or Higher Oxygenation Targets for Acute Hypoxemic Respiratory Failure. N Engl J Med. 2021 Jan 20. doi: 10.1056/NEJMoa2032510. Epub ahead of print. PMID: 33471452.
Category: Pharmacology & Therapeutics
Keywords: Buprenorphine, Acute Pain (PubMed Search)
Posted: 2/6/2021 by Wesley Oliver
Click here to contact Wesley Oliver
Buprenorphine is a partial opioid receptor agonist that has a higher binding affinity than pure opioid agonists. There can be unease in managing acute pain in patients sustained on buprenorphine for opioid use disorder due to many factors.
The main barriers to effective pain management in these patients are:
Take Home Points
In general, the treatment strategy for acute pain in patients on buprenorphine should be:
Category: Critical Care
Posted: 2/2/2021 by Mike Winters, MBA, MD
(Updated: 5/17/2026)
Click here to contact Mike Winters, MBA, MD
Mechanical Ventilation in COPD
Demoule A, et al. How to ventilate obstructive and asthmatic patients. Intensive Care Med. 2020; 46:2436-2449.
Category: Neurology
Keywords: seizure, status epilepticus, nonconvulsive, electrographic, EEG (PubMed Search)
Posted: 1/27/2021 by WanTsu Wendy Chang, MD
(Updated: 5/17/2026)
Click here to contact WanTsu Wendy Chang, MD
Bottom Line: Persistent or recurrent seizures are not uncommon in the first 24 hours after status epilepticus even in patients with resolved clinical seizure activity. Early use of EEG can help identify patients who need further escalation of treatment.
Follow me on Twitter @EM_NCC
Category: Airway Management
Keywords: Myocarditis, Covid-19 (PubMed Search)
Posted: 1/23/2021 by Brian Corwell, MD
(Updated: 5/17/2026)
Click here to contact Brian Corwell, MD
Exercise and Covid-19
The majority of COVID-19 cases fall into the mild-to-moderate category, with symptoms lasting less than 6 weeks on average.
The disease presents a challenge for clinicians seeking to offer counsel for patients wishing to return to exercise.
A recent cohort study in Germany looked at 100 patients (avg. age 49, 53% male) who had recovered from Covid-19 infection.
Most had been healthy, with no pre-existing medical conditions, before becoming infected.
The group had cardiac MRI (CMR) performed.
Average time interval between Covid-19 diagnosis and CMR was 71 days.
Cardiac involvement was seen in 78% of patients and ongoing myocardial inflammation in 60%.
Evidence based return to activity guidelines being developed are more conservative than in the past with other viral infections
https://link.springer.com/article/10.1007/s11420-020-09777-1/tables/1
1) Puntmann VO, Carerj ML, Wieters I, et al. Outcomes of Cardiovascular Magnetic Resonance Imaging in Patients Recently Recovered From Coronavirus Disease 2019 (COVID-19). JAMA Cardiol. 2020;5(11):1265–1273. doi:10.1001/jamacardio.2020.3557
2) Metzl, J.D., McElheny, K., Robinson, J.N. et al. Considerations for Return to Exercise Following Mild-to-Moderate COVID-19 in the Recreational Athlete. HSS Jrnl 16, 102–107 (2020).
Category: Toxicology
Keywords: alcoholic ketoacidosis, toxic alcohol ingestion, anion gap metabolic acidosis (PubMed Search)
Posted: 1/21/2021 by Hong Kim, MD
Click here to contact Hong Kim, MD
Anion gap metabolic acidosis is often found in ED patients. It can be difficult to distinguish between toxic alcohol (TA) ingestion and alcoholic ketoacidosis (AKA). A retrospective study attempted to identify risk factors associated with AKA when TA ingestion was the alternative diagnosis.
New York City poison center data was reviewed from Jan 1, 2000 to April 30, 2019.
Case definition of AKA included
Case definition of TA ingestion
Results
Univariate analysis showed following variables to be associated with AKA diagnosis
Multivariate logistic regression showed elevated ethanol concentration was associated with increased odd of AKA diagnosis
Conclusion
Category: Misc
Posted: 1/20/2021 by Michael Bond, MD
Click here to contact Michael Bond, MD
Title: Mammalian meat allergy (alpha-gal syndrome) following tick bites
Author: Dan Gingold, MD, MPH
Development of IgE antibodies to the oligosaccharide galactose-alpha-1-3-galactose (alpha-gal) appears to be responsible for an acquired allergy to non-primate mammalian meat (i.e., beef and pork) and derived products. Antigen in the salivary apparatus of certain ticks (gross!!) can sensitize an IgE-mediated response to alpha-gal which is present in mammalian meat.
Symptoms are similar to other IgE-mediated hypersensitivity reactions, and can cause a delayed-onset reaction with hives, GI upset, or anaphylaxis after ingestion of red meat. Treatment with standard anti-histamines and epinephrine is effective. Individuals with no prior history of meat sensitivity can develop the syndrome at any age, often after exposure to the outdoors in tick-endemic areas. Skin and blood allergy testing can confirm the diagnosis. Symptoms can persist for years, but can recede over time if not exposed to further tick bites.
In the US, the primary tick responsible is Lone Star Tick (Amblyomma americanum), found primarily in the Eastern, Southeastern, and Midwestern US. Other tick species in Europe, Australia, and Asia have been found to induce the syndrome as well. Interestingly, there is a cross-reactivity with the monoclonal antibody Cetuximab (used to treat colorectal and head and neck cancers), an allergic reaction to which can also induce similar alpha-gal meat sensitivity.
Having first been described in 2009, the syndrome often goes unrecognized; increased physician awareness can inform the evaluation, diagnosis, and education of patients presenting to the ED with undifferentiated allergic reaction.
Further Reading:
Khoury JK, Khoury NC, Schaefer D, Chitnis A, Hassen GW. A tick-acquired red meat allergy. Am J Emerg Med. 2018 Feb;36(2):341.e1-341.e3. doi: 10.1016/j.ajem.2017.10.044. Epub 2017 Oct 16. PMID: 29074067.
Crispell G, Commins SP, Archer-Hartman SA, Choudhary S, Dharmarajan G, Azadi P, Karim S. Discovery of Alpha-Gal-Containing Antigens in North American Tick Species Believed to Induce Red Meat Allergy. Front Immunol. 2019 May 17;10:1056. doi: 10.3389/fimmu.2019.01056. PMID: 31156631; PMCID: PMC6533943.
Category: Critical Care
Posted: 1/19/2021 by Lindsay Ritter, MD
Click here to contact Lindsay Ritter, MD
| Ever wonder what to tell the families regarding prognosis of the sickest COVID-19 patients you intubate in the ED or ICU? Introduction: Case fatality rates (CFR) for COVID-19 patients requiring invasive mechanical ventilation have been widely variable. A study in the Blue Journal (AJRCCM) examined patients requiring intubation in a systemic review and meta-analysis. The case fatality risk of an infection is represented by the proportion of patients who die among all infected cases in a population over a period of time. Methods: 69 studies axross 23 countries for a total of 57,420 patients with COVID-19 who required mechanical ventilation were included in analysis. Results: Overall case fatality rate was 45%, or about 1 death for every two intubated patients.. Among studies that included age stratification, pooled estimates of CFR were 47.9% in patients <40 (CI 46.4-49.4%) and 84.4% in patients >80 (CI 83.3-85.4%). Overall heterogeneity is high (I 2 .90%), In early COVID epicenters, CFR was 70% among patients aged more than 60 years of age. CFR increased exponentially with increasing age. Specifically in the US across 21 studies (3,811 intubated patients), CFR was 47% (95% CI, 36–57%). Studies from New York reported a CFR of 54% (95% CI, 36–72%) whereas other regions in the United States reported a CFR of 41% (95% CI, 30–53%). Definitive hospital CFR (aka for those with hospital discharge outcomes, 13,120 patients) was 56% (CI 47-65%). Conclusion: Almost half of patients with COVID-19 receiving IMV died based on the reported CFR. The reported CFR was higher in older patients and in early pandemic epicenters, which may be influenced by limited ICU resources. Limitations: Overall CFR of 45% still included patients in the hospital. Definitive hospital outcomes were only for 13,120 patients (36.6%). Significant variation in CFR exists between studies. |
Lim ZJ, Subramaniam A, Ponnapa Reddy M, Blecher G, Kadam U, Afroz A, Billah B, Ashwin S, Kubicki M, Bilotta F, Curtis JR, Rubulotta F. Case Fatality Rates for Patients with COVID-19 Requiring Invasive Mechanical Ventilation. A Meta-analysis. Am J Respir Crit Care Med. 2021 Jan 1;203(1):54-66.
Angriman F, Scales DC. Estimating the Case Fatality Risk of COVID-19 among Mechanically Ventilated Patients. Am J Respir Crit Care Med. 2021 Jan 1;203(1):3-4.
Category: Pediatrics
Keywords: Infection, sepsis, lactic acid (PubMed Search)
Posted: 1/15/2021 by Jenny Guyther, MD
(Updated: 5/17/2026)
Click here to contact Jenny Guyther, MD
Despite a lack of formal guidelines and evidence, lactate measurement has become a component of many pediatric emergency sepsis quality programs, with one survey showing that up to 68% of responding pediatric emergency medicine providers routinely measured it.
The Surviving Sepsis Campaign, last updated in February 2020, could not make a recommendation on the use of lactate in pediatric patients with suspected shock. The authors did state that lactate levels are often measured during the evaluation of septic shock if the lab can be obtained rapidly. However, lactate levels alone would not be an appropriate screening test.
Weiss SL, Peters MJ, Alhazzani W, et al. Surviving sepsis campaign international guidelines for the management of septic shock and sepsis-associated organ dysfunction in children. Intensive Care Med. 2020;46(Suppl 1):10-67.
Scott HF, Brou L, Deakyne SJet al. Association between early lactate levels and 30-day mortality in clinically suspected sepsis in children. JAMA Pediatr. 2017 Mar 1;171(3):249-255.
Category: Neurology
Keywords: stroke, thrombolysis, tissue plasminogen activator, tPA, monitoring (PubMed Search)
Posted: 1/13/2021 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
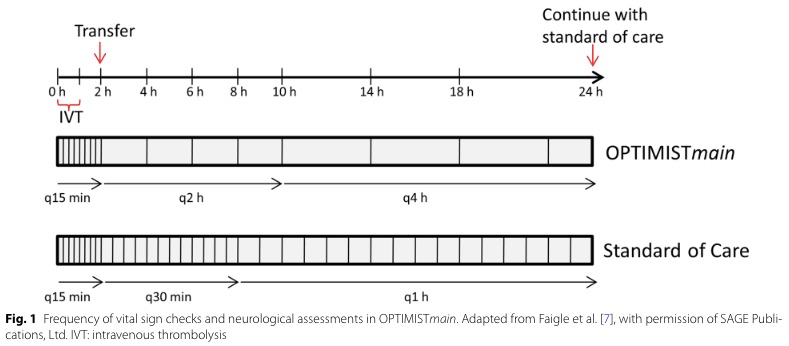
Bottom Line: Patients with NIHSS <10 may be safe for low-intensity post-tPA monitoring if they do not require critical care after an initial period of q15 min standard monitoring for the first 2 hours.
Follow me on Twitter @EM_NCC
Category: Critical Care
Keywords: COVID-19, Awake proning, intubation (PubMed Search)
Posted: 1/12/2021 by Quincy Tran, MD, PhD
(Updated: 5/17/2026)
Click here to contact Quincy Tran, MD, PhD
A single center (Nebraska, USA), retrospective analysis investigated the prevalence of intubation during hospital stay for 105 patients who had COVID-19 between March 24 to May 5, 2020 (1). 40 patients underwent awake proning vs. 60 patients did not undergo awake proning.
After adjusting for either SOFA or APACHE scores, patients with awake proning were associated with lower Hazard Ratios of intubation for SOFA (HR 0.30, 95% CI 0.09-0.96, p=0.043) and APACHE (HR 0.30, 95%CI 0.1-0.91, p=0.034).
Discussion
While this US study seemed promising, another Brazilian study being published earlier in July 2020 showed no difference in the prevalence of intubation between COVID-19 patients with proning or without proning (2).
These 2 studies highlighted the nature of this disease: high practice variability, uncertainty of therapeutic modalities. However, the complications from awake proning had been very low.
Conclusion:
Awake proning for hypoxic COVID-19 patients is a promising intervention but we will need more studies. In the meanwhile, we can try this therapeutic modality as the risk is low.
Category: Orthopedics
Keywords: tendon, antibiotics (PubMed Search)
Posted: 1/9/2021 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
A recent retrospective observational study looked at the association of oral antibiotics (primarily fluroquinolones) and tendon rupture.
Outcome data is very interesting for our practice, deviates from traditional teaching.
Population: 1 million Medicare fee for service beneficiaries from 2007-2016 (>65 years old)
Antibiotics queried: Seven total oral antibiotics of mixed class:
Outcome measures: all combined tendon ruptures and 3 by anatomic site (Achilles, rotator cuff {RC} and other)
Results: Of the 3 quinolones, only LEVOfloxacin showed a significant increase in risk of tendon rupture (16% for RC) and (120% for Achilles) in a 1 month window. The others did not show an increased risk
Among the other antibiotics, cephalexin showed an increase risk across all anatomic sites.
The authors note that the risk with levofloxacin never exceeded the risk of cephalexin in any comparison!
Baik S, Lau J, Huser V, McDonald CJ. Association between tendon ruptures and use of fluoroquinolone, and other oral antibiotics: a 10-year retrospective study of 1 million US senior Medicare beneficiaries.
BMJ Open. 2020;10(12):e034844. Published 2020 Dec 21.
Category: Critical Care
Posted: 1/6/2021 by Caleb Chan, MD
Click here to contact Caleb Chan, MD
Study Question: What is the association of relative hypotension (degree and duration of MPP deficit) in patients with vasopressor-dependent shock with the incidence of new significant AKI and major adverse kidney events (MAKE)?
Methods:
Results:
Take-aways:
Panwar R, Tarvade S, Lanyon N, et al. Relative hypotension and adverse kidney-related outcomes among critically ill patients with shock. A multicenter, prospective cohort study. Am J Respir Crit Care Med. 2020;202(10):1407-1418.
Category: Pharmacology & Therapeutics
Keywords: Octreotide, Vasopressin, Variceal Bleeding (PubMed Search)
Posted: 1/2/2021 by Wesley Oliver
Click here to contact Wesley Oliver
With a national shortage of octreotide an alternative treatment plan had to be implemented at our institution for patients presenting with variceal bleeding.
Drug references recommend a continuous infusion of vasopressin at 0.2 to 0.4 units/minute. Dose may be titrated as needed to a maximum dose of 0.8 units/minute with maximum duration of 24 hours to reduce incidence of adverse effects. Administer IV nitroglycerin concurrently to prevent ischemic complications and monitor closely for signs/symptoms of myocardial, peripheral, and bowel ischemia.
Protocol at our institution:
Vasopressin
Initiate vasopressin at 0.2 units/min.
Increase by 0.2 units/min if bleeding is not controlled after one hour (max dose: 0.8 units/min).
If bleeding controlled for 2 hours, can decrease by 0.2 units/min and reassess.
Limit use to 24 hours.
Nitroglycerin
Use nitroglycerin infusion to prevent adverse effects from vasopressin.
Initiate nitroglycerin at 40 mcg/min, titrate by 40 mcg/min to a max dose of 400 mcg/min.
Goal systolic blood press pressure of 90-100 mmHg. Do not start nitroglycerin if SBP <90 mmHg.
***Please note the vasopressin dose for this indication is significantly higher than the typical dose of 0.03 units/min we use for shock.***
Garcia-Tsao G, Abraldes JG, Berzigotti A, Bosch J. Portal hypertensive bleeding in cirrhosis: risk stratification, diagnosis, and management: 2016 practice guidance by the American Association for the Study of Liver Diseases [published correction appears in Hepatology. 2017;66(1):304]. Hepatology. 2017;65(1):310-335.
Terés J, Planas R, Panes J, Salmeron JM, Mas A, Bosch J, Llorente C, Viver J, Feu F, Rodés J. Vasopressin/nitroglycerin infusion vs. esophageal tamponade in the treatment of acute variceal bleeding: a randomized controlled trial. Hepatology. 1990 Jun;11(6):964-8.
Vasopressin. Lexicomp. UpToDate. Waltham, MA: UpToDate Inc. Available at: https://www.uptodate.com. Accessed on December 31, 2020.
Category: Toxicology
Keywords: Serum insulin level table (Attachment) (PubMed Search)
Posted: 12/31/2020 by Hong Kim, MD
Click here to contact Hong Kim, MD
Please see attachment for the table of serum insulin levels
Corcoran JN et al. Persistent hyperinsulinemia following high-dose insulin therapy: a case report. J Med Toxicol 2020;16:465-469.
Category: Toxicology
Keywords: high dose insulin. insulin kinetic (PubMed Search)
Posted: 12/31/2020 by Hong Kim, MD
Click here to contact Hong Kim, MD
High dose insulin (HDI) therapy is commonly used in patients with severe beta-adrenergic antagonist and calcium channel antagonist overdose. Hypoglycemia and hypokalemia are commonly known complication of HDI therapy. However, kinetics of insulin in patients who received HDI therapy is unknown.
A 51 year-old man with amlodipine overdose was infused HDI (10 unit/kg/hr) for 37 hours; Serial serum insulin levels were drawn after discontinuation of HDI.
Serum insulin levels are shown in below table
The serum insulin level remained significantly elevated during the first 24 hours (normal range: 2.6-24.9 microU/mL) and gradually decreased over 6 days.
Conclusion
Corcoran JN et al. Persistent hyperinsulinemia following high-dose insulin therapy: a case report. J Med Toxicol 2020;16:465-469.
Category: Orthopedics
Keywords: Hip pain, snapping hip, tendon (PubMed Search)
Posted: 12/27/2020 by Brian Corwell, MD
(Updated: 5/17/2026)
Click here to contact Brian Corwell, MD
Chief complaint: “My hip snaps when I exercise”
Both athletes and non-athletes may report a “snapping” sound with certain movements
This may affect up to 10% of the population
May be associated with activities than involve repetitive hip flexion
Symptoms may be due to an internal or an external cause
External causes are usually due to a tendon passing over a bony prominence
This can be felt as either an audible sensation and/or even a palpable snap
This may or may not involve pain or discomfort
This is most commonly due to a benign cause
During movements in flexion, extension or combined with internal rotation the iliotibial band may move over the greater trochanter.
Alternatively, the hamstring tendon may pass over the ischial tuberosity
There are several other causes with similar mechanisms
Symptoms are usually minimal and not serious
This can be reproduced on bedside clinical exam
Ask the patient to identify the area of snapping with one finger which will help with anatomic localization
First line therapy is physical therapy which focuses on:
Improving muscle length if muscle is too tight OR
Improving neuromuscular activation if problem is due to excessive muscle activation
Category: Pediatrics
Keywords: Procalcitonin, febrile infants, sepsis (PubMed Search)
Posted: 12/18/2020 by Jenny Guyther, MD
(Updated: 5/17/2026)
Click here to contact Jenny Guyther, MD
Young infants (0-90 days) have immature immune systems and are at higher risk for serious bacterial infections, particularly urinary tract infections, bacterial meningitis, and bacteremia. Infants less than 90 days old have an incidence of bacterial infections between 8 to 12.5%, while infants less than or equal to 28 days old have almost a 20% incidence.
Risk-stratification of this group has been a huge focus of research over the past couple of decades to help identify which patients require a full sepsis work-up, particularly in well-appearing infants if a source of fever is identified early. Recent studies have explored the utility of biomarkers in risk stratification in this population. A better ability to discriminate would hopefully decrease unnecessary lumbar punctures, antibiotic use, and hospital admission. Multiple studies have shown procalcitonin is able to outperform CRP for prediction of serious bacterial infections. Kuppermann et al developed a tool to identify low risk febrile infants < 60 days using procalcitonin and ANC. Their prediction rule gave a 97.7% sensitivity, 60% specificity, and 99.6% NPV for serious bacterial infection. There have been several other studies that have looked harder to detect infections such as osteomyelitis or septic arthritis across all pediatric patients and the data has not been as promising.
Bottom line: Procalcitonin shows promise as part of a risk stratification tool in infants younger than 60 days. Other studies have failed to show its relevance as a screening tool for osteomyelitis, septic arthritis, renal abscess or community acquired pneumonia.
Huppler AR, Eickhoff JC, Wald ER. Performance of low-risk criteria in the evaluation of young infants with fever: review of the literature. Pediatrics. 2010;125(2):228-233. doi:10.1542/peds.2009-1070
Schwartz S, Raveh D, Toker O, Segal G, Godovitch N, Schlesinger Y. A week-by-week analysis of the low-risk criteria for serious bacterial infection in febrile neonates. Archives of Disease in Childhood. 2009;94(4):287-292. doi:10.1136/adc.2008.138768
Woll C, Neuman MI, Aronson PL. Management of the Febrile Young Infant: Update for the 21st Century. Pediatr Emerg Care. 2017;33(11):748-753. doi:10.1097/PEC.
Kuppermann N, Dayan PS, Levine DA, et al. A Clinical Prediction Rule to Identify Febrile Infants 60 Days and Younger at Low Risk for Serious Bacterial Infections. JAMA Pediatr. 2019;173(4):342-351. doi:10.1001/jamapediatrics.
Category: Orthopedics
Keywords: Balance, mBESS, concussion (PubMed Search)
Posted: 12/12/2020 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
The Romberg test is part of the standard neurologic examination. The patient is asked to stand with feet together, hand on hips/sides and the eyes are closed. Vestibular and proprioceptive input is being tested.
This test is not very sensitive overall, but especially in concussed athletes.
Many concussed athletes are able to stand relatively stable despite their neurologic injury.
In order to better identify postural instability in concussion, we perform 3 separate balance tests (modified balance error scoring system, mBESS).
A) Romberg
B) Single leg stance
C) Tandem Stance
Have patient stand quietly with hands on hips
Have patient close eyes and start 20 second trial
If error occurs tell patient to return to start as quickly as possible
Examples of errors: opening eyes, lifting hands, falling out of position
