Category: Pharmacology & Therapeutics
Keywords: naloxone,overdose,heroin,opioid (PubMed Search)
Posted: 4/3/2014 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
1. https://www.networkforphl.org/_asset/qz5pvn/network-naloxone-10-4.pdf (Contains each law per state as of March 15, 2014)
2. http://www.usatoday.com/story/news/nation/2014/02/20/stateline-drug-overdose-deaths/5637519/
3. Intranasal Naloxone for Treatment of Opioid Overdose. The Medical Letter. Volume 56 (Issue 1438). March 17, 2014
Category: International EM
Keywords: HIV, global health, infectious disease, rash, puritis (PubMed Search)
Posted: 4/1/2014 by Andrea Tenner, MD
(Updated: 4/2/2014)
Click here to contact Andrea Tenner, MD
You are working in a clinic in Tanzania (or Baltimore, for that matter) when a 24 year old presents with this itchy rash on his feet. What's the diagnosis and what underlying systemic condition does it indicate?
Pruritic Papular Eruptions in HIV
Presentation:
University of Maryland Section for Global Emergency Health
Authors: Van Pham, MD and Colleen Holley, MD
Category: Critical Care
Posted: 4/1/2014 by Mike Winters, MBA, MD
(Updated: 5/19/2026)
Click here to contact Mike Winters, MBA, MD
Coagulopathies in Critical Illness - DIC
Hunt B. Bleeding and coagulopathies in critical care. NEJM 2014;370:847-59.
Category: Visual Diagnosis
Posted: 3/31/2014 by Haney Mallemat, MD
(Updated: 4/1/2014)
Click here to contact Haney Mallemat, MD
25 year-old female presents with the following. It seems to have occurred spontaneously and spontaneously resolves during her ED evaluation.
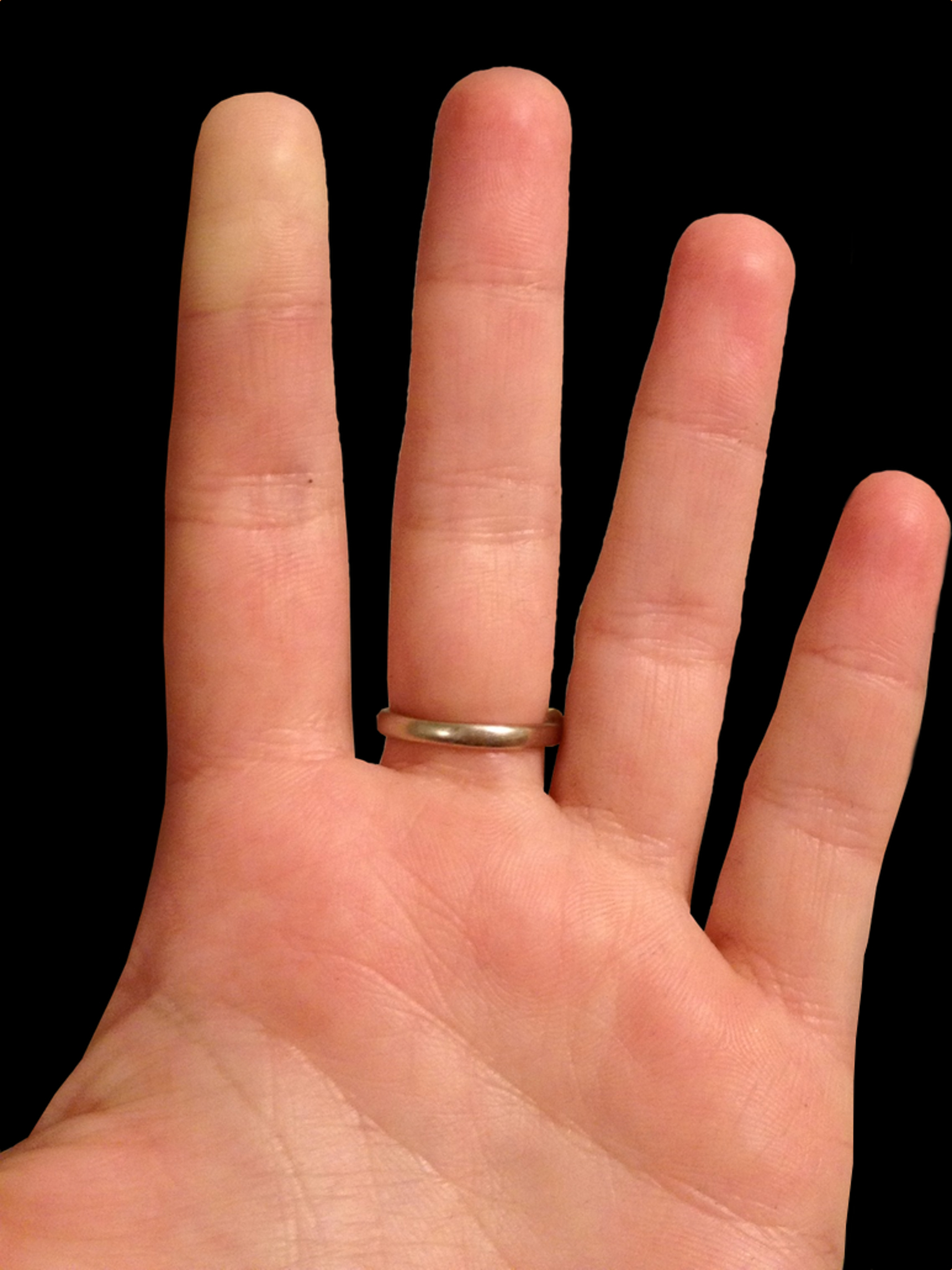
Answer: Raynaud phenomenon

Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Orthopedics
Keywords: DeQuervain, Intersection, Syndrome, Tenosynovitis (PubMed Search)
Posted: 3/30/2014 by Michael Bond, MD
(Updated: 5/19/2026)
Click here to contact Michael Bond, MD
DeQuervain and Intersection Syndromes:
Category: Toxicology
Keywords: opioids (PubMed Search)
Posted: 3/27/2014 by Fermin Barrueto
(Updated: 5/19/2026)
Click here to contact Fermin Barrueto
What are characteristics that increase the chance a patient is at risk for opioid-related death? A recent JAMA article begins to tackle this very issues. Baumblatt et al. found the following:
1) Patient with 4 or more prescribers had adjusted odds ratio 6.5 for opioid-related death
2) Patient with 4 or more pharmacies where they get their prescriptions aOR - 6.0
3) Patient with more than 100 mg of morphine equivalents mean per day aOR - 11.2
With the new Maryland Prescription Drug Monitoring program (PDMP) we can start looking at a patient's prescription drug use pattern. The recent JAMA article can help you identify patients at high risk to die an opioid-related death. Use the PDMP and be wary if a patient has more than 4 prescribers or pharmacies or has >100mg of morphine equivalents per day.
High-Risk Use by Patients Prescribed Opioids for Pain and Its Role in Overdose Deaths.
Baumblatt JA, Wiedeman C, Dunn JR, Schaffner W, Paulozzi LJ, Jones TF.
JAMA Intern Med. 2014 Mar 3. doi: 10.1001/jamainternmed.2013.12711. [
Category: International EM
Keywords: multiple myeloma, x-ray, global, neoplasm (PubMed Search)
Posted: 3/26/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
You are evaluating a 40 year old trauma victim and see this on pelvic xray. What are you worried about?
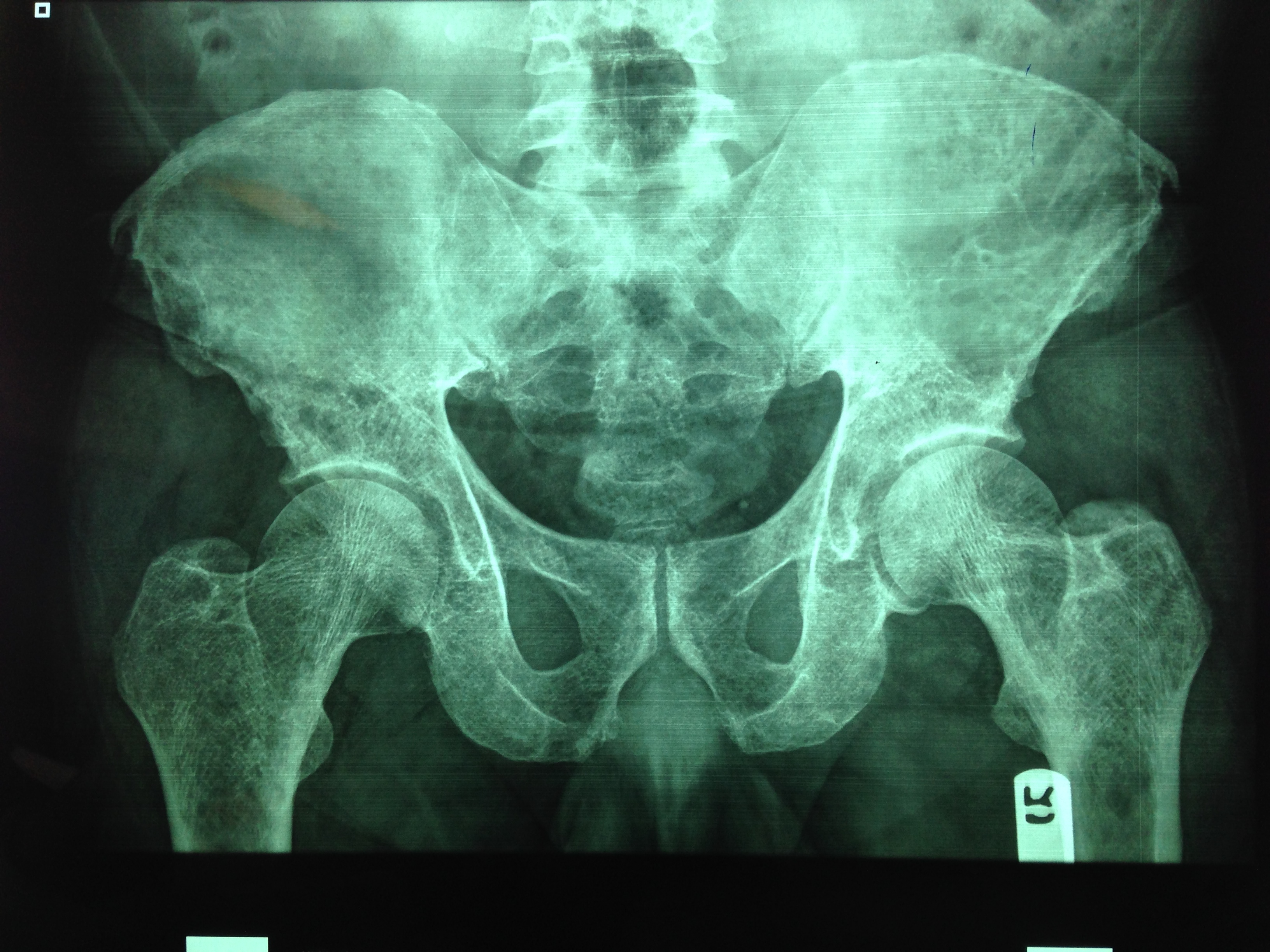
University of Maryland Section for Global Emergency Health
Authors: Colleen Holley, MD and Van Pham, MD
Mulligan, Michael. Multiple Myeloma Imaging. available: http://emedicine.
Category: Critical Care
Keywords: ARDS, Nitric Oxide, acute respiratory failure, mechanical ventilation (PubMed Search)
Posted: 3/23/2014 by John Greenwood, MD
(Updated: 3/26/2014)
Click here to contact John Greenwood, MD
Nitric Oxide appears to have NO role in ARDS
Background: The use of inhaled nitric oxide (iNO) in acute respiratory distress syndrome (ARDS) & severe hypoxemic respiratory failure has been thought to potentially improve oxygenation and clinical outcomes. It is estimated that iNO is used in up to 14% of patients, despite a lack of evidence to show improved outcomes.
Mechanism: Inhaled NO works as a selective pulmonary vasodilator which has been found to improve PaO2/FiO2 by 5-13%, but is costly ($1,500 - $3,000 per day) and increases risk of renal failure in the critically ill.
Study: A recent systematic review analyzed 9 different RCTs (N=1142) and compared mortality between those with severe (PaO2/FiO2 < 100) and less severe (PaO2/FiO2 > 100) ARDS and found that iNO does not reduce mortality in patients with ARDS, regardless of the severity of hypoxemia.
Bottom Line: Inhaled NO is an intriguing option for the treatment of refractory hypoxemic respiratory failure, however there does not appear to be a mortality benefit to justify it's high cost and potentially negative side effects. In the ED, it is important to focus on appropriate lung protective ventilation strategies (TV: 6-8 cc/kg IBW) and maintaining plateau pressures < 30 cm H2O in the initial stages of ARDS to prevent ventilator induced lung injury while awaiting ICU admission.
Reference
Adhikari NK, Dellinger RP, Lundin S, et al. Inhaled nitric oxide does not reduce mortality in patients with acute respiratory distress syndrome regardless of severity: systematic review and meta-analysis. Crit Care Med. 2014;42(2):404-12. [PMID: 24132038]
Follow me on Twitter (@JohnGreenwoodMD)
Category: Cardiology
Keywords: Cardiac arrest, LVAD, CPR, Chest compressions (PubMed Search)
Posted: 3/23/2014 by Ali Farzad, MD
Click here to contact Ali Farzad, MD
The number of patients with left ventricular assist devices (LVADs) is increasing and development of optimal resuscitative strategies is becoming increasingly important. Despite a lack of evidence, many device manufacturers and hospitals have recommended against performing chest compressions because of fear of cannula dislodgment or damage to the outflow conduit.
A recent retrospective analysis of outcomes in LVAD patients who received chest compressions for cardiac arrest did not support the theory that LVADs would be harmed by conventional resuscitation algorithms.
The study was a limited case series of only 8 LVAD patients over a 4 year period. All patients received compressions and device integrity was subsequently assessed by blood flow data from the LVAD control monitor or by examination on autopsy. Although more research is necessary to determine the utility and effectiveness of compressions in this population, none of the patients in this study had cannula dislodgment and half of the patients had return of neurologic function.
Shinar Z, Bellezzo J, Stahovich M, et al. Chest compressions may be safe in arresting patients with left ventricular assist devices (LVADs). Resuscitation. 2014. doi:10.1016/j.resuscitation.2014.01.003.
Category: Orthopedics
Keywords: ankle sprain (PubMed Search)
Posted: 3/22/2014 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Ankle Syndesmosis Injuries are also called high ankle sprains as they involve trauma to the ligaments above the ankle joint
Most ankle sprains are lateral ankle sprains. High ankle sprains are relatively uncommon.
Usual mechanism: External rotation injuries
Exam: Tenderness at the syndesmosis and compression of the tib/fib at the mid calf level causing syndesmosis pain (squeeze test)
Median recovery time is almost 4 times as long as a lateral ankle sprain 62days vs. 15days
Emergency department care is similar tto that of other ankle sprains but the added benefit of patient education and advice may improve overall care and follow-up.
Category: Pediatrics
Keywords: Head injury, vomiting, PECARN (PubMed Search)
Posted: 3/21/2014 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Category: International EM
Keywords: echocardiography, rheumatic heart disease, endocarditis, international (PubMed Search)
Posted: 3/19/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
35yo M with history of rheumatic heart disease presents with fever. What disease process is suggested by the echo?
Burke AP. Pathology of rheumatic heart disease. Medscape. 2013. Accessed 19 Mar 2013 at http://emedicine.medscape.com/article/1962779-overview#aw2aab6b4.
Category: Critical Care
Posted: 3/19/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
In 2001, Rivers et al. published a landmark article demonstrating an early-goal directed protocol of resuscitation that reduced mortality in septic Emergency Department patients.
Many questions have arisen throughout the years with respect to that trial; critics have complained about the overwhelming change in clinical practice based on this one single-center randomized trial.
Challenging Rivers data are the ProCESS (Protocolized Care for Early Septic Shock) investigators, who released the results from a multi-center randomized control trial of 1351 septic Emergency Department patients; the primary end-point was 60-day mortality. Click here for NEJM article.
Patients in this trial were randomized to one of three groups:
Protocol-based EGDT
Protocol-based standard (did not require central lines, inotropes, or blood transfusions
Usual care (no specific protocol; care was left to the bedside clinicians)
Bottom-line: The investigators did not find any difference in mortality between patients in the three groups and comment that the most important aspects of managing the septic patient may be prompt recognition and early treatment with IV fluids and antibiotics.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Visual Diagnosis
Posted: 3/17/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
62 year-old male presents with weakness, chills, cough, and malaise. Recently, he had four teeth extracted but felt fine immediately after the extraction. Past medical history includes diabetes and hypertension; CXR is below. What’s the diagnosis?
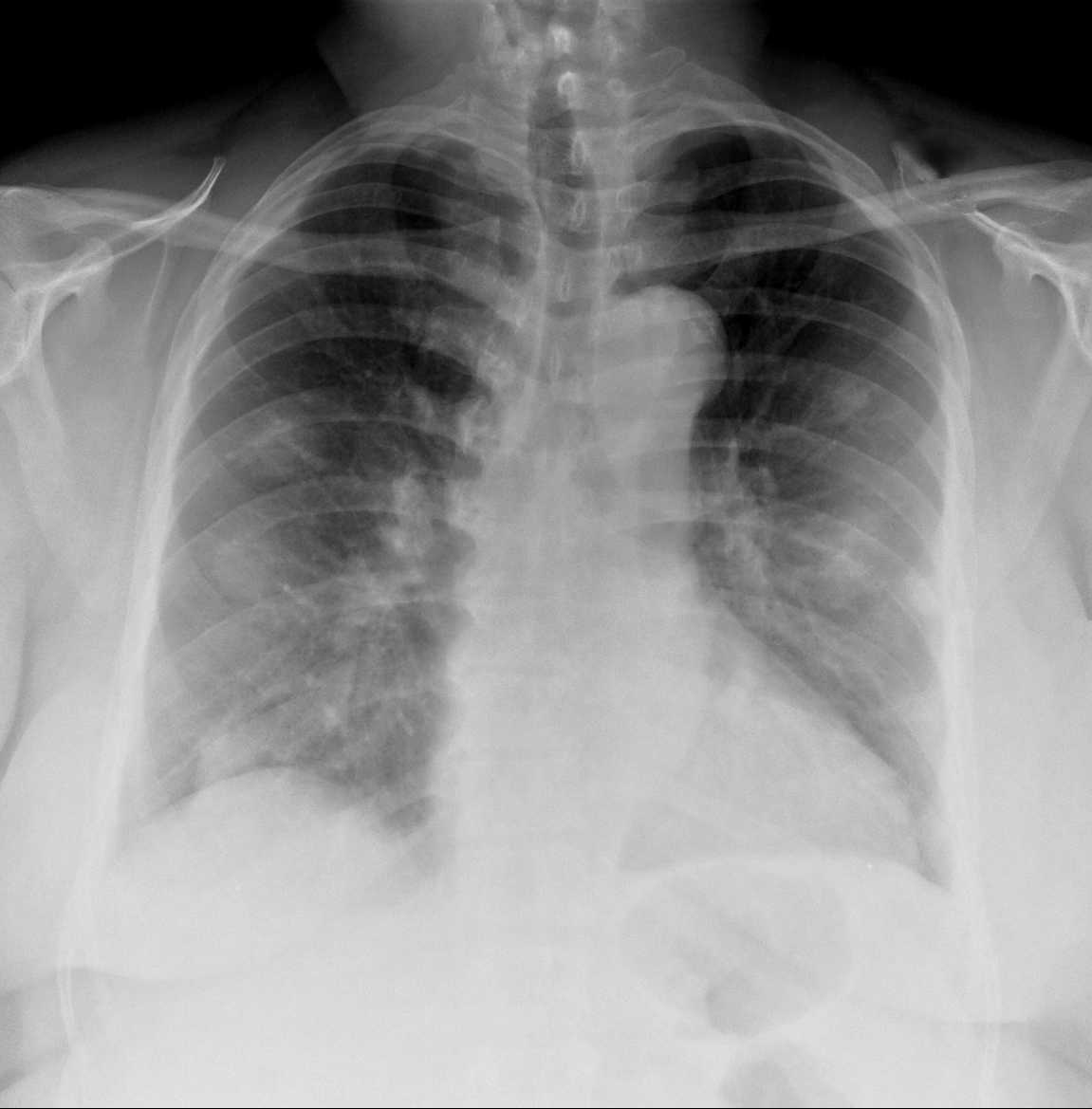
Answer: Septic pulmonary emboli (a.k.a. pulmonary puffballs); he was eventually diagnosed with bacterial endocarditis.
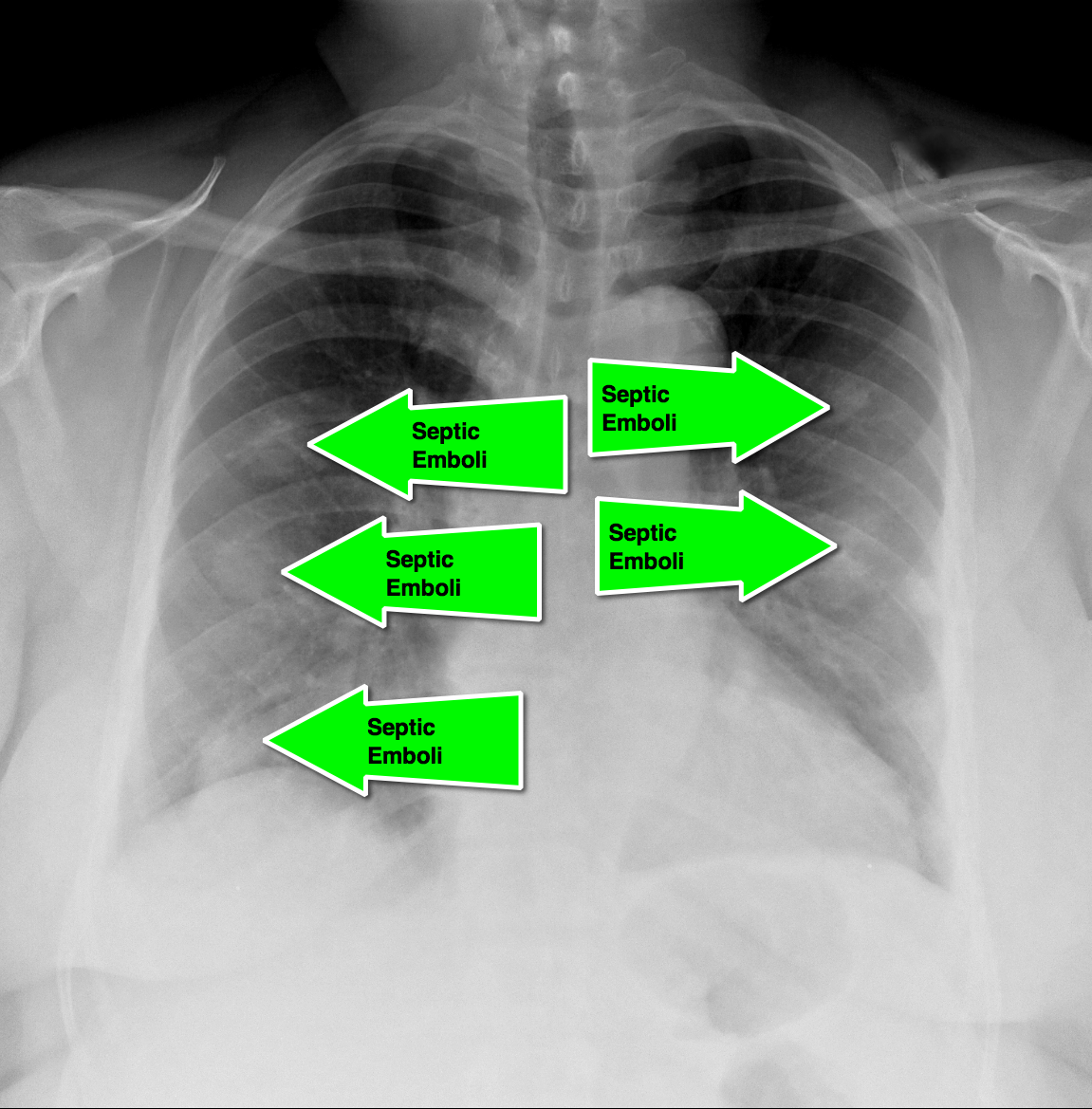
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Cardiology
Posted: 3/16/2014 by Semhar Tewelde, MD
Click here to contact Semhar Tewelde, MD
The HEART Score
Acute coronary syndrome defines a spectrum of diseases (unstable angina, NSTEMI, STEMI), without clear ECG abnormalities the diagnosis and disposition can be challenging
Several scoring systems have attempted to risk stratify patients: TIMI, PURSUIT, and GRACE
The TIMI & PURSUIT scores were designed to identify higher-risk patients and long-term mortality
A pilot/observational study has utilized a novel scoring system to risk stratify low to intermediate risk patients
The HEART (History, ECG, Age, Risk factors and Troponin) score:
This scoring system is limited given the small study size and requires further study/validation, but may be an easy, quick, and reliable predictor of outcome in chest pain patients
Six AJ, Backus BE, Kelder JC. Chest pain in the emergency room: value of the HEART score. Neth Heart J. Jun 2008; 16(6): 191–196.
Category: Toxicology
Keywords: Carbon Monoxide, (PubMed Search)
Posted: 3/15/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
Carbon Monoxide Half-Life:
Category: Visual Diagnosis
Posted: 3/14/2014 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
35 year-old carpet-layer presents with swelling of the superior portion of his knee that has progressively gotten worse over one week. He has no fever and has full range of motion (although pain is worse with movement). The knee is not tender to touch and the area is not erythematous or warm. What's the diagnosis?
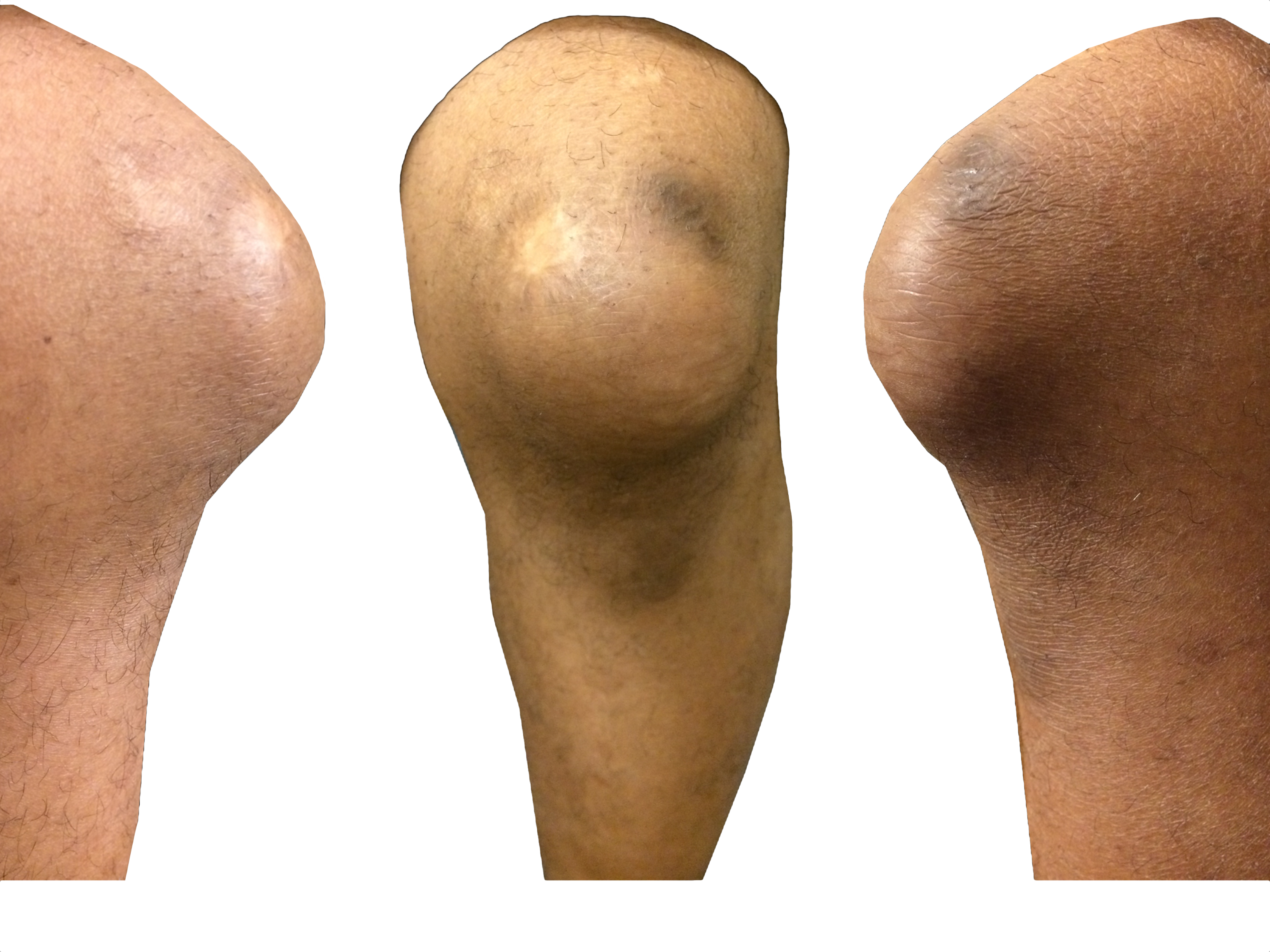
Answer: Pre-patellar bursitis
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Toxicology
Keywords: poison center, length of stay, hospital, charges (PubMed Search)
Posted: 3/11/2014 by Bryan Hayes, PharmD
(Updated: 3/13/2014)
Click here to contact Bryan Hayes, PharmD
In a collaborative effort between the Illinois Poison Center and the Illinois Hospital Association, a new study sought to determine a poison center's effect on hospital length of stay (LOS) and hospital charges.
While the methodology was understandably complex, the authors compared ~5,000 toxicology inpatients with poison center assistance to 5,000 toxicology inpatients without poison center assistance.
After adjusting for confounders, the LOS among patients with posion center assistance was 0.58 days shorter compared to that of patients without poison center assistance (CI 95%: -0.66, -0.51, p<0.001). Though hospital charges for poison center-assisted patients in the lower quintiles were significantly higher than patients without poison center-assistance (+$953; p<0.001), they were substantially lower in the most costly quintile of patients (-$4852; p<0.001).
Poison center assistance was associated with lower total charges only among the most expensive to treat. However, this outlier group is very important when discussing medical costs.
Friedman LS, et al. The association between U.S. Poison Center assistance and length of stay and hospital charges. Clin Toxicol 2014;52:198-206. [PMID 24580060]
Follow me on Twitter (@PharmERToxGuy) or Google Plus (+bryanhayes13)
Category: Visual Diagnosis
Keywords: international, global, hypoxia, clubbing (PubMed Search)
Posted: 3/12/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
What is this physical finding?
Answer: Clubbing
Differential Diagnosis of Clubbing in Children:
Clubbing was first documented by Hippocrates in a patient with empyema. It has been associated with cardiopulmonary disease, but also found in other disease processes such as hepatobiliary, infectious, and endocrine diseases. It can also occur without an underlying pathology. The pathophysiology behind these physical findings remain unknown. The workup and treatment should be aimed at managing the underlying cause.
University of Maryland Section for Global Emergency Health
Author: Van Pham, MD
Schwartz, Robert. Clubbing of the Nails. 3.12.14. http://emedicine.
Category: Critical Care
Keywords: lung ultrasound, pulmonary edema, B-lines (PubMed Search)
Posted: 3/11/2014 by Feras Khan, MD
Click here to contact Feras Khan, MD
1. A comet-tail artifact
2. Arising from the pleural line
3. Well defined
4. Hyperechoic
5. Long (does not fade)
6. Erases A lines
7. Moves with lung sliding
Technique
1. Lichtenstein D, Mezie re G, Biderman P, et al. The comet-tail artifact. An ultra- sound sign of alveolar-interstitial syndrome. Am J Respir Crit Care Med 1997; 156(5):1640–6.
