Category: Orthopedics
Keywords: Ossification Centers, Elbow (PubMed Search)
Posted: 3/27/2010 by Michael Bond, MD
(Updated: 5/19/2026)
Click here to contact Michael Bond, MD
Review of the Appearance of Ossification Centers in Children's Elbows
Determing if a child's elbow has a fracture or if you are looking at an ossification center is easier if you remember the mnemonic CRITOE. This is the order that the ossification centers appear:
Category: Pediatrics
Posted: 3/25/2010 by Rose Chasm, MD
(Updated: 4/11/2010)
Click here to contact Rose Chasm, MD
Category: Neurology
Keywords: hearing loss, sensorineural hearing loss, conductive hearing loss, acoustic neuroma, vestibulocholear nerve (PubMed Search)
Posted: 3/24/2010 by Aisha Liferidge, MD
(Updated: 4/11/2010)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 3/23/2010 by Evadne Marcolini, MD
Click here to contact Evadne Marcolini, MD
Catheter-related bloodstream infections occur in 3-8 percent of insertions, and are the highest cause of nosocomial bloodstream infections in the ICU.
The most effective measures to prevent catheter-related infections are as follows:
Especially applicable to those of us placing these lines in the ED or in the ICU is the last recommendation, based on a prospective study from Greece
-adequate knowledge and use of care protocols
-qualified personnel involved in changing and care
-use of biomaterials that inhibit microorganism growth and adhesion
-good hand hygiene
-use of an alcoholic formulation of chlorhexidine for skin disinfection and manipulation of the vascular line
-preference for subclavian route for placement
-use of full barrier protection during placement
-removal of unnecessary catheters
-use of ultrasound for placement of central lines
Frasca D, Dahyot-Fizelier C, Mimoz O: Prevention of central venous catheter-related infection in the intensive care unit. Crit Care; 2010; 14:212
Karakitsos D, Labropoulos N, De Groot E: Real time ultrasound guided catheterisation of the internal jugular vein: A prospective comparison with the landmark technique in critical care patients. Crit Care 2006; 10(6):175.
Category: Gastrointestional
Posted: 3/22/2010 by Rob Rogers, MD
(Updated: 5/19/2026)
Click here to contact Rob Rogers, MD
Complications of Liver Biopsy
Some considerations for the patient who presents with pain after a liver biopsy:
Consider getting a chest xray and a RUQ ultrasound to evaluate for these complications if they show up in the ED. CT scanning might also be required.
Also consider getting Interventional Radiology involved early in cases of bleeding as this is often the preferred treatment for biopsy site bleeding. In addition, a surgical consult is wise
in case the patient requires operative intervention.
Category: Cardiology
Keywords: oxygen, acute coronary syndromes (PubMed Search)
Posted: 3/22/2010 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
Although supplemental oxygen has long been considered standard care for patients with ACS, the evidence supporting this concept is largely based on animal studies in which acute MI was artificially induced. Should these studies be extrapolated to humans? Maybe not....
Further review of the animal and human literature actually indicates that the routine use of supplemental oxygen and induction of hyperoxia can actually induce adverse hemodynamic consequences such as increased coronary artery tone and reduction in coronary artery blood flow; reductions in cardiac output and increased systemic vascular resistance; and potentially increased infarction size. It certainly seems prudent to treat hypoxia, but if the patient is not hypoxic, skip the supplemental oxygen!
Wijesinghe M, et al. Routine use of oxygen in the treatment of myocardial infarction: systematic review. Heart 2009;95:198-202.
AND
Farquhar H, et al. Systematic review of studies of the effect of hyperoxia on coronary blood flow. Am Heart J 2009;158:371-377.
Category: Misc
Keywords: Billing, Critical Care (PubMed Search)
Posted: 3/20/2010 by Michael Bond, MD
Click here to contact Michael Bond, MD
Critical Care billing is time dependent and includes all time spent caring for and coordinating (i.e.: reviewing records, talking to consultants or family) the care of the patient except for the time spent doing separately billable procedures (i.e. central line, CPR, etc). The following procedures taken from the ACEP website are included in the Critical Care code so the time spent doing these procedures should BE included in your total Critical Care time .
They are :
ACADEMIC MEDICINE CAVEAT: For the reporting of time-based services, such as critical care or moderate sedation, the teaching physician must be directly present during the entire reported time period.
ACEP Coding and Reimburshment Website http://www.acep.org/practres.aspx?LinkIdentifier=id&id=33484&fid=910&Mo=No&taxid=117956#critcare
Category: Pediatrics
Keywords: Newborn screen, pediatrics, hypothyroidism, neonatal, congenital (PubMed Search)
Posted: 3/18/2010 by Adam Friedlander, MD
(Updated: 3/20/2010)
Click here to contact Adam Friedlander, MD
Congenital hypothyroidism (CH) is almost uniformly identified before symptoms develop because of newborn screening. Though this problem will rarely present to the Emergency Department, it is not uncommon for parents with poor access to care to present to EDs after being notified of an abnormal screen. Here is what you need to know:
So:
Category: Toxicology
Keywords: urine toxicology screen (PubMed Search)
Posted: 3/18/2010 by Fermin Barrueto
(Updated: 3/27/2010)
Click here to contact Fermin Barrueto
When you draw a urine toxicology screen it can mislead more often than help you. Here is a quick list of the test followed by some medications that cause false positives - when in doubt, call your lab to find out specifics since results will vary lab to lab:
TCA - diphenhydramine, carbamazepine, cyclobenzaprine (side note: TCA screen should never be used to determine TCA toxicity, your ECG and physical exam should be enough to determine if the patient is toxic from TCA
Cocaine - the most accurate test on the screen, positive for up to 5 days
PCP - dextromethorphan and ketamine can turn it positive
Amphetamines - pseudoephedrine, ephedrine, phenylephrine and many other OTC cough decongestants can as well, the worst screening test with the largest number of false positives
Category: Neurology
Keywords: temporal lobe epilepsy, seizure, focal seizure (PubMed Search)
Posted: 3/17/2010 by Aisha Liferidge, MD
(Updated: 5/19/2026)
Click here to contact Aisha Liferidge, MD
-- Deja' vu (feeling of familiarity) -- Jamais vu (feeling of unfamiliarity)
-- Specific or single set of memories -- Amnesia
-- Auditory -- Gustatory -- Visual -- Disphoric -- Euphoric
Category: Critical Care
Posted: 3/16/2010 by Mike Winters, MBA, MD
(Updated: 5/19/2026)
Click here to contact Mike Winters, MBA, MD
Warfarin and ICH
Rincon F, Mayer SA. Clinical review: Critical care management of spontaneous intracerebral hemorrhage. Crit Care 2008; 18:237.
Goldstein JN, Rosand J, Schwamm LH. Warfarin reversal in anticoagulant-associated intracerebral hemorrhage. Neurocrit Care2008; 9:277-83.
Category: Cardiology
Keywords: acute coronary syndromes, diaphoresis (PubMed Search)
Posted: 3/14/2010 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
A recent study of nearly 800 patients with chest pain evaluated symptoms and signs that are most predictive of ruling in for ACS. The following characteristics made acute MI more likely (likelihood ratios in parentheses): observed diaphoresis (5.18), central location of chest pain (3.29), associated vomiting (3.50), radiation of the pain to bilateral arms (2.69), and radiation of pain to the right arm (2.23).
As we've said before, if your patient sweats, it ought to make YOU sweat!
[BodyR, et al. Resuscitation 2010;81:281-286.]
Category: Orthopedics
Keywords: Knee, Dislocation (PubMed Search)
Posted: 3/13/2010 by Michael Bond, MD
(Updated: 5/19/2026)
Click here to contact Michael Bond, MD
Knee Dislocation:
Klineberg EO, Crites BM, Flinn W, et al: The role of arteriography in assessing popliteal artery injury in knee dislocations. J Trauma. 2004 Apr;56(4):786-90.
Hollis JD, Daley B, et al: 10-year review of knee dislocations: is arteriography always necessary? J Trauma. 2005 Sep;59(3):672-5.
Category: Toxicology
Keywords: food, allergy, propofol, soy, peanut, egg (PubMed Search)
Posted: 3/9/2010 by Bryan Hayes, PharmD
(Updated: 3/20/2010)
Click here to contact Bryan Hayes, PharmD
According to the Food Allergy and Anaphylaxis Network, the eight most common food allergies, which account for 90% of the food allergies in the U.S., are: dairy, soy, wheat, shellfish, fish, peanut, tree nut, and egg.
Several medications are formulated with these ingredients and should be avoided in patients with reported allergies.
Category: Neurology
Keywords: frontal lobe epilepsy, seizures (PubMed Search)
Posted: 3/10/2010 by Aisha Liferidge, MD
(Updated: 3/20/2010)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 3/5/2010 by Evadne Marcolini, MD
(Updated: 5/19/2026)
Click here to contact Evadne Marcolini, MD
Primary Intracranial hemorrhage is associated with the following risk factors:
Common causes of secondary ICH are as follows:
The question of how to address elevated blood pressure in spontaneous intracranial hemorrhage has been debated. High blood pressure may cause hematoma expansion, but this has not been proven. Lowering blood pressure may help reduce neurologic deterioration, but this has also not been proven in the literature.
The AHA recommended guidelines for blood pressure management in spontaneous ICH are as follows:
If SBP>200 or MAP>150, consider aggressive reduction of BP with continuous IV infusion, monitoring BP every 5 minutes
If SBP>180 or MAP>130, with evidence or suspicion of elevated ICP, consider monitoring ICP and reducing BP using intermittent or continuous IV medications to keep CPP>60 to 80
If SBP>180 or MAP>130 without evidence or suspicion of elevated ICP, then consider a modest reduction of BP (MAP of 110 or targeted SBP 160/90) using intermittent or continuous IV medications, monitoring BP every 15 minutes
Nyquist P: Management of Acute Intracranial and Intraventricular Hemorrhage. Crit Care Med 2010;38(3):946-953
Category: Vascular
Keywords: Aneurysm (PubMed Search)
Posted: 3/8/2010 by Rob Rogers, MD
(Updated: 5/19/2026)
Click here to contact Rob Rogers, MD
Splenic Artery Aneurysm (SAA)
Ever scanned someone and the report says "incidental note of a splenic artery aneurysm"? Well, if it hasn't happened yet, it will sooner or later. This type of aneurysm isn't that rare and with the number of abdominal CTs we order we are bound to see this in clinical practice.
Some important points to remember about SAA:
Category: Cardiology
Keywords: pericarditis, prognosis (PubMed Search)
Posted: 3/7/2010 by Amal Mattu, MD
(Updated: 5/19/2026)
Click here to contact Amal Mattu, MD
Major and minor clinical prognostic predictors for pericarditis have been described as follows:
Major: fever > 38 degrees C, subacute onset, large effusion, tamponade, lack of response to aspirin or NSAIDs after at least 1 week of therapy
Minor: myopericarditis, immunodepression, trauma, oral anticoagulant therapy
Patients with any of these criteria [major or minor] should strongly be considered for admission. In the absence of these factors, studies show that patients managed as outpatients do well.
[Imazio M, Spodick DH, Brucato A, et al. Controversial issues in the management of pericardial diseases. Circulation 2010;121:916-928.]
Category: Orthopedics
Keywords: Pelligrini, Steida (PubMed Search)
Posted: 3/6/2010 by Michael Bond, MD
Click here to contact Michael Bond, MD
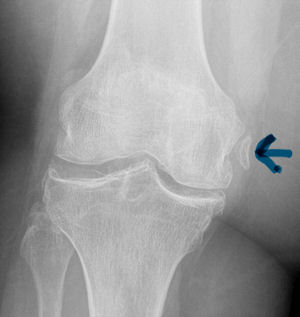
Pelligrini-Stieda Lesion:
A Pelligrini-Stieda lesion is shown in the radiograph below. This lesion was originally described in 1905, and is associated with a tear of the Medial Collateral Ligament. Heterotrophic calcification forms causing chronic pain, which typically needs to be surgically excised.
So for the students out there, it is possible to diagnosis an MCL tear on plain radiographs. Just not very often.
Category: Toxicology
Keywords: Lavage, activated charcoal, hyperinsulinemia, intralipid, toxicology, narcan (PubMed Search)
Posted: 3/4/2010 by Ellen Lemkin, MD, PharmD
(Updated: 5/19/2026)
Click here to contact Ellen Lemkin, MD, PharmD
| Cutting Edge | Old School |
| Gastric Lavage | |
| Hyperinsulinemia and Euglycemia | Supportive care, glucagon for beta blocker overdoses |
| Intralipid administration | Supportive care for anesthetic overdoses, TCAs, and other lipid soluble agents |
| Low dose or NO narcan | High dose narcan for opoid overdoses |
| Checking salicylates and tylenol levels for overdose | Tox screens for everyone |
