Category: Orthopedics
Keywords: Odontoid, fracture (PubMed Search)
Posted: 6/26/2010 by Michael Bond, MD
(Updated: 5/17/2026)
Click here to contact Michael Bond, MD
Odontoid Fractures:
There are three types of C2 odontoid fractures:

Category: Pediatrics
Posted: 6/24/2010 by Rose Chasm, MD
(Updated: 5/17/2026)
Click here to contact Rose Chasm, MD
MedStudy Pediatric Board Review, 1st edition
Category: Toxicology
Keywords: copperhead, crofab (PubMed Search)
Posted: 6/24/2010 by Fermin Barrueto
(Updated: 5/17/2026)
Click here to contact Fermin Barrueto
In the state of Maryland, the most common venomous snake is the copperhead. Though not as dangerous as the rattlesnake, it can still cause loss of function of limb and mortality in the pediatric patient.
Treatment has involved the use of CroFab (Protherics, Atlanta). This ovine derived monovalent immunoglobolin is actually made against the following snakes:
Though efficacy has been shown with these snakes, we are hoping for cross-reactivity when we treat copperheads. There are case series and case reports (1) that have shown anectdotal improvement. We are still awaiting a real randomized controlled trial - may never happen.
Lavonas EJ, Gerardo CJ, O'Malley G, Arnold TC, Bush SP, Banner W Jr, Steffens M, Kerns WP 2nd.
Ann Emerg Med. 2004 Feb;43(2):200-6.
Category: Neurology
Keywords: MS, multiple sclerosis, brain, mri, dawson's fingers (PubMed Search)
Posted: 6/23/2010 by Aisha Liferidge, MD
(Updated: 5/17/2026)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 6/22/2010 by Evadne Marcolini, MD
(Updated: 5/17/2026)
Click here to contact Evadne Marcolini, MD
Acute renal failure occurs in 1-25% of critically ill patients, with an associated mortality of 28 - 90%.
The RIFLE Criteria represent the first consensus definition of acute renal failure used to classify critically ill patients as to their kidney function. Notably, we use the worst possible classification according to the criteria, which measures either serum creatinine, urine output or both.
Rinaldo Bellomo1, Claudio Ronco, John A Kellum, Ravindra L Mehta, Paul Palevsky and the ADQI workgroup
Acute Renal Failure - definition, outcome measures, animal models, fluid therapy and information technology needs: The Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group.
Critical Care 2004, 8:R204-R212 (DOI 10.1186/cc2872)
This article is online at: http://ccforum.com/content/8/4/R204
Category: Geriatrics
Keywords: nitritie, infections, elderly, geriatric (PubMed Search)
Posted: 6/20/2010 by Amal Mattu, MD
Click here to contact Amal Mattu, MD
The nitrite test on urine dipstick is commonly used for diagnosis of UTI. However, the test is only reliable in those bacteria that convert nitrates to nitrites, which primarily includes enterobaceriaceae. However, elderly patients often develop UTIs with Staph saprophyticus, pseudomonas, and enterococcus, none of which produce positive nitrites on dipstick testing. The takeaway point here is very simply....don't assume you've excluded UTI (esp. in elderly populations) just because the nitrite test is negative.
reference: Anderson RS, Liang SY. Infections in the elderly. Critical Decisions in Emergency Medicine, April 2010.
Category: Dermatology
Keywords: Toxicodendron dermatitis, treatment (PubMed Search)
Posted: 6/19/2010 by Michael Bond, MD
(Updated: 5/17/2026)
Click here to contact Michael Bond, MD
Toxicodendron dermatitis:
This is the contact dermatitis caused by the plant genus Toxicodendronm, better known as Poison Ivy. Here are some types to prevent the dermatitis and how to treat it:
Category: Neurology
Keywords: nicardipine, calcium channelblocker, hypertensive emergency, intracranial hemorrhage, hypertension, stroke (PubMed Search)
Posted: 6/16/2010 by Aisha Liferidge, MD
(Updated: 5/17/2026)
Click here to contact Aisha Liferidge, MD
Category: Critical Care
Posted: 6/15/2010 by Mike Winters, MBA, MD
(Updated: 5/17/2026)
Click here to contact Mike Winters, MBA, MD
Hypotension after intubation and initiation of mechanical ventilation
Manthous CA. Avoiding circulatory complications during endotracheal intubation and initiation of positive pressure ventilation. JEM 2010; 38:622-31.
Category: Misc
Posted: 6/14/2010 by Rob Rogers, MD
(Updated: 5/17/2026)
Click here to contact Rob Rogers, MD
Submitted on behalf of Dr. Michael Abraham
Thyrotropin (TSH)
1. Spencer CA, Takeuchi M, Kazarosyan M. Current status and performance goals for serum thyrotropin (TSH) assays. Clin Chem. Jan 1996;42(1):140-145.
2. Liebert M. Thyrotropin/Thyroid Stimulating Hormone (TSH) Measurement. Http://www.medscape.com/
Category: Cardiology
Keywords: pericardial effusion, tamponade (PubMed Search)
Posted: 6/13/2010 by Amal Mattu, MD
(Updated: 5/17/2026)
Click here to contact Amal Mattu, MD
Pericardial tamponade is a physiological diagnosis, not an ECG diagnosis. At best, the ECG can suggest the presence of large pericardial effusions--look for the combination of low voltage, tachycardia, and electrical alternans.
Be aware, however, that electrical alternans is only present in < 1/3 of patients with large pericardial effusions. Although it is "classic" and always seems to show up on board exams, in the textbooks, and in lectures, electrical alternans in not a consistent finding in patients with large effusions or tamponade.
Category: Orthopedics
Keywords: Calcaneus Fracture, Bohler Angle (PubMed Search)
Posted: 6/13/2010 by Michael Bond, MD
Click here to contact Michael Bond, MD
Calcaneus Fractures:
Calcaneus fractures can easily be missed on plain films and the true extent of the injury might not be appreciated until a CT is done. However, you can increase your change of picking up a calcaneal fracture by evaluating Bohler's Angle.
Lateral radiographs of the foot are needed to evaluate the Bohler angle. This is the angle made by drawing a line from anterior process of the calcaneus to the peak of the posterior articular surface and a second one drawn from the peak of the posterior articular surface to the peak of the posterior tuberosity. (See Picture) The average angle is 25-40°. Angles less than 25' are strongly suggestive of a fracture and the patient should probably get a CT of their foot if there is clinical suspicion.
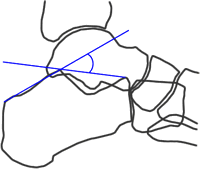
Photo and additional discussion can be found at http://www.blackburnfeet.org.uk/hyperbook/trauma/calcanealFx/imaging.htm and on eMedicine -- Calcaneus Fractures by Scott Nicklebur, MD http://emedicine.medscape.com/article/1232246-overview
Category: Pediatrics
Keywords: Pediatric Burns, Fire, Injury, Burn Injuries, Sage Diagram, TBSA (PubMed Search)
Posted: 6/11/2010 by Adam Friedlander, MD
(Updated: 5/17/2026)
Click here to contact Adam Friedlander, MD
Current American Burn Association guidelines state that any child with a greater than 10% total body surface area (TBSA) burn should be admitted to a center capable of caring for pediatric burns, rather than being discharged after wound management. However, physician use of TBSA% estimation techniques is variable. An excellent free tool for estimating TBSA is available online, allows for automatic weight based calculation, and allows printing of your diagram. The diagram is available at http://www.sagediagram.com/. More to come...
Category: Toxicology
Keywords: physostigmine, anticholinergic (PubMed Search)
Posted: 6/10/2010 by Bryan Hayes, PharmD
(Updated: 5/17/2026)
Click here to contact Bryan Hayes, PharmD
Physostigmine has been used extensively in the fields of anesthesiology and emergency medicine. The only use of physostigmine with sound scientific support is for the management of patients with an anticholinergic syndrome, particularly those without cardiovascular compromise who have an agitated delirium. In this population, physostigmine has an excellent risk-to-benefit profile.
Category: Neurology
Keywords: lumbar puncture, LP, spinal tap (PubMed Search)
Posted: 6/9/2010 by Aisha Liferidge, MD
(Updated: 5/17/2026)
Click here to contact Aisha Liferidge, MD
Once you've punctured the spinal canal space during lumbar puncture, the following tips can be used to improve the rate of cerebrospinal fluid (CSF) flow, should it be suboptimal:
Category: Critical Care
Posted: 6/8/2010 by Mike Winters, MBA, MD
(Updated: 5/17/2026)
Click here to contact Mike Winters, MBA, MD
Platelet Transfusions in the Critically Ill
Netzer G, Hess JR, Shanholtz C. Use of blood products in the intensive care unit: Concepts and controversies. Contemporary Critical Care June 2010;8(1):1-12.
Category: Vascular
Keywords: Pulmonary Embolism (PubMed Search)
Posted: 6/7/2010 by Rob Rogers, MD
(Updated: 5/17/2026)
Click here to contact Rob Rogers, MD
Thrombolytic Therapy for Pulmonary Embolism
Current, FDA-approved thrombolytic therapy for PE:
Category: Geriatrics
Keywords: geriatrics, elderly, appendicitis (PubMed Search)
Posted: 6/7/2010 by Amal Mattu, MD
(Updated: 5/17/2026)
Click here to contact Amal Mattu, MD
Up to 25% of elderly patients with appendicitis are initially sent home from the ED, an indication of the high misdiagnosis rate for appendicitis in the elderly population. Why are elderly patients so often misdiagnosed when they have appendicitis? The answer is simple....they present very atypically.
Expect the atypical in elderly patients!
Category: Orthopedics
Keywords: Wound Care, Antiseptics (PubMed Search)
Posted: 6/5/2010 by Michael Bond, MD
Click here to contact Michael Bond, MD
Wound Care:
Patients and many providers want to irrigate or wash a wound with an antiseptic solution in order to decrease the risk of infection. Most studies have shown that irrigation whether with tap water or sterile water is effective enough in reducing bacterial counts in a wound so does adding an antiseptic solution offer any additional benefit.
It turns out that hydrogen peroxide, and iodine based solutions can actually hinder wound healing as they causes delays in the migration and proliferation of fibroblasts at concentrations that are not even bactericidal. Chlorhexidine, and silver containing antiseptics [i.e.: silver sulfadiazine and silver nitrate] are bactericidal at concentrations that do not affect fibroblasts.
So in the end, if you feel the need to use an antiseptic, use chlorhexidine or a silver containing antiseptic. The use of hydrogen peroxide and iodine based solutions should be abandoned as they are not even bactericidal at concentrations that have profound affects on the fibroblasts.
Thomas, GS. Mechanisms of Delayed Wound Healing by Commonly Used Antiseptics. J Trauma 2009; 66:82-91
Category: Toxicology
Keywords: pediatrics, toxicology, antidepressant, antimalarial, antipsychotic, calcium channel, aspirin (PubMed Search)
Posted: 6/4/2010 by Ellen Lemkin, MD, PharmD
(Updated: 5/17/2026)
Click here to contact Ellen Lemkin, MD, PharmD
There are a several classes of medications that can kill a toddler with a single dose. Toddlers are particularly susceptible due to their low weights and propensity to place everything in their mouths.
1. Calcium channel blockers
2. Camphor-containing rubs
3. Opioids/opiates
4. Oil of wintergreen/ aspirin
5. Cyclic antidepressants
6. Topical blood pressure patches (clonidine)
7. Eye drops and nasal sprays (oxymetazoline)
8. Sulfonylureas
9. Antimalarial drugs (cloroquine)
1. Morris-Kukowski, C. England AG. Toxicity, Deadly in a Single Dose. Emedicine, Pediatrics.
