Category: Trauma
Keywords: TBI, management, parameters (PubMed Search)
Posted: 7/20/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Outcomes in traumatic brain injury are improved when physiologic homeostasis is achieved as soon as possible after injury. Here are the American College of Surgeons’ recommendations. Note SBP over 110 and a hemoglobin over 7. A study looking at a more liberal transfusion target showed worse ARDS and no mortality benefit.
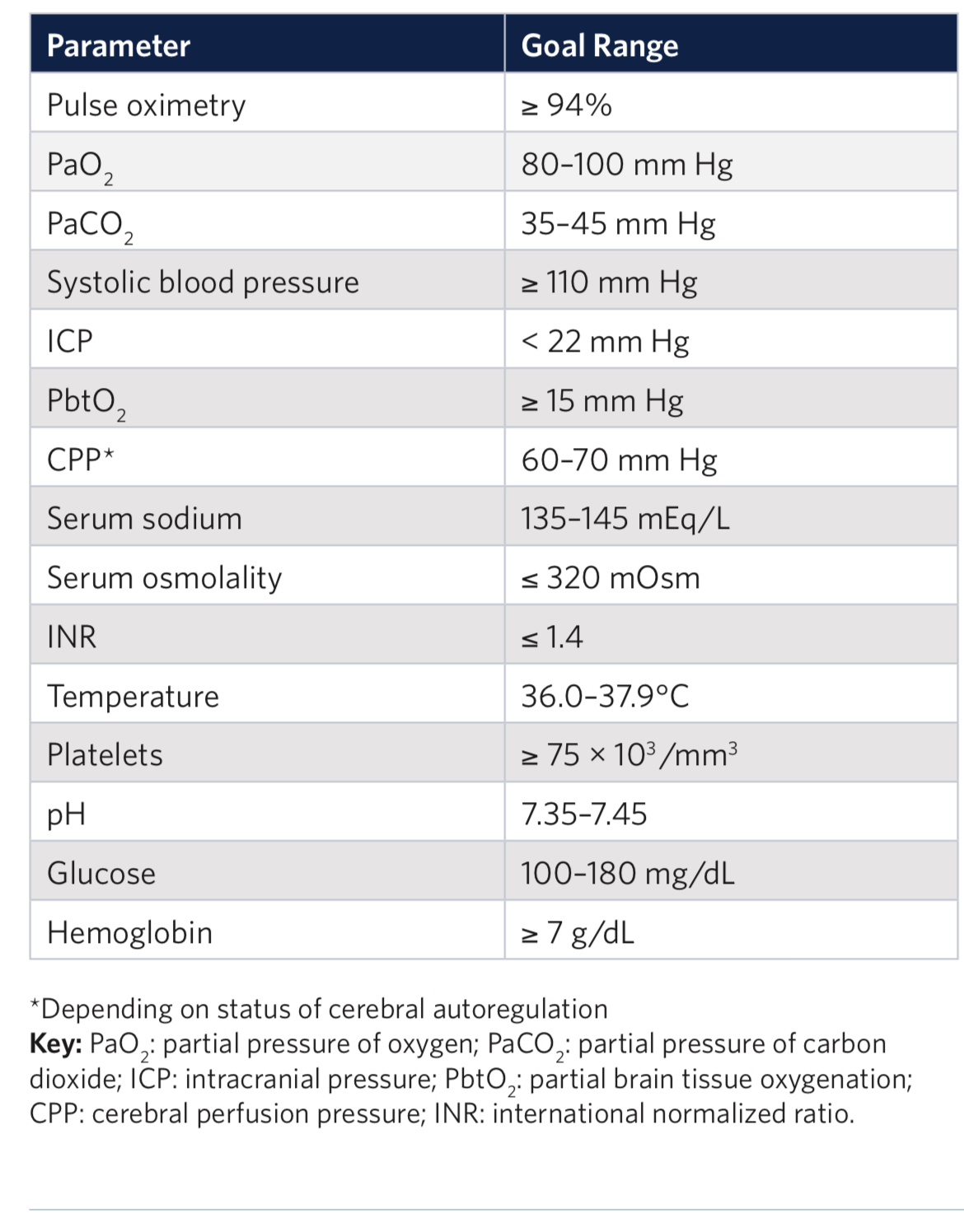
2. Liberal or Restrictive Transfusion Strategy in Patients with Traumatic Brain Injury
Authors: Alexis F. Turgeon, M.D. https://orcid.org/0000-0001-5675-8791, Dean A.Fergusson, Ph.D., Lucy Clayton, M.Sc., Marie-Pier Patton, M.Sc., Xavier Neveu, M.Sc., Timothy S. Walsh, M.D., Annemarie Docherty, M.D., Ph.D., +48 , for the HEMOTION Trial Investigators on behalf of the Canadian Critical Care Trials Group, the Canadian Perioperative Anesthesia Clinical Trials Group, and the Canadian Traumatic Brain Injury Research Consortium*
June 13, 2024N Engl J Med 2024;391:722-735DOI: 10.1056/NEJMoa2404360VOL. 391 NO. 8
Category: Geriatrics
Keywords: Geriatric, critical care, vasopressors. (PubMed Search)
Posted: 7/12/2025 by Robert Flint, MD
(Updated: 7/14/2025)
Click here to contact Robert Flint, MD
An open label pragmatic study in 29 Japanese hospitals randomized septic shock patients over age 65 to either a high (MAP 80-85) or control (65-70) group. They then looked at all cause 90 day mortality. The study was stopped early due to a significantly higher percentage of mortality in the higher MAP group.
The study isn’t blinded and is only done in one country, however it does raise the question of what is the ideal MAP for older septic shock patients.
Endo A, Yamakawa K, Tagami T, Umemura Y, Wada T, Yamamoto R, Nagasawa H, Takayama W, Yagi M, Takahashi K, Kojima M, Narita C, Kazuma S, Takahashi J, Shiraishi A, Todani M, Nakane M, Nagata T, Tanaka S, Yokokawa Y, Takahashi K, Ishikita H, Hisamune R, Sasaki J, Muramatsu KI, Sonobe H, Minami K, Hoshi H, Otomo Y; OPTPRESS trial investigators. Efficacy of targeting high mean arterial pressure for older patients with septic shock (OPTPRESS): a multicentre, pragmatic, open-label, randomised controlled trial. Intensive Care Med. 2025 May;51(5):883-892. doi: 10.1007/s00134-025-07910-4. Epub 2025 May 13. PMID: 40358717; PMCID: PMC12130109.
Category: Trauma
Keywords: Pedestrian, fatality, injury, cyclist (PubMed Search)
Posted: 7/12/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This study from Great Britain compared fatalities for pedestrians and cyclist struck by motor vehicles based on vehicle body type. They found :
“We conclude that in Great Britain, being hit by an SUV as opposed to a passenger car increases injury severity among pedestrians and cyclists, with the strongest effect in children.“
Goodman, Anna, Phil Edwards, and Anthony A. Laverty. 2025. “Do Sports Utility Vehicles (SUVs) Cause More Severe Injuries to Pedestrians and Cyclists than Passenger Cars, in the Case of a Crash? Findings from Great Britain, 2004-2023.” Findings, July. https:/?/?doi.org/?10.32866/?001c.141647.
Category: Geriatrics
Keywords: Age friendly, geriatric, healthcare, quality improvement (PubMed Search)
Posted: 7/6/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
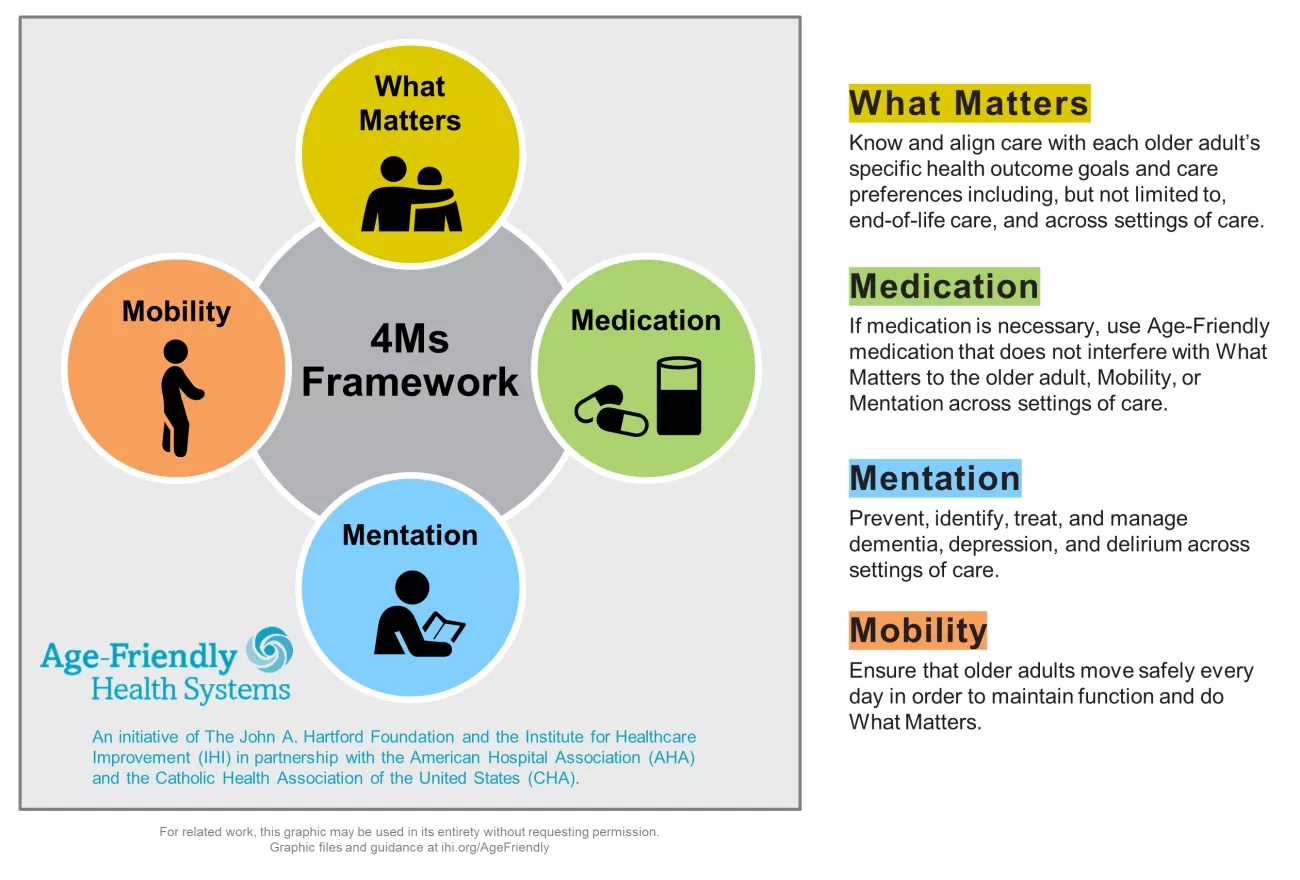
In mid-2024 the Center for Medicare and Medicaid Services introduced a new quality measure entitled Age Friendly Hospital Measure. The initial phase went into effect 1/1/25. It is built around programs from the American College of Surgeons, the American College of Emergency Physicians as well as the Institute for Healthcare Improvement (IHI). It is modeled around the IHI’s 4M Framework.
Category: Trauma
Keywords: Shock index, transfusion, hypotension (PubMed Search)
Posted: 7/5/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
These authors looked at 5958 trauma patients arriving at their trauma center with a systolic blood pressure greater than 90. They calculated shock index (heart rate /sbp) for all of these and then looked at who received a blood transfusion within one hour of arrival. 211 patients received blood in that time frame. “Patients were stratified by SI using the following thresholds: ? 0.7, > 0.7 to 0.9, > 0.9 to 1.1, > 1.1 to 1.3, and > 1.3.”
“A main effect was observed for shock index with increased risk for required transfusion for patients with admission shock index >0.7 (P < 0.001). In comparison to shock index of ? 0.7, odds ratios were 2.5(1.7 - 3.8), 8.2(5.4 - 12.2), 24.9(15.1 - 41.1), 59.0(32.0 - 108.6) for each categorical increase in SI.”
Lin TM, Memon AM, Reeson EA, Tolan GC, Low TM, Kupanoff KM, Huang DD, Jones MD, Czarkowski BR, Soe-Lin H, Bogert JN, Weinberg JA. Shock index identifies compensated shock in the 'Normotensive' trauma patient. Injury. 2025 May 8:112419. doi: 10.1016/j.injury.2025.112419. Epub ahead of print. PMID: 40379507.
Category: Trauma
Keywords: facial fracture, transfer, guidelines (PubMed Search)
Posted: 6/29/2025 by Robert Flint, MD
(Updated: 7/2/2025)
Click here to contact Robert Flint, MD
Based on a review of 511 patients transferred to a level one trauma center for evaluation of facial fractures, this group developed the Facial Fracture Transfer Guidelines. they found that over half of the patients transferred to them did not require intervention and were discharged within 6 hours. These guidelines are meant to decrease unneeded transfers yet provide appropriate care to those with traumatic facial injuries.
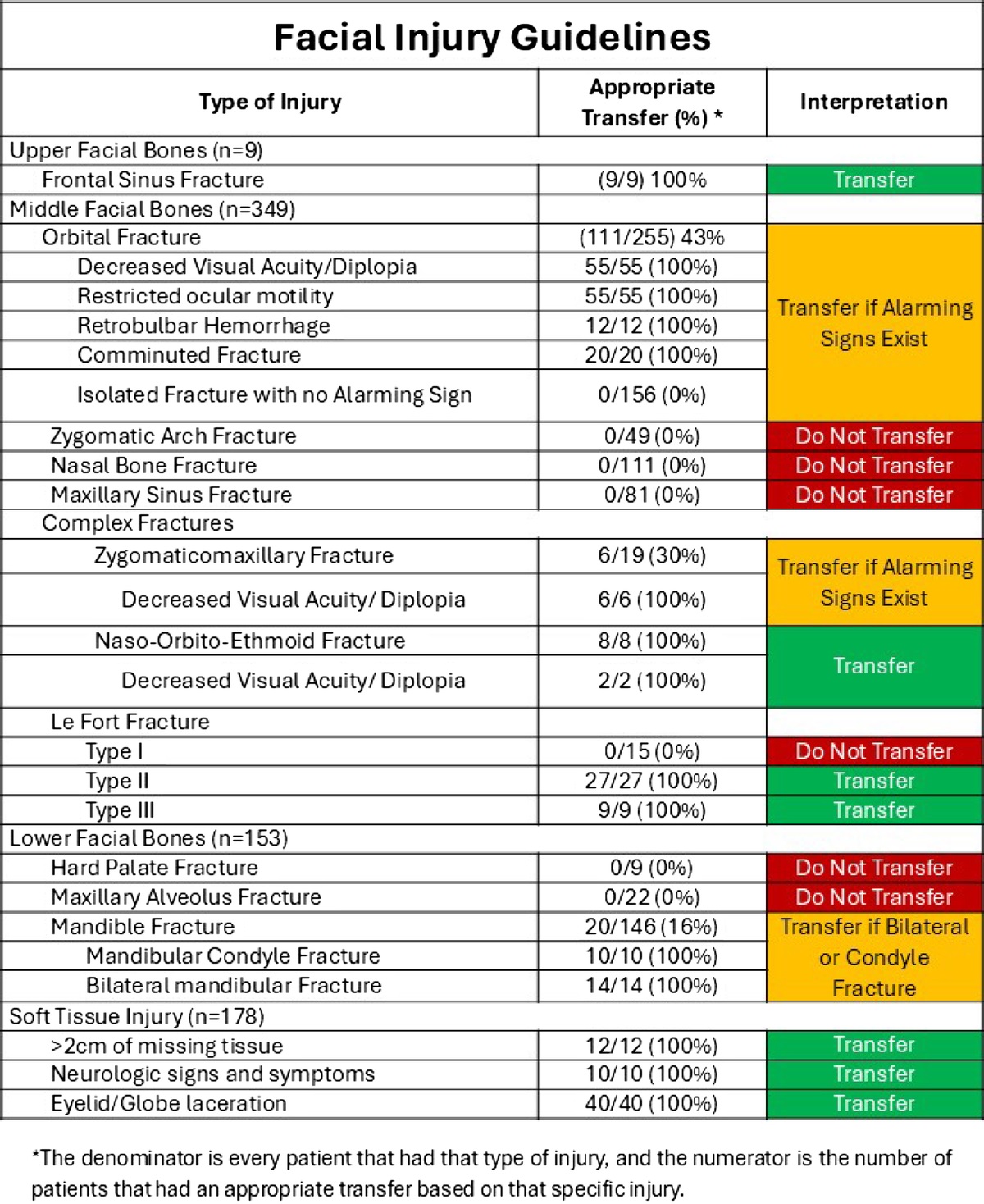
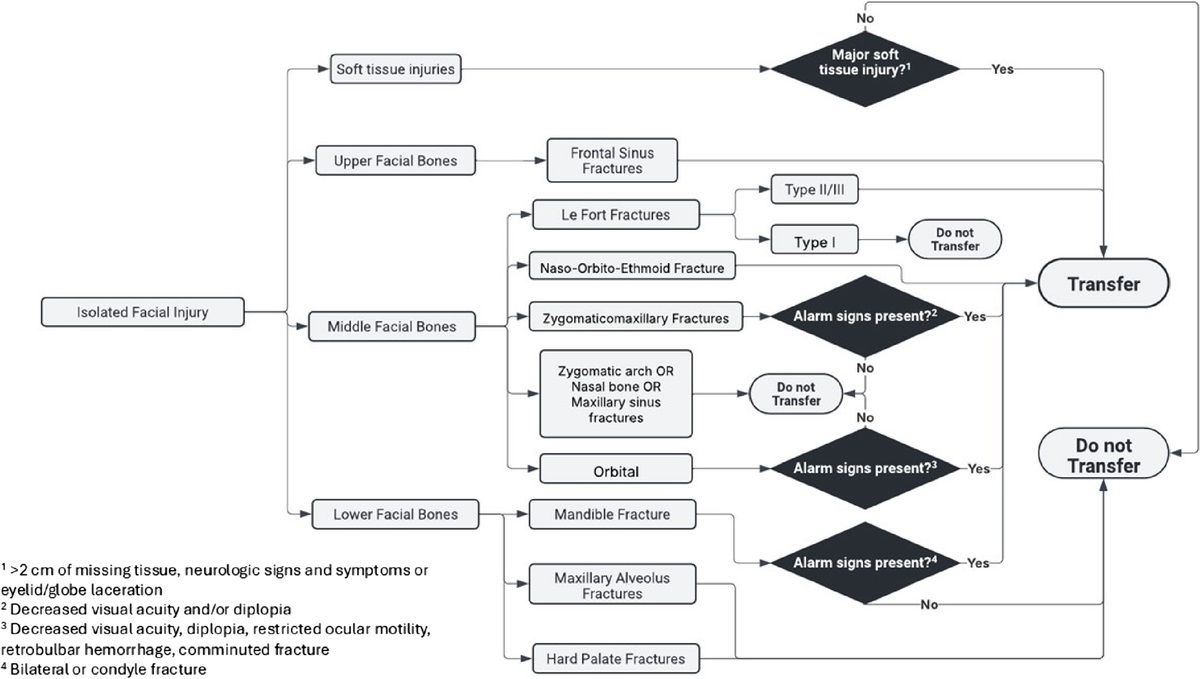
Castillo Diaz, Francisco MD; Anand, Tanya MD, MPH, FACS; Khurshid, Muhammad Haris MD; Kunac, Anastasia MD, FACS; Al Ma'ani, Mohammad MD; Colosimo, Christina DO, MS, FACS; Hejazi, Omar MD; Ditillo, Michael DO, FACS; Magnotti, Louis J. MD, MS, FACS; Joseph, Bellal MD, FACS. Look me in the face and tell me that I needed to be transferred: Defining the criteria for transferring patients with isolated facial injuries. Journal of Trauma and Acute Care Surgery ():10.1097/TA.0000000000004651, May 9, 2025. | DOI: 10.1097/TA.0000000000004651
Category: Trauma
Keywords: facial fracture, Le Fort, orbital fracture (PubMed Search)
Posted: 6/29/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Most common facial fracture is the nasal fracture followed by the zygomatic arch fractures.
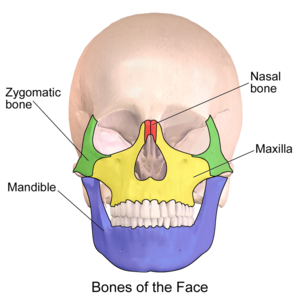
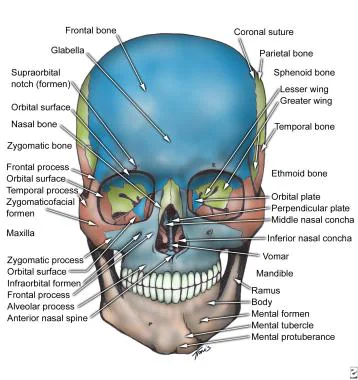
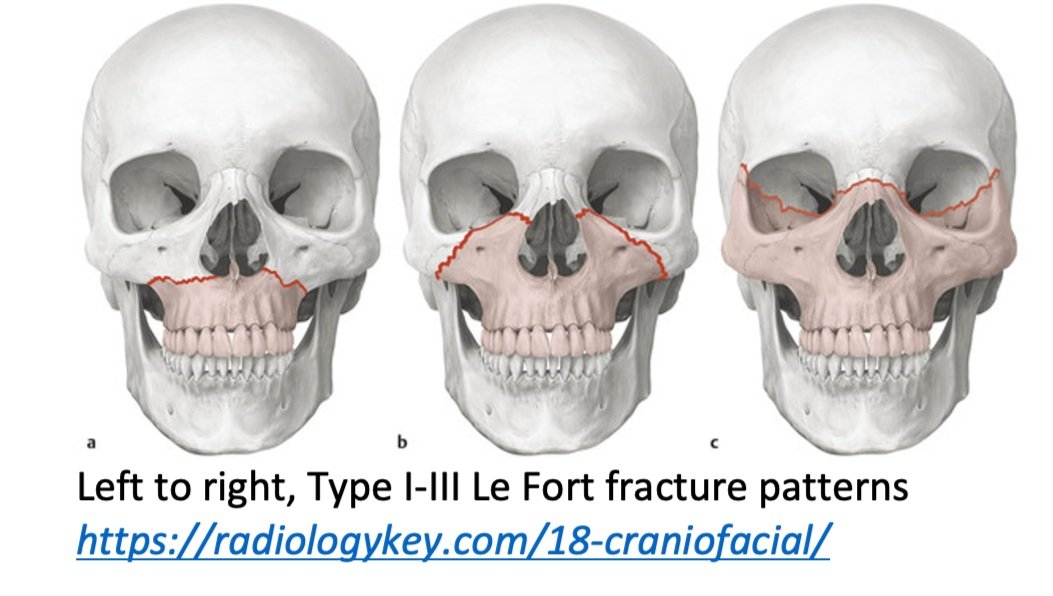
Le Fort Classification of facial fractures/facial stability. The higher the number, the more unstable.
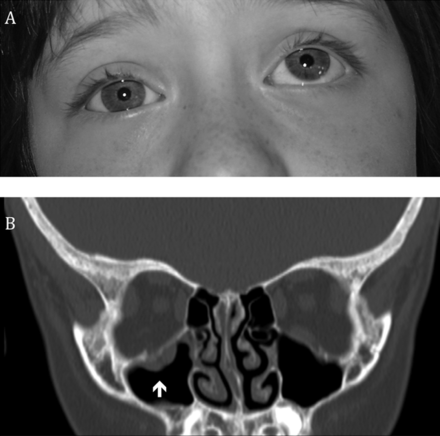
Orbital blow out fractures may entrap the ocular muscles leading to eye immobility in various directions.
Category: Trauma
Keywords: Head injury, BIG, pediatric (PubMed Search)
Posted: 6/23/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Brain injury guidelines were designed to decrease transfers and neurosurgical consults for adults with head injuries.
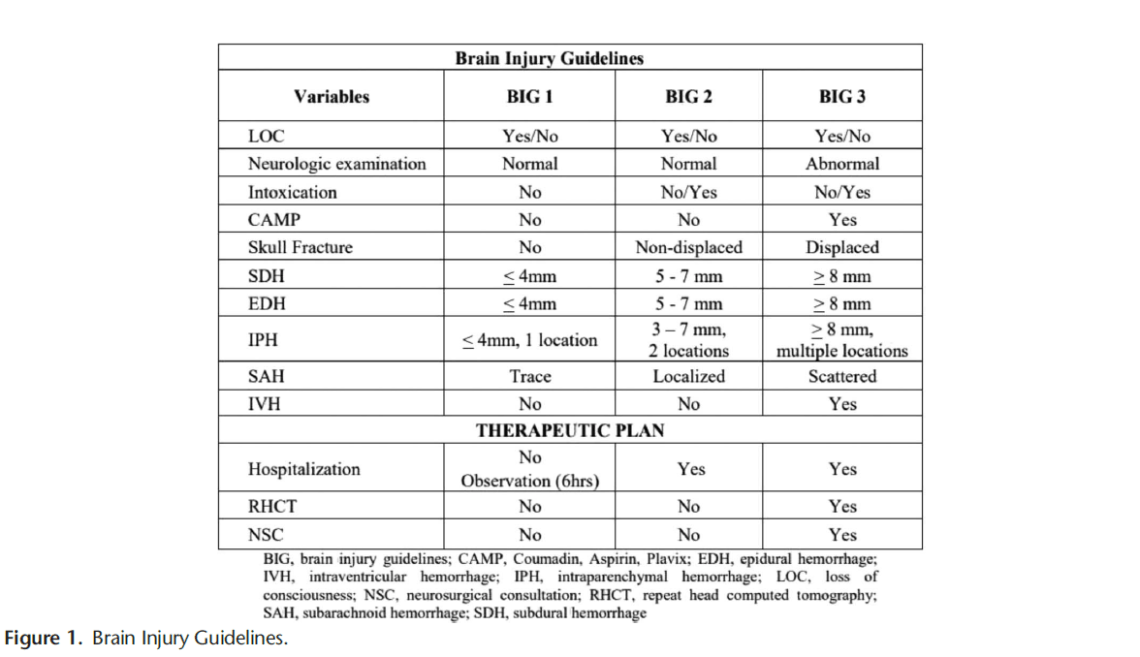
A new retrospective study suggests that modified guidelines may be feasible in the pediatric population as well. More data is needed but this is an important step in assuring safe resource utilization in pediatric head injury patients.
1. https://first10em.com/the-brain-injury-guidelines-can-we-avoid-talking-to-neurosurgeons/
2. Kay AB, Glasgow SL, Kahan AM, Swendiman RA, Kastenberg ZJ, Roach CM, Wan HY, Bollo RJ, Iyer RR, Ravindra VM, Morris DS, Yorkgitis BK, Joseph B, Russell KW. Small Change, BIG Impact: Proposal of the Brain Injury Guidelines for kids (kBIG). J Pediatr Surg. 2025 May 17;60(8):162372.
Category: Infectious Disease
Keywords: Abscess, brain, drainage, neurosurgery (PubMed Search)
Posted: 6/22/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
In a Danish study of 558 patients with a brain abscess, those that had early surgical drainage did better than those treated conservatively with antibiotics only. Prompt neurosurgical consultation is warranted for these patients.
Category: Trauma
Keywords: Intubation, trauma, mortality, operating room, Ed (PubMed Search)
Posted: 6/15/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
In this Israeli study comparing mortality for trauma patients intubated in the emergency department vs the operating room, in hospital mortality was higher for the ED group before controlling for injury severity score and shock. After controlling for injury severity and shock, there was no difference in In hospital mortality. Coupled with previous research, if intubation can wait until after resuscitation and in the OR, that is ideal. And sometimes it just has to happen in the ED and we should be prepared for rapid resuscitation.
Talmy T, Radomislensky I, Brzezinski Sinai I, Shaylor R, Katorza E, Gendler S; Israel Trauma Group Collaborators. Intubation Setting and Mortality in Trauma Patients Undergoing Hemorrhage Control Surgery: A Propensity Score-Matched Analysis. Anesth Analg. 2025 May 16. doi: 10.1213/ANE.0000000000007542. Epub ahead of print. PMID: 40378073.
Category: Trauma
Keywords: Hysterotomy (PubMed Search)
Posted: 6/8/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Another case series of 3 resuscitative hysterotomies, all performed by obstetricians, reported 33% maternal and 67% neonate survival.(1).
The mechanics of the procedure are:
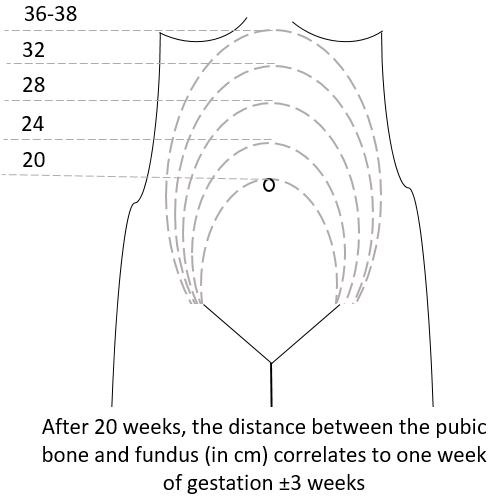
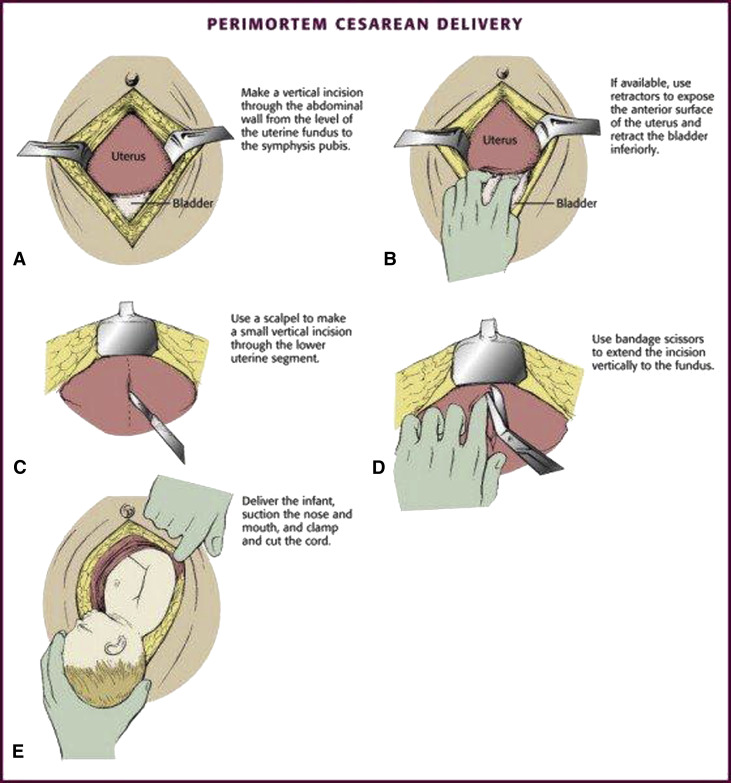
(3)
Category: Trauma
Posted: 6/7/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
A literature search revealed very little evidence, however in 66 women and 68 neonates who underwent resuscitative hysterotomy for out of hospital cardiac arrest 4.5% of women and 45% of neonates survived to discharge. The longest down time was 29 minutes and 47 minutes for women and neonates respectively. While more evidence is needed, it appears this procedure should be performed as early as possible and may lead to some survival benefit.
Leech C, Nutbeam T, Chu J, Knight M, Hinshaw K, Appleyard TL, Cowan S, Couper K, Yeung J. Maternal and neonatal outcomes following resuscitative hysterotomy for out of hospital cardiac arrest: A systematic review. Resuscitation. 2025 Feb;207:110479. doi: 10.1016/j.resuscitation.2024.110479. Epub 2024 Dec 29. PMID: 39736393.
Category: Trauma
Keywords: Femur fracture, splint (PubMed Search)
Posted: 6/6/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
The National Association of Emergency Medical Service Physicians reminds us that femur fractures rarely cause enough blood loss to cause hemodynamic instability (look for other sources), often have concomitant injuries in the pelvis or distal extremity, and can be effectively splinted either static or with traction (which has contraindications, complications, and technical hurdles).
John W. Lyng, Joshua G. Corsa, Philip S. Nawrocki, Brad D. Raetzke, Josh
Nackenson & Nichole Bosson (07 May 2025): Prehospital Trauma Compendium: Management
of Suspected Femoral Shaft Fractures – A position statement and resource document of
NAEMSP, Prehospital Emergency Care, DOI: 10.1080/10903127.2025.2493846
To link to this article: https://doi.org/10.1080/10903127.2025.2493846
Category: Trauma
Keywords: Nail gun injury, surgery, antibiotics (PubMed Search)
Posted: 5/31/2025 by Robert Flint, MD
(Updated: 6/1/2025)
Click here to contact Robert Flint, MD
An Australian retrospective study of 158 patients treated for nail gun injuries found those treated with operative debridement or with prophylactic antibiotics had no different 30 day infection rates compared to patients receiving no antibiotics.
Slater S, Vasudeva M, Mitra B, Sreedharan S. Penetrating nail gun injuries: Role of antibiotics and surgical management. Trauma. 2025;0(0). doi:10.1177/14604086251320524
Category: Trauma
Keywords: geriatric, trauma, CT scan (PubMed Search)
Posted: 5/29/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This literature search from 1946-2023 looking at comparing selective use of CT scans vs whole body scans in geriatric trauma found no benefit of whole body CT in mortality, hospital length of stay or ED discharge. This study only included 15,000 pts over that very long time line. More robust, current work needs to be done on this important topic.
Tang P, Elkington O, Stevens S. Whole body CT-scan vs. selective CT-scan in geriatric trauma: Systematic review and meta-analysis. Trauma. 2025;0(0). doi:10.1177/14604086241304629
Category: Infectious Disease
Keywords: Coccidioidomycosis, climate change (PubMed Search)
Posted: 5/26/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Typically Coccidioidomycosis is seen in the Southwestern US. The authors of this study, using climate modeling predict endemic areas will spread across the US to include Idaho, the Dakotas, Nebraska and Wyoming.
Clinically, “Patients with pulmonary Coccidioides infection frequently experience fever, cough, and shortness of breath. Chest radiographic imaging may demonstrate lobar, segmental, or multifocal consolidations; cavitary lesions; and lung nodules. Given these nonspecific findings, patients with coccidioidomycosis are often treated for community-acquired pneumonia. Coccidioidomycosis should be considered in patients not improving with antibiotic treatment or in those who have exposure to or reside in endemic areas. Up to 50% of patients with pulmonary coccidioidomycosis have erythema nodosum, approximately 25% to 30% have peripheral eosinophilia, and approximately 25% have arthralgias (particularly symmetric knee and ankle arthralgia). Up to 10% of patients diagnosed with coccidioidomycosis develop disseminated disease, including skin, central nervous system, and bone and joint infection.”
Lee PS, Swain DL, Johnson R. Climate Change and Coccidioidomycosis. JAMA. 2025;333(11):997–998. doi:10.1001/jama.2024.27274
Category: Neurology
Keywords: CVA, TIA, prediction, one year (PubMed Search)
Posted: 5/21/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
How likely is your TIA pt to go on to have a stroke? This study in JAMA gives us some answers. While EM providers aren’t as interested in 5 and 10 year prediction, it provides more evidence TIAs need to be evaluated and are risk factors for future events.
“In this systematic review and meta-analysis of 171?068 patients with TIA or minor stroke from 38 studies, the risk of subsequent stroke was 5.9% within 1 year, 12.8% within 5 years, and 19.8% within 10 years.”
Category: ENT
Keywords: Epistaxis prophylaxis (PubMed Search)
Posted: 5/18/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This large retrospective database study compared those receiving antibiotics after anterior nasal packing to those that did not. There was no difference in clinically significant infection between the groups leading the authors to conclude prophylactic antibiotics after anterior nasal packing is not required.
Tran QK, Vashee I, Vanga R, Camp S, Rallo MK, Najafali D, Bontempo LJ, Pourmand A. Is antibiotic prophylaxis necessary for anterior epistaxis with packing? Insights from a large database. Am J Emerg Med. 2025 Mar 19;93:64-72. doi: 10.1016/j.ajem.2025.03.040. Epub ahead of print. PMID: 40147155.
Category: Trauma
Keywords: Incarcerated, trauma, mortality, disparity (PubMed Search)
Posted: 5/11/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Looking at a year’s worth of data from the National Trauma Databank, the authors found incarcerated trauma patients were more likely to be stabbed, male, persons of color and have a higher adjusted mortality rate.
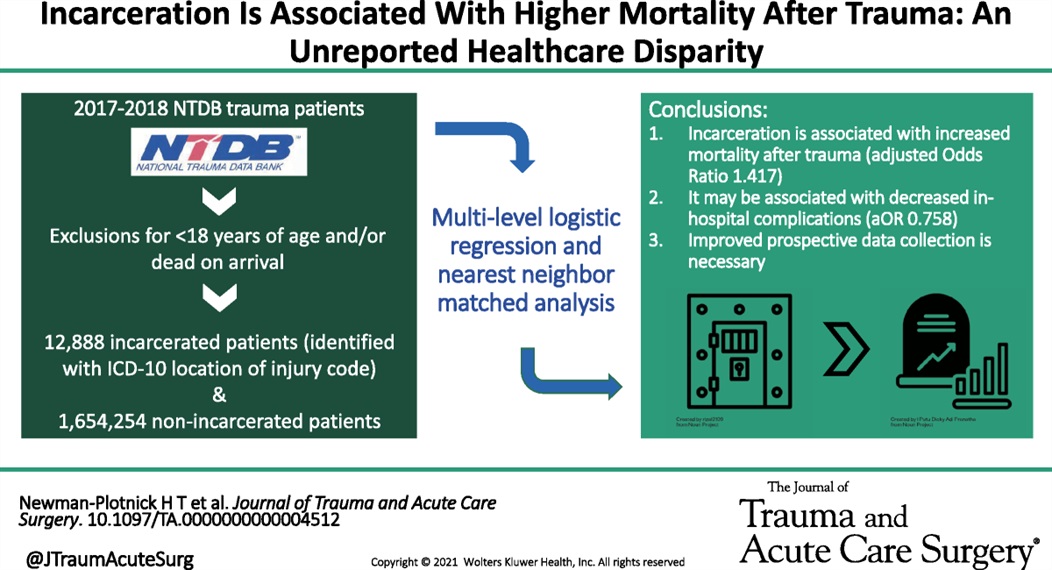
Newman-Plotnick, Harry MD, MPH; Byrne, James P. MD, PhD; Haut, Elliott Richard MD, PhD, FACS; Hultman, Charles Scott MD, MBA, FACS
Journal of Trauma and Acute Care Surgery 98(5):p 785-793, May 2025. | DOI: 10.1097/TA.0000000000004512
Category: Orthopedics
Keywords: Hip fractures, geriatrics, complications (PubMed Search)
Posted: 5/7/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This article reminds us that hip fractures have a one year mortality rate of 12-25% and 50% of hip fracture patients develop complications while in the hospital. “Almost half of individuals hospitalized with hip fractures experience complications, such as delirium, pneumonia, acute kidney injury, urinary tract infection, and deep vein thrombosis”
Because of these complications, multidisciplinary teams should be caring for these patients and great care should be exercised when evaluating these patients.
JAMA Insights
March 24, 2025
Yiju Teresa Liu, MD1,2; Eva Tovar Hirashima, MD, MPH3; Kabir Yadav, MDCM, MS, MSHS1,4
JAMA. Published online March 24, 2025. doi:10.1001/jama.2025.0999
