Category: Pediatrics
Keywords: Nail bed injuries, wound closure (PubMed Search)
Posted: 1/20/2017 by Jenny Guyther, MD
(Updated: 5/25/2026)
Click here to contact Jenny Guyther, MD
More studies are needed, but the existing data shows that medical adhesives may be quicker without impacting cosmetic and functional outcome.
Nail bed injuries occur in 15-24% of children with fingertip injuries.
In 1997, medical adhesive was first used to secure the avulsed nail plate back to the nail bed instead of suturing back into place. By 2008, there were small studies looking at the utility of using medical adhesive to close the laceration of the nail bed. The studies were small, but there was a tendency towards shorter repair times and no difference between pain, cosmetic outcome or function.
A total of 6 articles were included in this review – 2 using histoacryl and 4 using demabond.
Edwards, S, Parkinson L. Is Fixing Pediatric Nail Bed Injuries with Medical Adhesives as Effective as Suturing? A Review of the Literature. Pediatric Emergency Care. 2016.
Category: Pediatrics
Posted: 12/31/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
In pediatrics, providers typically prescribe 10 mg/kg (max 500 mg) and 5 mg/kg daily x 4 (max 250 mg) for treatment of pneumonia, but this dosing regimen is NOT recommended for all azithromycin usage. There are other dosing regimens that are important to keep in mind during the respiratory season:
1) Pharyngitis/ tonsillitis (ages 2-15 yr): 12 mg/kg daily x 5 days (max 500 mg/ 24 hr)
2) Pertussis
3) Acute sinusitis >/= 6 months: 10 mg/kg daily x 3 days
Tschudy MM, Arcara KM. The Harriet Lane Handbook 19th edition. Elsevier Mosby; 2012
Category: Pediatrics
Keywords: fever, diarrhea, urinary tract infection (PubMed Search)
Posted: 12/16/2016 by Jenny Guyther, MD
(Updated: 5/25/2026)
Click here to contact Jenny Guyther, MD
After 4 months old, the answer MAY be no.
80 children between 4 months and 6 years of age with fever > 101 degress F and watery stools (> 3 episodes) were evaluated for hydration status using urine samples. The urine was collected either by catheterization or clean catch, depending on age. All urine cultures were negative.
Nibhanipudi KV. A Study to determine the Incidence of Urinary Tract Infections in Infants and Children Ages 4 months to 6 Years with Febrile Diarrhea. Glob Pediatr Health. 2016. Published online Sept 12, 2016.
Category: Pediatrics
Keywords: septic shock, cold shock, vasopressor, dopamine, epinephrine (PubMed Search)
Posted: 11/25/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Which first-line vasoactive drug is the best choice for children with fluid-refractory septic shock? A prospective, randomized, blinded study of 120 children compared dopamine versus epinephrine in attempts to answer this debated question in the current guidelines for pediatric sepsis.
Bottom line: Dopamine was associated with an increased risk of death and healthcare–associated infection. Early administration of peripheral or intraosseous epinephrine was associated with increased survival in this population.
This was a small double-blind, prospective randomized controlled trial of 120 children with fluid-refractory septic shock in a PICU in Brazil. The primary outcome was to compare the effects of dopamine or epinephrine in severe sepsis on 28-day mortality; secondary outcomes were the rate of healthcare–associated infection, the need for other vasoactive drugs, and the multiple organ dysfunction score. Dopamine was associated with death (OR, 6.5; 95% CI, 1.1–37.8; p = 0.037) and healthcare–associated infection (odds ratio, 67.7; 95% CI, 5.0–910.8; p = 0.001). The use of epinephrine was associated with a survival odds ratio of 6.49. Further multicenter trials or single-center studeis are necessary to verify the reproducibiltiy of these results.
Ramaswamy KN, Singhi S, Jayashree M, Bansal A, Nallasamy K. Double-Blind Randomized Clinical Trial Comparing Dopamine and Epinephrine in Pediatric Fluid-Refractory Hypotensive Septic Shock.Pediatr Crit Care Med. 2016 Nov;17(11):e502-e512.
Category: Pediatrics
Keywords: Ketamine, conscience sedation, pharmacology, pediatrics (PubMed Search)
Posted: 11/18/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Using 1.5 mg/kg or 2 mg/kg of IV ketamine led to less redosing compared to using 1 mg/kg IV.
This was a prospective, double blinded, randomized controlled trial of children 3-18 years. 125 children were included in the study. They compared 1mg/kg, 1.5 mg/kg and 2 mg/kg doses. All doses were IV. Adequate sedation was achieved with all 3 doses of ketamine, and there was no increased risk of adverse events with the higher doses. However, using 1.5mg/kg or 2 mg/kg required less redosing.
Previous studies suggested a higher risk of adverse events if the initial dose was greater than 2.5 mg/kg or the total dose was more than 5 mg/kg.
Kannikeswaran et al. Optimal dosing of intravenous ketamine for procedural sedation in children in the ED – a randomized control trial. American Journal of Emergency Medicine 24 (2016) 1347-1353.
Category: Pediatrics
Keywords: sickle cell, acute chest syndrome, pneumonia (PubMed Search)
Posted: 10/28/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Typically, empiric treatment for lobar community acquire pneumonia (CAP) in immunized < 5 year olds (preschool) is amoxicillin (45mg/kg BID or 30 mg/kg TID for resistant S. pneumoniae) for outpatient and ampicillin or ceftriaxone for inpatient. Additional coverage with azithromycin is typically recommended for school age and adolescent patients (>= 5 years), but not necessarily for younger children unless there is a particular clinical suspicion for atypical pneumonia with history, xray findings, or sick contacts.
However, in sickle cell patient with suspicion for acute chest syndrome, azithromycin is recommended for all ages groups, as atypical bacteria such as Mycoplasma are a common cause of acute chest syndrome in patients of all ages with sickle cell disease even young children. In a prospective series of 598 children with acute chest syndrome, 12% of the 112 cases in children less than 5 had positive serologic testing of M. pneumoniae (9% of all cases had M. pneumoniae) (Neumayr et al, 2003).
1) Bradley et al. The Management of Community-Acquired Pneumonia in infants and children older than 3 months of age: Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin. Infect. Dis. 53:617-630 (2011)
2) Miller, S. How I treat acute chest syndrome in children with sickle cell disease. Blood 117:5297-5305 (2011)
3) Neumayr L, et al. Mycoplasma disease and acute chest syndrome in sickle cell disease. Pediatrics 1212:87-95 (2003)
Category: Pediatrics
Keywords: Fluid resuscitation, gastroenteritis, dehydration (PubMed Search)
Posted: 10/21/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Plasma-Lyte A outperformed 0.9% NaCl for rehydration in children with acute gastroenteritis showing a more rapid improvement in serum bicarbonate levels and dehydration scores.
This was a prospective randomized double blinded study in 8 pediatric emergency departments. Patients were at least 6 months old and younger than 11 years. To be included they had to have at least 3 episodes of vomiting or diarrhea in the previous 12 hours and a Gorelick score of at least 4. 100 children were included. Serum bicarbonate was measured at 0 and 4 hours and dehydration scores were reassessed. There was a change of bicarbonate of 1.6 mEq/L for plasma-lyte A (PLA) and no change for sodium chloride. There as an improvement in the dehydration score at 2 hours for the PLA group, but the dehydration scores were not statistically significant between the 2 groups at the 4 hours mark.
Allen et al. A randomized trial of Plasma-Lyte A and 0.9% sodium chloride in acute pediatric gastroenteritis. BMC Pediatrics 2016 16:117.
Category: Pediatrics
Keywords: nickel dermatitis, contact irritant, allergy (PubMed Search)
Posted: 10/1/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
A 12 year old male who recently started middle school presents to the ED with a rash in the periumbilical region that has been developing over the last few weeks. The rash is scaly, somewhat itchy, but otherwise benign appearing. The patient has no known medical conditions other than eczema, and is otherwise well. What is the diagnosis?
Picture courtesy of Mara Haseltine, MD
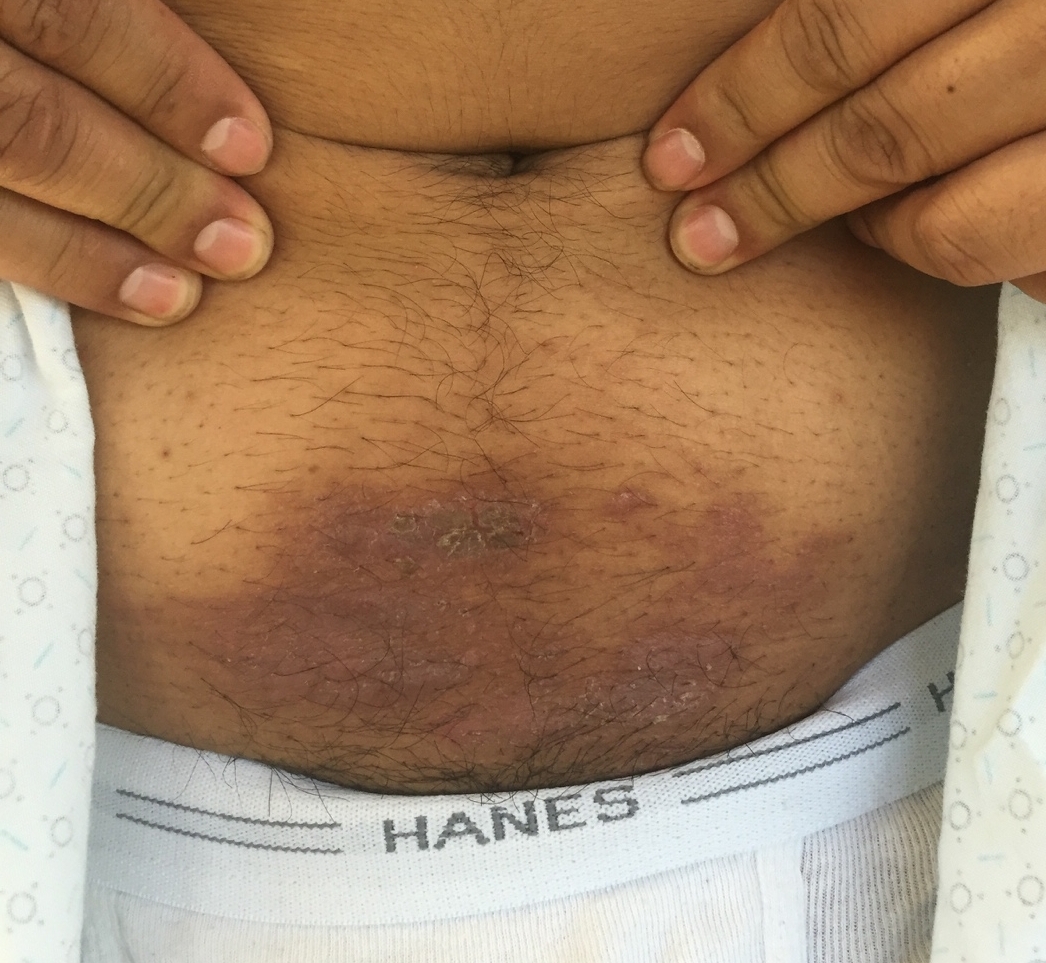
-Nickel allergy dermatitis is a type of allergic contact dermatitis common in skin tests in 8-16% of the pediatric population. Unlike irritant dermatitises (such as exposure to poison ivy), it usually takes repeated exposure over time to develop. In this case, the back of the button on a pair of blue jeans was the offending agent, though belt buckles, earrings, watches, piercings, and any other metal that touches skin can also cause a similar reaction. -The process is a delayed type hypersensitivity reaction mediated by T cells. Topical steroids can help clear up the rash, but the best treatment is to remove contact with the offending agent. One simple method is to apply clear nail polish to the back of the metal button or otherwise cover it with a piece of cloth. -Between 10 and 16 percent of blue jean buttons may contain nickel according to two studies. -Commercial test kits are available to help determine what metal components contain nickel -Known metal allergies should be communicated and documented as it can complicate orthopedic appliances or cardiac stents
1. T. Suneja, K. Flanagan and D. Glaser, "Blue-jean button nickel; prevalence and prevention of its release from buttons," Dermatitis, vol. 18, no. 4, pp. 208-211, December 2007 .
2. T. Byer and D. Morrell, "Periumbilical Allergic Contact Dermatitis: Blue Jeans or Belt Buckles?," Pediatric Dermatology, vol. 21, no. 3, pp. 223-226, May-June 2004.
3. J. Brasch and J. Geier, "Patch Test REsults in Schoolchildren. Results from the Information Netowrk of Departments of Dermatology (IVDK) and the German Contact Dermatitis Group (DKG)," Contact Dermatitis, vol. 37, pp. 286-93, 1997.
4. W. Weston, J. Weston and J. Kinoshita, "Prevalence of Positive Epicutaneous Tests Among Infants, Children, and Adolescents," Pediatrics, vol. 78, pp. 1070-1074, 1986.
Category: Pediatrics
Keywords: Bronchiolitis, ETCO2 (PubMed Search)
Posted: 9/16/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
114 children with bronchiolitis had end tidal carbon dioxide (ETCO2) measured on presentation to the ED. The ETCO2 levels did not differ significantly between admitted and discharged patients. In the subset of admitted patients, there was no correlation with ETCO2 on admission and days of oxygen requirement or length of stay.
Bottom line: Initial ETCO2 does not predict outcome for patients with bronchiolitis.
Jacob R, Bentur L, Brik R, Shavit I and Hakim F. Is capnometry helpful in children with bronchiolitis? Respir Med 2016; 113:37-41.
Category: Pediatrics
Keywords: procedural sedation (PubMed Search)
Posted: 8/26/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Alai, A. Nitrous Oxide Administration. Medscape/emedicine. http://emedicine.medscape.com/
Guideline for Monitoring and Management of Pediatric Patients During and After Sedation Diagnostic and Therapeutic Procedures. American Academy of Pediatrics. 2011
Clinical Policy: Critical Issues in the Sedation of Pediatric Patients in the Emergency Department. Annals of Emergency Medicine, 51(4):378-399 (2008)
Category: Pediatrics
Keywords: Trampoline, injury patterns (PubMed Search)
Posted: 8/19/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
From 2010-2014 ED visits in the US for injuries from trampoline parks (TPI) increased from 581 visits per year to 6932 visits per year. There was no change in the number of injuries related to home trampoline use. TPI were more likely to involve the lower extremity, be a dislocation and warrant admission and less likely to involve the head.
Bottom line: TPIs are increasing and have a different injury pattern compared to home trampolines.
Kasmire K, Rogers S and Sturm J. Trampoline Park and Home Trampoline Injuries. Pediatrics 2016: 138 (3).
Category: Pediatrics
Keywords: airway. mac (PubMed Search)
Posted: 7/29/2016 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
The pediatric epiglottis is more "U" shaped, often overlies the glottic opening, and is "less in line with the trachea."1 Because of this, it has traditionally been taught that a Miller blade is the ideal laryngoscope.
Varghese et al compared the efficacy of the Macintosh blade and the Miller blade when placed in the vallecula of children between the ages of 1 and 24 months. The blades provided similar views and suffered similar failure rates. When the opposite blade was used as a backup, it had a similar success rate as the opposing blade.2 Passi et al also compared these two blades, this time placing the Miller blade over the epiglottis. Again, similar views were achieved.3
1. Harless J, Ramaiah R, Bhananker S. Pediatric airway management. Int J. Crit Illn Inj Sci. 2014;4(1):65-70.
2. Varghese E, Kundu R. Does the Miller blade truly provide a better laryngoscopic view and intubating conditions than the Macintosh blade in small children? Paediatr Anaesth. 2014;24:825-829.
3. Passi Y, Sathyamoorthy M, Lerman J, et al. Comparison of the laryngoscopy views with the size 1 Miller and Macintosh laryngoscope blades lifting the epiglottis or the base of the tongue in infants and children <2 yr. of age. Br J Anaesth. 2014;113(5):869-874.
Category: Pediatrics
Keywords: Intranasal vaccine, immunizations (PubMed Search)
Posted: 7/15/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Although it is summer, preparations are being made for the 2016-2017 influenza season. The Center for Disease Control (CDC) no longer recommends the live attenuated influenza vaccine (LAIV4). The American Academy of Pediatrics has supported this statement.
The LAIV4 (the only intranasal vaccine available) was offered to patients over the age of 2 years without respiratory problems. Observational studies during the 2013-2015 seasons have shown that the LAIV4 has an adjusted vaccine efficacy of 3% compared to 63% for the inactivated vaccine (intramuscular). Children who received the intranasal vaccine were almost 4 times more likely to get the flu compared to children who received the injection.
Bottom line: Only the intramuscular shot is recommended for this upcoming season. This is causing many primary care practices to scramble to obtain enough vaccine.
Bernstein HH and Kimberlin DW. Intranasal FluMISSED its target. AAP News. July 2016.
Chung J et al. Seasonal Effectiveness of Live Attenuated and Inactivated Influenza Virus. Pediatrics 2016: 137 (2).
Category: Pediatrics
Keywords: hypertension, pediatrics (PubMed Search)
Posted: 6/17/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Stein DR, Ferguson MA. Evaluation and treatment of hypertensive crisis in children. Integr Blood Press Control 2016; 9:49-58.
Category: Pediatrics
Keywords: Apparent life threatening event, ALTE, apnea, low risk infants, brief unexplained resolved events (PubMed Search)
Posted: 5/20/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
The American Academy of Pediatrics has developed a new set of clinical practice guidelines to help better manage and think about patients who have experienced an ALTE (Apparent Life Threatening Event). The term BRUE (Brief Resolved Unexplained Event) will replace ALTE.
BRUE is defined as an event in a child younger than 1 year where the observer reports a sudden, brief and now resolved episode of one or more of: cyanosis or pallor; absent, decreased or irregular breathing, marked change in tone or altered level of responsiveness. A BRUE can be diagnosed after a history and physical exam that reveal no explanation.
BRUE can be classified as low risk or high risk. Those that can be categorized as low risk do not require the extensive inpatient evaluation that has often occurred with ALTE.
LOW risk BRUE:
Age > 60 days
Gestational age at least 32 weeks and postconceptual age of at least 45 weeks
First BRUE
Duration < 1 minute
No CPR required by a trained medical provider
No concerning historical features (outlined in the article)
No concerning physical exam findings (outlined in the article)
Recommendations for low risk BRUE:
-SHOULD: Educate, shared decision making, ensure follow up and offer resources for CPR training
-May: Obtain pertussis and 12 lead; briefly monitor patients with continuous pulse oximetry and serial observations
-SHOULD NOT: Obtain WBC, blood culture, CSF studies, BMP, ammonia, blood gas, amino acids, acylcarnitine, CXR, echocardiogram, EEG, initiate home cardiorespiratory monitoring, prescribe acid suppression or anti-epileptic drugs
-NEED NOT: obtain viral respiratory tests, urinalysis, glucose, serum bicarbonate, hemoglobin or neuroimaging, admit to the hospital solely for cardiorespiratory monitoring
*When looking at the evidence strength behind these recommendations, the only one that had a strong level was that you should not obtain WBC, blood culture or CSF
Tieder JS, Bonkowsky JL, Etzel RA, et al. Brief Resolved Unexplained Events (Formerly Apparent Life-Threatening Events) and Evaluation of Lower-Risk Infants. Clinical Practice Guideline. Pediatrics. 2016; 137 (5):e20160590.
Category: Pediatrics
Posted: 4/29/2016 by Mimi Lu, MD
(Updated: 4/30/2016)
Click here to contact Mimi Lu, MD
Neonatal jaundice- Incidence ~85% of term newborns
Bili levels are EXPECTED to rise during first 5 days of life
Be aware of CONJUGATED hyperbilirubinemias (biliary atresia, infection)
Majority of cases due to increase in unconjugated (indirect) bilirubin 2/2 residual fHgb breakdown and insufficient capacity of hepatic conjugation
Severe hyperbilirubinemia (Tbili >20mg/dL) <2% of term infants
⇒
Acute bilirubin encephalopathy(ABE)- Hypertonia, arching, opisthotonos, fever, high pitched cry
⇒
Kernicterus (5% of ABE)-CP, MR, auditory dysfunction, upward gaze palsy
When to refer for phototherapy/exchange transfusion
“Evaluation and Treatment of Neonatal Hyperbilirubinemia” Muchowski MD, Naval Hospital Camp Pendleton Family Medicine Residency Program, Camp Pendleton, California; Am Fam Physician. 2014 Jun 1;89(11):873-878.
Management of Hyperbilirubinemia in the Newborn Infant35 ore More Weeks of Gestatiion, Pediatrics 2004 July; 114(1)
Category: Pediatrics
Keywords: Intracranial hemorrhage, ultrasound, non accidental trauma (PubMed Search)
Posted: 4/15/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Typically, if an infant or young child presents to the ED with concern for intracranial hemorrhage (ICH), CT is performed as a rapid diagnostic tool. Now that clinicians are more aware of the radiation associated with head CT, the possible use of ultrasound was studied. Ultrasound is commonly used in the neonatal population for detecting ICH. A study by Elkhunovich et al looked at children younger than 2 years who had cranial ultrasounds preformed. Over a 5 year period, 283 ultrasounds were done on patients between 0 to 485 days old (median 33 days). There were 39 bleeds detected. Ultrasound specificity and sensitivity was calculated by comparing the results with CT, MRI and/or clinical outcome. For significant bleeds, the sensitivity for ultrasound was 81%. The specificity for detecting ICH was 97%.
Only 2 patients in the study were older than 1 year. The proper windows are easiest to visualize in children younger than 6 months.
Bottom Line: The sensitivity of cranial ultrasound is inadequate to justify its use as a screening tool for detection of ICH in an infant with acute trauma, but it could be considered in situations when obtaining advanced imaging is not an option because of availability or patient condition.
Elkhunovich M, Sirody J, McCormick T, Goodarzian F and Claudius I. The Utility of Cranial Ultrasound for Detection of Intracranial Hemorrhage in Infants. Ped Emerg Care 2016 [epub ahead of print].
Category: Pediatrics
Keywords: End tidal capnography, diabetic ketoacidosis (PubMed Search)
Posted: 3/19/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
A previous pearl has looked at serum HCO3 as a predictor of DKA (see pearl from 8/21/15). The article by Gilhotra looks at using end tidal CO2 (ETCO2) to exclude DKA. 58 pediatric patients were enrolled with 15 being in DKA. No patient with ETCO2 > 30 mmHg had DKA. Six patients with ETCO2 < 30 mmHg did not have DKA. Other studies done in children have shown similar results.
An article recently published by Chebl and colleagues examined patients older than 17 years with hyperglycemia. In this study, 71 patients were included with 32 having DKA. A ETCO2 >35 excluded DKA in this group while a level <22 was 100% specific for DKA.
Bottom line: ETCO2 >35 mmHg is a quick bedside test that can aid in the evaluation of hyperglycemic patients.
Gilhotra Y and Porter P. Predicting diabetic ketoacidosis in children by measuring end-tidal CO2 by non-invasive nasal capnography. J Paediatr Child Health 2007; 43 (10): 677-80.
Chebl BR, Madden B, Belsky J, Harmouche E, Yessayan L. Diagnostic value of end tidal capnography in patients with hyperglycemia in the emergency department. BCM Emerg Med 2016: 16 (1).
Category: Pediatrics
Posted: 2/26/2016 by Mimi Lu, MD
(Updated: 2/27/2016)
Click here to contact Mimi Lu, MD
Perianal Group A Strep is an infectious dermatitis seen in the perianal region that is caused by Group A beta-hemolytic Strep. Children will have a characteristic rash with a sharply-demarcated area of redness, swelling, and irritation around the perianal region. There may be associated swelling and irritation of the vulva and vagina (in girls) and penis in boys. Patients can have bleeding or itching during bowel movements.
The age range is often <10 years of age. There is often an absence of fever or other systemic symptoms.The diagnosis can be confirmed by obtaining a Rapid Strep swab from the area of interest. You can also collect a bacterial culture of the area.
Treatment requires a 14 day course of penicillin. Amoxicillin (40 mg/kg/day divided TID) and clarithromycin are alternative treatments. The additional of topical bactroban (mupirocin) can be effective, but it should not be used as monotherapy. Re-occurrence is common, so close follow-up is key.
Category: Pediatrics
Keywords: UTI, fever, infant (PubMed Search)
Posted: 2/19/2016 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
There is not much data published on susceptabilities of urinary pathogens in infants. What resistance patterns are seen in infants < 2 months in gram negative uropathogens?
A retrospective study of previously healthy infants diagnosed with urinary tract infections in Jerusalem over a 6 year period examined this question. The standard treatment at this hospital included ampicillin and gentamycin for less than 1 month olds and ampicillin or cefuroxime for 1-2 month olds.
306 UTIs were diagnosed
74% were resistant to ampicillin
22% were resistant to cefazolin and augmentin
8% were resistant to cefuroxime
7% were resistant to gentamycin
Of the organisms cultured, 76% were E. coli and 14% were Klebsiella.
Bottom line: Know your local resistance patterns.
Segal Z et al. Infants under two months of age with urinary tract infections are showing increasing resistance to empirical and oral antibiotics. Acta Paediatrica. Dec 2015. Epub ahead of print.
