Category: Pediatrics
Posted: 2/1/2013 by Lauren Rice, MD
Click here to contact Lauren Rice, MD
This winter season has brought a rise in influenza and RSV activity in Maryland and in many parts of the country. It is also important to remember other potentially lethal infections that are prevalent in the winter and early spring months, such as Neisseria meningitidis. In fact, a recent study2 showed a potential increase in meningococcal disease when influenza and RSV activity is high.
What:
Encapsulated, gram-negative diplococcus
Where:
Found in nasopharyngeal secretions, carrier rates 2-30% in normal populations
Who:
Age of incidence has 2 peaks: children < 2 years old, teens 15-19 years old
Young adults who live in shared housing, such as college dorms and military recruits
Clinical Presentation:
Early non-specific symptoms of URI, fever, malaise, myalgias
Meningitis: non-specific prodrome + headache, stiff neck (not found in younger children who often present atypically with irritability and/or vomiting)
Meningococcemia: above symptoms + hypotension + petechial rash (>60% of patients)
Treatment:
Early (!) antibiotics: 3rd generation cephalosporins (<3mo: cefotaxime; older infants, children, and teens: ceftriaxone); PCN G is antibiotic of choice for susceptible isolates
Early and aggressive management of shock
Prevention:
Tetravalent vaccine, MCV4 (Menactra, Menveo), available for serogroups A, C, Y and W-135 is given routinely at age 11-12 years old with an additional booster at 16-17 years old. MCV4 does not protect against serogroup B which accounts for 30% of infections.
1. Cross JT, Hannaman RA. Infectious Disease. MedStudy Pediatrics Board Review Core Curriculum: 5th edition. 2012; 5-11.
2. Jansen AG, Sanders EA, VAN DER Ende A, VAN Loon AM, Hoes AW, Hak E. Invasive pneumococcal and meningococcal disease: association with influenza virus and respiratory syncytial virus activity?. Epidemiol Infect. Nov 2008;136(11):1448-54.
3. Javid MH. Meningococcemia. Available at http://emedicine.medscape.com/article/221473. Medscape Reference. Last updated Aug. 2. 2012.
Category: Pediatrics
Keywords: magnets, bowel perforation, ischemic necrosis, ingestion (PubMed Search)
Posted: 11/30/2012 by Mimi Lu, MD
(Updated: 1/18/2013)
Click here to contact Mimi Lu, MD
Patient: A 10 year old female is brought to the ED after swallowing 2 beads (see image). Based on the findings, what are your concerns and what is the disposition?
Answer: Multiple Magnet Ingestion
The mother was eventually able to produce the magnetic beads ingested at home 2 hours prior to presentation
The ingestion of multiple magnets is a medical emergency. If the 2 magnets separate and reconnect it can lead to:
- pressure necrosis
- bowel perforation
- fistula formation
- and/or bowel obstruction secondary to kinking, inflammatory reaction, and/or internal herniation
Patients with a multiple magnet ingestion should be taken emergently to the OR for endoscopic evaluation.
If the magnets have passed the pylorus, conservative management with laxatives and serial X-rays may be performed, however if their position becomes fixed on serial imaging then an emergent laparotomy may need to be performed for the removal of the FBs before the symptoms and signs occur.
Bottom line: Patients presenting with a multiple magnet ingestion need to be admitted regardless of the FB location. Consult GI and pediatric surgery early, since prompt removal can prevent devastating outcomes. Single magnet ingestions can be managed conservatively with serial exams and imaging.
Reference:
Alzaham AM et al, Ingested magnets and gastrointestinal complications. Journal of Paediatrics and Child Health; 43 (2007) 497–498.
Category: Pediatrics
Posted: 1/11/2013 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
CDC MMWR 1/2011
FDA 12/2012
Category: Pediatrics
Posted: 1/4/2013 by Lauren Rice, MD
(Updated: 5/13/2026)
Click here to contact Lauren Rice, MD
Rotavirus is the leading cause of gastroenteritis worldwide and a leading cause of infant death in the developing world.
95% of U.S. children have had a rotavirus infection by the age of 5 years.
Most cases occur in late winter and early spring.
Route of transmission is mostly fecal-oral but may be airborne in cooler months.
Most common presenting signs and symptoms include fever (1/3 of cases), vomiting (in the first 1-2 days), and diarrhea (copious, watery, lasting 5-21 days).
Diagnosis is largely based on clinical manifestations, but antigen assays are available and may be useful in patients with extraintestinal complications, such as hepatitis, pneumonitis, or encephalopathy.
Treatment is largely supportive with efforts to maintain hydration.
Prevention is key to disease control and accomplished with good hand hygiene and widespread vaccination.
Newly implemented vaccine programs worldwide have proven to be effective in decreasing hospitalizations and deaths in developing countries.
Cox, Elaine and Christenson, John. Rotavirus. Pediatrics in Review. 2012; 33 (10): 439 - 447.
Category: Pediatrics
Posted: 12/28/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 12/15/2012 by Mimi Lu, MD
(Updated: 12/21/2012)
Click here to contact Mimi Lu, MD
Parents bring in their child who placed a bead, seed, or other object up her nose. What do you do? Who should you call?
Research suggests that a decades-old home remedy (of sorts) known as the “mother’s kiss” may do the trick for children 1-8 years of age. It’s also much less invasive or frightening than some of the tools and techniques used in emergency departments with a success rate approaching 60%
First described in 1965, here’s how the mother’s kiss technique works:
Category: Pediatrics
Posted: 12/7/2012 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Epidemiology:
Trampoline injuries doubled between 1991 and 1996, increasing from 39,000 injuries per year to more then 83,000 injuries per year. Injury rates and trampoline sales peaked in 2004 and have been decreasing since; however, hospitalization rates are still between 3% and 14%.
Risk Factors:
¾ of injuries occur when multiple people are on the trampoline at once
Smaller participants were 14x more likely to be injured then their heavier playmates
Falls account for 27-39% of all injuries
Springs and frames account for 20% of injuries
Up to ½ of injuries occur despite adult supervision
Injury types:
Lower extremity injuries are more common than upper extremity
Head and neck injuries accounted for 10-17% of trampoline injuries
Unique Injuries:
Proximal tibial fractures
Manubriosternal dislocations and sternal injuries
Vertebral artery dissection
Atlanto-axial subluxation
Trampoline Saftey in Childhood and Adolescence. Pediatrics 2012; 130; 774-779.
Category: Pediatrics
Keywords: meningitis, neck pain, retropharyngeal abscess (PubMed Search)
Posted: 11/16/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
A 1 year old gets sent from their pediatrician’s office for rule out meningitis. They presented with fever for 2 days and neck rigidity. Your LP results are normal. What additional test should you consider?
Answer:
Lateral neck x-ray
http://www.hawaii.edu/medicine/pediatrics/pemxray/v2c20.html
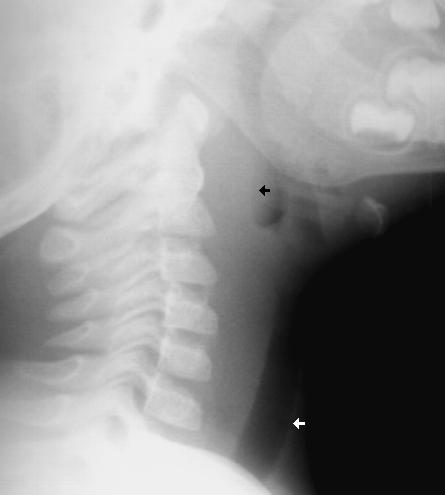
Retropharyngeal abscess (RPA) can commonly present like meningitis. Have a high suspicion in
children who are too young to complain of sore throat or difficulty swallowing.
A recent article in Pediatric Infectious Disease Journal detailed the rising incidence of retropharyngeal abscess, especially in younger patients, which is attributed to community acquired MRSA.
From 2004-2010 there was a 2.8 fold increase in RPA from the previous study period (1993-2003).
Children whose abscess grew MRSA were younger (mean 11 months) than the others (mean 62 months) (P < 0.001) and required longer duration of hospitalization (mean 8.8 days) than the rest (mean 4.5 days) (P = 0.002).
Bottom line: Consider a plain film in the child you are preparing to LP for meningitis.
Reference:
Abdel-Haq, N, Quezada M, Asmar BI. Retropharyngeal abscess in children: the rising incidence
of methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2012; 31: 696–699
Category: Pediatrics
Posted: 11/2/2012 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Conventional pediatric nasal cannula can safely deliver up to 4 lpm but are limited by cooling and drying of the airway. This leads to decreased airway patency, nasal mucosal injury, bleeding and possibly increase in coagulase negative staph infections.
HFNC delivers flow up to 40 lpm with 95-100% relative humidity at a controlled temperature. In infants, the initial flow rate is set between 2-4 lpm and can be increased to 8 lpm. Older children and can be started at 10 lpm and increased as high as 40 lpm. Oxygen is also adjustable.
Studies have shown improved comfort, respiratory rate and oxygenation compared to nasal CPAP.
Noninvasive Ventilation Techniques in the Emergency Department: Applications in Pediatric Patients. Pediatric Emergency Medicine Practice. Vol 6 No 6. June 2009.
Spentzas et al. Children with Respiratory Distress Treated with High-Flow Nasal Cannula. Journal of Intensive Care Medicine. Vol 24 No 5. September/October 2009.
Category: Pediatrics
Keywords: croup, laryngomalacia (PubMed Search)
Posted: 10/26/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 10/12/2012 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Glaser N, Barnett P, et al. Risk factors for cerebral edema in children with diabetic ketoacidosis. The Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics. N Engl J Med 2001;344:264.
Category: Pediatrics
Keywords: Vaccines (PubMed Search)
Posted: 10/5/2012 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
We often ask our pediatric patients if there vaccines are up to date, but what does this mean?
Hepatitis B: birth, 2 and 6 months
Diphtheria/Tetanus and Acellular Pertussis: 2, 4 and 6 months
Pneumococcal vaccine: 2, 4 and 6 months
Haemophilus influenzae B : 2, 4 and 6 months
Polio: 2, 4 and 6 months
Rotavirus: 2 and 4 months or 2, 4 and 6 months depending on the brand.
Influenza: 6 months and older
Children less than 8 years old should receive 2 doses of flu vaccine at least 4 weeks apart during the first flu season that they are immunized. Children older than 2 years are eligible for the nasal vaccine if they do not have asthma, wheezing in the past 12 months or other medical conditions that predispose them to flu complications.
To see the full vaccine schedule including exact time frames between doses and catch up schedules, see: http://www.cdc.gov/vaccines/
Category: Pediatrics
Keywords: dysrhythmia, arrhythmia (PubMed Search)
Posted: 9/28/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
The incidence of pediatric syncope is common with 15%-25% of children and adolescents experiencing at least one episode of syncope before adulthood. Incidence peaks between the ages of 15 and 19 years for both sexes.
Although most causes of pediatric syncope are benign, an appropriate evaluation must be performed to exclude rare life-threatening disorders. In contrast to adults, vasodepressor syncope (also known as vasovagal) is the most frequent cause of pediatric syncope (61%–80%). Cardiac disorders only represent 2% to 6% of pediatric cases but account for 85% of sudden death in children and adolescent athletes. 17% of young athletes with sudden death have a history of syncope.
Key features on history and physical examination for identifying high-risk patients include exercise-related symptoms, a family history of sudden death, a history of cardiac disease, an abnormal cardiac examination, or an abnormal ECG.
Category: Pediatrics
Keywords: premedication, RSI, ventilator, high flow nasal cannula (PubMed Search)
Posted: 9/21/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 9/15/2012 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Category: Pediatrics
Keywords: cervical spine, trauma, pediatrics (PubMed Search)
Posted: 9/7/2012 by Lauren Rice, MD
Click here to contact Lauren Rice, MD
Ligamentous laxity is increased in children and ligamentous injury is more common than fractures.
If fractures occur, they are more likely to be in the upper cervical spine in infants and the lower cervical spine in older children.
Pseudosubluxation: physiologic subluxation between C2-3 and C3-4 may exist until age 16 years
Screening Assessment/Clearance for Verbal Children
-Midline C-spine tenderness?
-Pain with active motion?
-Altered level of alertness?
-Evidence of intoxication?
-Focal neurological deficit?
-Distracting painful injury?
-High impact injury?
Screening Assessment/Clearance for Pre-Verbal Children
-Neurological assessment of basic reflexes
-Response to painful stimuli
-Equal movements of all extremities
-Response to sound (eye tracking)
-Extremity strength and resistance
-Palpate posterior C-spine (observe for facial grimace)
-Feel for step-offs, deformities
-Verify full range of motion of neck (may need to be creative)
-Repeat neurological assessment
If concern arises on screening assessment, keep child in hard cervical collar and image (may start with x-ray and progress to CT if still concerned and x-rays negative).
If imaging negative, but persistent suspicion based on neurological deficits consider SCIWORA (Spinal Cord Injury WithOut Radiographic Abnormality) which exists in up to 50% of children with cervical cord injury, and may require MRI to further identify injury.
Category: Pediatrics
Keywords: septic shock, fluid resuscitation, PALS (PubMed Search)
Posted: 8/31/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 8/24/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Types:
- Uniphasic anaphylaxis: occuring immediately after exposure to allergen, resolves over minutes to hours and does not recur
- Biphasic anaphylaxis: occuring after apparent resolution of symptoms typically 8 hours after the first reaction. Occur in up to 23% of adults and up to 11% of children with anaphylaxis
Treatment:
1. First line: IM epinephrine 1:1000 solution
- vasoconstrictor effects on hypotension and peripheral vasodilation; bronchodilator effects on upper respiratory obstruction
- NO absolute contraindication for use in anaphylaxis
- Dosage: Adult: 0.3 - 0.5mg; Peds: 0.01mg/kg (max 0.3mg)
- can be repeated every 5-15 minutes
2. Adjunctive therapy:
- H1 Blocker: diphenhydramine 1-2mg/kg up to 50mg IV
- H2 Blocker: ranitidine 1-2mg/kg
- Corticosteroid: 1-2 mg/kg for prevention of biphasic reactions
- Bronchodilator: Albuterol for bronchospasm
- Glucagon: for refractory hypotension or if patient is on beta blocker
- Dosage: Adult: 1-5 mg; Peds 20-30microgm/kg
- Dose may be repeated or followed by infusion of 5-15 mg/min
- place patient in recumbent position if tolerated with lower extremities elevated
- supplemental O2
- IV fluids for hypotension
Fatalities: typically seen with peanut or treenut ingestions from cardiopulmonary arrest. Associated with delayed or inappropriate epinephrine dosing
Disposition:
- Mild reaction with symptom resolution: observe for 4-6 hrs (ACEP, AAP)
- Recurrent symptoms or incomplete resolution: admit
Reference:
1. World Allergy Organization Guidelines for the Assessment and Management of Anaphylaxis, Feb 2011
2. Guidelines for the Diagnosis and Management of Food Allergy in the United States: Report of the NIAID-Sponsored Expert Panel Oct 2010
Category: Pediatrics
Keywords: vaccination, whooping cough (PubMed Search)
Posted: 8/17/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
If you have a patient who meets (or has had close exposure to someone meeting) the clinical case definition of pertussis (a cough lasting at least 2 weeks with one of the following: paroxysms of coughing, inspiratory “whoop,” or post-tussive vomiting) here are some important points to keep in mind:
Vaccination
Testing
Treatment
References:
Altunaiji SM, Kukuruzovic RH, Curtis NC, Massie J. Antibiotics for whooping cough (pertussis). Cochrane Database of Systematic Reviews 2007, Issue 3. Art. No.: CD004404. DOI: 10.1002/14651858.CD004404.pub3
http://www.cdc.gov/vaccines/pubs/surv-manual/chpt10-pertussis.html
Category: Pediatrics
Posted: 8/10/2012 by Rose Chasm, MD
Click here to contact Rose Chasm, MD
