Category: Orthopedics
Keywords: Steroids, Sciatica (PubMed Search)
Posted: 6/20/2015 by Michael Bond, MD
Click here to contact Michael Bond, MD
Steroid Use in the treatment of Acute Sciatica
Have you used oral steroids in the treatment of your patient with acute sciatica thought to be secondary to a herniated disk.
Well a recent randomizaed, double-blind, placebo-controlled trial from 2008 to 2013 in a large integrated health care system in Northern California enrolled 269 patients to look at whether steroids improved pain or function. The intervention arm (twice as large as placebo arm) received a tapering 15-day course of oral prednisone (5 days each of 60 mg, 40 mg, and 20 mg; total cumulative dose = 600 mg; n = 181).
In the end there were no differences in surgery rates at 52-week follow-up, and the steroid arm had a modest improvement in function but no improvement in pain. There were also more adverse events at 3-week follow-up in the prednisone group than in the placebo group.
Conclusion: Giving steroids for acute sciatica does not appear to improve the patients pain, only has a modest improvement in function, and was associated with more adverse events. Put another way there was minimal benefit and more harm.
You can check out the full article at http://jama.jamanetwork.com/article.aspx?doi=10.1001/jama.2015.4468
Goldberg H, Firtch W, Tyburski M, Pressman A, Ackerson L, Hamilton L, Smith W, Carver R, Maratukulam A, Won LA, Carragee E, Avins AL. Oral steroids for acute radiculopathy due to a herniated lumbar disk: a randomized clinical trial. JAMA. 2015 May 19;313(19):1915-23. doi: 10.1001/jama.2015.4468.
Category: Orthopedics
Keywords: tensor fascia latae, hip, pain (PubMed Search)
Posted: 5/16/2015 by Michael Bond, MD
Click here to contact Michael Bond, MD
Tensor Fascia Latae (Iliotibial Band) Pain Syndrome:
Some patients will complain of hip and back pain and can have multiple visits before somebody considers Tensor Fascia Latae Pain Syndrome AKA Iliotibial Band Syndrome.
The tensor fascia latae helps with thigh flexion at the hip, abduction, and medial rotation; and stabilizes the knee laterally
When this muscle/fascia gets tight and overcontracted it will lead to dysfunction of the gluteus and rectus femoralis muscles leading to increased hip pain due to abnormal movement of the joint.
Patients often complain of increased pain with running, especially downhill and exam is notable for local tenderness (approx. 2cm above lateral joint line) & occasional swelling over the distal lateral thigh.
Most patients respond to conservative treatment involving NSAIDs, stretching of the iliotibial band, physical therapy, strengthening of the gluteus medius, and altering their running regimens.
Category: Orthopedics
Keywords: knee, hip, back, pain, acetaminophen (PubMed Search)
Posted: 4/18/2015 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Is acetaminophen good for pain control in patients with Osteoarthritic of the Knee or Hip or Low Back Pain? Most of my patients request narcotics, but conventional teaching is that we should try to start with Acetaminophen or NSAIDs.
This recent study, http://www.bmj.com/content/350/bmj.h1225, published in the BMJ analyzed 13 studies looking at over 5400 patients. In the end, they found that acetaminophen did not appear to improve pain, disability or the patient’s quality of life in patients with back pain. Also, there was a small improvement in pain and disability in those with hip and knee pain, but it was not deemed clinically significant.
Even worse, patients taking acetaminophen had a 4x greater chance of having abnormal liver function tests.
This meta-analysis really questions whether Acetaminophen should be first line therapy in patients with osteoarthritis of the knees or hips, or in those with low back pain. For now I will stick with a course of a NSAID. Especially with the risk of unintentional overdose if they are taking other over the counter medicaitons that might also contain acetaminophen.
Machado GC, Maher CG, Ferreira PH, Pinheiro MB, Lin CW, Day RO, McLachlan AJ, Ferreira ML. Efficacy and safety of paracetamol for spinal pain and osteoarthritis: systematic review and meta-analysis of randomised placebo controlled trials. BMJ. 2015 Mar 31;350:h1225. doi: 10.1136/bmj.h1225
Category: Orthopedics
Keywords: Back Pain, Elderly (PubMed Search)
Posted: 3/21/2015 by Michael Bond, MD
Click here to contact Michael Bond, MD
It is commonly taught that radiographs are not needed in non-traumatic back pain unless the patient is <18 or > 65 years old. Several studies have started to disprove this in the pediatric population, and a recent study in JAMA is giving some weight to not having to do this in the eldery.
The JAMA study was a prospective cohort of 5239 patients over age 65 who presented to a PCP or urgent care center in three different health systems from 2011-2013 with a complaint of back pain without radiculopathy. Patients were determined to have early imaging if they had a plain films, CT, or MRI done within 6 weeks of their initial visit for back pain. The primary outcome measure was back or leg-pain related disability at 12 months when comparing those that had early imaging versus late (> 6 weeks). They excluded patients with prior surgery, prior back pain, or if they had a cancer visit in the prior year.
At one year they found that there was no statistical difference in the primary outcome of back or leg-pain related disability at one year. The early imaging did pick up more fractures of the spine, but again no change in long term outcomes. The serious diagnoses were summarized in this graph.
This study was not done in the Emergency Medicine setting, and our patients may not be equivilant, but it suggests that we do NOT have to get radiographs on all patients over 65 years old with non-traumatic back pain without radiculopathy. If you are not going to get radiographs make sure your patient has clear discharge instructions on what to return for and that they should follow up with their primary care provider within a week.
A link to the full article is here http://jama.jamanetwork.com/article.aspx?articleid=2203801
Jarvik JG, Gold LS, Comstock BA, et al. Association of Early Imaging for Back Pain With Clinical Outcomes in Older Adults. JAMA. 2015;313(11):1143–11. doi:10.1001/jama.2015.1871.
Category: Orthopedics
Keywords: Orthopaedic, Chest Pain (PubMed Search)
Posted: 2/28/2015 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Orthopedic Causes of Chest Pain
The first thing that pops into everybody’s mind when they hear a patient state they have chest pain radiating to the left arm is Acute Coronary Syndrome and specifically a Myocardial Infarction. However, there are a lot of orthopedic causes of chest pain that can also radiate to the left arm. It is estimate that up to 20% of patients with pectoral symptoms have an underlying orthopedic problem.
Some of them are:
Some other less common causes are
So instead of just ordering some troponin and admitting to medicine, consider that the cause can be orthopedic in origin.
Fromm B. Often an orthopedic problem can manifest as chest pain. Cervical vertebrae syndrome mimics myocardial infarct. MMW Fortschr Med 2002 Apr 25; 144(17):31-3.
http://www.ncbi.nlm.nih.gov/pubmed/12048845
Category: Orthopedics
Keywords: heel, pain, causes (PubMed Search)
Posted: 1/17/2015 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
We often think of Plantar Fascitis as the cause of heel pain but there are a lot of other causes. Some of those include:
Category: Orthopedics
Keywords: back pain, red flag (PubMed Search)
Posted: 11/29/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
A recent meta-analysis of 14 studies looked at the typical red flags of back pain to see which ones actually truly increase the risk that the patient will have a fracture or malignancy.
The typical historical red flags that are taught are
And physical exam red flags are
However, this meta-analysis showed that the only red flags that actually increased the risk of fracture or malignancy were
So this study highlights that a lot of the red flags that we have learned do not actually increase the risk fracture or malignancy, although some like fever, IVDA, and immunocomproromised increase the risk of epidural abscesses, which was not addressed in this meta-analysis.
The take home point for me is that plain radiographs/CT scans are probably only needed in patients with older age, prolonged corticosteroid use, severe trauma or presence o contusion or abrasion. If you are really worried about others with back pain just proceed directly to MRI as the plain films/CT scans are not going to be very helpful.
Downie A, Williams CM, Henschke N, et al. Red flags to screen for malignancy and fracture in patients with low back pain. British Journal of Sports Medicine. 2014;48(20):1518–1518. doi:10.1136/bjsports-2014-f7095rep.
Category: Orthopedics
Keywords: felon, management (PubMed Search)
Posted: 11/15/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Management of Felons
For good photos of the incision technique please visit the reference article listed.
Category: Orthopedics
Keywords: Segond, Reverse, Fracture (PubMed Search)
Posted: 10/19/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
The Reverse Segond Fracture
Most people have heard of a segond fracture (avulsion fracture of the lateral tibeal platuea) seen on knee xrays which is a marker for Anterior Cruciate Ligament and medial meniscus injuries. See Pearl https://umem.org/educational_pearls/1015/
However, there is also a Reverse Segond Fracture that is another benign appearing avulsion fracture of the medial tibeal plateau that is marker for significant injury to the Posterior Cruciate Ligament (PCL).
If a Segond or Reverse Segond Fracture is seen consider immobilzing the patients knee until they can follow up with Orthopedics and/or get an MRI to determine if additional injuries are present.
Category: Orthopedics
Keywords: Tendon, Laceration, Repair (PubMed Search)
Posted: 9/19/2014 by Michael Bond, MD
(Updated: 9/20/2014)
Click here to contact Michael Bond, MD
Tendon Lacerations:
A reasonable approach to all tendon lacerations is to loosly reapproximate the wound and splint the hand in the position of function until the patient can be seen by a hand surgeon in the next 1-3 days. These injuries do not require immediate surgical repair, and with the high rate of complications it is probably best to discuss with your hand surgeon before attempting a repair.
Wheeless Textbook of Orthopaedics. http://www.wheelessonline.com/ortho/extensor_tendon_lacerations
Category: Orthopedics
Keywords: radiology, ankle, fracture (PubMed Search)
Posted: 8/30/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
Some radiology pearls concerning ankle pain and fractures courtesy of David Bostick and Michael Abraham
Maisonneuve fracture – fracture of the medial malleolus with disruption of the tibiofibular syndesmosis with associated fracture of the proximal fibular shaft (http://radiopaedia.org/articles/maisonneuve-fracture)
When to look for high fibular fracture
Always look for avulsion fracture of 5th metatarsal styloid in patients with ankle pain and
no obvious fractures
Dans-Weber Classification – for lateral malleolar fractures (http://radiopaedia.org/articles/ankle-fracture-classification-weber)
Category: Orthopedics
Keywords: Back Pain, Prednisone (PubMed Search)
Posted: 8/17/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Is there any benefit to the use of prednisone in the treatment of lower back pain? One study showed that about 5% of patients receive prednisone for the treatment of their low back pain, but does it work.
A recent study by Eskin et al published in the Journal of Emergency Medicine looked at this question. They conducted a randomized controlled trial of 18-55 year olds with moderately severe low back. Patients were randomized to receive prednisone 50mg for 5 days or placebo.
The study enrolled a total of 79 patients, and 12 were lost to follow up. At followup there was no difference in their pain, or in them resuming normal activities, returning to work, or days lost from work. To make matters worse more patients in the prednisone group sought additional medical treatment 40% versus 18%.
Conclusion: With the results of this study we should continue the treatment of low back pain with non-steroidials, muscle relaxants and exercise. There does not appear to be any role for steroids in the treatment of these patients.
Eskin B, Shih RD, Fiesseler FW, et al. Prednisone for emergency department low back pain: a randomized controlled trial. Journal of Emergency Medicine. 2014;47(1):65–70. doi:10.1016/j.jemermed.2014.02.010.
Category: Orthopedics
Keywords: knee, injury, dislocation (PubMed Search)
Posted: 6/21/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Some quick facts about Knee Injuries:
Category: Orthopedics
Posted: 6/1/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
When examining a knee for a meniscal injury the commonly described tests are the McMurray Test and Apley Test. However, these tests have sensitivities of 48-68% and 41% respectfully, and specificities of 86-94% and 86-93% respectfully. Depending on whether you are looking at the medical or lateral meniscus.
The Thessaly Test that was first described in 2005 can be performed with knee in either 5 or 20 degrees of flexion and has a senstivity of 89-92% and specificity of 96-97% when performed in 20 degrees flexion. The test also tends to be easier to perform.
To perform the test:
Essentially you and your patient will look like you are doing the twist as they rotate their knee with you holding their hands.
A video of the technique can be found at http://youtu.be/R3oXDvagnic
The Journal of Bone and Joint Surgery (American). 2005;87:955-962.
Category: Orthopedics
Keywords: lisfranc, fracture (PubMed Search)
Posted: 5/17/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
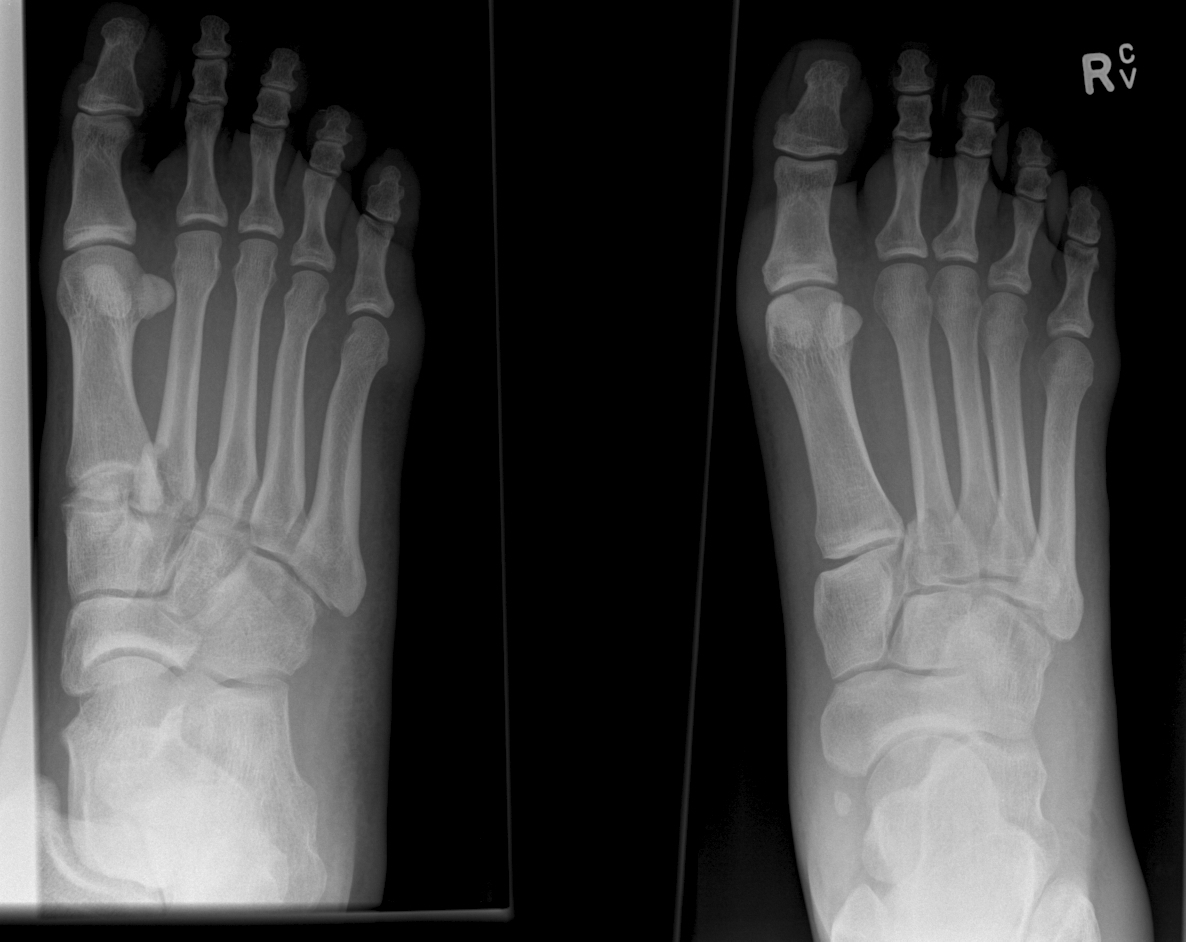
Lisfranc Fracture:
Typically consists of a fracture of the base of the second metatarsal and dislocation, though it can also be associated with fractures of a cuboid. Common current mechanism of injury is when a person steps into a hole and twists the foot. The original mechanism of injury that was described was when a horseman would fall of their horse with their foot still trapped in a stirrup.
Diagnosis should be considered if patient has difficultly weight bearing with pain on palpation over the 2nd and 3rd metacarpal head with an appropriate mechanism.
Pearls:
Category: Orthopedics
Keywords: DeQuervain, Intersection, Syndrome, Tenosynovitis (PubMed Search)
Posted: 3/30/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
DeQuervain and Intersection Syndromes:
Category: Toxicology
Keywords: Carbon Monoxide, (PubMed Search)
Posted: 3/15/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
Carbon Monoxide Half-Life:
Category: Misc
Keywords: Postoperative, fever, cause (PubMed Search)
Posted: 1/18/2014 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
Post Operative Fever is extremely common, and with the increase in same day surgery this is a common complaint presenting to the ED. The mnemonic "5Ws" are often taught to remember the causes. They are:
Though many surgical textbooks report that atelectasis is the most common cause of early post-operative fever, some even claiming that it is responsible for over 90% of febrile episodes in the first 48 hours after surgery; a recent review in CHEST (reference below) showed that there is no evidence to support this. We often see atelectasis in medical patients too, and few if any of them have fever. The CHEST review found that there was no clear evidence that atelectasis causes fever at all.
Pearl: Temperature >38.9C should raise concern for a true infection, where lower temperatures can be due to pulmonary embolism, DVT, drug fever, etc….
Mavros MN, Velmahos GC, Falagas ME.Atelectasis as a cause of postoperative fever: where is the clinical evidence? Chest. 2011 Aug;140(2):418-24. doi: 10.1378/chest.11-0127. Epub 2011 Apr 28. Review. PMID: 21527508
Category: Misc
Keywords: Frostbite (PubMed Search)
Posted: 1/7/2014 by Michael Bond, MD
Click here to contact Michael Bond, MD
Category: Pharmacology & Therapeutics
Keywords: Hypertension, treatment (PubMed Search)
Posted: 12/21/2013 by Michael Bond, MD
(Updated: 5/10/2026)
Click here to contact Michael Bond, MD
JNC8 (the Eigth Joint National Commission) released their recommendations for blood pressure management this week. The full article as published in JAMA can be found at http://jama.jamanetwork.com/article.aspx?articleid=1791497
Highlights from this report are
General Pearl: Remember to be cautious in acutely lowering the blood pressure in asymptomatic patients. Acute lowerings can cause watershed ischemia leading to strokes.
