Category: Orthopedics
Keywords: Runner, injury (PubMed Search)
Posted: 6/10/2017 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Shin Splints
Medial tibial stress syndrome (MTSS) aka shin splints is an overuse injury of the tibia
Very common
-10 to 15% of running injuries and over 50% of leg pain syndromes
3 Characteristics
1) Pain along the posteromedial border of the tibia
2) Diffuse pain
3) Pain that is activity related
Risk Factors
Female sex, increased weight, previous running injury, and
Higher navicular drop (amount of foot pronation) and
Greater hip external rotation with the hip in flexion
Differential Diagnosis
Tibial stress fracture, compartment syndrome, nerve entrapment (sural), lumbar radiculopathy and popliteal artery entrapment.
Category: Orthopedics
Keywords: Wrist fracture, splinting (PubMed Search)
Posted: 5/27/2017 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
High energy mechanism in younger patients
Falls more common in older patients
Higher incidence in older women due to osteoporosis
May indicate overall poor bone health
Avoid splinting in positions of flexion (palmer) and ulnar deviation
Palmer flexed positions may have a higher rate of displacement
Extra-articular fx, less than 5mm shortening of radius, Less than 5 degrees of dorsal angulation.
Consider fractures than are only stable in extreme positions to be unstable
If fx involves the ulnar styloid or DRUG (distal radial ulnar joint) place in long area posterior splint with arm in mid supination (anatomic position of forearm)
Category: Orthopedics
Keywords: Reverse Segond Fracture (PubMed Search)
Posted: 5/21/2017 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
It is common teaching that a Segond Fracture is associated with ACL tears. A reverse Segond fracture, avulsion fracture of the knee due to avulsion of the deep fibers of the medial collateral ligament, has also been described that was initially reported as associated with PCL tears. However, a more recent study has not been able to collaborate the PCL connection, but has shown that a reverse Segond fracture is associated with multiple ligamentous injuries to the knee.
Take home point: If you note a Reverse Segond fracture on your plain flips have the patient followup with orthopedics for a possible MRI, as they probably have other ligamentous injuries that might need treatment.
In the study by Peltola et al they looked at 11 years of patients who had CT of their knee and found 10 patiens with a reverse Segond fracture. They found "Reverse Segond fracture is a rare finding even in a level 1 trauma center. Cruciate ligament injuries appear to be associated with avulsion frac- ture, but every patient does not have PCL injury, as previously reported. Our results do not support the association of knee dislocation with reverse Segond fracture."
For a detailed discussion of Segond Fractures please visit Radiopaedia at https://radiopaedia.org/articles/segond-fracture
For Reverse Segond Fractures please visit https://radiopaedia.org/articles/reverse-segond-fracture
Category: Orthopedics
Keywords: Lateral knee pain (PubMed Search)
Posted: 5/13/2017 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Iliotibial band tendonitis
IT band is the continuation of the tensor fascia lata and inserts on the tibia at Gerdy's tubercle
Common cause of lateral knee pain seen in Primary care/Sports med clinics
Mechanism: May be due to excessive friction between the IT band and the lateral femoral condyle
Second most common overuse injury of the knee (PF syndrome). Not an acute event.
Affects up to15% of active individuals
Impingement zone is at 30 degrees of knee flexion
Most common in runners and cyclists
Pain localized over the lateral femoral condyle. Better w/ rest. Often occurs at a predictable distance into the run and not at onset.
Exacerbated with changes to mileage or running terrain.
Additional risks include poor shoes (best to change every 300 to 500 miles), excessive foot pronation (pes planus), quad versus hamstring strength asymmetry, weak hip ABductors, leg length discrepancy, tight IT band.
Category: Orthopedics
Keywords: Lisfranc Fracture (PubMed Search)
Posted: 4/29/2017 by Michael Bond, MD
(Updated: 5/1/2017)
Click here to contact Michael Bond, MD
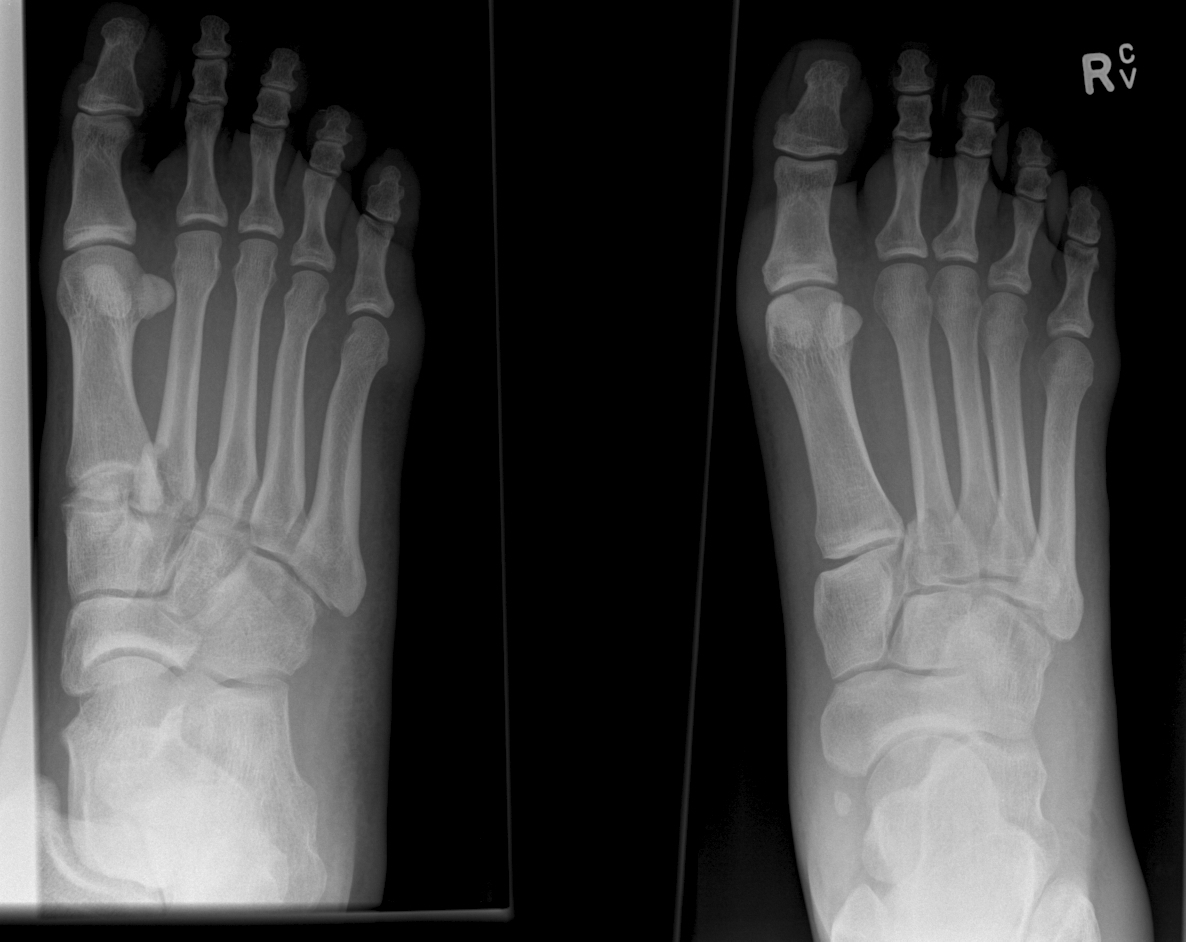
Lisfranc Fracture: Typically consists of a fracture of the base of the second metatarsal and dislocation, though it can also be associated with fractures of a cuboid.
Click below see image of fracture
Lisfranc Fracture:
Common current mechanism of injury is when a person steps into a hole and twists the foot. The original mechanism of injury that was described was when a horseman would fall of their horse with their foot still trapped in a stirrup.
Diagnosis should be considered if patient has difficultly weight bearing with pain on palpation over the 2nd and 3rdmetatarsals with an appropriate mechanism.
Category: Orthopedics
Keywords: Hip, pediatrics, arthritis (PubMed Search)
Posted: 4/22/2017 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Septic Arthritis in Children
Classic presentation: Pain, fever (may not always be present)
Limited range of motion of joint or refusal to bear weight,
Joint swelling (difficult to visualize in hip or shoulder),
Limb held in position that allows greatest capsular volume (elbow held in 30° flexion for example)
Diagnostic testing may include diagnostic markers (ESR, CRP) or imaging (US/MRI)
Most common organisms: Staph and Strep, Neisseria (adolescents), HACEK organisms, consider gram negatives in immunocompromised children
DDX: Transient synovitis, osteonercrosis or osteomyelitis, Psoas abscess, acute leukemia, Lyme disease
A common ED presentation is the child with the painful limp
35% of all cases of septic arthritis
>50% of cases occur in children younger than 2yo
Hip held in flexion, Abduction, external rotation
Fever and inflammatory markers are more sensitive than WBC count and refusal to bear weight
Kocher criteria:
1) Refusal to weight bear on affected side
2) Sed rate greater than 40mm/hr
3) Fever (>38.5°C
4) WBC count of >12,000 mm3
IF
- 4/4 criteria are met, there is a 99.6% chance of septic arthritis;
- when 3/4 criteria are met, there is a 93% chance of septic arthritis;
- when 2/4 criteria are met, there is a 40% chance of septic arthritis;
- when 1/4 criteria are met, there is a 3% chance of septic arthritis;
CRP can also be incorporated into a diagnostic algorithm
CRP>2.0 (mg/dl) in a child who refuses to bear weight yields a 74% probability of septic arthritis
https://www.ncbi.nlm.nih.gov/pubmed/10608376
Category: Orthopedics
Keywords: back pain, manipulation (PubMed Search)
Posted: 4/15/2017 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
We all wish there was a great treatment regimen for our patients with back pain. However, most studies have shown that it really does not matter what you do, as most patients will get better in 6 weeks.
A recent study published in JAMA looked at the role of spinal manipulation to improve pain and function in adults with low back pain. They looked at 26 randomized controlled trails and found that there was modest benefit for spinal manipulation and it was similar to using NSAIDs.
So spinal manipulation may or may not work for some patients. Something to consider along with physical therapy if patients are not getting relief with home remedies.
Category: Orthopedics
Keywords: EKG, athletes (PubMed Search)
Posted: 4/8/2017 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Most of our knowledge of the athlete’s EKG is based on white athletes.
African/Afro-Caribbean athletes are more likely to have an abnormal EKG than white athletes in multiple studies.
Different selective criteria have been developed to minimize classification of benign normal patterns as abnormal.
The 2010 ESC criteria classified 40.4% of black athletes as abnormal versus the Refined criteria which resulted in 11.5% of EKGs classified as abnormal.
This reduction was aided by the recognition that isolated anterior TWI in asymptomatic black athletes is considered a benign finding.
Note this does NOT apply if the TWI extend to the lateral leads
For example, T-wave inversion (TWI) was present in 23% of African/Afro-Caribbean athletes vs. 3.7% of white athletes (usually in contiguous anterior leads).
Other changes included a higher prevalence of early repolarization, RV hypertrophy, and LA/RA enlargement.
1) Jacob et al., 2016. Ethnic and Gender Specific Differences Among Athletes Participating in ECG Screening.
2 )WIlson et al., 2012. Significance of deep T-wave inversions in asymptomatic athletes with normal cardiovascular examinations: practical solutions for managing the diagnostic conundrum.
3) Brown et al., 2017. THe Complex Phentype of the Athlete's Heart: Implications for the Preparticipation Screening.
Category: Orthopedics
Keywords: team doctor, sports medicine (PubMed Search)
Posted: 3/25/2017 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Physicians are often called upon to serve as a team physician for a local high school in an official or unofficial capacity.
To aid in preparedness for sport-related emergencies, multiple national organizations have defined institutional best practices.
Knowledge of the following 3 best practice recommendations is important before taking on the role of “Doc covering the game”
1)The written Emergency Action Plan (EAP) – details the standard of emergency care at the particular venue.
2)The availability of life saving equipment: AED – where is it, charged and working?
3)Are the coaches trained in use of the AED and CPR. You can’t be everywhere and often multiple sporting events occur on campus simultaneously. It’s imperative that your first responder (coach or athletic trainer) can perform these tasks until you are able to respond
Please investigate these best practice recommendations before agreeing to serve as the physician for the local high school.
Category: Orthopedics
Keywords: stress fracture, runner (PubMed Search)
Posted: 3/11/2017 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
22yo college track athlete presents with 3 weeks of gradual onset groin and thigh pain, worse with running, better with rest.
Stress fractures are a common cause of groin pain in athletes, particularly in long distance runners
Fractures occur in the pubic rami and femoral neck
Ask about a sudden change in training regimens
PE: check for tenderness to deep palpation over the pubic ramus. Ask athlete to stand and support full weight on affected leg or perform one legged hop on affected side. Pain out of proportion to physical examination findings.
Imaging: XR usually negative. Bone scans can be positive as early as 4 to 8 days after symptom onset. MRI used to diagnose and rule out other causes of groin pain.
Treatment: Rest for 4 to 6 weeks. Consider making patient non weight bearing if walking causes pain especially with femoral neck fractures on the superior side. Inferior side neck fractures may benefit from prophylactic fixation.
Groin Injuries (Athletic Pubalgia) and return to play. Elattar et al., Sports Health Aug 2016.
Category: Orthopedics
Keywords: forearm trauma (PubMed Search)
Posted: 2/25/2017 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
The Essex-Lopresti injury pattern is the lesser known of the triad of forearm injuries (Monteggia & Galeazzi).
It follows the “rule of the ring” aka the life saver candy rule: You can’t break a life saver in just one place.
These injury patterns are frequently missed because our eyes are drawn to the fracture and miss the associated dislocation.
The Essex-Lopresti fracture pattern involves a fracture of the radial head with concomitant dislocation of the distal radio-ulnar joint (DRUG)
-With associated interosseous membrane disruption
Think of it as the Maisonneuve fracture of the forearm.
Mechanism: fall from height/high energy forearm trauma.
PE: Suspect if patient has significant tenderness at the DRUG with a radial head fx.
Patients have worse outcomes if injury is missed on initial presentation due to radial migration and instability.
Take home point: Remember the rule of the ring. Remember to exam the elbow with wrist injuries and the wrist with all elbow injuries
Category: Orthopedics
Keywords: Back Pain, Treatment (PubMed Search)
Posted: 2/18/2017 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
Treatment of Low Back Pain
A recent recommendation from the American College of Physicians (Internal Medicine) now recommends nonpharmacologic therapies as the first line treatment of acute or subacute lower back pain lasting 12 weeks or less. This might bring more people to our Emergency Departments so it is important that we know their current recommendations.
Some nonpharmacologic therapies recommended are:
For acute back pain they recommend:
For chronic back pain:
Category: Orthopedics
Keywords: nerve, entrapment (PubMed Search)
Posted: 1/28/2017 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
During a busy ED shift, your 40yo charge nurse asked you to look at his hand. He is known avid mountain biker. He has pain in his right 4th and 5th digits. . He feels a lack of coordination and a feeling of “clumsiness” of the hand. Where is his possible nerve compression and what do you expect to find on exam?
Ulnar nerve entrapment is sometimes called “handlebar palsy.”
Compression location is Guyon’s canal.
The ulnar nerve supplies the intrinsic muscles of the hand AND the extrinsic muscles for flexion of the 4th and 5th digits. This is what aids in a “power grip” and why he may have diminished grip strength on exam.
Also innervates the ADDuctor pollicis and 1st dorsal interosseous muscles (pinch)
Note the ulnar nerve also passes through the radial tunnel at the elbow. Entrapment here is called Radial tunnel syndrome or Cubital tunnel syndrome and causes forearm pain and paresthesias in the 4th and 5th digits with grossly normal motor and sensory function.
Category: Orthopedics
Keywords: Airway, wheezing, exercise (PubMed Search)
Posted: 1/14/2017 by Brian Corwell, MD
(Updated: 6/26/2021)
Click here to contact Brian Corwell, MD
You are covering a sporting event or working an ED shift when a young adolescent athlete without significant PMH presents with SOB and wheezing associated with exercise.
You immediately think exercise-induced asthma, prescribe a short-acting bronchodilator and pat yourself on the back.
While you may be right, there is increasing recognition of an alternative diagnosis
Exercise-induced laryngeal obstruction (EILO)
During high intensity exercise, the larynx can partially close, thereby causing a reduction in normal airflow. This results in the reported symptoms of SOB and wheezing.
This diagnosis has previously been called exercise induced vocal cord dysfunction. As the narrowing most frequently occurs ABOVE the level of the vocal cord, EILO is a more correct term.
While exercise induced bronchoconstriction has a prevalence of 5-20%, EILO is less common with a prevalence of 5-6%.
Patients are typically adolescents, with exercise associated wheezing and SOB, frequently during competitive or very strenuous events. Wheezing is inspiratory and high-pitched. Symptoms are unlikely to be present at time of medical contact unless you are at the event as resolution occurs within 5 minutes though associated cough or throat discomfort can persist after exercise cessation. EIB symptoms typically last up to 30 minutes following exercise.
Inhaler therapy is unlikely to help though some athletes report subjective partial relief. This may be explained as approximately 10% of individuals have both EIB and EILO.
In athletes with respiratory symptoms referred to asthma clinic, EILO was found in 35%.
Consider EILO in athletes with unexplained respiratory symptoms especially in those with ongoing symptoms despite appropriate therapy for EIB.
Category: Orthopedics
Keywords: DVT, Leg, Cast (PubMed Search)
Posted: 12/31/2016 by Michael Bond, MD
Click here to contact Michael Bond, MD
Take Home Point:
Low-molecular-weight heparin doesn't seem to prevent symptomatic venous thromboembolism (VTE) in patients undergoing knee arthroscopy or lower leg casting, suggest two trials in the New England Journal of Medicine.
The study was conducted by Dutch researcheers and randomized 1500 patients who underwent lower leg casting or knee arthoscopy to receive no anticoagulation or low molecular weight heparin. Patients were either treated for the entire duration of immobilzation or 8 days after their surgery (arthroscopy patients)
The rates of VTE in patients at 3 months of follow up where arthroscopy: 0.7% vs. 0.4%; casting: 1.4% vs. 1.8%. So overall very low rates of VTE, and no real difference between the groups.
A large cohort might have shown some benefit, but since the incidence is so low there is probably no reason to prophlactically treat these patients and increase their risk of major bleeding events, which was also low in the study.
The article can be found at http://www.nejm.org/doi/full/10.1056/NEJMoa1613303?query=pfw&jwd=000100949960&jspc=EM
van Adrichem RA, Nemeth B, Algra A, le Cessie S, Rosendaal FR, Schipper IB, et al. Thromboprophylaxis after Knee Arthroscopy and Lower-Leg Casting. N Engl J Med 2016.
Category: Orthopedics
Keywords: Concussions, musculoskeletal injury (PubMed Search)
Posted: 12/24/2016 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Significant associations were found between concussion and
Lateral ankle sprain (P = 0.012)
Knee injury (P = 0.002)
Lower extremity muscle injury (P = 0.031)
Keep in mind that 50 – 80% of concussions may go undiagnosed or unreported.
A discussion about risks of early return after concussion should include mention of risks beyond repeat head injury/2nd impact syndrome
Study limits: Retrospective design limits ability to establish causation/reporting bias
Gilbert, Burdette, et al., 2016 Association between concussion and lower extremity injuries in collegiate athletes. Sports Health 8 (6), 561-567.
Category: Orthopedics
Keywords: Ankle Sprains (PubMed Search)
Posted: 11/26/2016 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Incidence and Cost of Ankle Sprains US Emergency Departments
In a sample of 225,114 ED patients with ankle sprains:
Lateral ankle sprains represent the vast majority of all ankle sprains (91%).
Lateral ankle sprains incur greater ED charges than medial sprains ($1008 vs. $914).
Lateral ankle sprains were more likely to have associated pain in the limb, sprain of the foot and abrasions of the hip/leg than medial sprains.
Medial sprains were more likely to include imaging.
Hospitalizations were more likely with high ankle sprains than lateral sprains.
There is a higher incidence of ankle sprains in younger patients (≤25 years) and in female patients (57%).
Shah et al., 2016. Incidence and Cost of Ankle Sprains in United States Emergency Departments. Sports Health Novemebr 2016.
Category: Orthopedics
Posted: 11/12/2016 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
https://images.radiopaedia.org/images/3173801/1ee24da1a6fe907a27d2bf20481174.jpg
Young toddler presents with left lower leg pain. What is the diagnosis??
Metaphyseal Corner Fracture.
These are often very subtle findings! This fracture pattern was first seen in association with children with subdural hematomas.
https://images.radiopaedia.org/images/3173808/48ab0d13eb24f10de978b5c65af064_jumbo.jpg
It occurs due to shearing forces on the growth plate.
Most frequently seen in the distal femur, proximal humerus and tibia.
Can be bilateral.
Similar to bucket handle fracutres
Category: Orthopedics
Keywords: MI, exercise (PubMed Search)
Posted: 10/15/2016 by Brian Corwell, MD
(Updated: 10/22/2016)
Click here to contact Brian Corwell, MD
Many of us use exercise as a coping strategy when emotionally stressed or to blow off steam when angry. This may place your heart at risk.
A recent observational study in Circulation surveyed 12,000 first MI patients about potential triggers. The associations didn't depend on age, smoking status, hypertension, or baseline physical activity.
Anger or emotional upset in the hour before onset elevated odds of MI 2.44 fold
A similar 2.31 fold elevation was observed form heavy exertion
However, the combination of the two raised the odds to 3.05 fold (P<0.001 for interaction)
http://circ.ahajournals.org/content/134/15/1059
Category: Orthopedics
Keywords: Davos, Shoulder, Reduction (PubMed Search)
Posted: 10/15/2016 by Michael Bond, MD
Click here to contact Michael Bond, MD
Davos Shoulder Reduction Technique
Take Home Points
Interested, well find out more by watching this video by Larry Mellick https://www.youtube.com/watch?v=u2MsnjVNoPM or clicking the link below.
The Davos technique is a novel technique that requires no exertion on the part of the provider and can be done without sedation
Do the technique by:
The original article can be found here http://www.jem-journal.com/article/S0736-4679(16)00030-5/abstract
