Category: Visual Diagnosis
Keywords: ultrasound, ectopic, free fluid, hypotension, pregnancy (PubMed Search)
Posted: 2/27/2011 by Haney Mallemat, MD
(Updated: 8/28/2014)
Click here to contact Haney Mallemat, MD
24 yo woman presents with syncope, abdominal pain, and normal menses 4 days prior. Urine HCG(+) and quantitative beta-HCG is 1300 with the transvaginal ultrasound seen below. Diagnosis?
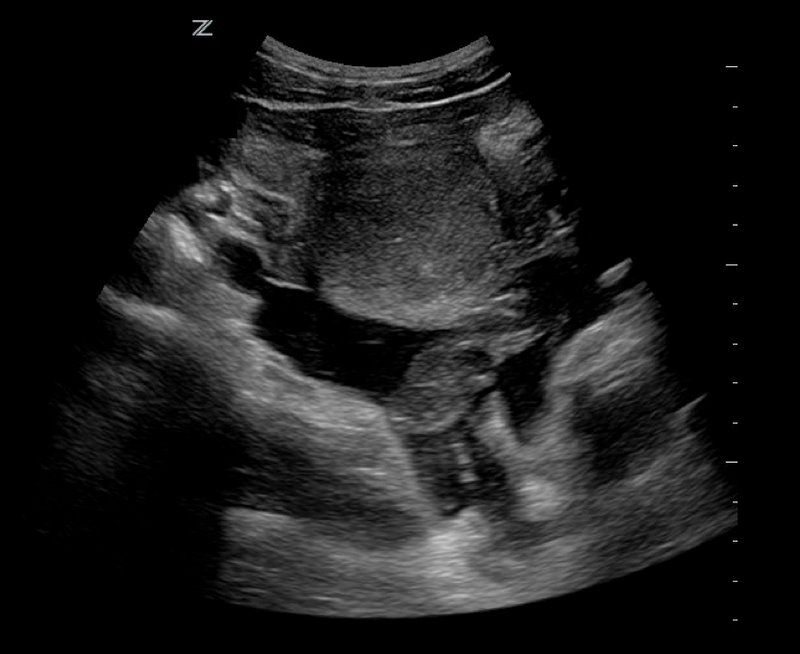
Ectopic Pregnancy Pearls
Tintinalli, Judith, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7th Edition. 2011, McGraw-Hill Companies, Inc, China
Category: Critical Care
Keywords: Pulmonary embolism, PE, echocardiography, ultrasound, hemodynamics, McConnell sign, right ventricle (PubMed Search)
Posted: 2/15/2011 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
Casazza F., et al. Regional right ventricular dysfunction in acute pulmonary embolism and right ventricular infarction.Eur J Echocardiography 2005 Jan; 6(1): 11-4.
Category: Trauma
Keywords: blunt trauma, pneumothorax, CXR supine, ultrasound, seashore, stratasphere (PubMed Search)
Posted: 2/14/2011 by Haney Mallemat, MD
(Updated: 8/28/2014)
Click here to contact Haney Mallemat, MD
(Please note the prior version of this pearl was incorrect with respect to the images referenced. This version is corrected.)
Patient s/p blunt chest trauma. CXR (image 1) vs. lung ultrasound (image 2), do you see any inconsistencies?
Lung ultrasound in traumatic pneumothorax: The "Stratosphere Sign"
Written by Dr. Michael Allison.
For advanced sonographers:
1. Blaivas, M. et al. A prospective comparison of supine chest radiography and bedside ultrasound for the diagnosis of traumatic pneumothorax. Academic Emergency Med. 2005 Sep;12(9):844-9.
2. Lichtenstein D et al. Ultrasound diagnosis of occult pneumothorax. Crit Care Med. 2005 June;33(6): 1231-8.
Category: Critical Care
Keywords: hemoglobin, anemia, transfusions, hemorrhage, conservative, liberal, hemorrhaging (PubMed Search)
Posted: 2/1/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
The optimal hemoglobin concentration during critical illness is unknown. Although a liberal transfusion strategy (Hb 10-12 g/dL) was once believed to be beneficial for hemodynamics, evidence suggests targeting a conservative strategy (Hb 7-9 g/dL) does not increase mortality, while the unnecessary transfusion of blood products can cause harm (transfusion associated lung injury, infection, etc.) in the non-hemorrhaging patient.
1. Harder, L. Et al. The Optimal Hematocrit. Critical Care Clinics (2010) vol. 26 (2) pp. 335-354
2. Hebert P, Wells G, Blajchman M, et al. A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. N Engl J Med 1999; 340(6):409–17
Category: Trauma
Keywords: Apical cap, dissection, blunt aortic injury, chest xray, radiology (PubMed Search)
Posted: 1/31/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
44 y/o female restrained driver s/p motor vehicle crash complaining of chest pain and shortness of breath.
Answer: Left pleural apical cap.
The Apical Cap
An apical cap is a unilateral or bilateral irregular density over the apex of the lung, generally less than 5mm. The lower border is often sharp but undulating.
Differential diagnosis:
Fabian TC, Richardson JD, Smith JS Jr, et al. Prospective study of blunt aortic injury: multi-center trial of the American Association for the Surgery of Trauma. J Trauma 1997;42:374-383.
McLoud TC, Isler RJ, Novelline RA, et al. The apical cap. Amer J Rad 1981; 137:299-306.
Rivas LA, Fishman JE, Munera F, et al. Multislice CT in thoracic trauma. Radiol Clin North Am2003; 41:599-616.
Category: Critical Care
Keywords: Apnea test, brain death, brain stem death, coma, death, cardiopulmonary death (PubMed Search)
Posted: 1/17/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Brain death is the permanent absence of cerebral and brainstem functions (coma, absent pupillary reflexes, no spontaneous respiration, etc.). Legally, brain death is equivalent to cardiopulmonary death.
If brain death is suspected, confirmation is necessary. The apnea test is most commonly used, evaluating for spontaneous breaths when disconnected from the ventilator. If apnea testing is not possible (e.g., ambiguous clinical exam or cardiopulmonary instability) ancillary testing is needed:
Wijdicks EF, The diagnosis of brain death. N Engl J Med. 2001 Apr 19;344(16):1215-21.
Category: Visual Diagnosis
Keywords: boxer's, fracture, orthopedics, hand, brawler's, radiology, xray (PubMed Search)
Posted: 1/17/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
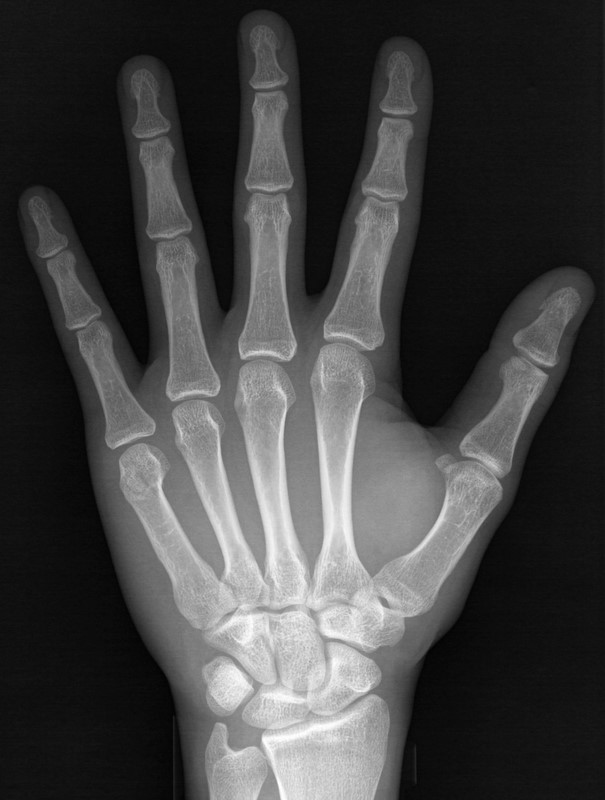
Boxer's (or Brawler's) Fracture
Many thanks to Dr. George Kochman for submitting this case!
Category: Critical Care
Keywords: PRES, hypertensive crisis, seizures, visual loss, ecclampsia, hypertensive emergency, cyclopsporine, tacrolimus (PubMed Search)
Posted: 1/4/2011 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Posterior reversible encephalopathy syndrome (PRES) is a syndrome of visual loss, headache, altered mental status, and seizures, typically with severe hypertension. PRES usually occurs with hypertensive encephalopathy or ecclampsia, although cyclosporin and tacrolimus use have been implicated.
PRES is due to a combination of endothelial damage, impaired auto-regulation and increased cerebral perfusion pressure. Classic CT and MRI findings are parietal-occipital, cerebellar, or brainstem cortical and subcortical edema.
Early recognition and symptomatic treatment is key; IV anti-hypertensives (hypertensive encephalopathy), anti-epileptics (seizures), IV magnesium and emergent delivery (ecclampsia), and discontinuing offending medications (cyclosporin and tacrolimus).
With treatment, partial to complete recovery is normal, although residual neurological and visual deficits may persist.
Pula, J. Posterior reversible encephalopathy syndrome. Current Opinion in Ophthalmology. 2008 vol. 19 (6) pp. 479-84
Category: Critical Care
Keywords: thrombocytopenia, critically0ill, sepsis, death, mortality, prognosis (PubMed Search)
Posted: 12/21/2010 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
The incidence and prevalence of thrombocytopenia in the ICU is poorly defined however, it has been found to be an independent predictor of death in the critically-ill. Increased mortality does not appear to be related to bleeding complications. On the other hand, survivors of critical illness tend to recover platelet faster as compared to non-survivors.
Thrombocytopenia in the critically-ill is a marker for systemic inflammation/infection although the exact mechanisms are unknown. Common risk factors associated with thrombocytopenia in the ICU population are:
Sepsis
Renal failure
High-illness severity
Organ dysfunction
Bottom line: Thrombocytopenia in the critically-ill is associated with increased mortality.
Hui, P., The Frequency and Clinical Significance of Thrombocytopenia Complicating Critical Illness: A Systematic Review. Chest. 2010 Nov 11. [Epub ahead of print]
Category: Critical Care
Keywords: Antibiotics, linezolid, serotonin syndrome, delirium, critical care (PubMed Search)
Posted: 12/7/2010 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Linezolid is used for gram-positive infections resistant to conventional therapy (e.g., Vancomycin-resistant enterococcus and Methicillin Resistant Staph Aureus). Linezolid is an oxazolidinone, but more importantly it is a weak monoamine oxidase inhibitor (MAOI) and serotonin syndrome (e.g., altered mental status, neuromuscular abnormalities, autonomic instability) may occur when combined with selective serotonin re-uptake inhibitors (SSRIs) or with recent discontinuation of SSRI.
Be aware that the following drugs can precipitate serotonin syndrome when combined with Linezolid:
Mirtazpine Buproprion Fentanyl
Trazodone Buspirone Bromocryptine
Levodopa Lithium Amphetamines
Cocaine Codeine Reserpine
Ergots MAOI's
Narita, M. Linezolid-Associated Peripheral and Optic Neuropathy, Lactic Acidosis, and Serotonin Syndrome Pharmacotherapy (2007) vol. 27 (8) pp. 1189-97
Category: Critical Care
Keywords: Status epilepticus, non-convulsive, altered mental status, seizure, critical care, ICU, neurology (PubMed Search)
Posted: 11/23/2010 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Non-Convulsive Status Epilepticus (NCSE) is generally under reported. An ICU study found 10% admissions for altered mental status (AMS) were eventually diagnosed as NCSE.
Pearls:
- Include NCSE in the AMS differential
- NCSE may occur with or without convulsive seizures
- Difficult to distinguish from a post-ictal state (14% of convulsive seizures convert to
NCSE)
- Reported mortality is up to 44%
Consider NCSE when:
- Seizure history / recent seizures
- Post-ictal period >1 hour
- Odd behaviors (e.g., chewing, blinking, personality change) and abnormal eye
movements (86% specific)
- AMS without structural, metabolic or traumatic etiology
- Patient intubated for status epilepticus
If you are unsure but suspicious of NCSE order a STAT EEG. Treat NCSE like a convulsive status.
Slattery, D. Seizures as a cause of altered mental status. Emerg Med Clin North Am. 2010 Aug;28(3):517-34.
Category: Critical Care
Keywords: ultrasound, ocular, sonography, intracranial pressure, optic nerve sheath, ICP (PubMed Search)
Posted: 11/9/2010 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Ocular sonography is a fast, simple, and non-invasive tool to detect elevated intracranial pressure (ICP) by measuring the optic nerve sheath diameter (ONSD). Several studies have shown a positive correlation between increased ONSD (>5.7mm) and elevated ICP (>20mmHg). Although ultrasound may not replace CT or MRI to diagnose the cause of the increased ICP, its use as a triage tool can expedite these tests.
The technique:
Please see the references below for more information and, as with any new technique please consult local experts prior to making clinical decisions.
http://www.sonoguide.com/smparts_ocular.html
Soldatos, T. et al. Optic nerve sonography in the diagnostic evaluation of adult brain injury. Crit Care. 2008; 12(3): R67. Epub 2008 May 13.
Category: Critical Care
Keywords: delirium, dementia, ICU, (PubMed Search)
Posted: 10/25/2010 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
Increasing literature demonstrates ICU delirium is bad. Delirium in mechanically ventilated patients is an independent predictor for long-term cognitive defects (e.g., managing money, following detailed instructions, reading maps, and developing dementia). The cited study found 80% of patients with ICU delirium had cognitive dysfunction at three months, and 70% had residual dysfunction at one year (33% had severe dysfunction).
You must be aggressive to prevent delirium:
- Implement daily assessment tools (e.g., CAM-ICU)
- Daily awakening and spontaneous breathing trials
- Early patient mobilization
- Aggressive pharmacological treatment of delirium
- For more information: www.icudelirium.org
Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Girard, T., et al. Crit Care Med. 2010 Jul;38(7):1513-20.
Category: Critical Care
Keywords: asthma, heliox, airway (PubMed Search)
Posted: 10/12/2010 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
Heliox is a mixture of oxygen and helium resulting in a gas less dense than air. In asthma, airway resistance causes turbulent airflow which increases the work of breathing. Heliox reduces airway resistance by increasing laminar airflow.
Benefits:
Better lung mechanics
Improved nebulizer delivery
Few known side-effects/complications
Drawbacks:
Expensive
Contraindicated in hypoxemic patients.
Paucity of large prospective randomized trials.
McGarvey JM, Pollack CV. Heliox in Airway Management. Emerg Med Clin North Am. 2008 Nov;26(4):905-20, viii.
Category: Critical Care
Keywords: HAART HIV AIDS Critical illness (PubMed Search)
Posted: 9/27/2010 by Haney Mallemat, MD
(Updated: 9/28/2010)
Click here to contact Haney Mallemat, MD
While you should always involve ID consultants when managing critically-ill HIV/AIDS patients on HAART, consider this; sub-therapeutic levels of anti-retrovirals may promote HIV resistance, potentially invalidating a class of drug for future use. Therefore, it may be advantageous to discontinue the drug(s) during critical-illness to avoid resistance.
Two examples leading to sub-therapeutic HAART levels in critical-illness:
Current issues in critical care of the human immunodeficiency virus-infected patient. Morris A, Masur H, Huang L Crit Care Med. 2006 Jan;34(1):42-9.
Category: Critical Care
Keywords: Necrotizing Soft Tissue Infections, sepsis, critical care, surgery (PubMed Search)
Posted: 9/13/2010 by Haney Mallemat, MD
(Updated: 9/14/2010)
Click here to contact Haney Mallemat, MD
(Sorry for the previously mislabeled pearl...)
Necrotizing soft tissue infections (NSTI) are on the rise and, despite improved surgical and critical care, over the years there has only been a mild reduction in mortality. Survival is associated with early diagnosis and treatment. Unfortunately, NSTI are not always obvious because deeper tissues made be involved first. Despite a validated scoring system and better radiology, our clinical suspicion still rules and relies on a meticulous history and physical exam.
Here are some subtle signs of NSTI:
Pain out of proportion to exam
Edema beyond region of erythema
Skin anesthesia
Skin erythema and/or hyperthermia
Epidemolysis
Skin bronzing
If NSTI is suspected, be vigilant! Start broad-spectrum antibiotics, begin appropriate resuscitation and involve your surgeons early.
Necrotizing soft tissue infections in the intensive care unit. Crit Care Med. 2010 Sep; 38: S460-8. Phan HH, et al.
Category: Critical Care
Keywords: SIADH, CSW, syndrome of inappropriate adh, cerebral salt wasting, hyponatremia, neurosurgery (PubMed Search)
Posted: 8/30/2010 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
Hyponatremia plagues many neurosurgical patients due to the syndrome of inappropriate secretion of ADH (SIADH) or the cerebral salt wasting syndrome (CSW). Both diseases may appear similar (hyponatremia, increased urine osmolarity, increased urine sodium, normal adrenal, renal and thyroid function), but there is one BIG difference. Patients with SIADH are euvolemic or hypervolemic (excess ADH causes fluid retention) whereas patients with CSW are fluid depleted (impaired renal handling of sodium and water). To differentiate, look for signs of hypovolemia: orthostatics, dry mucus membranes, hemoconcentration, pre-renal azotemia, and/or hemodynamics (IVC collapse anyone?).
Bottom line: Distinguish SIADH from CSW because the treatments are exact opposites:
SIADH: Fluid restrict
CSW: Give water and salt (i.e., 0.9% saline)
Cerebral salt wasting syndrome: a review. Harrigan MR
Neurosurgery. 1996 Jan;38(1):152-60.
Category: Critical Care Literature Update
Keywords: Subclavian,ultrasound, cvc, central venous catheter (PubMed Search)
Posted: 8/17/2010 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
2. Distinguish artery from vein with compression and/or Doppler.*
3. Sterilely prep the site and ultrasound probe.
4. Cannulate the vein in the transverse or longitudinal plane.
Category: Visual Diagnosis
Posted: 1/14/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
50 year-old male with cough and dyspnea. What's the diagnosis?
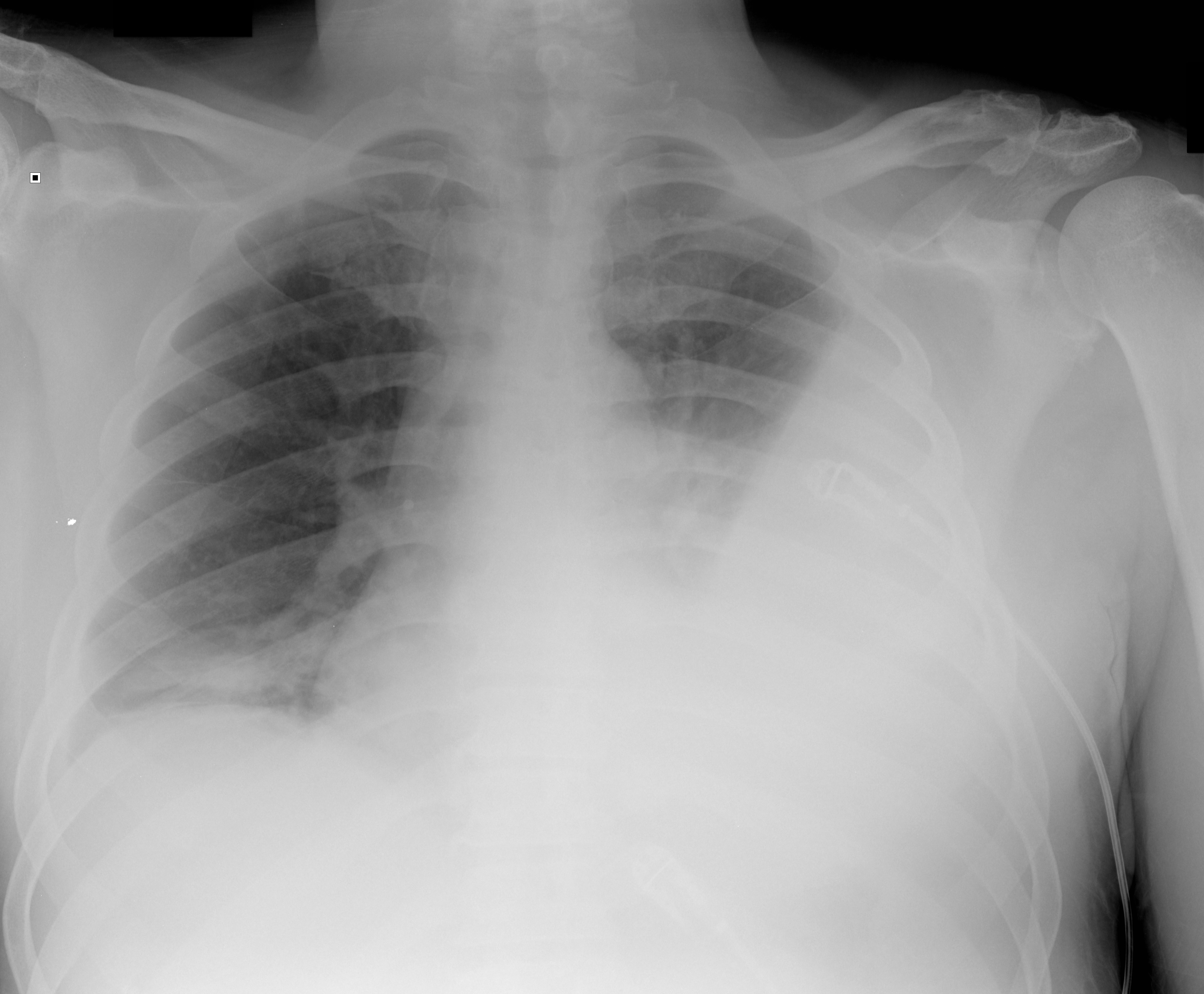
Here's your answer: http://www.youtube.com/watch?v=Z4yxqRoKX04&feature=youtu.be
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Posted: 4/12/2013 by Haney Mallemat, MD
(Updated: 5/10/2026)
Click here to contact Haney Mallemat, MD
Adrenal insufficiency (AI) can be a life-threating condition and is classified as primary (failure of the adrenal gland) or secondary (failure of hypothalamic- pituitary axis).
Common causes of primary adrenal insufficiency include autoimmune destruction, infectious causes (TB and CMV), or interactions with drugs (e.g., anti-fungals, Etomidate, etc.). Secondary causes are usually due to abrupt withdrawal of steroids after chronic use, although sepsis and diseases of the hypothalamus or pituitary (e.g., CVA) may occur.
Signs and symptoms include fatigue, weakness, skin pigmentation, dizziness, abdominal pain, and orthostatic hypotension; it should be suspected with any of the following: hyponatremia, hyperkalemia, hypoglycemia, hypercalcemia, low free-cortisol level, and hemodynamic instability despite resuscitation.
Treatment:
• Correct underlying the disorder
• Resuscitation and hemodynamic support
• Correct hypoglycemia and electrolyte abnormalities
• Treat with hydrocortisone, cortisone, prednisone, or dexamethasone +/- fludrocortisone (Note: dexamethasone is attractive choice in the ED because it will not interfere with ACTH stimulation test)
Neary, N and Nieman, L. Adrenal Insufficiency: Etiology, diagnosis and treatment. Curr Opin Endocrinol Diabetes Obes. 2010 Jun;17(3):217-23.
