Category: Critical Care
Posted: 8/7/2012 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Lung Protective Ventilator Settings Still Underutilized
Needham DM, et al. Lung protective mechanical ventilation and two-year survival in patients with acute lung injury: A prospective cohort study. BMJ 2012;344:e2124.
Category: Critical Care
Posted: 7/31/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Crystalloids (i.e., 0.9% saline and lactated ringers) have been used during resuscitation for more than a century. Their invention, however, was more accidental than intentional.
Crystalloids were first used during the European Cholera epidemic of 1831. Hartog Hamburger later modified this solution in 1896 to the solution we know today as "normal" saline. Hamburger's solution was only intended for in vitro study of RBC lysis and was never intended for clinical use.
Around this time, Sydney Ringer was testing several fluids to use for physiologic studies. Ringer's lab assistant was erroneously substituting tap water for distilled water when preparing these solutions. Ringer later discovered that this tap water contained minerals making the solution "physiologic", isotonic, and safe for human use; Alexis Hartmann later added sodium lactate to create Ringer's Lactate.
Since the invention of crystalloids, many types of resuscitation fluids have been created and studied (i.e., albumins, gelatins, and starches); all have been shown to be more expensive, with no more benefit, and with possibly more harm when compared to crystalloids.
The "perfect" resuscitation fluid still alludes us today, but of all of the solutions marketed crystalloids are arguably the best...despite their accidental history.
Awad, S. et al. The history of 0.9% saline. Clinical Nutrition 2008 Apr;27(2):179-88.
Follow me on Twitter (@criticalcarenow) and Google+ (+haney mallemat)
Category: Critical Care
Posted: 7/24/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Steroids and Septic Shock
Sherwin RL, Garcia AJ, Bilkovski R. Do low-dose corticosteroids improve mortality or shock reversal in patients with septic shock? A systematic review and position statement prepared for the American Academy of Emergency Medicine. JEM 2012;43:7-12.
Category: Critical Care
Posted: 7/17/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Wernicke encephalopathy (WE) is a neurologic disorder secondary to prolonged thiamine deficiency; it is characterized by confusion, ataxia, and ocular abnormalities.
Traditional medical teaching advises against the administration of glucose (or glucose containing fluid) in thiamine deficient patients, without first giving thiamine, as this may precipitate WE.
This teaching is problematic, however, in hypoglycemic patients who require the immediate administration of glucose while simultaneously being suspected of thiamine deficiency (e.g., malnourished alcoholics). Delays in treating hypoglycemia may be more harmful (e.g., seizures, permanent neurologic deficits, etc.) than the risk of WE.
Schabelman et. al performed a literature search to unearth the origins of this teaching. Nineteen papers related to this topic were found consisting of case reports, animal studies, and expert opinion; there were no randomized trials, cohort studies, or case-control studies.
Bottom-line: The available evidence does not support withholding glucose treatment until thiamine can be administered and educators should consider abolishing this dogmatic teaching until better evidence is available.
Schabelman, et al. Glucose before thiamine for Wernicke encephalopathy: a literature review. J Emerg Med. 2012 Apr; 42(4): 488-94
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 7/10/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Anaphylaxis
De Bisschop MB, Bellou A. Anaphylaxis. Curr Opin Crit Care 2012; 18:308-17.
Category: Critical Care
Keywords: hydroxyethyl starch crystalloid, colloid, lactated ringers, normal saline, resuscitation, sepsis, hypotension (PubMed Search)
Posted: 7/3/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Septic patients with hemodynamic instability often require intravenous fluids as part of their resuscitation. Major debate has occurred whether the optimal resuscitation fluids are crystalloids (e.g., normal saline) or colloids (e.g., albumin).
In theory, colloids are more potent intravascular expanders than crystalloids because their oncotic pressure is higher and should increase intravascular volume similarly to larger amounts crystalloid (i.e., colloids require less volume during resuscitation).
Despite these theoretical benefits, the colloid hydroxyethyl starch (HES), has come under scrutiny after prior studies have linked its use with adverse outcomes.
A recent prospective randomized-control trial compared the use of HES to lactated acetate for resuscitating septic patients and found that HES significantly increased both the incidence of renal-replacement therapy and mortality at 90 days (both primary end-points in the study).
Bottom line: There is no convincing data that HES performs superiorly to crystalloid for resuscitation in sepsis and there is increased harm with its use. Furthermore, the increased cost of HES compared to crystalloids does not justify its routine use.
Perner A., et al. Hydroxyethyl Starch 130/0.4 versus Ringer's Acetate in Severe Sepsis. NEJM. 2012 Jun 27.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 6/26/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Acute Kidney Injury and Tumor Lysis Syndrome
McCurdy MT, Shanholtz CB. Oncologic emergencies. Crit Care Med 2012; 40:2212-2222.
Category: Critical Care
Posted: 6/19/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Two recently presented abstracts at the 2012 Society of Critical Care Medicine conference suggest that the combination of vancomycin and piperacillin-tazobactam may lead to acute kidney injury (AKI) in the critically ill. There may also be evidence to suggest that piperacillin-tazobactam alone increases the risk of AKI.
Both abstracts retrospectively compared patients who received either vancomycin alone or the combination of vancomycin and piperacillin-tazobactam. In both studies, the rates of AKI were significantly lower in patients treated with vancomycin alone as compared to patients receiving both vancomycin and piperacillin-tazobactam.
Bottom line: Although the current evidence does not support a change in our clinical practice, more prospective studies exploring this topic are necessary.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Min, et al. Acute Kidney Injury in Patients Recieving Concomitant Vancomycin and Piperacillin/Tazobactam. Critical Care Medicine. December 2011. 39(12); p 200
Hellwig, et. al. Retrospective Evaluation of the Incidence of Vancomycin and/or Piperacillin-Tazobactam Induced Acute Renal Failure. Critical Care Medicine. December 2011. 39(12); p 79
Category: Critical Care
Posted: 6/13/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Use the Measured Sodium Concentration!
Beck, L. Cleveland Clin J Med 2001;68:673.
Category: Critical Care
Posted: 6/4/2012 by Haney Mallemat, MD
(Updated: 6/5/2012)
Click here to contact Haney Mallemat, MD
Consider rhabdomyolyisis secondary to heat exposure as summertime approaches; have a low threshold to screen patients if they are at risk (e.g., people exercising in high-ambient temperatures).
Symptoms include muscle tenderness, cramping, and swelling with associated weakness. Patients with altered mental status (e.g., heat stroke) should be examined for limb induration, skin discoloration (i.e., ischemia), or compartment syndrome.
Complications:
Treatment
Khan, F. Y. Rhabdomyolysis: a review of the literature. The Netherlands journal of medicine, 67(9), 272 – 283.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 5/29/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Severe UGIB
Srygley FD, et al. Does this patient have a severe upper gastrointestinal bleed? JAMA 2012;307:1072-9.
Category: Critical Care
Posted: 5/21/2012 by Haney Mallemat, MD
(Updated: 5/22/2012)
Click here to contact Haney Mallemat, MD
Carcinoid tumors are neuroendocrine malignancies typically located in the GI tract; most commonly in the terminal ilium and appendix.
Carcinoid tumors produce serotonin, histamine, bradykinin, and/or prostaglandin that result in diarrhea, facial flushing, or bronchospasm. These vasoactive substances may also lead to hypotension and vasodilatory shock.
The tumor may also affect the tricuspid and pulmonary valves leading to right-heart failure secondary to valvular regurgitation, stenosis or both.
Treatment is directed at controlling the malignancy (e.g., octotrotide and tumor resection) as well as managing the right-sided heart failure when it occurs (e.g., inotropes, diuretics, vasopressors, etc.).
Fox, D. J. (2004). Carcinoid heart disease: presentation, diagnosis, and management. Heart, 90(10), 1224–1228
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 5/15/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Balloon Tamponade for Variceal Bleeding
Category: Critical Care
Posted: 5/8/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Severe acute pancreatitis (SAP) is a life-threatening form of pancreatitis, with up to 30% mortality.
SAP may lead to hypovolemic shock (secondary to vasodilation and capillary leak), hypoxemia (from acute respiratory distress syndrome), and multi-organ failure.
Suspect SAP with signs and symptoms of pancreatitis plus any of the following:
Treatment of SAP should focus on:
Greer, S. E., & Burchard, K. W. (2009). Acute pancreatitis and critical illness: a pancreatic tale of hypoperfusion and inflammation. Chest, 136(5), 1413–1419.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Keywords: spontaenous bacterial peritonitis, hepatorenal syndrome, albumin (PubMed Search)
Posted: 5/1/2012 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
SBP, HRS, and Albumin
Bernardi M, et al. Human albumin in the management of complications of liver cirrhosis. Crit Care 2012; 16:211.
Category: Critical Care
Posted: 4/24/2012 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Mediastinitis is an infection of the mediastinum; a rapidly fatal surgical emergency if not recognized and treated early.
Causes include esophageal perforation, oropharyngeal infections (e.g., Ludwig’s angina), prevertebral or carotid space infections, and iatrogenically (endoscopy, hypopharyngeal perforations during intubation, etc.).
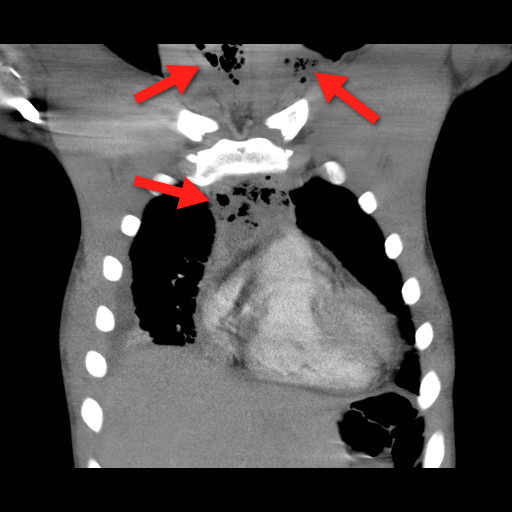
Plain films (neck / chest) may serve as a screening tool, but CT best defines the source and extent of disease; the CT below demonstrates gas within the soft-tissues and the mediastinum (red arrrows).
Infections may be polymicrobial and broad-spectrum antibiotics with anaerobic coverage (e.g., pipercillin-tazobacam) should be started initially.
Immediate treatment should also include:
Bonus Pearl
Can't keep up with all the great educational stuff in Emergency Medicine and Critical Care? Let the professionals at Life in the Fastlane do it for you (http://lifeinthefastlane.com). These guys scour the web and blog about the best educational pearls, podcasts, and radoiolgic finds...and they're also quite the laugh. Check them out today!
Ridder G, et al. Descending necrotizing mediastinitis: contemporary trends in etiology, diagnosis, management, and outcome. Ann Surg. Mar 2010;251(3):528-34.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 4/17/2012 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Cuff Pressures and the Prevention of VAP
Grap MJ, et al. Ventilator-associated pneumonia: The potential critical role of emergency medicine in prevention. JEM 2012; 42:353-362.
Category: Critical Care
Posted: 4/9/2012 by Haney Mallemat, MD
(Updated: 8/12/2014)
Click here to contact Haney Mallemat, MD
Sepsis is one of the top 10 causes of death in the U.S. and its incidence is on the rise.
The financial burden of sepsis is also growing; it is estimated that between 2000 and 2005 the overall cost of ICU hospitalization rose from $56.6 billion to $81.7 billion per year with severe sepsis accounting for $16.7 billion.
Although we may not be able to immediately modify the incidence of community-acquired sepsis, hospital-acquired sepsis can be reduced; for example, many cases of nosocomial sepsis are associated with catheter blood stream infections secondary to central-lines.
There are several simple strategies to prevent catheter-related blood-stream infections:
Remember: We play a large role in reducing nosocomial sepsis; be vigilant about your sterile techniques during central catheter insertions and question the need for every single line.
Bonus pearl (only for iPhone): MDRNTools is a FREE app (that’s right, FREE!) with lots of ED and ICU applications such as an IV med calculator, an RSI handbook, a Stroke Scale calculator, and more.
Download http://itunes.apple.com/us/app/mdrntools/id505794224?mt=8&ls=1
Chalupka, A. N., & Talmor, D. (2012). The Economics of Sepsis. CCC, 28(1), 57–76.
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
Category: Critical Care
Posted: 4/3/2012 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Transferring Multidrug-Resistant Organisms
Morgan DJ, et al. Transfer of multidrug-resistant bacteria to healthcare workers' gloves and gowns after patient contact increases with environmental contamination. Crit Care Med 2012; 40:1045-1051.
Category: Critical Care
Keywords: apnea time, rapid sequence intubation, atelectasis, crticial care, intubation, hypoexemia, obesity (PubMed Search)
Posted: 3/26/2012 by Haney Mallemat, MD
(Updated: 3/27/2012)
Click here to contact Haney Mallemat, MD
The supine position during rapid sequence intubation may result in posterior lung atelectasis thereby reducing lung volumes, oxygenation reserve, and ultimately apnea time.
Several studies have shown that elevating the head of the bed by at least 20 degrees or placing a patient in reverse Trendelenberg position (for patients with contra-indications to elevating the head of the bed) during RSI may significantly increase apnea time.
Elevating the head of the bed may be especially helpful for patients with BMIs >35
Weingart, S and Levitan, R. Preoxygenation and prevention of desaturation during emergency airway management. Ann Emerg Med. 2012 Mar; 59(3):165-175.e1; here's the article for FREE: http://www.annemergmed.com/article/S0196-0644(11)01667-2/fulltext
Follow me on Twitter (@criticalcarenow) or Google+ (+haney mallemat)
