Category: Infectious Disease
Keywords: Risk, soft tissue, infection (PubMed Search)
Posted: 1/30/2025 by Robert Flint, MD
(Updated: 2/2/2025)
Click here to contact Robert Flint, MD
Risk factors for necrotizing soft tissue infections include: obesity, diabetes mellitus, peripheral vascular disease, immunosuppression, injection drug use, and deep traumatic wounds.
“Any anatomical site can be involved, but the most common sites are perineal, anorectal, foot, or lower extremities.”
Category: Trauma
Keywords: Cervical sound, age, geriatric, trauma, clearance (PubMed Search)
Posted: 2/1/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
Not based on currently available literature.
This editorial reminds us that the only evidenced based screening criteria we have for C-spine clearance in those over age 65 after trauma is the Canadian C-Spine Rule (2002). This rule recommends imaging for all patients over age 65. No large, well done study indicates physical exam or other means can be used to clear C-Spines in those over age 65.
Rodriguez R, Greenberg S. Is older age an appropriate criterion alone for ordering cervical spine CT after trauma. Acad Emerg Med. 2024; 00: 1-2. doi:10.1111/acem.15001
Category: Infectious Disease
Keywords: Soft tissue infection (PubMed Search)
Posted: 1/30/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
These infections remain difficult to diagnose early and early diagnosis is key to limiting morbidity and mortality.
“The classic clinical signs and symptoms are rarely all present especially in early disease. Crepitus or gas in the soft tissues, while specific, is only present in approximately 10% of patients. More often, the presenting symptoms are nonspecific: fever, pain, induration, and edema. Pain out of proportion to examination is a more specific finding that may assist in differentiation of NSTI from cellulitis.”
Bisgaard, Erika K. MD; Bulger, Eileen M. MD
Journal of Trauma and Acute Care Surgery 97(5):p 678-686, November 2024. | DOI: 10.1097/TA.0000000000004351
Category: Trauma
Keywords: Chest trauma, ketorolac, ketamine (PubMed Search)
Posted: 1/26/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This small study randomized patients with 2 or greater rib fractures or requiring chest tube insertion into a kerorolac (30 mg) or ketamine (0.25 mg/kg) group and evaluated pain levels pre, 30 and 60 minutes post medication administration. They also looked at need for morphine rescue medication. The ketamine group had superior pain control and required less rescue medication.
Hossein Zabihi Mahmoodabadi MD, Zeynab Seyed Javadein MD, Fatemeh Moosaie MD, MPH, Ali Faegh, Maryam Bahreini MD
First published: 31 December 2024
Category: Trauma
Keywords: occipital, condyles, fracture, cervical spine (PubMed Search)
Posted: 1/19/2025 by Robert Flint, MD
Click here to contact Robert Flint, MD
Fractures of the occipital condyles are a relatively rare injury that occur in high energy blunt mechanisms (IE roll over MVC) most commonly. Physical exam will show signs of basilar skull fracture and significant pain at the base of the skull/upper C-spine. CT scan is the gold standard to make the diagnosis. Look for signs of upper extremity weakness on physical exam or cranial nerve injuries. Those type of findings should also prompt emergent MRI evaluation. Treatment generally is long term immobilization in a collar however Type 3 and those with neurologic findings may require surgical intervention.
Anderson and Montesano Classification
Type I 3% of occipital condyle fracturesImpaction-type fracture with comminution of the occipital condyle
Due to compression between the atlantooccipital joint
Stable injury due to minimal fragment displacement into the foramen magnum
Type II 22% of occipital condyle fracturesBasilar skull fracture that extends into one or both occipital condyles
Due to a direct blow to skull and a sheer force to the atlantooccipital joint
Stable injury as the alar ligament and tectorial membrane are usually preserved
Type III 75% of occipital condyle fractures Avulsion fracture of condyle in region of the alar ligament attachment (suspect underlying occipitocervical dissociation)
Due to forced rotation with combined lateral bending
Has the potential to be unstable due to craniocervical disruption

Category: Pharmacology & Therapeutics
Keywords: tpa, frostbite, iloprost, therapy (PubMed Search)
Posted: 1/13/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This meta analysis of studies looking at thrombolytics and prostaglandins in treating significant frost bite offers some insight into the possibilities these therapeutics offer. Unfortunately, the studies available are not high quality and most are case reports.
“Our results suggest that thrombolysis or intravenous iloprost is effective when administered promptly to treat severe frostbite. For grade 3–4 frostbite the Wilderness Medical Society frostbite guidelines recommend the use of intravenous iloprost within 48 h of injury, and thrombolysis within 24 h of injury. The Helsinki protocol recommends the use of tPA for patients with grade 3–4 frostbite presenting within 48 h of injury with angiographic evidence of thrombosis."
“Iloprost is a synthetic prostaglandin I2 that has been used to treat frostbite . Like other prostacyclins, it inhibits platelet aggregation and promotes vasodilation. Iloprost may stimulate the release of endogenous tissue plasminogen activator or counteract its inhibitory effects [35]. Iloprost reduces vasoconstriction induced by thromboxane A2 , and may reduce oxidative stress from free radicals, moderating reperfusion injury [37, 38]. The effect on platelet aggregation may be reversed within two hours), but prostacyclin effects may disrupt the vicious cycle of activated platelets and leukocytes that damages endothelium .”
More research in this area is needed. Transfer to a center with these capabilities seems worth a discussion in the case of severe frostbite.
Regli, I.B., Oberhammer, R., Zafren, K. et al. Frostbite treatment: a systematic review with meta-analyses. Scand J Trauma Resusc Emerg Med 31, 96 (2023). https://doi.org/10.1186/s13049-023-01160-3
Category: Trauma
Keywords: Frail, trauma, mortality, outcome (PubMed Search)
Posted: 1/12/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
The Trauma Frailty Index has been validated to predict inpatient mortality, major complications and discharge to rehab facility. “In addition, frailty was significantly associated with higher adjusted odds of mortality, major complications, readmissions, and fall recurrence at 3 months postdischarge ( p < 0.05).”
It is a simple 15 variable index.

Joseph B, Saljuqi AT, Amos JD, Teichman A, Whitmill ML, Anand T, Hosseinpour H, Burruss SK, Dunn JA, Najafi K, Godat LN, Enniss TM, Shoultz TH, Egodage T, Bongiovanni T, Hazelton JP, Colling KP, Costantini TW, Stein DM, Schroeppel TJ, Nahmias J; AAST Frailty MIT Study Group. Prospective validation and application of the Trauma-Specific Frailty Index: Results of an American Association for the Surgery of Trauma multi-institutional observational trial. J Trauma Acute Care Surg. 2023 Jan 1;94(1):36-44. doi: 10.1097/TA.0000000000003817. Epub 2022 Oct 17. PMID: 36279368.
Category: Critical Care
Keywords: Frailty, morbidity, mortality, geriatric (PubMed Search)
Posted: 1/5/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
The level of fitness/health a patient has entering the marathon of recovery from critical illness or trauma has a major impact on morbidity and mortality. Frailty is a measure of this fitness level. The clinical frailty scale can be used to assess your patients ability to survive critical illness. Age is a number. Frailty is more useful.


Category: Cardiology
Keywords: Hypertension, MACE, end organ (PubMed Search)
Posted: 1/4/2025 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This study followed patients presenting to the ED with elevated (SBP>180, DBP>120) blood pressure without evidence of end organ dysfunction for one year. The patients were followed for major adverse cardiac events. They found:
“A total of 12,044 patients were enrolled. The prevalence of MACE within one year was 1,865 (15.5%). Older age, male gender, history of cardiovascular disease, cerebrovascular disease, diabetes, smoking, presentation with chest pain, altered mental status, dyspnea, treatment with intravenous and oral hydralazine, and oral metoprolol were independent predictors for one-year MACE. Additionally, discharge with an SBP ?160 mm Hg was not associated with 30-day MACE-free survival after propensity matching (hazard ratio 0.99, 95% confidence interval 0.78–1.25, P?=?0.92).”
Treating to reach a magic number did not help. Most likely, long term control of blood pressure is a more important factor than attempts to lower in the ED. While this is a high risk group, there is no evidence that acute lowering of blood pressure impacts long term survival.
Category: Trauma
Keywords: chest injury, exercise, chronic pain, (PubMed Search)
Posted: 12/30/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This study suggests no. The control arm was given standard physical therapy and the intervention arm was instructed in four basic exercises to do on their own daily for a week. Patents were then surveyed to assess for long term pain. There was no difference in pain between the two groups. Meaning, at least in this study reliant on patient journaling and follow up, that these four simple exercises did not impact long term pain in chest wall injured patients. More work needs to be done in this important area.
Cheri Battle, Timothy Driscoll, Deborah Fitzsimmons, Shaun Harris, Fiona Lecky, Claire O'Neill, Alan Watkins, Jane Barnett, Susan Davies, Hayley Anne Hutchings, Kate Jones, Andrew Eglington, Sophie Place, Hannah Toghill, Katie Foster, Bethan Uzzell, Elizabeth Ford, Mark Baker, Sophie Lewis, Sara Davies, Sarah Nicholls, Amy Charnock, Claire Watkins, Sarah-Jane Garside, Jeannie Bishop, Thomas Dawson, Jessica Pendlebury, Reece Doonan,
EarLy Exercise in blunt Chest wall Trauma: A multi-centre, parallel randomised controlled trial (ELECT2 Trial),
Injury,
2024,
112075,
ISSN 0020-1383,
https://doi.org/10.1016/j.injury.2024.112075.C
Category: Misc
Keywords: Neck pain, crowned dens syndrome (PubMed Search)
Posted: 12/22/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
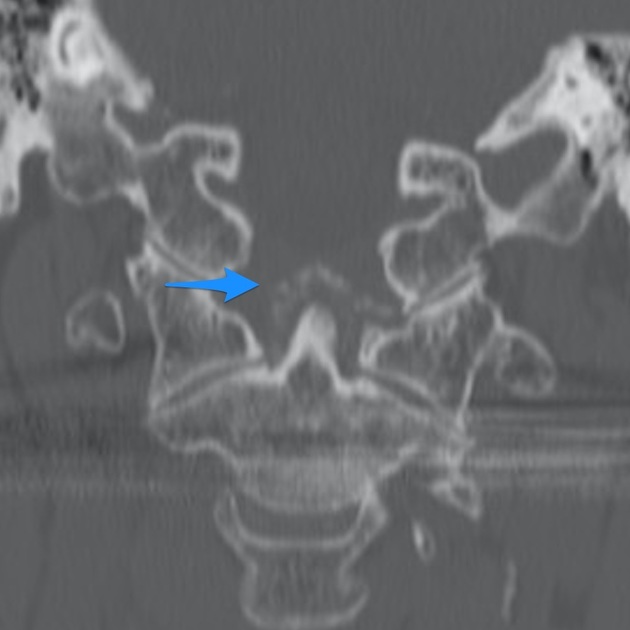
Crowned dens syndrome is an acute inflammatory disease caused by deposition of calcium pyrophosphate dihydrate crystals or hydroxyapatite crystals in the soft tissue and ligaments surrounding the dense. Patient presentation is severe pain in the neck and base of the skull, low grade fever, and elevated inflammatory markers. It is most commonly seen in elderly females. Ct scan is the gold standard for diagnosis. Once meningitis and other significant infectious process has been excluded, treatment is anti inflammatory medications including steroids.
Category: Airway Management
Keywords: Ketamine, etomidate, RSI, induction (PubMed Search)
Posted: 12/19/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Another large database evaluation of the use of etomidate vs. ketamine as an induction agent for intubation found a trend toward higher mortality in the etomidate group. Even when trying to control for steroid use (to control for etomidate’s possible adrenal suppression), etomidate had a higher mortality rate.
A well done study that adds to the chorus advocating for choosing ketamine when looking for a hemodynamically neutral induction agent.
Wunsch H, Bosch NA, Law AC, Vail EA, Hua M, Shen BH, Lindenauer PK, Juurlink DN, Walkey AJ, Gershengorn HB. Evaluation of Etomidate Use and Association with Mortality Compared with Ketamine among Critically Ill Patients. Am J Respir Crit Care Med. 2024 Nov 15;210(10):1243-1251. doi: 10.1164/rccm.202404-0813OC. PMID: 39173173.
Category: Trauma
Keywords: Trauma, oxygen, mortality (PubMed Search)
Posted: 12/14/2024 by Robert Flint, MD
(Updated: 12/15/2024)
Click here to contact Robert Flint, MD
In this randomized trial of restrictive oxygen (arterial oxygen sat of 94% ) vs. liberal oxygen (12-15 L of O2 per minute) for 8 hours after traumatic injury there was no difference in mortality or major respiratory complications at 30 days between the two groups.
Further evidence that managing hypoxia is important but over oxygenation at best offers no benefit and may add harm.
Arleth T, Baekgaard J, Siersma V, et al. Early Restrictive vs Liberal Oxygen for Trauma Patients: The TRAUMOX2 Randomized Clinical Trial. JAMA. Published online December 10, 2024. doi:10.1001/jama.2024.25786
Category: Trauma
Posted: 12/8/2024 by Robert Flint, MD
(Updated: 12/9/2024)
Click here to contact Robert Flint, MD
What is the diagnosis? Treatment? Other imaging indicated?
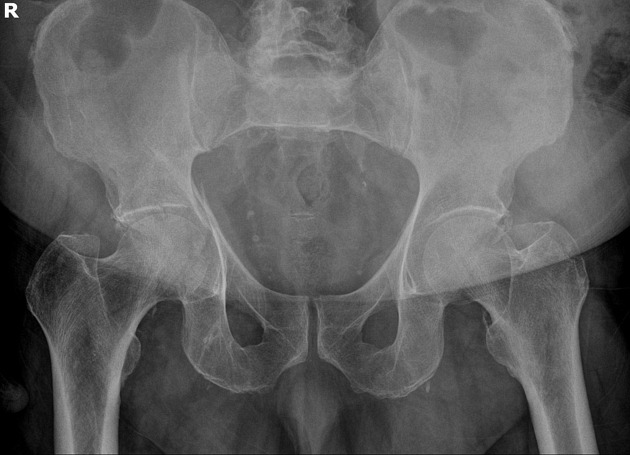
Acetabulum fracture.
Usually seen in high mechanism situations such as MVCs. Can be seen in elderly fall patients.
Treatment is usually surgical (ORIF) unless non-displaced or if it involves less than 20% of posterior column. These can be managed with 6 weeks of minimal weight bearing. CT scan is almost universally used for better visualization and operative management.
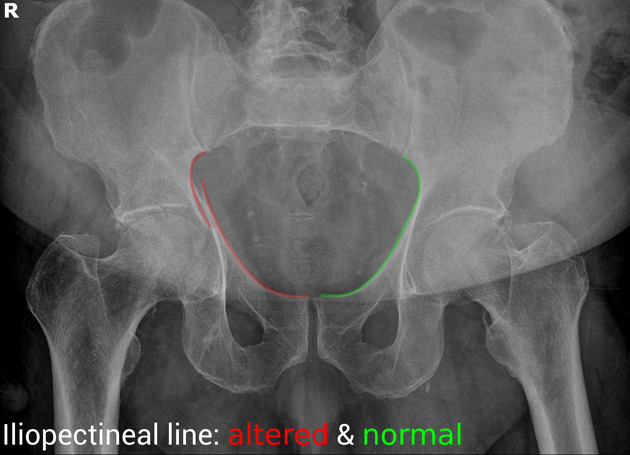
“Some landmarks of the hip are compared on the right and left sides of the pelvis:
https://radiopaedia.org/cases/acetabular-fracture-anterior-and-posterior-columns
https://www.orthobullets.com/trauma/1034/acetabular-fractures
Category: Trauma
Keywords: Liver laceration, embolization, observation. (PubMed Search)
Posted: 12/7/2024 by Robert Flint, MD
(Updated: 12/8/2024)
Click here to contact Robert Flint, MD
This prospective observational study looked at patients with liver lacerations and active contrast extravasation who either had immediate embolization vs. observation. After matching for age, injury score etc. the observation first approach did as well as those who had immediate embolization.
Journal of Trauma and Acute Care Surgery 97(5):p 764-769, November 2024. | DOI: 10.1097/TA.0000000000004372
Category: Cardiology
Keywords: Aaa (PubMed Search)
Posted: 12/7/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
This study tried to expand upon what they describe as the classic triad of signs to diagnose ruptured AAA “(1) abdominal pain, (2) hypotension and (3) a pulsatile abdominal mass”. They tested these against the _modified abdominal aortic aneurysm rupture signs. “_The MARS-signs encompassed (1) the registered pain-associated symptoms or signs, (2) all hypovolemic associated signs, and (3) pulsatile abdominal mass and/or ultrasound finding”. The MARS did slightly better in identifying ruptured AAA retrospectively. For me, this doesn’t add a great deal of help in making this can’t miss diagnosis and further work is necessary.
Bergmark, P., Sadeghi, M., Talvitie, M. _et al._Initial signs in patients with ruptured abdominal aortic aneurysms: time for an expanded triad?.Scand J Trauma Resusc Emerg Med 32, 94 (2024). https://doi.org/10.1186/s13049-024-01268-0
Category: Trauma
Keywords: vetebral fracture, trauma, fall, spinal injury (PubMed Search)
Posted: 12/1/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
Fall from a height of 6 feet with back pain. Plain film shown. What is the diagnosis? Any further imaging indicated? Treatment? Disposition?
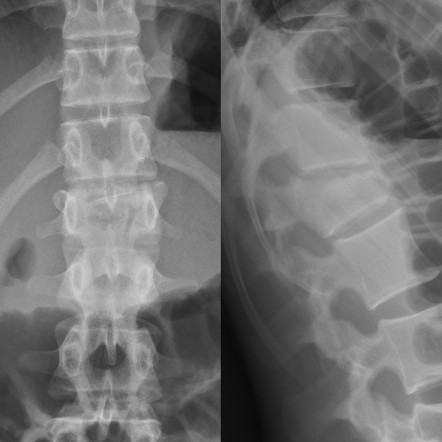
The question that must be answered is, is this a compression fracture or a burst fracture. A compression fracture without any retropulsion into the canal and any other associated injuries is a stable fracture that can be managed with pain control, out patient follow up and possible kyphosplasty for significant loss of vertebral height. A burst fracture is inherently unstable and is a risk for spinal cord injury. CT imaging answers are questions most efficiently.
To help distinguish burst from compression: “Burst fractures are a type of compression fracture related to high-energy axial loading spinal trauma that results in disruption of a vertebral body endplate and the posterior vertebral body cortex. Retropulsion of posterior cortex fragments into the spinal canal is frequently included in the definition. However, some authors, including the popular AO spine classification system, define a burst fracture as any axial compression fracture involving an endplate and the posterior cortex regardless of retropulsion." 2
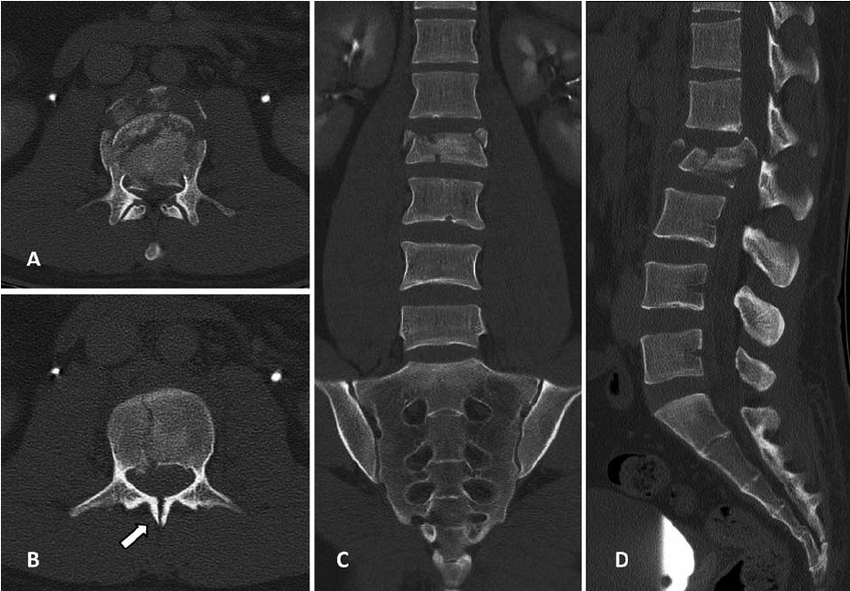
1. https://radiopaedia.org/cases/acute-l1-burst-compression-fracture
Category: Geriatrics
Keywords: Beers criteria, geriatric, prescribing, elderly, drug interaction, pharmacology (PubMed Search)
Posted: 11/30/2024 by Robert Flint, MD
Click here to contact Robert Flint, MD
As a reminder, prescribing medications to older patients should be done with caution because of changed physiology, co-morbid conditions and other currently used medications. The Beers Criteria is a helpful list of medications that may cause trouble for your older patients. https://www.guidelinecentral.com/guideline/340784/#section-2776198 is a list of medications to either avoid or prescribe carefully in this patient population.
Pay particular attention to medications that have anticholinergic properties as they cause change in mental status and increase the risk for falls.
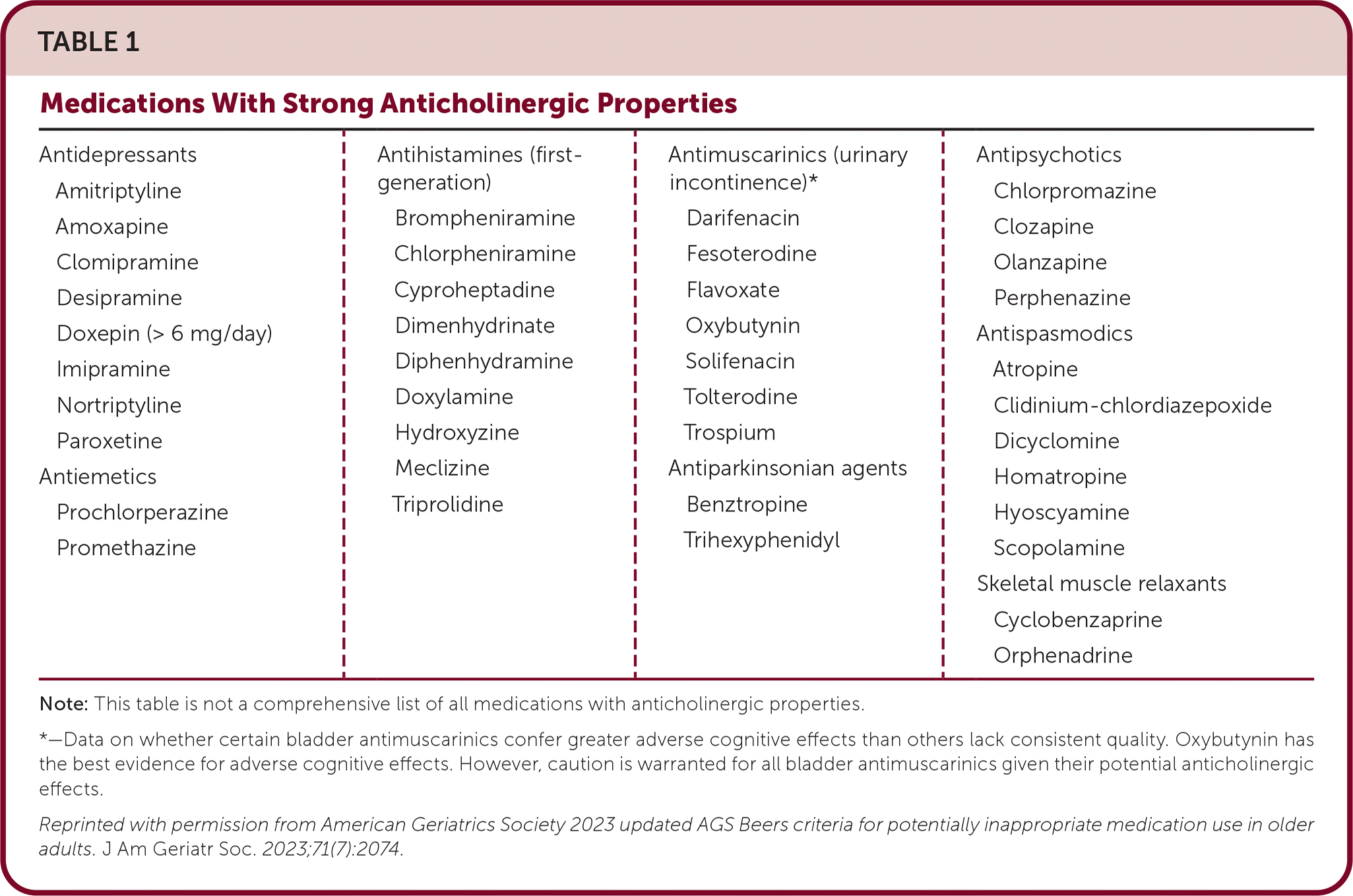
By the 2023 American Geriatrics Society Beers Criteria® Update Expert Panel
Pages: 2052-2081
First Published: 04 May 2023 https://agsjournals.onlinelibrary.wiley.com/doi/epdf/10.1111/jgs.18372
2. https://www.carepatron.com/templates/beers-criteria-template
Category: Administration
Keywords: Thanksgiving (PubMed Search)
Posted: 11/27/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
From all of us at UMEM, Happy Thanksgiving!!
We are incredibly Thankful for each of you and all that you do to care for patients and their families.
We are Thankful for those legends who have blazed the path in EM like Greg Henry who the EM community lost yesterday. Our thoughts are with his family. Thank you Dr. Henry for inspiring so many of us. Our pearls today are two of his famous quotes:
“Medicine is show business for ugly people.”
“You don’t go to Disney and see Mickey taking a smoke break. You have to be on when you are on shift”
Category: Trauma
Keywords: collision, extrication, trauma, motor vehicle, extraction, rapid, spinal immobilization (PubMed Search)
Posted: 11/24/2024 by Robert Flint, MD
(Updated: 5/13/2026)
Click here to contact Robert Flint, MD
It is important for trauma and emergency care providers to understand what our patients experience prior to arrival in our clean, safe, and structured emergency department. It is also vitally important that we are involved in training and education in the pre-hospital environment. A group in the United Kingdom is challenging the age old “wisdom” that post-motor vehicle crash extrication should be slow, methodical, and work to have absolutely no movement in the spinal canal. Spinal immobilization and slow extrication instead of rapid resuscitation appears to be bad for patients. Based on several of their ground breaking papers they have published a 14 point recommendation of patient extrication post motor vehicle collision. Here are two important tenets they propose. For an in-depth discussion check out November 14, 2024 / CPD, Podcasts, Roadside to Resus.


