Category: Neurology
Keywords: myelopathy, myelitis, physical exam (PubMed Search)
Posted: 5/23/2018 by Danya Khoujah, MBBS
(Updated: 5/10/2026)
Click here to contact Danya Khoujah, MBBS
Lhermitte’s phenomenon is as a sign of cervical spinal cord demyelination. It is considered positive if flexion of the neck causes a tingling sensation moving down the limbs or trunk, and may be reported as a symptom or elicited as a sign. This is due to stretching of the dorsal column sensory fibers, the commonest cause of which is multiple sclerosis. Other causes include other myelopathies, such as B12 deficiency, radiation and toxic (due to chemotherapy) or idiopathic myelitis. Its sensitivity is low at 16%, but its specificity for myelopathy is high at 97%.
Kempster PA, Rollinson RD. The Lhermitte phenomenon: variant forms and their significance. J Clin Neurosci 2008;15(4):379–81.
Khare S, Seth D. Lhermitte's Sign: The current status. Ann Indian Acad Neurol. 2015 Apr-Jun; 18(2): 154-156.
Category: Neurology
Keywords: Intracerebral hemorrhage, ICH, hematoma expansion, prediction score, BAT score (PubMed Search)
Posted: 5/9/2018 by WanTsu Wendy Chang, MD
(Updated: 5/10/2026)
Click here to contact WanTsu Wendy Chang, MD
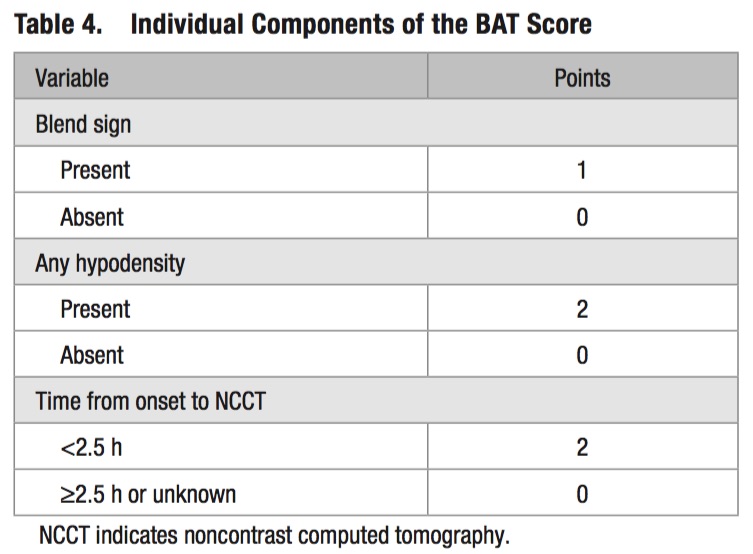
Morotti A, Dowlatshahi D, Boulouis G, et al. Predicting intracerebral hemorrhage expansion with noncontrast computed tomography: The BAT score. Stroke 2018;49(5):1163-9.
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: stroke, altered mental status, gender, sex, confusion (PubMed Search)
Posted: 3/28/2018 by Danya Khoujah, MBBS
(Updated: 5/10/2026)
Click here to contact Danya Khoujah, MBBS
Patients may present atypically with ischemic strokes, reporting symptoms such as face or hemibody pain, lightheadedness, mental status change, headache and non-neurological symptoms.
Up to 25% of patients will have these symptoms.
Women are more likely than men to present with these atypical (or “nontraditional”) symptoms, especially altered mental status.
Labiche LA, Chan W, Saldin KR, Morgenstern LB. Sex and acute stroke presentation. Ann Emerg Med. 2002;40(5):453-460.
Lisabeth LD, Brown DL, Hughes R, et al. Acute stroke symptoms: comparing women and men. Stroke. 2009;40(6):2031-2036.
Category: Neurology
Keywords: stroke, prehospital, large vessel occlusion, NIHSS, RACE, LAMS, VAN (PubMed Search)
Posted: 3/14/2018 by WanTsu Wendy Chang, MD
(Updated: 5/10/2026)
Click here to contact WanTsu Wendy Chang, MD
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: headache, steroids, bleed (PubMed Search)
Posted: 2/28/2018 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
Benign headaches are common in bodybuilders. However, several less benign headaches are worth noting:
All except the first two are exclusively reported in patients on anabolic steroids, growth hormone, and/or “energy” supplements. Make sure to ask your patient about these risk factors.
Busche K. Neurologic Disorders Associated with Weight lifting and Bodybuilding. Neurology Clinics. 26 (2008) 309–324
Category: Neurology
Keywords: occipital nerve block, migraine, headache (PubMed Search)
Posted: 2/14/2018 by WanTsu Wendy Chang, MD
(Updated: 2/15/2018)
Click here to contact WanTsu Wendy Chang, MD
Zhang H, Yang X, Lin Y, Chen L, Ye H. The efficacy of greater occipital nerve block for the treatment of migraine: a systematic review and meta-analysis. Clin Neurol Neurosurg. 2018;165:129-133.
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: edema, hemorrhage, tumor, CT, MRI, contrast (PubMed Search)
Posted: 1/24/2018 by Danya Khoujah, MBBS
(Updated: 5/10/2026)
Click here to contact Danya Khoujah, MBBS
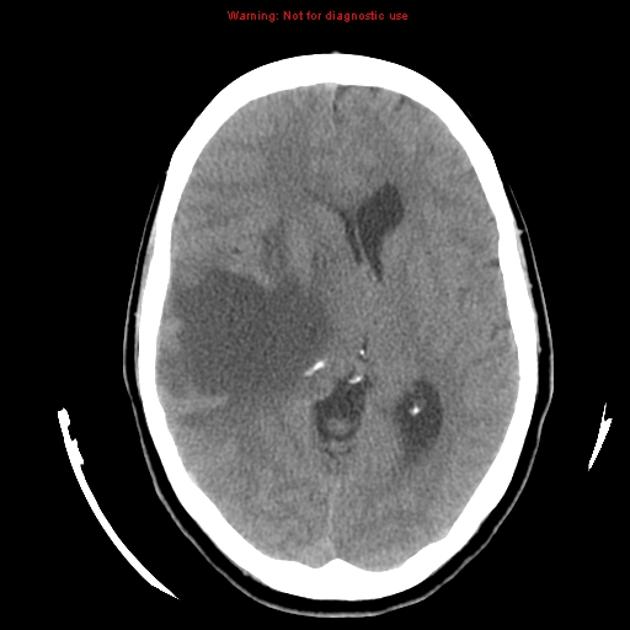
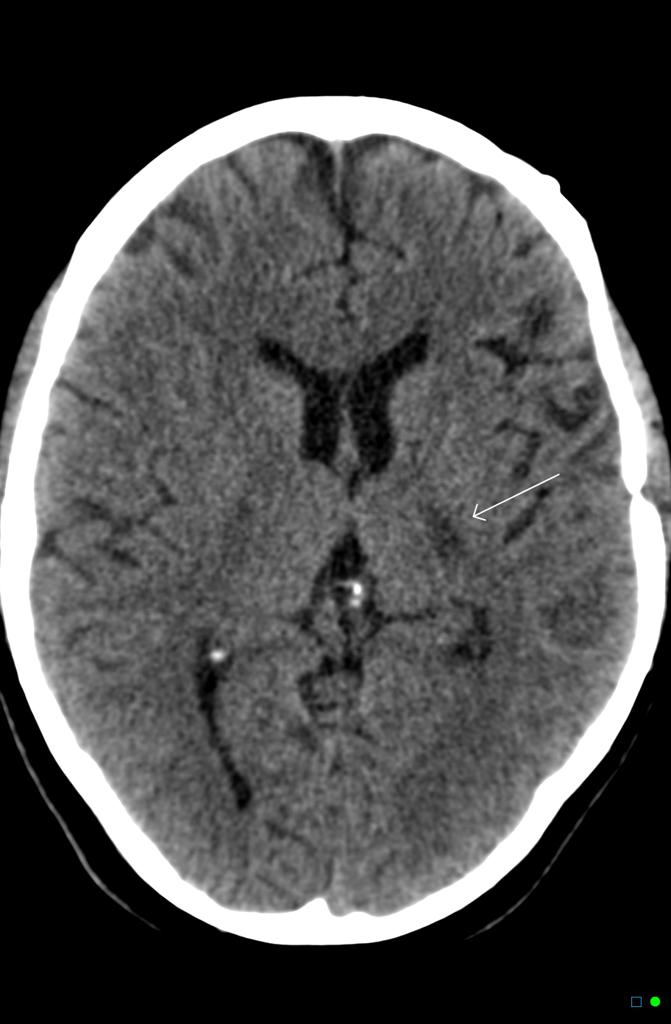
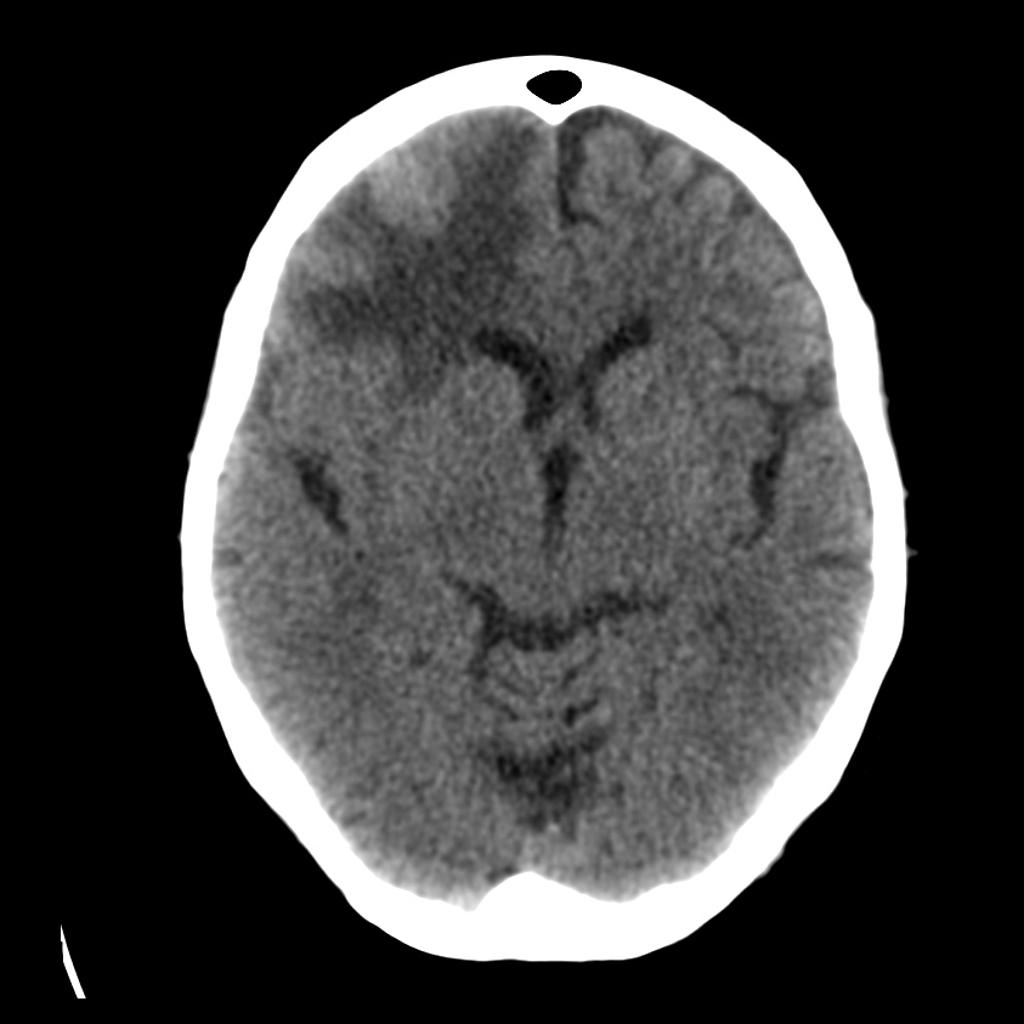
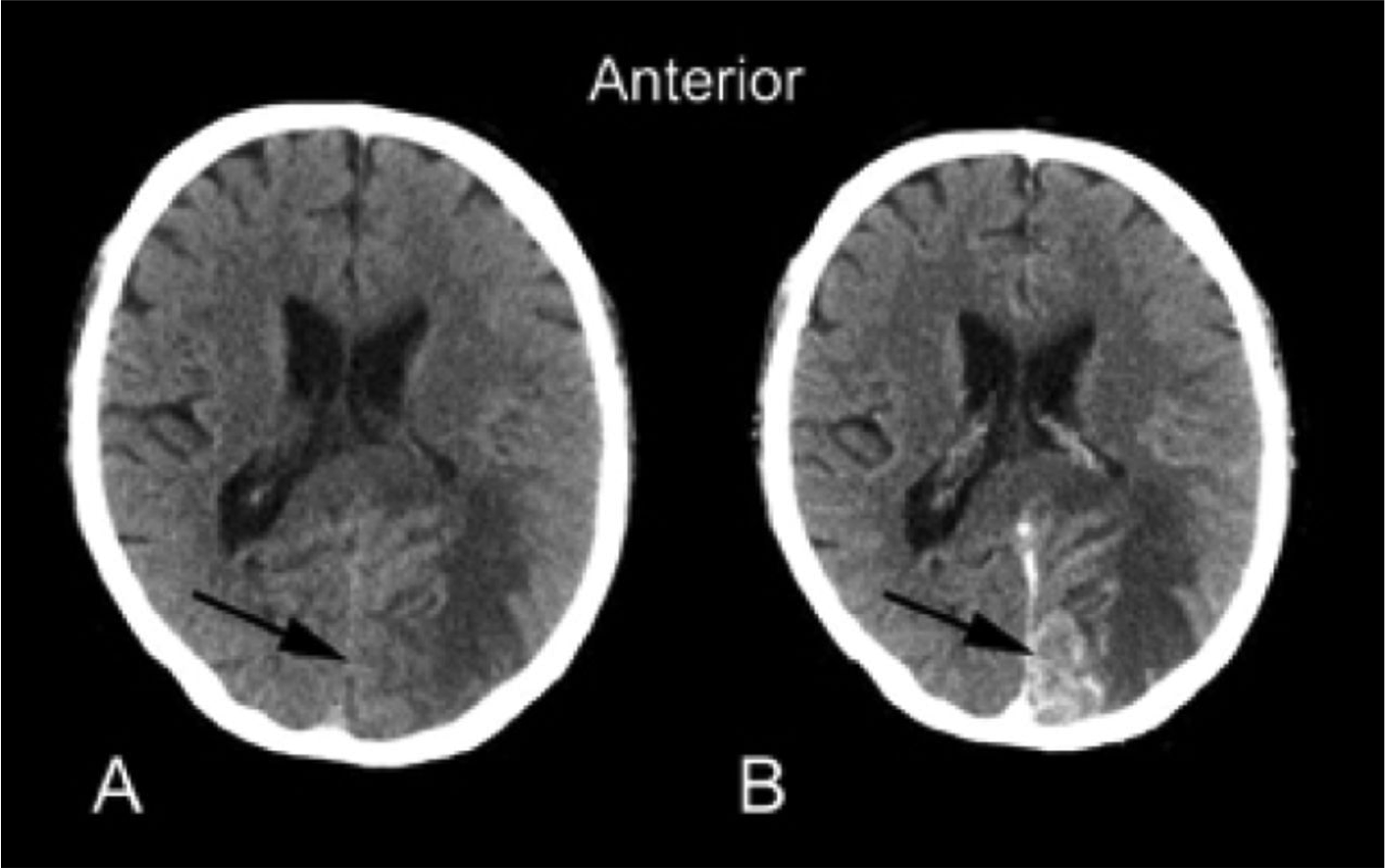
Klein JP, Dietrich J. Neuroradiologic Pearls for Neuro-oncology. Continuum 2017;23(6):1619-1634.
Category: Neurology
Keywords: RCVS, thunderclap headache, migraine, SAH (PubMed Search)
Posted: 1/10/2018 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Bottom Line: Consider RCVS in the differential of thunderclap headache and in patients who present with worse than usual migraine headache.
Arrigan MT, Heran MKS, Shewchuk JR. Reversible cerebral vasoconstriction syndrome: an important and common cause of thunderclap and recurrent headaches. Clin Radiol. 2017 Dec 21 [Epub ahead of print]
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: headache, seizure, stroke, neurological deficit, thrombogenic (PubMed Search)
Posted: 12/27/2017 by Danya Khoujah, MBBS
(Updated: 5/10/2026)
Click here to contact Danya Khoujah, MBBS
Long B, Koyfman A, Runyon MS. Cerebral Venous Thrombosis: A Challenging Neurologic Diagnosis. Emerg Med Clin N Am 35 (2017) 869–878
Category: Neurology
Keywords: DAWN, thrombectomy, mismatch, wake-up, stroke, penumbra (PubMed Search)
Posted: 12/13/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Bottom Line: The use of neuroimaging to identify an ischemic penumbra that may benefit from thrombectomy may be considered even for patients with time of last known well beyond 6 hours.
Nogueira RG, Jadhav AP, Haussen DC, et al. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med. 2017 Nov 11. [Epub ahead of print]
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: GBS, weakness, intubation, CSF, LP (PubMed Search)
Posted: 11/22/2017 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
Allen JA. Chronic Demyelinating Polyneuropathies. Continuum 2017;23(5):1310–1331
Category: Neurology
Keywords: aphasia, stroke, middle cerebral artery, MCA, mimic, NIHSS (PubMed Search)
Posted: 11/8/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Take Home Point: This small but interesting study looked at the incidence of isolated aphasia presenting for concern of stroke. They found that none of their patients had evidence of an infarct, suggesting that strokes affecting language without motor or sensory deficits are uncommon.
Casella G, Llinas RH, Marsh EB. Isolated aphasia in the emergency department: The likelihood of ischemia is low. Clin Neurol Neurosurg 2017:163:24-26.
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: weakness, infection, paralysis, intubation, influenza, vaccine (PubMed Search)
Posted: 10/25/2017 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
It's respiratory infection and flu vaccine season! Time to brush up on Guillain-Barré Syndrome..
- It is the most common cause of acute or subacute flaccid weakness worldwide
- 70% of cases are preceded by an infection in the past 10-14 days, but most are minimized or forgotten by the patient. 40% of these infections are by Campylobacter jejuni.
- 30% develop respiratory failure requiring intubation and ventilation
- Half of the patients will develop their maximum weakness by 2 weeks, most will develop it by 4 weeks.
Donofrio PD. Guillain-Barré Syndrome. Continuum 2017;23(5):1295–1309.
Category: Neurology
Keywords: traumatic brain injury, TBI, fall, subdural hematoma, SDH, elderly (PubMed Search)
Posted: 10/11/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Traumatic brain injury (TBI) is associated with close to half of major trauma admissions in adults over age 65 in the U.K.
Falls accounted for 85% of all TBIs, while 45% of patients had subdural hematomas (SDH).
More than 3/4 of patients were treated conservatively, though outcomes were not significantly better than those who underwent neurosurgical intervention.
Higher age is associated with higher mortality and greater disability.
Bottom Line: Trauma in older adults is increasing and fall prevention is important in reducing significant injuries.
Hawley C, Sakr M, Scapinello S, et al. Traumatic brain injuries in older adults - 6 years of data for one UK trauma centre: retrospective analysis of prospectively collected data. Emerg Med J 2017;0:1-8.
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: stroke, tPA, thrombolytics, ICH, hemorrhage, adverse events (PubMed Search)
Posted: 9/28/2017 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
Category: Neurology
Keywords: seizure, status epilepticus, benzodiazepine, RAMPART, pediatric (PubMed Search)
Posted: 9/13/2017 by WanTsu Wendy Chang, MD
(Updated: 9/14/2017)
Click here to contact WanTsu Wendy Chang, MD
IV vs. Non-IV Benzodiazepines for Cessation of Seizures
Follow me on Twitter @ EM_NCC
Category: Neurology
Keywords: meningitis, CSF, glucose, glucometer (PubMed Search)
Posted: 8/24/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
Category: Neurology
Keywords: pituitary apoplexy, subarachnoid hemorrhage, meningitis, headache, CT, MRI (PubMed Search)
Posted: 8/9/2017 by Danya Khoujah, MBBS
(Updated: 5/10/2026)
Click here to contact Danya Khoujah, MBBS
Bottomline: Keep pituitary apoplexy in your differential when considering SAH or meningitis, especially in the presence of risk factors, and have a low threshold to order an MRI.
Category: Neurology
Keywords: Terson syndrome, vitreous hemorrhage, intraocular hemorrhage, subarachnoid hemorrhage (PubMed Search)
Posted: 7/12/2017 by WanTsu Wendy Chang, MD
Click here to contact WanTsu Wendy Chang, MD
50 YOF with acute onset of worst headache of life associated with nausea and vomiting. Patient is somnolent, will rouse to noxious stimuli and complains of a headache as well as decreased vision.
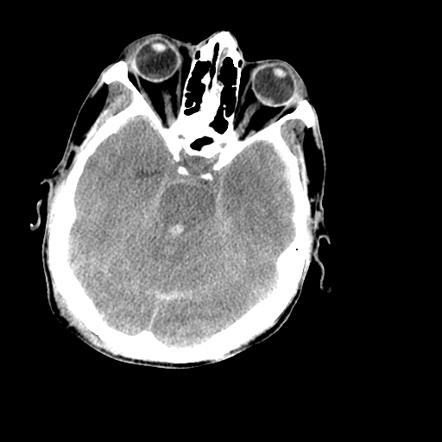
Image courtesy of Dr. Nasir Siddiqui, Radiopaedia.org. From the case rID: 36469
Follow me on Twitter @EM_NCC
Category: Neurology
Keywords: autoimmune, cancer, encephalopathy (PubMed Search)
Posted: 6/28/2017 by Danya Khoujah, MBBS
Click here to contact Danya Khoujah, MBBS
