Category: Toxicology
Keywords: latex, allergy, kiwi, cross-reactivity (PubMed Search)
Posted: 4/13/2011 by Bryan Hayes, PharmD
(Updated: 4/14/2011)
Click here to contact Bryan Hayes, PharmD
Kiwi fruit and latex share several antigens in common. Thus, individuals who are allergic to either kiwi or latex may also suffer hypersensitivity reactions to the other material.
Murali MR, et al. Case 9-2011: A 37-year old man with flushing and hypotension. N Engl J Med 2011;364(12):1155-65.
Category: Toxicology
Keywords: radiation, iodide, KI, thyroid, iodine-131 (PubMed Search)
Posted: 4/7/2011 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
· In the event a nuclear power plant accident, people may be exposed to a mixture of radioactive products. The main radionuclides representing health risk are radioactive caesium and radioactive iodine.
· Iodine-131 is concentrated in the thyroid gland and may eventually lead to development of thyroid nodules and thyroid cancer.
· Radioiodine uptake by the thyroid can be blocked by taking potassium iodide (KI) pills or solution, preventing these effects.
· KI should not be taken in the absence of a clear risk of exposure to a potentially dangerous level of radioactive iodine because KI can cause allergic reactions, skin rashes, salivary gland inflammation, hyperthyroidism or hypothyroidism.
· Since radioactive iodine decays rapidly, current estimates indicate there will not be a hazardous level of reaching the United States from this accident.
· There are three FDA approved KI products: Iosat, Thyrosafe and ThyroShield.
http://www.who.int/hac/crises/jpn/faqs/en/index2.html
briefs.com/briefs/ATAORG/ATAORG031611.php
Pharmacist's Letter April 2011 Vol 27(4) 19-20.
Category: Toxicology
Keywords: phenytoin, vinca alkaloids, (PubMed Search)
Posted: 3/31/2011 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
Extravasation from radiocontrast, phenytoin and promethazine have resulted in significant tissue necrosis sometimes requiring surgical debridement and reconstructive plastic surgery.
Pearl: Keep the infiltrated peripheral IV in and inject hyaluronidase 3-5mL (150U/mL) into the same subcutaneous pocket of medication. Hyaluronidase will increase the systemic absorption of the drug, decreasing its time in the SQ tissue. Extremely safe drug (we have the enzyme in our body) and has been used in neonates as well as adults. Also used for SQ hydration in palliative care and pediatrics.
Controversy: Hot vs Cold - Heat will cause vasodilation and hopefully increase systemic absorption but will likely also increase SQ spread possibly increasing the surface area of injury. Cold will cause vasoconstriction and decrease size of injury however will concentrate drug and possibly worsen the local injury.
1: Sokol DK, Dahlmann A, Dunn DW. Hyaluronidase treatment for intravenous phenytoin extravasation. J Child Neurol. 1998 May;13(5):246-7. 2: Cochran ST, Bomyea K, Kahn M. Treatment of iodinated contrast material extravasation with hyaluronidase. Acad Radiol. 2002 Aug;9 Suppl 2:S544-6. 3: Few BJ. Hyaluronidase for treating intravenous extravasations. MCN Am J Matern Child Nurs. 1987 Jan-Feb;12(1):23. 4: Kuensting LL. Treatment of intravenous infiltration in a neonate. J Pediatr Health Care. 2010 May-Jun;24(3):184-8. Epub 2010 Mar 20. 5: Raszka WV Jr, Kueser TK, Smith FR, Bass JW. The use of hyaluronidase in the treatment of intravenous extravasation injuries. J Perinatol. 1990 Jun;10(2):146-9.
Category: Toxicology
Keywords: antipsychotics, thromboembolism (PubMed Search)
Posted: 3/24/2011 by Fermin Barrueto
Click here to contact Fermin Barrueto
Could this be another risk factor for DVT/PE. Maybe not yet but it is worth mention. A recent observatioal study in BMJ showed that there was an associated increase with DVT or PE. From a database of 25,532 patients over a 3 year period of time and finding match controls, the results were:
Limitations were this is was an observational study with missing data. BMI was missing in these records and it is always difficult to tease out the multiple medications these patients are on. Also don't have a great biological mechanism (yet). Still makes you go hmm....
Antipsychotic drugs and risk of venous thromboembolism, Parker, BMJ, 2010.
Category: Toxicology
Keywords: rocuronium, succinylcholine (PubMed Search)
Posted: 3/17/2011 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
Most have converted from succinylcholine to rocuronium for their choice of paralytic in RSI. Succinylcholine-induced hyperkalemia secondary to muscle fasciculations is considered usually clinically insignificant though there may be a hyperkalemic renal patient that this may tip them over. The fasciculations also may worsen traumatic long bone fractures. Here is the argument in a head to head comparison:
| Succinylcholine | Rocuronium | Winner | |
| Onset | 1-1.5min | 1.5-3min | Tie |
| Duration Recovery Index | 3-7min 2min
| 30-40min 10min | Mild S |
| Fasciculations | Yes | No | Roc |
| Histamine | Yes - Released | None | Roc |
| Pulse | Rare Brady | Rare Tachy at high dose | Tie |
Duration = injection of drug to 25% recovery of single twitch height (clinically relevant recovery in ED - essentially breathing may return)
Recovery Index = time from 25% to 75% recovery of single twitch height
The main reason succinylcholine was utilized was because of its fast onset and short duration. Rocuronium is comparable enough to succinylcholine in these characteristics tilting the overall benefits to rocuronium. If the FDA ever approves it, suggamadex is a possible reversal agent for rocuronium - currently used in Europe. Imagine having that in your RSI kit.
Category: Toxicology
Keywords: benzyl alcohol, clonidine, ethanol, chloramphenicol (PubMed Search)
Posted: 3/9/2011 by Bryan Hayes, PharmD
(Updated: 3/10/2011)
Click here to contact Bryan Hayes, PharmD
Several medications/chemicals can cause unique toxicologic reactions in pediatric patients.
Category: Toxicology
Keywords: Brown Recluse,envenomation,spider,loxoscelism (PubMed Search)
Posted: 3/3/2011 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
Recently a case report was published in which a child was incorrectly diagnosed with MRSA. He actually had systemic loxoscelism from a Brown Recluse spider bite.
A patient who has been bitten by brown recluse spider bite may present with pruritis, pain and swelling. The classic lesion has a bluish-purple central region, surrounded by concentric rings of pale ischemia and erythema. (“red, white and blue”) Bites may progress over days to a bleb with necrosis and eschar formation, followed by ulceration.
Systemic loxoscelism presents with a scarlatiniform rash that spreads dependently. It may have the classic purple lesion surrounded by concentric rings of pale ischemia and erythema. The patient may be uncomfortable but is usually stable. Treatment is supportive care.
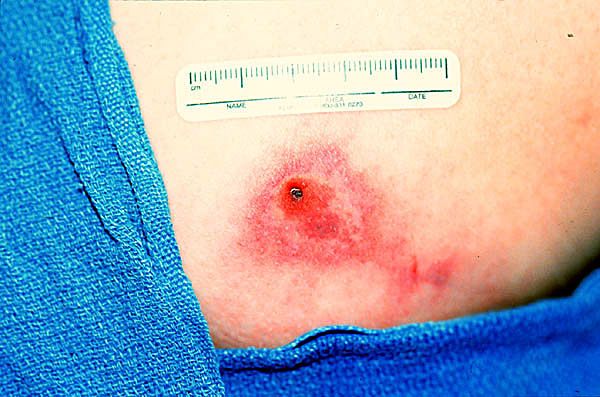
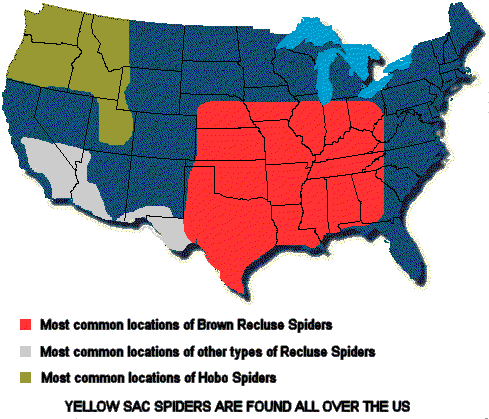
Rogers, KM, Klotz CR, Jack M, Seger D. Systemic Loxoscelism in the Age of Community-Acquired Methicillin-Resistant Staphylococcus aureus. Ann of EM Feb 2011 57(2); 138-40.
Category: Toxicology
Keywords: mephedrone, bath salts (PubMed Search)
Posted: 2/24/2011 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
Continuing with the synthetic/designer drug theme. Last time we were discussing synthetic marijuana. Another old drug making a resurgence under the designer drug category is mephedrone.This amphetamine-like drug has been purportedly the active substance in "bath salts". It has also been sold as "plant food" - still trying to figure that one out.
Sold in head shops under the name Bliss or Cloud 9 - they have been reported to be available in Baltimore, MD recently. They can also be bought over the internet. Crushed, snorted or ingested, the effect is similiar to cocaine with a largely sympathomimetic toxidrome. Mephedrone has been labeled an entactogen with users behaving similiar to an MDMA ingestion. A Baltimore news station incorrectly called it "synthetic cocaine" - though the effect may be similiar, completely different molecular structure.
Treatment is cooling, check lytes (especially sodium), check for rhabdomyolysis and sedation with benzodiazepines. Below is one link from a Denver News Station. Attached is a picture of a bath salt product.
The latest and greatest on the street - synthetic marijuana and bath salts!
http://www.thedenverchannel.com/news/26567376/detail.html
Category: Toxicology
Keywords: THC, marijuana (PubMed Search)
Posted: 2/18/2011 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
Sold under the name of K2, Spice. Patients exposed to this will present with dry mouth, paranoia, tachycardia, hallucinations but will resolved rather quickly over several hours. Observation in the ED and supportive care is usually all that is needed. A little history about synthetic marijuana:
Category: Toxicology
Keywords: dose-response, paracelsus (PubMed Search)
Posted: 1/26/2011 by Bryan Hayes, PharmD
(Updated: 2/10/2011)
Click here to contact Bryan Hayes, PharmD
Many consider Paracelsus (1493–1541) as the father of modern toxicology.
The introduction of the dose–response concept might have been his most important contribution to toxicology, meaning that everything is toxic at the right dose (even oxygen and water).
Category: Toxicology
Keywords: Methemoglobinemia,methylene blue (PubMed Search)
Posted: 2/3/2011 by Ellen Lemkin, MD, PharmD
(Updated: 5/10/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Category: Toxicology
Keywords: Dabigatran, anti-coagulation, toxicology, coumadin (PubMed Search)
Posted: 1/27/2011 by Fermin Barrueto
Click here to contact Fermin Barrueto
Dabigatran (Pradaxa), an antithrombin medication, was discussed in an earlier pearl and thought I would play devil's advocate and explain the possible concerns:
Toxicology Mantra: You never want to be the first person or the last person to use a drug
Category: Toxicology
Keywords: acetaminophen, rumack-matthew nomogram (PubMed Search)
Posted: 1/13/2011 by Bryan Hayes, PharmD
Click here to contact Bryan Hayes, PharmD
The Rumack-Matthew nomogram is a well studied and validated tool to help assess the potential for liver toxicity following acute acetaminophen poisoning. Here is a brief review of when it is best utilized.
Outside-the-box situations:
Category: Toxicology
Keywords: Vitamin K1,anaphylaxis,coumadin,warfarin (PubMed Search)
Posted: 1/6/2011 by Ellen Lemkin, MD, PharmD
(Updated: 5/10/2026)
Click here to contact Ellen Lemkin, MD, PharmD
Smythe MA, Dager WE, Patel NM. Managiing Complications of Anticoagulation Therapy. Journal of Pharmacy Practice 200417(5)327-46.
Dentali F, Crowther MA. Management of Excessive Anticoagulant Effect Due to Vitamin K Antagonists. Hematology 2008;266-9.
DeZee K et all. Treatment of Excessive ANticoagulation with Phytodione. Arch Intern Med Feb 27, 2006;166:391-7.
Category: Toxicology
Keywords: naloxone, opioids (PubMed Search)
Posted: 12/30/2010 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
Naloxone is the epitomy of an antidote with complete reversal of opioid toxicity within 60 seconds of administration. Remember your clinical endpoint should be respiratory effort. If you utilize "the vial" of either 0.4mg or 2mg and there is a higher probability of withdrawal and for acute lung injury. Here are some tips for administration:
1) IV Access: Try 0.1 mg or even 0.05 mg - anesthesiology typically doses naloxone in micrograms. Reversal is slower so you have to be patient. It is also not as dramatic so closely monitor respirations to see if you have improvement, that may be all that you get. These are probably patients that you don't want that awake anyways.
2) No IV Access: advantage of naloxone is it is bioavailable IV, intranasal and even by nebulizer. Here you want the dose to be 0.4mg to start for intranasal. Nebulizer is difficult to measure and probably safe to start with 2mg in the nebulizer container.
There is a difference when you know it is an opioid overdose and are reversing apnea versus a diagnostic administration to determine if it is opioid toxicity. In the latter instance you can rationalize the large dose - just be ready and be sure you are not in line of the possible projectile vomiting.
Category: Toxicology
Keywords: HF (PubMed Search)
Posted: 12/23/2010 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
When you think of an acid or base causing a burn, you usually think of the local damage but there is one particular acid that causes systemic illness. Hydrofluoric Acid, found in your local Home Depot in brick/stone cleaning products, can cause severe illness despite a small total body surface area burn and exposure. A recent case report came out that illustrates how deadly HF can be. The reason is that this acid enters the body and chelates cations like calcium and potassium. The abstract is below but essentially hypocalcemia, hypokalemia leading to asystole 16hrs after exposure all from a 3% TBSA Burn - very impressive.
Wu ML, Deng JF, Fan JS.Survival after hypocalcemia, hypomagnesemia, hypokalemia and cardiac arrest following mild hydrofluoric acid burn. Clin Toxicology 2010
Category: Toxicology
Keywords: fomepizole, disulfiram (PubMed Search)
Posted: 12/17/2010 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
The answer was fomepizole would be the treatment for life-threatening disulfiram reaction. Blocks Alcohol Dehydrogenase and ironically prevent metabolism of ethanol and prolong intoxication.
I forgot how many see the pearls and the response was overwhelming. That was great and cost a me a little more. There were two winners:
Katie Baugher, PGY-1
Ari Keslter
Please email me how to best send you the gift certificate.
Category: Toxicology
Keywords: disulfiram reaction (PubMed Search)
Posted: 12/16/2010 by Fermin Barrueto
(Updated: 5/10/2026)
Click here to contact Fermin Barrueto
There are medications, if taken with ethanol, will cause a disulfiram reaction. This reaction results from inhibition of aldehyde dehydrogenase, the enzyme in ethanol metabolism that breaks acetaldehyde to acetic acid. The increase in acetaldehyde results in nausea, vomiting, diarrhea, flushing, palpitations and orthostatic hypotension. So if you prescribe a patient with any of these medications you must make certain to tell them NOT to drink any ethanol - that includes cough/cold preparations that have ethanol:
Antibiotics: Metronidazole(Flagyl), Trimethoprim-sulfamethoxazole (Bactrim)
Sulfonylureas: Chlorpropamide and tolbutamide
These have possible reactions: griseofulvin, quinacrine, procarbazine, phentolamine, nitrofurantoin
Bonus Question: $10 Starbuck's Gift Card for first person that emails me with the answer to this question
What treatment could you give to someone suffering from a life threatening disulfiram reaction that biochemically should cure him?
Category: Toxicology
Keywords: anion gap, metabolic acidosis (PubMed Search)
Posted: 12/8/2010 by Bryan Hayes, PharmD
(Updated: 12/9/2010)
Click here to contact Bryan Hayes, PharmD
Most cases of normal anion gap metabolic acidosis result from either urinary (RTA) or gastrointestinal HCO3- losses (diarrhea). A number of xenobiotics can also cause this disorder:
Category: Toxicology
Keywords: holly, berry, poinsettia, mistletoe, berries (PubMed Search)
Posted: 12/2/2010 by Ellen Lemkin, MD, PharmD
Click here to contact Ellen Lemkin, MD, PharmD
Toxic Holiday Plants
Of the three plants listed, which is NOT poisonous?
1. Holly plant
2. Poinsettia
3. Mistletoe
Poinsettia plants were once thought to be very poisonous. Contrary to popular belief, poinsettias are safe to have in the home during the holidays.
Although there are reported cases of death with ingestion of Holly plants in older literature, recent experience shows gastrointestinal effects in small doses, and serious toxicity such as CNS depression in large ingestions.
Mistletoe ingestion of few of the berries would, at most, produce mild gastroenteritis; however, ingesting concentrated extracts of the plant, including the berries, may produce serious effects such as seizures, mental confusion, drowsiness, and hallucinations.
Happy holidays!
Poisondex.
