Category: Pediatrics
Keywords: seat belt, car seats (PubMed Search)
Posted: 5/15/2020 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
NHTSA recommends that car seats be replaced following a moderate or severe crash. Car seats do not automatically need to be replaced following a minor crash.
A minor crash is one in which ALL of the following apply:
-The vehicle was able to be driven away from the crash site.
-The vehicle door nearest the car seat was not damaged.
-None of the passengers in the vehicle sustained any injuries in the crash.
-If the vehicle has air bags, the air bags did not deploy during the crash
-There is no visible damage to the car seat.
NEVER use a car seat that has been involved in a moderate to severe crash. Always follow manufacturer's instructions.
Car Seat Use After a Crash. https://www.nhtsa.gov/car-
Category: Pediatrics
Keywords: MVC, anticipatory guidance, seatbelts. (PubMed Search)
Posted: 4/17/2020 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
The leading cause of death in the US for those aged 16 to 24 years is motor vehicle collisions (MVCs). Teen drivers are more likely than any other age group to be involved in an MVC that result in injury or fatality. Texting while driving, nighttime driving, inexperienced driving, and driving under the influence of alcohol or drugs may play a role in these collisions.
Can anticipatory guidance related to safe driving be done in the ED? YES!
This study implemented a toolkit that contained a copy of the driving law, a sample parent-teen driving contract and statistics on teen driving injuries. Post toolkit questionnaires showed that both teens and their guardians learned new information.
Bottom line: Engage in anticipatory guidance in the ED with teens and their parents about seatbelt use, the dangers of driving under the influence and local driving laws.
Spears et al. Teen driving education in the pediatric emergency department: effectiveness of a tool kit. Southern Medical Journal 2019; 112(11): 562-565.
Category: Pediatrics
Keywords: pandemic, coronavirus, pediatric (PubMed Search)
Posted: 3/20/2020 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Category: Pediatrics
Keywords: cardiac arrest, prehospital, epinephrine (PubMed Search)
Posted: 2/21/2020 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Matsuyama et al. Pre-Hospital Administration of Epinephrine in Pediatric Patients with Out-of-Hospital Cardiac Arrests. JACC: 75 (2); 2020.
Category: Pediatrics
Keywords: avulsion fracture, orthopedics, pelvic injury, trauma (PubMed Search)
Posted: 2/14/2020 by Mimi Lu, MD
(Updated: 2/15/2020)
Click here to contact Mimi Lu, MD
A 15 y.o. female presents to your emergency department with sudden onset hip pain after winding up to kick a soccer ball during her game today. You see a well-developed female in obvious discomfort, with tenderness to palpation over her lateral hip and pain with passive ROM at the hip. You obtain this x-ray. What is your diagnosis?
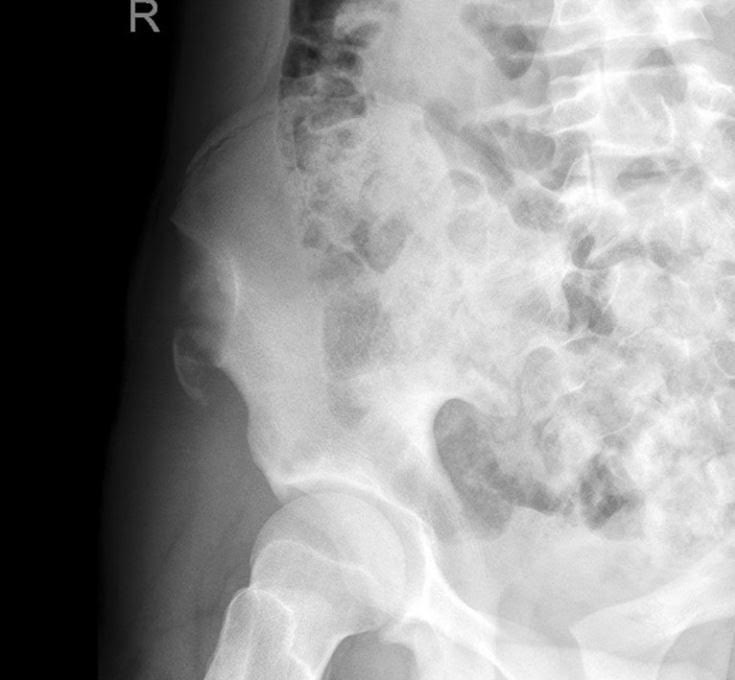
Answer: Avulsion fracture of the anterior superior iliac spine.
Injury:
An avulsion fracture of the anterior superior iliac spine is an uncommon injury seen almost exclusively in adolescent athletes.
They mostly result from a sudden, forceful, and/or unbalanced contraction of the attached musculotendinous unit (sartorius muscle or tensor fascia lata) during the starting phase of running, jumping, kicking, etc.
The most implicated sports include soccer, running, and ice hockey.
History/Exam:
The patient may report sudden shooting pain referred to the involved tuberosity.
Physical exam may include localized edema and tenderness to palpation and pain on passive ROM at the hip.
Anatomy:
The iliac crest is the weakest component of the pelvic ring during adolescence.
The avulsed fragment is usually displaced distally and laterally.
Treatment:
Conservative therapy includes 2-3 weeks of limited activity and walking with partial weight bearing restrictions and crutches. May also include bed rest with the affected lower extremity positioned with the hip and knee in flexion to ensure minimal tension of the muscles attaching to the ASIS. This is considered for minimally displaced fractures in younger children.
Surgical management generally consists of ORIF with a lag screw, and is generally recommended for patients with fracture fragments > 3cm or severely displaced fragments that cause compression of the lateral cutaneous nerve resulting in meralgia parasthetica.
Rossi F, Dragoni S. Acute avulsion fractures of the pelvis in adolescent competitive athletes: prevalence, location and sports distribution of 203 cases collected. Skeletal Radiol. 2001;30(3):127-31.
Kautzner J, Trc T, Havlas V. Comparison of conservative against surgical treatment of anterior-superior iliac spine avulsion fractures in children and adolescents. Int Orthop. 2014;38(7):1495-8.
Category: Pediatrics
Keywords: ENT, post tonsillectomy bleeding, T and A (PubMed Search)
Posted: 1/17/2020 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Tonsillectomy and adenoidectomy (T&A) is the second most common ambulatory surgery performed in the US. Children younger than 3 years, children with craniofacial disorders or sleep apnea are typically admitted overnight as studies have shown an increase rate of airway or respiratory complications in this population.
The most common late complications include bleeding and dehydration. Other complications include nausea, respiratory issues and pain.
Post-operatively, the overall 30-day emergency department return rate is up to 13.3%. Children ages 2 and younger were more likely to present to the ED. There is significantly higher risk of dehydration for children under 4 years. Children over the age of 6 had significantly higher bleeding risk and need for reoperation for hemorrhage control.
Lindquist NR, Feng Z and Mukerji SS. Age-related causes of emergency department visits after pediatric adenotonsillectomy at a tertiary pediatric referral center. International Journal of Pediatric Otorhinolaryngology 2019; 127: 109668.
Category: Pediatrics
Keywords: Urinary retention, formulas (PubMed Search)
Posted: 12/20/2019 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Urinary retention in pediatrics is defined as the inability to void for more than 12 hours in the presence of a palpable bladder or a urine volume greater than expected for age.
Maximum urine volume calculation for age: (age in years + 2) x 30ml.
Causes of urinary retention include mechanical obstruction, infection, fecal impaction, neurological disorders, gynecological disorders and behavioral problems.
The distribution is bimodal occurring between 3 and 5 years and 10 to 13 years.
Nevo A, Mano R, Livne P, Sivan B and Ben-Meir. Urinary Retention in Children. Urology 2014; 84(6):1475-1479.
Category: Pediatrics
Posted: 11/29/2019 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Antibiotic stewardship has led various organizations such as the AAP, AAFP, and IDSA to introduce two different approaches to the treatment of acute otitis media (AOM):
Immediate treatment with antibiotics should always include the following patients:
The observation approach can be considered in the following very slect patient group:
Often the issue with pediatric AOM isn't necessarily the overprescribing of antibiotics, but the inaccurate/inappropriate over diagnosis of acute otitis media. An erythematous tympanic membrane does not equal AOM. Crying and fever can result in a red TM. Fluid seen behind the TM, is often just serous otitis media, which isn't AOM.
When antibiotics are warranted, first-line treatment is with high dose amoxicillin, 90 mg/kg per day divided into two doses; unless the child has received beta-lactam antibiotics in the previous 90 days and/or also has puruent conjunctivitis mandating amoxicillin-clavulanate instead. In the later case, prescribing the Augment ES, 600 mg/5mL formlation with a lower clavulanic concentration lessening GI upset and diarrhea is prefered.
Liebeerthal AS, et al. The diagnosis and management of acute otitis media. Pediatrics 2013; 131.
Shaikh N, et al. Development of an algorithm for the diagnosis of otitis media. Acad Pediatr 2012;12:214.
Category: Pediatrics
Keywords: Sore throat, strep throat (PubMed Search)
Posted: 11/15/2019 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Streptococcal pharyngitis is common in the pediatric population however in children younger than 3 years, group A streptococcus (GAS) is a rare cause of sore throat and sequela including acute rheumatic fever are very rare. Inappropriate testing leads to increased healthcare and unnecessary exposure to antibiotics.
The national guidelines published by the Infectious Diseases Society of America do NOT recommend GAS testing in children less than the age of 3 years unless the patient meets clinical criteria and has a home contact with documented GAS.
Ahluwalia et al. Reducing streptococcal testing in patients less than 3 years old in an emergency department. Pediatrics 2019;144:4.
Category: Pediatrics
Keywords: lactated ringer, LR, normal saline, NS (PubMed Search)
Posted: 10/25/2019 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Bottom line: Balance fluid resuscitation with LR was not associated with improved outcomes compared to NS and pediatric sepsis. Selective LR use necessitates a prospective trial to definitively determine comparative effects among crystalloids.
1. Weiss SL, Keele L, Balanmuth F, Vendetti N, Ross R, Fitzgerald JC, Gerber JS. Crystalloid Fluid Choice and Clinical Outcomes in Pediatric Sepsis: A Matched Retrospective Cohort Study. J Pdatr.207 Mar:182:304-310.
2. Balamuth F, Kittick M, McBride P, Woodford AL, Vestal N, Casper TC, Metheney M, Smith K, Atkin NJ, Baren JM, Dean JM, Kuppermann N, Weiss SL. Pragmatic Pediatric Trial of Balanced versus Normal Saline Fluid in Sepsis: The PRoMPT BOLUS Randomized Controlled Trial Pilot Feasibility Study. Acad Emerg Med. 2019 Jun 10
Category: Pediatrics
Keywords: sedation, autism spectrum disorder (PubMed Search)
Posted: 10/18/2019 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Brown et al. Procedural sedation in children with autism spectrum disorders in the emergency department. Am J Emerg Med. 2019 Aug;37(8):1404-1408.
Category: Pediatrics
Keywords: Orthopedics, compartment syndrome (PubMed Search)
Posted: 9/20/2019 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
- Tibial tubercle avulsion fractures are rare and pediatrics, accounting for less than 3% of all epiphyseal injuries in children ages 11-17 years.
- The typical mechanism is a sudden forceful quadriceps contraction. Patients present with sudden pain after sprinting or jumping with pain, bruising, deformity or swelling over the tibial tubercle and with a decrease ability to extend the leg.
- 10 to 20% of cases result in anterior compartment syndrome related to the rupture of the anterior tibial recurrent artery.
- Although directly measured intra-compartmental pressures can facilitate the diagnosis of compartment syndrome, interpretation of these values can be challenging with healthy children having higher average lower leg compartment pressures than adults. Treatment of subsequent compartment syndrome is often based on a high index of suspicion.
Yue et al. Bilateral tibial tubercle avulsion fractures: Pediatric orthopedic injury at high risk for compartment syndrome. The American Journal of Emergency Medicine. Available online May 2019.
Category: Pediatrics
Keywords: UTIcalc, SBI, serious bacterial infection, febrile infant, urinary tract infection (PubMed Search)
Posted: 9/13/2019 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Question: In febrile children younger than 2 years, what combination of clinical and laboratory variables best predicts the probability of a urinary tract infection?
Given that urinary tract infections (UTI) are the most common source of serious or invasive bacterial infections in young febrile infants, early identification and treatment has the potential to reduce poor outcomes. Wouldn't it be great if there was an easy way to identify patients at highest risk?
Researchers from the Children’s Hospital of Pittsburgh formulated a calculator (UTICalc) that first estimates the probability of urinary tract infection (UTI) based on clinical variables and then updates that probability based on laboratory results.
Bottom line:
The UTICalc calculator can be used to guide to tailor testing and treatment in children with suspected urinary tract infection with the hope of improving outcomes for children with UTI by reducing the number of treatment delays.
Go ahead and give it a click!! https://uticalc.pitt.edu/
Shaikh N, Hoberman A, Hum SW, Alberty A, Muniz G, Kurs-Lasky M, Landsittel D, Shope T. Development and Validation of a Calculator for Estimating the Probability of Urinary Tract Infection in Young Febrile Children. JAMA Pediatr. 2018 Jun 1;172(6):550-556.
Category: Pediatrics
Posted: 8/31/2019 by Rose Chasm, MD
Click here to contact Rose Chasm, MD
There is no standardized national reporting of dog bites in the US. Based on the reported figures, it is estimated that 2% of Americans are bitten annually, and children are affected disproportionately. With kids, it's usually the family dog, and occurs at home.
To avoid infection, usually from Pasturella species, many of us were taught never to primarily repair dog bites by suturing, and to always prescribe prophylactic antibiotic coverage with amoxicillin-clavulanate. However, the literature recommends otherwise in certain cases.
Bite wounds to the face and hands should have special considerations. In general, face wounds heal with lower rates of infection, but provide the greatest concern for cosmetic appearance. Hand wounds have notoriously higher rates of infection.
The latest recommendations for dog bites are as follows:
1. All dog bites should be copiously irrigated under high pressure.
2. Dog bites to the face should be primarily repaired when <8 hours old, as infection rates are not significantly different and cosmesis is greatly improved.
3. Injuries to the hands should be left open, unless function is in jeopardy or there are neurovascular concerns.
4. Prophylactic antibiotics do not always have to be prescribed, especially in low risk patients. Examples of high risk patients include, but are not limited to: primarily repaired bites, injuries in the hand, >8 hours old, deep or macerated or multiple bites, and the immunocompromised.
Paschos NK et al. Primary closure versus non-closure of dog bite wounds. A randomised controlled tira. Injury 2014 45(1): 23l7-40
Chen, HH et al. Analysis of Pediatric Facial Dog Bites. Cranomaxillofac Trauma Reconstr. 2013 Dec; 6(4):225-232
Ellis, R; Ellis, C (2014). "Dog and cat bites". American Family Physician. 90 (4): 239–43.
Category: Pediatrics
Keywords: NV exam, neurovascular, upper extremity injury, orthopedics, hand, fracture, supracondylar (PubMed Search)
Posted: 5/24/2019 by Mimi Lu, MD
(Updated: 8/23/2019)
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: GSW, mass shooting, bleeding (PubMed Search)
Posted: 8/16/2019 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
Gunshot injuries are a leading cause of morbidity and mortality in the pediatric population. The Pediatric Trauma Society supports the use of tourniquets in severe extremity trauma. The Combat Application Tourniquet (CAT) that is commonly used in adults has not been prospectively tested in children. This study used 60 children ages 6 through 16 years and applied a CAT to the upper arm and thigh while monitoring the peripheral pulse pressure by Doppler. The CAT was successful in occluding arterial blood flow in all of the upper extremities and in 93% of the lower extremities.
Bottom line: The combat application tourniquet can stop arterial bleeding in the school aged child.
Harcke et al. Adult tourniquet use for school-age emergencies. Pediatrics. 2109; 143 (6) e:20183447.
Category: Pediatrics
Keywords: Keppra, Dilantin, status epilepticus (PubMed Search)
Posted: 7/20/2019 by Jenny Guyther, MD
(Updated: 5/13/2026)
Click here to contact Jenny Guyther, MD
-Benzodiazepines alone are effective in terminating status epilepticus in 40 to 60% of pediatric patients
-The guidelines for second line agents are based on observational studies and expert opinion
-Adverse effects of phenytoin include hepatotoxicity, pancytopenia, Stevens-Johnson syndrome, extravasation injuries, hypotension and arrhythmias
- Levetiracetam has a reduced risk of serious adverse events, greater compatibility with IV fluids and can be given in 5 minutes versus 20 minutes for phenytoin.
Bottom line: In a recent randomized control trial they found that levetiracetam was not superior to phenytoin as a second line agent for management of convulsive status epilepticus in children. There was no difference between efficacy or safety outcomes between the two groups.
Phenytoin is the second line treatment for pediatric convulsive status epilepticus after failure of first-line benzodiazepines but is only effective in approximately 60% of cases. This study was an open label, multicenter, randomized control trial conducted in Australia and New Zealand with children aged 3 months to 16 years with status epilepticus who had failed first-line benzodiazepine treatment. Patients were randomly assigned to to receive 20 mg/kg of phenytoin or 40 mg/kg of levetiracetam with the primary outcome being seizure resolution at 5 minutes
There were 233 children included in the study and seizure activity stopped in 60% of the patients in the phenytoin group and 50% of the patients in the levetiracetam which was not a statistically significant difference.
Dalziel at al. Levetiracetam versus phenytoin for second line treatment of convulsive status epilepticus in children; an open label, multicenter, randomized control trial. The Lancet. Published online April 17, 2019.
Category: Pediatrics
Keywords: appendicitis, hospitalization, operative management (PubMed Search)
Posted: 6/21/2019 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Fugazzola et al. Early appendectomy versus conservative management and complicated acute appendicitis in children: a meta-analysis. J Pediatr Surg. 2019 Feb 25 S0002-3468 (19)30125-3.
Category: Pediatrics
Posted: 5/24/2019 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Presentation:
- Prepubertal females are especially susceptible to urethral prolapse
- Can present incidentally is a painless mass found during bathing or on exam
- More commonly presents as urogenital bleeding, dysuria, or (rarely) urinary retention
Evaluation:
- Appears as a partial or circumferential "donut" of bright red, often friable prolapsed mucosa
- Typically occurs in the setting of UTI, cough, or constipation
- Need to rule out complications: UTI, urethral necrosis, and urinary retention
Treatment:
- Medical management start with sitz baths twice daily and addressing causative factors (treatment constipation, UTI, etc.)
- Can add either topical corticosteroid (hydrocortisone) or estrogen (Estrace or Premarin 0.01% twice daily)
- Urology follow-up necessary as many will require surgical resection of prolapsed mucosa
Category: Pediatrics
Keywords: ingestion, drug overdose, marijuana (PubMed Search)
Posted: 5/17/2019 by Jenny Guyther, MD
Click here to contact Jenny Guyther, MD
Washington state was one of the first states to legalize recreational marijuana use. Toxicology call center data was collected on patient's 9 years old and younger with marijuana exposure between July 2010 and July 2016. There were 161 cases during that time frame and of those 130 occurred after the legalization of recreational marijuana (over a 2.5 year period). The median age range was 2 years old. There were increasing cases noted after recreational marijuana was legalized and again after marijuana shops became legal.
Thomas et al. Unintentional pediatric marijuana exposures prior to and after localization and commercial availability of recreational marijuana in Washington state. J Emerg Med 2019 Mar 4.S0736-4679 (19).
