Category: Orthopedics
Keywords: Apprehension test, patellar dislocation, (PubMed Search)
Posted: 9/8/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Apprehension test for patellar dislocation
Test is used to access for the possibility of a patellar dislocation, prior to evaluation, now spontaneously reduced.
Similar to the shoulder apprehension test
Designed to place the patella in a position of imminent subluxation or dislocation
http://mulla.pri.ee/Kelley%27s%20Textbook%20of%20Rheumatology,%208th%20ed./HTML/f4-u1.0-B978-1-4160-3285-4..10042-7..gr16.jpg
http://www.youtube.com/watch?v=9AJxcbd9g8A
Place the knee in 20 - 30 degrees of flexion with the quadripces relaxed. Grasp the patella and attempt to place lateral directed stress.
If the patella is about to dislocate, the patient will experience apprehension due to the familiar pattern of dislocation, report the laxity and resist further motion by contracting the quadriceps
Category: Orthopedics
Keywords: shoulder dislocation, apprehension (PubMed Search)
Posted: 8/25/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Apprehension test for shoulder dislocation
Tests for chronic shoulder dislocation
Similar to the patellar apprehension test
Designed to place the humeral head in a position of imminent subluxation or dislocation
http://www.maitrise-orthop.com/corpusmaitri/orthopaedic/112_kelly/kelly-fig11.jpg
ABduct and externally rotate arm to a position where the shoulder may dislocate
If the shoulder is about to dislocate, the patient will experience apprehension due to the familiar pattern of dislocation, report the laxity and resist further motion.
Category: Orthopedics
Keywords: lactate, synovial fluid, (PubMed Search)
Posted: 8/18/2012 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
The Analysis of Synovial Fluid Analysis
When trying to diagnosis a septic joint, it is common to order the following labs on the synovial fluid:
Unfortunately, there is no value of glucose or protein that has enough sensitivity and specificity to make the tests diagnostically helpful. Gram stains are only postive in culture positive septic joints in approximately 50% of the cases. Cultures take too long to be helpful in the ED. The synovial WBC count can be helpful if very high, but a low value does not ensure that the patient does not have a septic joint.
The one test that has been shown to have a Positive Likelihood ratio of Infinity is a synovial lactate level >10. A synovial lactate should be sent on all synovial fluid as a level of 10 and greater makes the diagnosis of septic arthritis, regardless of the gram stain or synovial WBC level.
Carpenter CR, Schuur JD, Everett WW, Pines JM. Evidence-based diagnostics: adult septic arthritis. Acad Emerg Med. 2011 Aug;18(8):781-96.
Category: Orthopedics
Keywords: Humerus Fractures (PubMed Search)
Posted: 7/21/2012 by Michael Bond, MD
(Updated: 8/28/2014)
Click here to contact Michael Bond, MD
Humerus Fractures, Proximal
Category: Orthopedics
Keywords: Ulnar nerve, compression, neuropathy, wrist (PubMed Search)
Posted: 7/14/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
The median nerve is not the only compression neuropathy of the wrist
The ulnar nerve can become compressed at the level of the wrist as it 1) enters Guyon's canal or 2) or as the deep branch curves around the hook of the hamate
Compression can occur due to carpal bone fractures, local inflammation, ganglias, lipomas, anatomic abnormalities, etc
In sports medicine, the most common mechanism is injury is seen in cyclists (cyclist/handlebar palsy)
http://www.hughston.com/hha/b_15_3_2a.jpg
Also seen in those who participate in racquet sports, baseball, and golf
Symptoms can be isolated motor (claw hand = rare), sensory or both
http://en.academic.ru/pictures/enwiki/85/Ulnar_claw.jpg
Can be associated w/ median nerve compression
Tx: Activity modification such as wearing padded gloves, padding the object, or changing hand position on the handlebars
If above fails, surgical decompression is very effective.
Category: Orthopedics
Keywords: Bennett, Rolando, fracture (PubMed Search)
Posted: 6/30/2012 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
First Metacarpal Fractures:
There are two types of fractures that commonly occur at the base of the 1st metacarpal. They are:
Bennett Fracture: This is an intraarticular fracture at the base of the 1st metacarpal that always involves some degree of subluxation or dislocation of the 1st carpometacarpal joint.
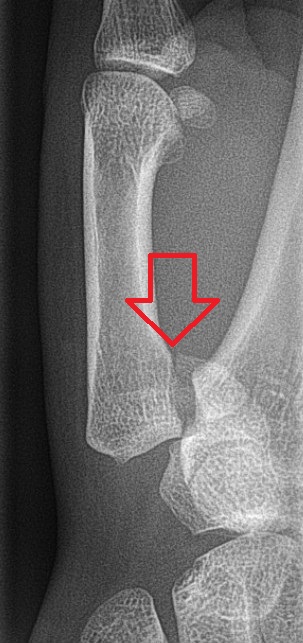
Image from Wikipedia Commons
Rolando Fracture: This is a communited intraarticular fracture at the base of the first metacarpal that typically has a T or Y shaped configuration with 3 fragments.

Image courtesy of WikiPedia Commons
Category: Orthopedics
Keywords: knee, cartilage, physical activity (PubMed Search)
Posted: 6/23/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
I am often asked whether physical activity has a positive or negative effect on the overall health of knee cartilage. The answer is unclear. Published data are conflicting.
What is known and generally agreed on:
1) Physical activity has been shown to facilitate cartilage development in children
2) Forced immobility (spinal cord injury) results in rapid cartilage loss
3) The medial knee compartment experiences significant mechanical loads during weight-bearing activity and is often the primary site of knee OA
A recent study attempted to answer whether 1) long-term (10yrs) participation in vigorous physical activity would benefit knee cartilage in healthy adults and 2) whether there were certain subgroups with asymptomatic preexisting structural knee changes which predict a harmful cartilage response to long-term physical activity.
Vigorous = activity generating sweating or SOB at least 20min 1/wk
Healthy older adults (mean age 57.8 yr) performing persistent vigorous physical activity had an increased risk (odds ratio 1.5) of worsening medial knee cartilage defects but not of a change in cartilage volume
In those w/ asymptomatic preexisting structural knee changes, there was worsening of cartilage defects (odds ratio 3.4) and a trend toward increased rate of loss of cartilage volume (again in the medial knee compartment)
Long-term effects of vigorous physical activity may depend on the preexisting health of the joint
Teichtahl, A.J., et al. Effect of long-term vigorous physical activity on healthy adult knee cartilage. Medicine and Science in Sports and Exercise. June 2012
Category: Orthopedics
Keywords: back, vertebae, fracture (PubMed Search)
Posted: 6/9/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
• Wedge compression fractures
http://jbjs.org/data/Journals/JBJS/855/JBJA0851224560G02.jpeg
Category: Orthopedics
Keywords: hamate, wrist, fracture (PubMed Search)
Posted: 5/26/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Hamate Fractures
Occur in two locations: the body of the hamate and the hook (hamular process) of the hamate
Fractures are present in 2 to 4% of carpal bone fractures
Body fractures are less common and are associated with dislocation of the fourth and fifth metacarpals
Axial force transmitted down the metacarpal shaft (a fall or fist strike)
Hook fractures occur from a direct force from an object strikes the palm such as that from a bat, golf club or racket
Have increased suspicion in these athletes who present w/ ulnar sided wrist pain
Diagnosis is frequently missed; chronic fractures are associated w/ flexor tendon rupture and ulnar neuropathy
PE: Tenderness localized over the hamate (in the hypothenar eminence) and over the dorsal ulnar aspect of the wrist. Swelling may be present. Look for resisted flexion of the 5th digit when the wrist is held in ulnar deviation. May note sensory changes in ulnar nerve distribution
Imaging: PA and lateral views of the wrist will show a body fracture but will frequently MISS a fracture of the hook of the hamate. In those with a clinical suspicion for this entity, order a “carpal tunnel view.” In the proper clinical setting, CT imaging is excellent for those with high suspicion and normal plain films.
Category: Orthopedics
Keywords: Elbow, osteochondritis, capitellum (PubMed Search)
Posted: 5/12/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Panner's disease refers to osteochondrosis of the capitellum.
Affects the dominant elbow of boys between the ages of 5 and 10
Associated with the repetitive trauma of throwing
Must be differentiated from osteochondrosis dissicans (occurs in the older child >13yo)
Hx: Intermittent pain and stiffness of the elbow. Better w rest, worse w activity.
PE: tenderness over capitellum w/ slight effusion. Loss of 20 degrees full extension
The articular surface of the capitellum appears irregular with areas of radiolucency.
Tx: Symptomatic treatment with rest. In severe cases a long arm splint/cast may be applied for 2-3 weeks.
http://www.ultrasoundcases.info/files/Jpg/org_34277-Afbeelding1.jpg
Category: Orthopedics
Keywords: Inferior shoulder dislocation (PubMed Search)
Posted: 4/28/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Luxatio erecta, aka inferior shoulder dislocation, is an uncommon form of shoulder dislocation (0.5-2%)
2 Mechanisms: 1) Forceful, direct axial loading of an ABducted arm.
2) Hyperabduction of the arm leads to impingement of the humeral head against the acromion, If forceful enough, this leverage can rupture the capsule and drive the humeral head downward, resulting in an inferior dislocation. This mechanism is more common.
Classic presentation: Arm locked in marked ABduction with the flexed forearm lying above the head.
http://uconnemig.files.wordpress.com/2011/11/emimages-8c.jpg
http://img.medscape.com/pi/features/slideshow-slide/sdrt/fig1.jpg
http://www.mypacs.net/repos/mpv3_repo/viz/full/76563/3828172.jpg
One may palpate the humeral head against the lateral chest wall
Bony injuries include fractures to surrounding structures such as the coracoid process, acromion, glenoid rim, clavicle, greater tuberosity and humeral head.
Nerve injuries include damage to the brachial plexus/axillary nerve (usually reversed with reduction)
Vascular injuries: Axillary artery thrombosis
Category: Orthopedics
Posted: 4/21/2012 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
Some quick board review pearls. Remember these fractures/dislocations and the neurologic injury that is associated with them
Category: Orthopedics
Keywords: stress fracture, shin splints (PubMed Search)
Posted: 4/7/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Exertional leg pain in the athlete carries a wide range of possible etiologies. In a recent review article, etiologies included, stress fracture (25%), exertional compartment syndrome (33%), medial tibial stress syndrome (13%), nerve entrapment (10%), and popliteal artery entrapment syndrome.
Medial Tibial Stress Syndrome (MTSS) is also known as shin splints. It is a repetitive-stress overuse injury.
Risk factors include: hyperpronation, higher BMI, increased hip internal rotation, and hyperplantar flexion.
While MTSS may be on a stress reaction spectrum that includes fracture, the causes are likely to also include tendinopathy and muscle dysfunction (tibialis anterior, posterior and soleus).
Radiographs will be normal with this condition. MRI and bone scan may show signal abnormality along the posterior medial tibial surface.
Treatment: In most cases participation in sports may continue. Also consider, rest/activity modification, ice, NSAIDs, physical therapy for calf stretching and strengthening, and rigid orthotics (to correct foot hyperpronation). Semi rigid and neoprene orthotics may be considered for prevention in those with a prior history.
Category: Orthopedics
Keywords: cardiac arrest, exercise, marathon (PubMed Search)
Posted: 3/24/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
A recent study looked at the risk of sudden cardiac death during a marathon.
Many isolated reports of sudden death make headlines in the national news.
However, of nearly 11 million runners, only 59 went into cardiac arrest during a race. This equates to an incidence rate of 0.54 per 100,000 participants,
This rate appears to be on par with sudden death from other athletic endeavors such as triathlons and college athletics.
Median age was 42. Men affected more than women (men also more likely to die from the event).
71% of events were fatal.
Further, risk is greater for both cardiac arrest and sudden death for full marathons than half marathons.
Interestingly, older patients fared better (increased survival in those >40yo), thought to be due to an increased incidence of hypertrophic cardiomyopathy in younger aged runners.
Baggish et al., New England Journal of Medicine.
Category: Orthopedics
Keywords: foot, plantar fasciitis (PubMed Search)
Posted: 3/10/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
The plantar fascia arises from the medial tuberosity of the calcaneous and extends to the proximal phalanges of the toes.
Pkantar Fasciitis is the most common cause of heel pain in adults.
Etiology is thought to be from a degenerative tear at the fascial origin followed by a tendinosis type reaction and .
Affects women 2x> men
More common in overweight patients.
Onset is insidious and not related to trauma.
Hx: Pain and tenderness directly over the medial calcaneal tuberosity and 1-2cm distally along the plantar fascia.
Pain is worse with prolonged standing/walking. Pain is most intense however when rising from a resting position such as first thing in the morning.
PE: Pain is increased with passive dorsiflexion of the toes. Tenderness to palaption over the medial calcaneal tuberosity and 1-2cm distally along the plantar fascia.(At times, one may have to apply increased pressure to approximate weight bearing type stress)
XR: Usually not necessary with a good history and exam. Heel spurs are seen in up to 50% with the disease (and in up to 20% without it!)
DDx: Tarsal tunnel syndrome. Calcaneal stress fracture. Fat pad atrophy. traumatic rupture of planter fascia.
Category: Orthopedics
Keywords: Heel, overuse injury, apophysis (PubMed Search)
Posted: 2/25/2012 by Brian Corwell, MD
(Updated: 5/15/2026)
Click here to contact Brian Corwell, MD
Severs disease
- Perhaps the most common overuse injury
-Pain is due to inflammation of the calcaneal apophysis growth plate
- Caused by repetitive microtrauma from the pull of the Achilles tendon on the apophysis.
- Occurs in young athletes ages 7-14
Sx’s bilateral in >50%
Hx – Gradual onset of posterior heel pain, worse with activity, better with rest.
PE – Tenderness at the insertion of the Achilles tendon onto the calcaneous. Swelling is mild.
This is a self limited condition because as the adolescent ages, the physis closes
Tx – Rest (no running or jumping), ice, NSAIDs, heel lifts/arch supports. Outpatient physical therapy for stretching and strengthening exercises.
Category: Orthopedics
Keywords: Morton, neuroma (PubMed Search)
Posted: 2/18/2012 by Michael Bond, MD
(Updated: 5/15/2026)
Click here to contact Michael Bond, MD
Morton's Neuroma
Thomas JL, et al. Diagnosis and treatment of forefoot disorders: Morton's intermetatarsal neuroma. Journal of Foot and Ankle Surgery. 2009;48:251.
Category: Orthopedics
Keywords: herbal, supplements, complementary medicine (PubMed Search)
Posted: 2/11/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Common herbs and supplements used to treat pain
1) Turmeric root - used for arthritis pain. Little evidence to support its use. May slow blood clotting/enhance anticoagulant/antiplatelet effects.
2) Boswellia - used for OA and RA pain. Little evidence to support its use.May interfere with anticoagulant drugs and leukotreine inhibitors.
3) St. John's Wort - used for HA, migraine, neuralgia, muscle pain, sciatica, fibromyalgia. Little to no evidence to support its use.May interfere with numerous medications including anticoagulants, digoxin and SZ medications.
4) Glucosamine and Chondroitin - used for OA, knee pain, back pain. The glucosamine/chondroitin arthritis intervention trial found that "the dietary supplements Glucosamine and Chondroitin, taken alone or in combination are generally ineffective for OA pain of the knee." May increase the effect of Warfarin.
5) KavaKava - used for HA, muscle pain. Insufficient evidence demonstrating effectiveness for treatment of painful conditions. May cause severe liver damage and potentiate drowsiness side effects of other medications.
6) Echinacea - used for pain, migraines, arthritis. Little evidence to support its use. May exacerbate symptoms of autoimmune disorders.
7) Valerian root – used for joint and muscle pain. Insufficient evidence to support its use. May potentiate sedative side effects of barbiturates and benzos.
8) Chinese Thunder God Vine – used for arthritis. There is some evidence to suggest that this agent has anti-inflammatory properties. Long term this agent may decrease bone mineral density in women, decrease fertility in men, and may produce GI side effects.
9) Feverfew – used for muscle pain, arthritis. Some evidence to suggest that may reduce frequency of migraine headaches. No evidence for benefit in RA. May enhance effects of anticoagulants and some drugs that undergo hepatic metabolism.
10) Cat’s claw – used for herpes zoster, bone pain, arthritis. Possible benefit for OA and RA in small studies in humans but no large study has shown benefit. May interact with clotting agents, BP meds and cyclosporine.
11) Black Cohosh – used for muscle pain and arthritis. Insufficient evidence demonstrating benefit. May be associated with severe liver side effects.
12) Bromelain – used for muscle pain, arthritis, knee pain. The NIH reports that bromelain may be effective for arthritis when used in combination with trypsin and rutin. May interact with amoxicillin and other antibiotics, anticoagulants and antiplatelet drugs.
13) Devil’s claw – used for muscle pain, back pain, arthritis, migraine. The NIH reports that “taking devil’s claw alone or with NSAIDs seems to help decrease OA related pain.” May increase effects of warfarin.
Category: Orthopedics
Keywords: Hip dislocation, technique, reduction (PubMed Search)
Posted: 1/28/2012 by Brian Corwell, MD
Click here to contact Brian Corwell, MD
Our old friend Captain Morgan (the rum pirate) may now be able to assist us during a shift, not just afterwards.
http://www.inquisitr.com/wp-content/2011/08/captain-morgans-pirate-ship-satisfaction-panama.jpg
In a small case series in last months Annals of Emergency Medicine, a new reduction maneuver was described as an alternative to the traditional Aliis's maneuver.
The maneuver is named after the pirate spokesperson for the similarities in body positioning.
The patient is placed supine on a stretcher. The pelvis is fixed to a backboard with a strap. The patient's hip and knee are flexed to 90 degrees. The physician places one foot on the back board with the same knee behind the patient's knee. By holding the patient's ankle down, the patient's knee is kept in flexion. The physician then lifts his/her calf, thereby applying an upward force to the hip while gently rotating the lower leg from side to side.
http://www.youtube.com/watch?v=l07K-mO2X84
with a slight variation
http://www.youtube.com/watch?v=sGQZaqB48rw
The success rate was 12 of 13 cases. The single failure occurred in a patient with an acetabular fracture with an intra-articular fragment requiring open reduction. There were no described neurovascular complications or injuries to the knee. The technique limits the physician's risk of back strain and of falling from the stretcher.
The Captain Morgan technique for the reduction of the dislocated hip.
Hendey GW, Avila A.
Ann Emerg Med. 2011 Dec;58(6):536-40. Epub 2011 Aug 12.
Category: Orthopedics
Keywords: Flexor, Tenosynovitis (PubMed Search)
Posted: 1/21/2012 by Michael Bond, MD
Click here to contact Michael Bond, MD
Flexor Tenosynovitis
You can follow this link, http://www.youtube.com/watch?v=qf9SW0ChsCU , to see the physical exam findings of flexor tenosynovitis
