Category: Vascular
Keywords: aortic dissection (PubMed Search)
Posted: 2/16/2009 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
BEWARE sudden onset thoracic back pain
Just reviewed a case last week of a person who presented with back pain (thoracic) as the sole manifestation of an aortic dissection. No chest pain, belly pain, etc. JUST severe, acute, thoracic back pain.
Keys to staying out of trouble:
Elefteriades, 2008
Category: Vascular
Keywords: Pulmonary Embolism (PubMed Search)
Posted: 2/3/2009 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Pulmonary Embolism-Beware Two Important Atypical Presentations
Seems like we have had several atypical PE presentations recently so I thought it timely to quickly highlight some of the well-reported presentations of pulmonary embolism. Remember, although we won't and can't diagnose every case, these types of presentations should at the very least prompt us to consider the diagnosis.
Atypical PE Presentations:
Category: Vascular
Posted: 1/12/2009 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Thrombolytic Therapy for Pulmonary Embolism
Indications for administration of fibrinolytic therapy for acute PE:
Kline. Carolinas Medical Center.
Stein. Pulmonary Embolism. 2008
Category: Vascular
Keywords: Acute, Aortic Dissection, Neurologic (PubMed Search)
Posted: 1/6/2009 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Neurologic Manifestations of Acute Aortic Dissection
A myriad of neurologic presentations of acute aortic dissection have been reported in the literature. Although classic CVA symptoms may occur, nonspecific neurologic symptoms are much more common
These include:
Take Home Point:
Elefteriades
Category: Vascular
Keywords: Hypertension, Epistaxis (PubMed Search)
Posted: 12/8/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Hypertension and Epistaxis
We commonly encounter patients with epistaxis who are found to be hypertensive. Some have taught over the years that hypertension causes nosebleeds and that some nose bleeds won't stop until the BP is lowered...
Some pearls about HTN/Epistaxis:
Category: Vascular
Keywords: Warfarin, Skin Necrosis (PubMed Search)
Posted: 12/1/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Warfarin-Induced Skin Necrosis (WISN)
Some pearls about a rare, but serious side effect of Warfarin...
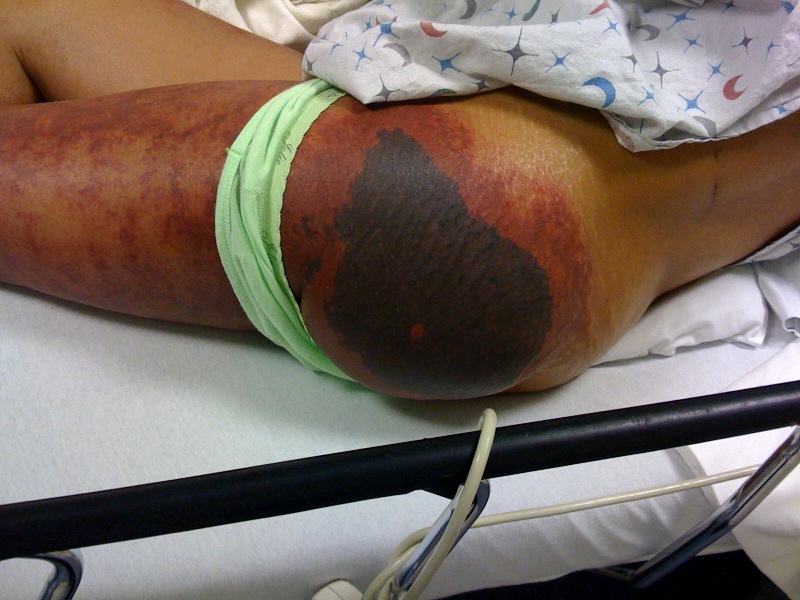
55 yo female presented to the ED on the day of hospital discharge for evaluation of this rash.
The rash began 4 days after starting Warfarin. Was being treated for a DVT.
Category: Vascular
Keywords: Hypertension (PubMed Search)
Posted: 11/24/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
What Hypertensive Patient Needs a Workup for End-Organ Damage?
Ah, the age old question...which hypertensive patients need an ED workup for end-organ damage? The "workup" for patients includes renal function, urinalysis, CXR, ECG, etc.
Some pearls regarding working patients up:
Category: Vascular
Keywords: hypertension (PubMed Search)
Posted: 11/10/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Category: Vascular
Keywords: PERC Rules (PubMed Search)
Posted: 11/4/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Category: Vascular
Keywords: Warfarin (PubMed Search)
Posted: 10/27/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Reversal of Warfarin
Reversal of Warfarin can be accomplished by administering any of the following:
A few pearls:
Category: Vascular
Keywords: HeparinPro (PubMed Search)
Posted: 10/20/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Anticoagulation with Heparin-How to Reverse?
So you just started Heparin on that ACS patient? Just bolused the patient in room 12 with the large PE with a slug of Heparin? The nurse tells you that one of them just vomited blood and the other just had a large bloody bowel movement. What to do, oh, what to do?
How to reverse Heparin...use Protamine:
Category: Vascular
Keywords: Thrombosis, Cerebral (PubMed Search)
Posted: 10/13/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Cerebral Venous Sinus Thrombosis (CVST)
An uncommon but very serious entity that leads to three distinct types of presentations:
Caused by thrombosis of one of the intracerebral venous sinuses (most commonly the transverse sinus) The major risk factor is hypercoagulable disease. May be the underlying cause of a majority of cases of idiopathic intracranial hypertension.
When to suspect:
Diagnosis:
Treat:
Category: Vascular
Keywords: Hypertension, Headache (PubMed Search)
Posted: 10/6/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Does Hypertension (elevated BP) Cause Headache?
This is an age old question that many of us have struggled with in the ED for many years...
Other questions include: Does elevated BP cause headaches? Do we need to scan hypertensive patients with headache just because they have a headache? At what level of BP does the BP actually cause headache?
A few quick pearls:
Category: Vascular
Keywords: Hypertension (PubMed Search)
Posted: 9/29/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Avoidable Pitfalls in Managing the Hypertensive Patient
We all see very hypertensive patients on almost every shift. Dr. Winters has an earlier pearl related to pitfalls in treating patients with hypertensive encephalopathy, but I thought it was time to reiterate just a few points.
Category: Vascular
Keywords: aortic dissection, chest xray (PubMed Search)
Posted: 9/23/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
So, how good is a screening CXR for aortic dissection?
vonKodolitsch, 2005
Category: Vascular
Keywords: Cardiovascular, CocaineC (PubMed Search)
Posted: 9/15/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Key Cardiovascular complications of cocaine:
Pearls:
Restrepo CS, et al. Cardiovascular complications of cocaine: Imaging findings. Emerg Radiol 2008
Category: Vascular
Keywords: Ischemia (PubMed Search)
Posted: 9/9/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Management of acute limb ischemia
Just a few pearls regarding acute limb ischemia
Vasc Surg Reviews 2007
Category: Vascular
Keywords: subrachnoid hemorrhageRebeleeding (PubMed Search)
Posted: 8/19/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Complications of Subarachnoid Hemorrhage
The three dreaded complications of SAH include the following:
Edlow, et al. Aneurysmal subarachnoid hemorrhage: update for emergency physicians. JEM 2008
Category: Vascular
Keywords: LMWH, PE, Pulmonary Embolism (PubMed Search)
Posted: 8/11/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Currently Approved LMWHs for the Treatment of Acute PE:
Make sure to monitor platelet counts regardless of agent chosen.
Konstantinides. Acute pulmonary embolism revisited. Heart. June 2008
Category: Vascular
Keywords: D-Dimer (PubMed Search)
Posted: 7/29/2008 by Rob Rogers, MD
(Updated: 5/1/2026)
Click here to contact Rob Rogers, MD
Causes of an Elevated D-Dimer
Don't forget the multiple causes of an elevated d-dimer:
**See attached PDF-Differential Diagnosis of Elevated D-Dimer
Journal of Thrombosis and Hemostasis, 2008
