Category: Critical Care
Posted: 10/16/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
There have been so many great talks at ACEP 2013, but Dr. Michael Winters' talk "The ICU is NOT Ready for Your Patient" was chock full of great critical care pearls. Here are just a few:
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Keywords: CPR, Cardiac Arrest, ACLS, Chest Compression (PubMed Search)
Posted: 10/4/2013 by John Greenwood, MD
Click here to contact John Greenwood, MD
Want to improve your chances of success in the resus room? Download a metronome app on your smartphone and set it to a rate of 100-120 beats per minute. There are a number of cheap (usually free) metronome applications for both iOS and Android devices.
A recent review looked at the evidence behind CPR feedback devices and found:
So instead of going to iTunes and downloading the Bee Gees, go over to the App store and download a free metronome. Your resus team will be able to stay on track with their compressions and even better - they won't have to hear you sing!
Category: Critical Care
Posted: 9/30/2013 by Haney Mallemat, MD
(Updated: 10/1/2013)
Click here to contact Haney Mallemat, MD
The efficacy of epinephrine during out-of hospital cardiac arrest has been questioned in recent years, especially with respect to neurologic outcomes (ref#1).
A recent study demonstrated both a survival and neurologic benefit to using epinephrine during in-hospital cardiac arrest when used in combination with vasopressin and methylprednisolone.
Researchers in Greece randomized 268 consecutive patients with in-hospital cardiac arrest to receive either epinephrine + placebo (control group; n=138) or vasopressin, epinephrine, and methylprednisolone (intervention arm; n=130)
Vasopressin (20 IU) was given with epinephrine each CPR cycle for the first 5 cycles; Epinephrine was given alone thereafter (if necessary)
Methylprednisolone (40 mg) was only given during the first CPR cycle.
If there was return of spontaneous circulation (ROSC) but the patient was in shock, 300 mg of methylprednisolone was given daily for up to 7 days.
Primary study end-points were ROSC for 20 minutes or more and survival to hospital discharge while monitoring for neurological outcome
The results were that patients in the intervention group had a statistically significant:
probability of ROSC for > 20 minutes (84% vs. 66%)
survival with good neurological outcomes (14% vs. 5%)
survival if shock was present post-ROSC (21% vs. 8%)
better hemodynamic parameters, less organ dysfunction, and better central venous saturation levels
Bottom-line: This study may present a promising new therapy for in-hospital cardiac arrest and should be strongly considered.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Keywords: Procalcitonin, Upper respiratory infections, antibiotics (PubMed Search)
Posted: 9/24/2013 by Feras Khan, MD
(Updated: 5/13/2026)
Click here to contact Feras Khan, MD
Background:
Clinical Question:
Meta-analysis:
Conclusions:
Limitations:
Bottom Line:
Clinical Outcomes Associated With Procalcitonin Algorithms to Guide Antibiotic Therapy in Respiratory Tract Infections
Philipp Schuetz, MD, MPH; Matthias Briel, MD, MSc; Beat Mueller, MD
JAMA. 2013;309(7):717-718. doi:10.1001/jama.2013.697.
http://jama.jamanetwork.com/article.aspx?articleid=1653510
Category: Critical Care
Posted: 9/17/2013 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
Peri-Intubation Cardiac Arrest
Heffner AC, Swords DS, Neale MN, Jones AE. Incidence and factors associated with cardiac arrest complicating emergency airway management. Resuscitation 2013. [Epub ahead of print].
Category: Critical Care
Keywords: critical care, necrotizing pneumonia, infectious disease, pulmonary (PubMed Search)
Posted: 9/5/2013 by John Greenwood, MD
(Updated: 9/10/2013)
Click here to contact John Greenwood, MD
Necrotizing Pneumonia
Necrotizing pneumonia is a rare, but potentially deadly complication of bacterial pneumonia.
It is characterized by the finding of pneumonic consolidation with multiple areas of necrosis within the lung parenchyma. Necrotic foci may coalesce, resulting in a localized lung abscess, or pulmonary gangrene if involving an entire lobe.
Most common pathogens: S. aureus, S. pneumoniae, and Klebsiella pneumonia.
Others include S. epidermidis, E. coli, Acinetobacter baumannii, H. influenzae and Pseudomonas.
Contrast-enhanced chest CT is the diagnostic test of choice and is also helpful in evaluating for parenchymal complications.
Empiric antibiotic therapy should include:
Consider an early surgical evaluation for the patient with necrotizing pneumonia complicated by septic shock, empyema, bronchopleural fistula, or hemoptysis.
Reference
Tsai YF, Ku YH. Necrotizing pneumonia: a rare complication of pneumonia requiring special consideration. Curr Opin Pulm Med. 2012 May; 18(3):246-52.
Category: Critical Care
Posted: 9/3/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
UEDVT comprise 10% of all DVTs (majority are lower extremity), but incidence of UEDVT is rising; UEDVTs are categorized into distal (veins distal to axillary vein) or proximal (from superior vena cava to axillary vein)
Compared to lower extremity DVT, UEDVTs have lower:
75% of UEDVT are secondary (indwelling catheters, pacemakers, malignancy, etc.) and 25% are primary in nature; #1 primary cause of UEDVT is Paget – Schroetter disease
Up to 25% of patients with primary UEDVTs are eventually found to have an underlying malignancy; patients with idiopathic UEDVT should be referred for cancer workup
Treatment includes removal of the catheter (if no longer needed) and:
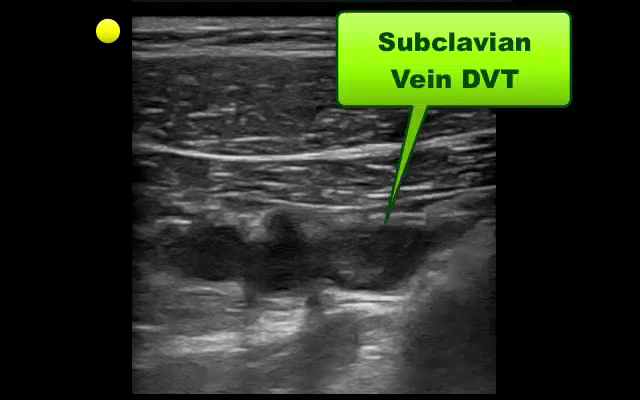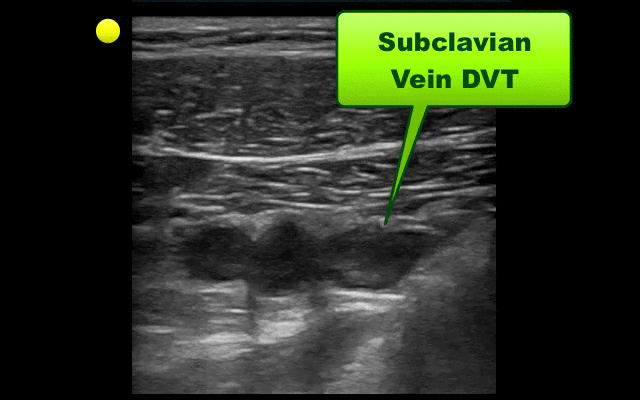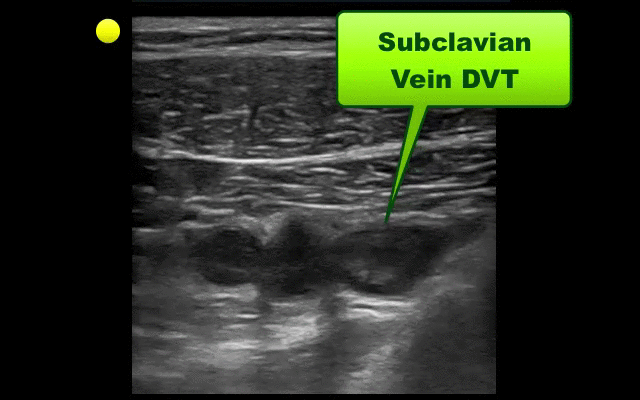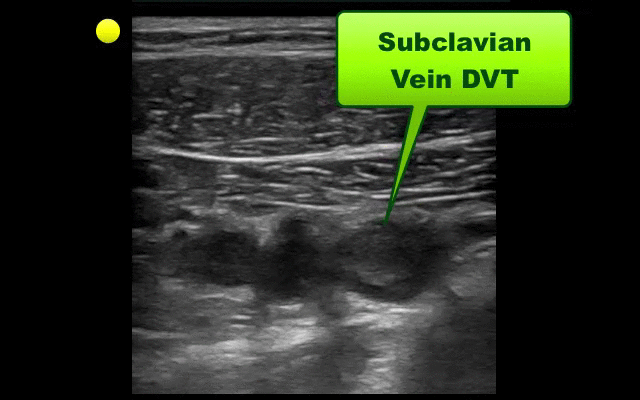
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Keywords: TIA, Minor Stroke, Antiplatelet therapy (PubMed Search)
Posted: 8/27/2013 by Feras Khan, MD
(Updated: 5/13/2026)
Click here to contact Feras Khan, MD
Background
Trial
Results
Conclusions
Bottom Line:
Clopidogrel with Aspirin in Acute Minor Stroke or Transient Ischemic Attack
Y. Wang and Others | N Engl J Med 2013;369:11-19 | Published Online June 26, 2013
Category: Critical Care
Posted: 8/14/2013 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Clostridium Difficile Associated Diarrhea and The Elderly Patient
Heppner HJ, et al. Infections in the Elderly. Crit Care Clin 2013; 29:757-774.
Category: Critical Care
Keywords: Neurocritical care, Ventilator Strategies, ARDS, Intracranial hemorrhage (PubMed Search)
Posted: 8/5/2013 by John Greenwood, MD
(Updated: 8/6/2013)
Click here to contact John Greenwood, MD
Bad brain, good lungs.... Right?
A recent retrospective study reviewed the incidence of acute respiratory distress syndrome (ARDS) in patients presenting with spontaneous intracerebral hemorrhage over a 10-year period. After reviewing 1,665 patients, the authors found that:
It's of particular importance to note that high tidal volume ventilation (>8cc/kg) was the single greatest modifiable factor for the development of ARDS.
Bottom line: Try and use lung-protective ventilation strategies (6-8cc/kg ideal body weight) and avoid excessive volume resuscitation in your critically-ill patients whenever possible. Even in cases of isolated intracerebral hemorrhage - where the patient's lungs may appear to be completely normal - traditional tidal volume settings may be harmful.
Category: Critical Care
Posted: 7/30/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Elderly patient who originally presented for severe pancreatitis now intubated for worsening hypoxemia. CXR is shown below, what's the diagnosis?
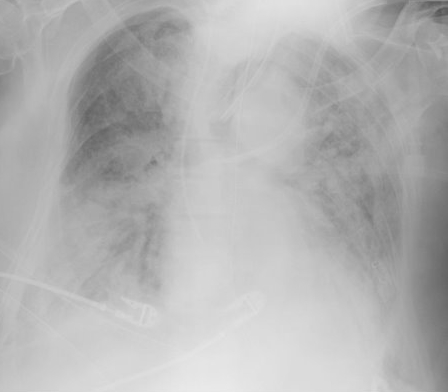
Acute Respiratory Distress Syndrome (ARDS)
Acute Respiratory Distress Syndrome (ARDS) is defined as hypoxemia secondary to increased pulmonary capillary permeability and non-hydrostatic (i.e., non-cardiogenic) leakage of fluid into the interstitial lung tissue and alveoli. Lung radiographs diffuse and symmetric infiltrates (see below)
ARDS may occur secondary to a primary (or pulmonary) insult (e.g., aspiration, pneumonia) or secondary (or systemic) insult (e.g., pancreatitis, trauma, etc.)
The newest classification system for ARDS no longer includes the previously known category of acute lung injury; there are three categories of ARDS determined by the PaO2 (on ABG) divided by administered FiO2 (as a fraction of 100%):
A number of interventions have been demonstrated to improve outcomes for patients with ARDS:
Follow me on Twitter (@criticalcarenow) or on Google+ (+criticalcarenow)
Category: Critical Care
Posted: 7/23/2013 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
HIV, ART, and the ICU
Tan DHS, Walmsley SL. Management of persons infected with human immunodeficiency virus requiring admission to the intensive care unit. Crit Care Clin 2013; 29:603-20.
Category: Critical Care
Posted: 7/16/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
COPD treatment guidelines (e.g., GOLD) recommend 10-14 days of steroid therapy following a COPD exacerbation to prevent recurrences; the supporting data is weak.
A recent noninferiority trial (here) compared patients with a severe COPD exacerbation who received either a 5-day course (n=156) or 14-day course (n=155) of prednisone 40mg.
The results were:
What you need to know:
Bottom-line: 5 days of prednisone may be as effective as 14-days for COPD exacerbations.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Posted: 7/2/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Hydroxyethyl starch (HES) is a colloid used for volume resuscitation in critically-ill patients.
Previous studies (click here) have compared crystalloids to HES during fluid resuscitation and have demonstrated that HES has an increased cost with more adverse effects. Adverse effects may include:
In the United States, the Federal Drug Administration published a warning on June 24th 2013 with respect to the use of HES in critically ill adult patients. Specifically, it warned about the use of HES in patients,
If a decision to use HES is made, the FDA warning advises to:
Bottom line: With an increased cost and evidence of harm compared to crystalloids, it appears the indications for use of HES are rapidly declining.
http://www.fda.gov/BiologicsBloodVaccines/SafetyAvailability/ucm358271.htm
Perner A., et al. Hydroxyethyl Starch 130/0.4 versus Ringer's Acetate in Severe Sepsis. NEJM. 2012 Jun 27.
MyBurgh, J. Hydroxyethyl Starch or Saline for Fluid Resuscitation in Intensive Care. N Engl J Med. 2012 Oct 17.
Category: Critical Care
Posted: 6/25/2013 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
CVP and Fluid Responsiveness
Marik PE, Cavallazzi R. Does the central venous pressure predict fluid responsiveness? An updated meta-analysis and a plea for some common sense. Crit Care Med 2013:41:1774-1781.
Category: Critical Care
Posted: 6/18/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Keep Immune Thrombocytopenic Purpura (ITP) in your differential for patients with thrombocytopenia and evidence of bleeding. Although ITP has classically been described in children, it can occur in adults; especially between 3rd- 4th decade.
Thrombocytopenia leads to the extravasation of blood from capillaries, leading to skin bruising, mucus membrane petechial bleeding, and intracranial hemorrhage.
ITP occurs from production of auto-antibodies which bind to circulating platelets. This leads to irreversible uptake by macrophages in the spleen. Causes of antibody production include:
Suspect ITP in patients with isolated thrombocytopenia on a CBC without other blood-line abnormalities. Abnormality in other blood-line warrants consideration of another diagnosis (e.g., leukemia).
ITP cannot be cured; treatments include:
Category: Critical Care
Posted: 6/11/2013 by Mike Winters, MBA, MD
Click here to contact Mike Winters, MBA, MD
Rhabdomyolysis in the Critically Ill
Shapiro ML, Baldea A, Luchette FA. Rhabdomyolysis in the Intensive Care Unit. J Intensive Care Med 2012; 27:335-342.
Category: Critical Care
Posted: 6/4/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
Therapeutic hypothermia (TH) following out-of-hospital cardiac arrest (OHCA) has increasingly been utilized since it was first described. TH following in-hospital cardiac arrest (IHCA), on the other hand, is not as commonplace or consistent despite a recommendation by the American Heart Association (AHA).
A recent prospective multi-center cohort-study demonstrated that of 67,498 patients with return of spontaneous circulation (ROSC) following IHCA only 2.0% of patients had TH initiated; of those 44.3% did not even achieve the target temperature (32-34 Celsius).
The factors found to be most associated with instituting TH were:
Bottom-line: Hospitals should consider instituting and adhering to local TH protocols for in-house cardiac arrests.
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
Category: Critical Care
Posted: 5/28/2013 by Mike Winters, MBA, MD
(Updated: 5/13/2026)
Click here to contact Mike Winters, MBA, MD
End-expiratory Occlusion Test
Monnet X, Teboul JL. Assessment of volume responsiveness during mechanical ventilation: recent advances. Critical Care 2013; 17:217.
Category: Critical Care
Posted: 5/21/2013 by Haney Mallemat, MD
Click here to contact Haney Mallemat, MD
The Macklin Effect
Pneumomediastinum (click here for image) may be caused by many things:
The "Macklin Effect" is typically a self-limiting condition leading to spontaneous pneumomediastinum and massive subcutaneous emphysema after the following:
Pneumomediastinum secondary to the Macklin effect frequently leads to an extensive workup to search for other causes of mediastinal air. Although, no consensus exists regarding the appropriate workup, the patient's history should guide the workup to avoid unnecessary imaging, needless dietary restriction, unjustified antibiotic administration, and prolonged hospitalization.
Treatment of spontaneous pneumomediastinum includes:
Follow me on Twitter (@criticalcarenow) or Google+ (+criticalcarenow)
