Category: International EM
Keywords: tetanus, global, international, infectious disease (PubMed Search)
Posted: 6/25/2014 by Andrea Tenner, MD
(Updated: 4/14/2026)
Click here to contact Andrea Tenner, MD
General Information: Tetanus is caused by the toxin of Clostridium tetani--a gram-positive bacillus found in soil and animal excrement. It is a life-threatening but preventable disease. Cases have declined by > 95% in the past 65 years, but dozens of cases still occur annually in the US and it is still frequently seen in developing countries.
Clinical Presentation:
Diagnosis:
Clinical Case Definition: In the absence of a more likely diagnosis, an acute illness with muscle spasms or hypertonia. There is no diagnostic laboratory test for tetanus.
Treatment:
Bottom Line:
Tetanus is not as rare as we would like to think. Acute diagnostic acumen and assertive clinical management can help save the life of someone with this potentially deadly disease
University of Maryland Section for Global Emergency Health
Author: Jon Mark Hirshon, MD, MPH, PhD
http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6012a1.htm
http://www.cdc.gov/vaccines/pubs/surv-manual/chpt16-tetanus.html
http://emedicine.medscape.com/article/229594-treatment
Category: International EM
Keywords: Schistosomiasis, parasites, international (PubMed Search)
Posted: 6/18/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Clinical Presentation:
A 35-year-old female presents to your emergency department complaining of fever, malaise, myalgias, headache and an urticarial rash. Her physical exam reveals a papular rash and hepatosplenomegaly. You also find out that she traveled to Sudan 6 weeks earlier. She stayed mostly in Kharotum, but while there, she swam in the Nile. You send a smear for malaria, which is negative. What other major parasite should you consider?
Diagnosis:
Discussion:
While the acute presentation is generally non-specific, chronic complications may be more serious. Many organ systems can be impacted and symptoms of chronic infection can include liver dysfunction, including portal hypertension and esophageal varacies or hematuria and renal failure.
Treatment:
Bottom Line:
Consider a broader differential in travelers. There are many infectious killers that can be easily treated.
University of Maryland Section of Global Emergency Health
Author: Jon Mark Hirshon, MD, MPH, PhD
Category: International EM
Keywords: Malaria, International, Travel, fever (PubMed Search)
Posted: 6/11/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation:
A 64 yo male with a history of IDDM presents with generalized fatigue. He felt so weak last night that he missed his pm dose of Lantus and vomited this morning. He arrived with a critically elevated BG of 590. He flew to the US from Sierra Leone 3 days ago.
Labs include:
Wbc 3.5 Plt 34 Hb 12 Hct 36
Na 125 CL 93 Co2 14 K 4.5 BUN 25 Cr 1.9 Glu 590 AG 18
VBG pH 7.23
Clinical Question:
Other than treating his diabetic ketoacidosis and renal failure, would you send any further tests?
Answer:
Thick smear for Malaria.
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Bradford Schwartz, MD
Ansari, Khoharo, Akhund, and Qureshi. Thrombocytopenia in plasmodium falciparum malaria.J Ayub Med Coll Abbottabad. 2009 Apr-Jun;21(2):145-7.
Kumar and Shashirekha. Thrombocytopenia--an indicator of acute vivax malaria. Indian J Pathol Microbiol. 2006 Oct;49(4):505-8.
Lacerda, Mourao, Coelho, and Santos. Thrombocytopenia in malaria: who cares? Mem Inst Oswaldo Cruz. 2011 Aug;106 Suppl 1:52-63.
Category: International EM
Keywords: diarrhea, international, infectious disease, stool, parasite (PubMed Search)
Posted: 5/28/2014 by Andrea Tenner, MD
(Updated: 4/14/2026)
Click here to contact Andrea Tenner, MD
General Information:
Bottom Line for the EM Physician: Use these guidelines to test stool only when helpful to patient care and avoid flushing resources down the toilet.
University of Maryland Section of Global Emergency Health
Author: Alex Skog
DuPont HL. Acute infectious diarrhea in immunocompetent adults. N Engl J Med. 2014 Apr 17;370(16):1532–40.
Fischer Walker CL, Perin J, Aryee MJ, Boschi-Pinto C, Black RE. Diarrhea incidence in low- and middle-income countries in 1990 and 2010: a systematic review. BMC Public Health. 2012;12:220.
Category: International EM
Keywords: Mesoamerican, Nephropathy, Central America, Nicaragua, El Salvador, (PubMed Search)
Posted: 5/21/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Area of the world affected:
Relevance to the US physician:
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Emilie J.B. Calvello, MD, MPH & Alex Skog
Correa-Rotter R, Wesseling C, Johnson RJ. CKD of unknown origin in Central America: the case for a Mesoamerican nephropathy. Am J Kidney Dis. 2014 Mar;63(3):506–20.
Category: International EM
Keywords: rabies, global, video, international, infectious disease (PubMed Search)
Posted: 5/14/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Clinical Presentation
Rabies is, initially, a clinical diagnosis. To see what a patient with rabies looks like, check out this 3 minute YouTube video: (There is a bit of commentary by the person who posted it at the beginning that you might want to skip through.)
https://www.youtube.com/watch?v=EZbrNN9KeUI
Bottom Line
Rabies, while a rare disease in the US, can occur through either contact with infected animals (especially while traveling) or via organ transplantation. Recognizing the clinical syndrome is key to diagnosis.
University of Maryland Section for Global Emergency Health
Author: Andi Tenner, MD, MPH, FACEP
http://www.cdc.gov/rabies/location/usa/surveillance/human_rabies.html
Category: International EM
Keywords: Polio, Vaccine, Eradication (PubMed Search)
Posted: 5/7/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Relevance to the EM Physician:
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Jenny Reifel Saltzberg, MD
Category: International EM
Keywords: Seizure, International, Valproate (PubMed Search)
Posted: 4/30/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Background Information:
ACEP has recently revised its 2004 policy on critical issues in the evaluation and management of adult patients with seizures in the emergency department.
Pertinent Study Design and Conclusions:
Bottom Line:
As an alternative to phenytoin or fosphenytoin, valproate may be considered for refractory convulsive status epilepticus if benzodiazepines fail.
University of Maryland Section of Global Emergency Health
Author: Walid Hammad, MB ChB
Category: International EM
Keywords: International, virus, middle east, (PubMed Search)
Posted: 4/23/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Area of the world affected:
Relevance to the US physician:
Bottom Line:
Evaluate patients for MERS-CoV infection if they develop fever and pneumonia within 14 days after traveling to countries in or near the Middle East or if they had close contact with someone from this area.
University of Maryland Section of Global Emergency Health
Author: Walid Hammad, MB ChB
Category: International EM
Keywords: International, Mental Health, burden of disease (PubMed Search)
Posted: 4/15/2014 by Andrea Tenner, MD
(Updated: 4/16/2014)
Click here to contact Andrea Tenner, MD
General Information:
Relevance to the US physician:
Bottom Line:
Mental illness is an often-forgotten cause of significant morbidity worldwide. Front-line care delivered by appropriately trained and supervised community-based health workers operating in partnership with emergency physicians, primary care physicians, and mental health specialists is key to address this health crisis.
University of Maryland Section of Global Emergency Health
Author: Terrence Mulligan DO, MPH
Transforming Lives, Enhancing Communities — Innovations in Global Mental Health. February 6, 2014 Patel V. and Saxena S. N Engl J Med 2014; 370:498-501
Category: International EM
Keywords: International, Fever, Hemorrhagic (PubMed Search)
Posted: 4/9/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Clinical Presentation:
Diagnosis:
Treatment:
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Veronica Pei
The CDC Yellow Book 2014 available at: http://wwwnc.cdc.gov/travel/yellowbook/2014/chapter-3-infectious-diseases-related-to-travel/viral-hemorrhagic-fevers
Category: International EM
Keywords: HIV, global health, infectious disease, rash, puritis (PubMed Search)
Posted: 4/1/2014 by Andrea Tenner, MD
(Updated: 4/2/2014)
Click here to contact Andrea Tenner, MD
You are working in a clinic in Tanzania (or Baltimore, for that matter) when a 24 year old presents with this itchy rash on his feet. What's the diagnosis and what underlying systemic condition does it indicate?
Pruritic Papular Eruptions in HIV
Presentation:
University of Maryland Section for Global Emergency Health
Authors: Van Pham, MD and Colleen Holley, MD
Category: International EM
Keywords: multiple myeloma, x-ray, global, neoplasm (PubMed Search)
Posted: 3/26/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
You are evaluating a 40 year old trauma victim and see this on pelvic xray. What are you worried about?
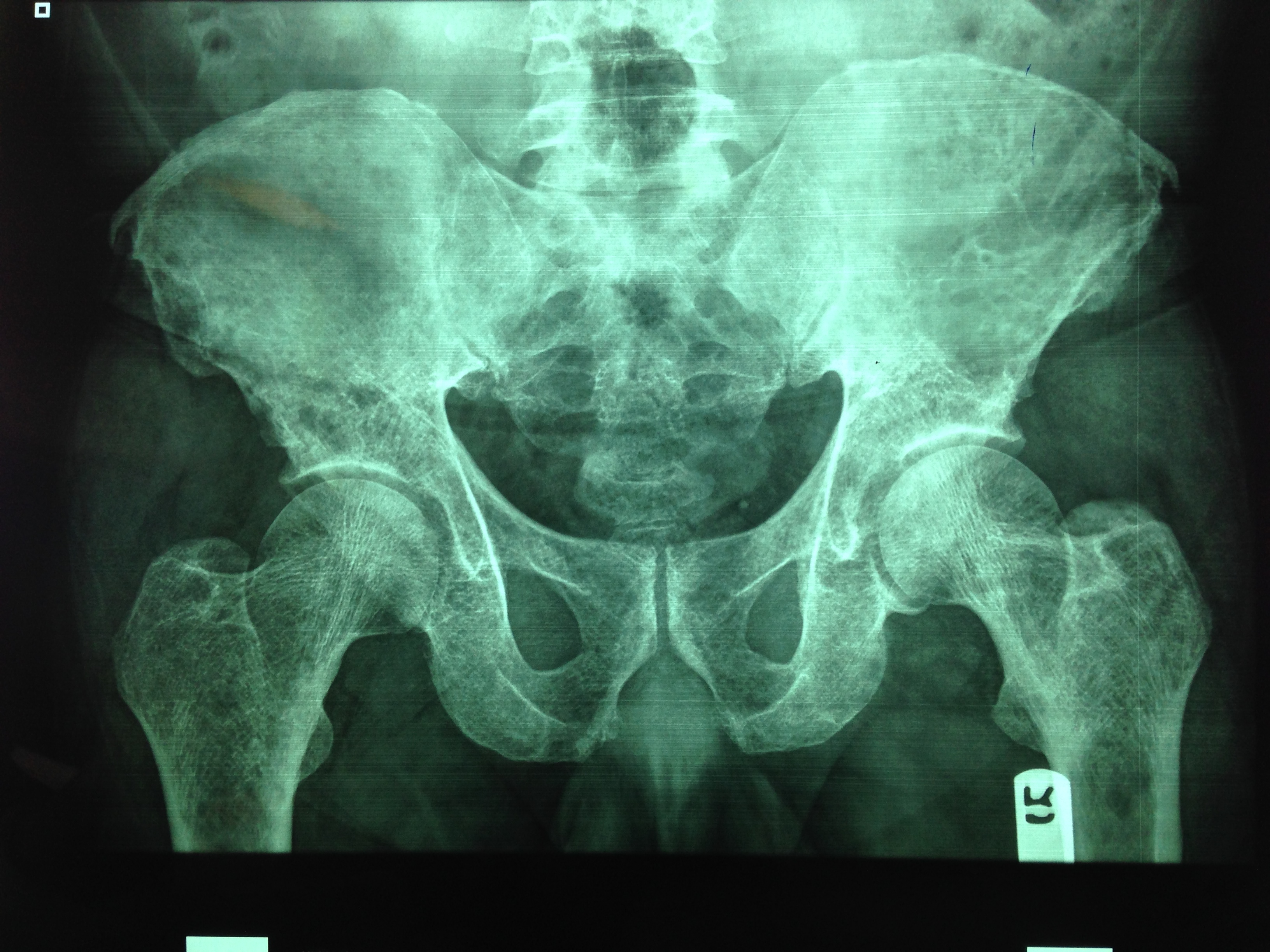
University of Maryland Section for Global Emergency Health
Authors: Colleen Holley, MD and Van Pham, MD
Mulligan, Michael. Multiple Myeloma Imaging. available: http://emedicine.
Category: International EM
Keywords: echocardiography, rheumatic heart disease, endocarditis, international (PubMed Search)
Posted: 3/19/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
35yo M with history of rheumatic heart disease presents with fever. What disease process is suggested by the echo?
Burke AP. Pathology of rheumatic heart disease. Medscape. 2013. Accessed 19 Mar 2013 at http://emedicine.medscape.com/article/1962779-overview#aw2aab6b4.
Category: Visual Diagnosis
Keywords: international, global, hypoxia, clubbing (PubMed Search)
Posted: 3/12/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
What is this physical finding?
Answer: Clubbing
Differential Diagnosis of Clubbing in Children:
Clubbing was first documented by Hippocrates in a patient with empyema. It has been associated with cardiopulmonary disease, but also found in other disease processes such as hepatobiliary, infectious, and endocrine diseases. It can also occur without an underlying pathology. The pathophysiology behind these physical findings remain unknown. The workup and treatment should be aimed at managing the underlying cause.
University of Maryland Section for Global Emergency Health
Author: Van Pham, MD
Schwartz, Robert. Clubbing of the Nails. 3.12.14. http://emedicine.
Category: International EM
Keywords: Vaccine, disaster, international, (PubMed Search)
Posted: 2/26/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Bottom Line:
University of Maryland Section of Global Emergency Health
Author: Veronica Pei
Use the CDC web module for travelers:
http://wwwnc.cdc.gov/travel/destinations/list
Category: International EM
Keywords: Cirrhosis, Hepatitis, International (PubMed Search)
Posted: 2/19/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
General Information:
Bottom Line:
Tenofovir has already become standard therapy for HIV (contained in Truvada and Atripla). This HBV study shows promise that this drug can not only decrease progression of disease but also reverse the cirrhosis associated with long-term infection. Given the prevalence of chronic HBV, larger scale role-out of this drug could markedly change the epidemiologic landscape of morbidity and mortality due to hepatitis B.
University of Maryland Section of Global Emergency Health
Author: Emilie J.B. Calvello
References: Marcellin P et al. Regression of cirrhosis during treatment with tenofovir disoproxil fumarate for chronic hepatitis B: A 5-year open-label follow-up study. Lancet 2012 Dec 10.
Category: International EM
Keywords: boarding, ACEP, america, american, global (PubMed Search)
Posted: 2/12/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Bottom line
ED crowding remains a critical problem in the US and globally. It is frequently driven by the “boarding” of admitted patients. Improved patient flow is needed to be able to take care of patients presenting with acute care needs.
University of Maryland Section of Global Emergency Health
Author: Jon Mark Hirshon, MD, MPH, PhD
www.emreportcard.org; America's Emergency Care Environment, A State-by-State Report Card: 2014 Edition. Report Card Task Force Members; ACEP Staff. Ann Emerg Med. 2014. Feb;63(2):100-243
Category: International EM
Keywords: road traffic accidents, international, global, public health (PubMed Search)
Posted: 2/5/2014 by Andrea Tenner, MD
(Updated: 4/14/2026)
Click here to contact Andrea Tenner, MD
General Information:
Area of the world affected:
Relevance to the US physician:
Bottom Line:
VRU traffic injuries are the greatest challenge of today's worldwide road safety.
University of Maryland Section of Global Emergency Health
Author: Terrence Mulligan DO, MPH
http://www.who.int/gho/road_safety/en/
http://www.plosmedicine.org/article/info%3Adoi%2F10.1371%2Fjournal.pmed.1000228
http://www.grsproadsafety.org/our-knowledge/safer-road-users/vulnerable-road-users
Category: International EM
Keywords: Virus, Fever, West Nile, Dengue (PubMed Search)
Posted: 1/29/2014 by Andrea Tenner, MD
Click here to contact Andrea Tenner, MD
Case Presentation: A 63 year old woman from Texas with no recent international travel presents to the ED with persistent fatigue which onset a month ago and is associated with anorexia and occasional fevers and chills. She has been to her family doctor who tested her for a number of viral illnesses and was told she had West Nile virus.
Clinical Question:
What other febrile illness could this be?
Answer:
This patient had dengue. Dengue is now endemic in the US, and locally-acquired cases have been reported in Florida, Texas and Hawaii. The fatigue and anorexia are typical and can last for weeks after other symptoms have resolved.
West Nile virus testing may be falsely positive when another flavivirus is present such dengue, yellow fever or Japanese encephalitis.
Bottom Line:
Other possible illnesses like dengue should be considered in patients who have tested positive for West Nile virus.
University of Maryland Section of Global Emergency Health
Author: Jenny Reifel Saltzberg, MD, MPH
Sharp TM, et al. Fatal hemophagocytic lymphohistiocytosis associated with locally acquired dengue virus infection - New Mexico and Texas, 2012. MMWR Morb Mortal Wkly Rep. 2014 Jan 24;63(3):49-54. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6303a1.htm?s_cid=mm6303a1_w
Centers for Disease Control and Prevention. Dengue and Dengue Hemorrhagic Fever: Information for Health Care Practitioners. http://www.cdc.gov/dengue/resources/Dengue&DHF%20Information%20for%20Health%20Care%20Practitioners_2009.pdf
