Category: Pediatrics
Posted: 2/10/2012 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Emergency Medicine Clinics of North America
Orothopedic Emergencies
November 2010, Volume 28, Number 4
Category: Pediatrics
Posted: 1/27/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Potential Causes of Neonatal Apnea and Bradycardia
• Central nervous system
Intraventricular hemorrhage, drugs maternal/fetal, seizures, hypoxic injury, herniation, neuromuscular disorders, brainstem infarction or anomalies (e.g., olivopontocerebellar atrophy), general anesthesia.
• Respiratory
Pneumonia, obstructive airway lesions, upper airway collapse, atelectasis, extreme prematurity (<1,000 g), phrenic nerve paralysis, severe hyaline membrane disease, pneumothorax, hypoxia, malformations of the chest.
• Infectious
Sepsis, meningitis (bacterial, fungal, viral), RSV
• Metabolic
Hypoglycemia, hyper/hyponatrmia, hyperammonemia, decreased organic acids, hypothermia.
• Cardiovascular
Hypotension/hypovolemia, heart failure, PDA, anemia, vagal tone.
Category: Pediatrics
Keywords: infectious disease, neonatal infections, umbilical disorders (PubMed Search)
Posted: 1/20/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: sedation, ketamine (PubMed Search)
Posted: 1/6/2012 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
There are limited direct comparisons of (intravenous (IV) vs. intramuscular (IM) ketamine for pediatric procedural sedation in the emergency department. The only RCT comparing IV and IM ketamine was by Roback et al. and compared an IV dose of 1mg/kg vs. IM 4mg/kg. The study authors reported less procedural pain with IM administration compared with IV. However, vomiting occurred more frequently in the IM group, 26.3% compared to 11.9% in the IV group and recovery time was 49 minutes shorter with IV vs IM use.
Route Onset Duration Dose
IM 3-5 min 20-30min 3-5 mg/kg
IV 1 min 5-10 min 1-2 mg/kg
Category: Pediatrics
Posted: 12/30/2011 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Pediatrics Board Review, MedStudy
Category: Pediatrics
Keywords: Bayonet, fracture reduction technique, radius (PubMed Search)
Posted: 12/16/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Pediatric forearm fractures:
Category: Pediatrics
Posted: 12/9/2011 by Rose Chasm, MD
Click here to contact Rose Chasm, MD
NMS Pediatrics
Category: Pediatrics
Keywords: child abuse, skeletal survey (PubMed Search)
Posted: 12/3/2011 by Vikramjit Gill, MD
Click here to contact Vikramjit Gill, MD
You just finished assessing a 6 month old in the Pediatric ED who can’t move his right leg. You suspect child abuse. You’re ready to order labs, a head CT, ophtho consult, skeletal survey and call Child Protective Services. While your doing all of this, your medical student asks you, “What exactly are you looking for on the skeletal survey?”
A skeletal survey is mandatory for cases of suspected child abuse in children under the age of 2 years. Approximately 60% of the fractures seen in abused children are younger than 18 months old.
When you are looking at a skeletal survey, carefully look for the following:
1. Multiple, healing fractures of various ages
2. Rib fractures, especially in the posterior ribs
3. Metaphyseal chip and buckle fractures
4. Spiral fractures in long bones (especially in children that can’t walk)
5. Skull fractures which are not simple and linear
6. Scapula fractures
More to come about child abuse….
References:
Category: Pediatrics
Keywords: Kawasaki, vasculitis, fever, (PubMed Search)
Posted: 11/25/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Classic Kawasaki is diagnosed by fever for greater than 5 days plus 4 out of 5 classic signs.
But what about an 8 month-old with 6 days of fever plus nonexudative conjunctivitis, unilateral cervical adenopathy and a diffuse maculopapular rash? Send some labs!
Incomplete Kawasaki is defined as fever for >5 days with 2 or more of the classic findings plus elevated ESR (>40mm/hr) and CRP (>3.0mg/dL). It is most common in infants under 12 months of age.
Disposition for the 8 month-old?
If the echo is normal, follow up in 24-48 hours and will need a repeat echo if fever persists.
TREAT kids with IVIG and aspirin (which generally means admission) if echo is positive, or with normal echo and the presence of 3 or more supplemental criteria:
Category: Pediatrics
Keywords: Passenger Safety (PubMed Search)
Posted: 11/18/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Child Passenger Safety.
Perhaps one of the greatest contributions emergency physicians can provide to society comes in the form of anticipatory guidance. It is important to take the opportunity during the ED encounter to provide information to parents to prevent future injuries. Child passenger safety is one clear example. With over 330,000 pediatric visits to EDs across the US annually attributed to motor vehicle collisions, the need to provide clear recommendations to parents on how to restrain their children in their vehicle is paramount. Despite a recent survey of over 1000 EPs in which 85% of respondents indicated child passenger safety should routinely be a part of pediatric MVC discharge instructions, only 36% of EPs knew the latest guidelines on child passenger safety. The American Academy of Pediatrics provides such guidelines. These recommendations were recently adjusted in 2011.
(1) Infants up to 2 years must be in REAR-facing car seats
(2) Children through 4 years in forward-facing car safety seats
(3) Belt-positioning booster seat for children through at least 8 years old
(4) Lap-and-shoulder seat belts for those who have outgrown booster seats. How does one know when the child has outgrown the booster seat?
a. Can the child sit with his/her knees bent at the edge of the seat?
b. Does the shoulder belt lie across the middle of the chest/shoulder?
c. Does the lap belt lie across the upper thighs and not the abdomen?
(5) Children younger than 13 should sit in the rear seats
Special Thanks to JV Nable, MD, EMT-P for writing this pearl.
1. Zonfrillo MR, Nelson KA, Durbin DR. Emergency physician's knowledge and provision of child passenger safety information. Acad Emerg Med 2011;18:145-151.
2. Durbin DR. Child passenger safety. Pediatrics 2011;127:788-793
Category: Pediatrics
Posted: 11/11/2011 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
MedStudy Pediatrics Board Review
Core Curriculum
Category: Pediatrics
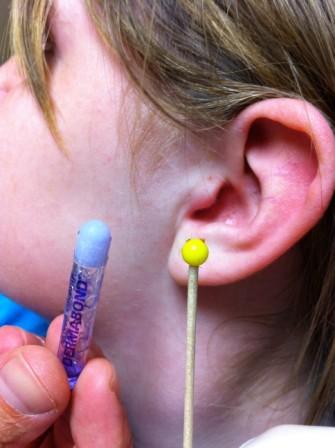
Keywords: dermabond, glue, foreign body, (PubMed Search)
Posted: 10/21/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 10/14/2011 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
Category: Pediatrics
Posted: 10/8/2011 by Vikramjit Gill, MD
(Updated: 5/13/2026)
Click here to contact Vikramjit Gill, MD
Peritoneal dialysis (PD) is a commonly used form of dialysis for pediatric patients with end-stage renal disease, particularly in children less than five years of age.
One well known complication to this mode of dialysis is PD-associated peritonitis.
Children may present with fever, abdominal pain and a cloudy dialysate.
If peritonitis is suspected, obtain sample of dialysate fluid and send for cell count, Gram’s stain and culture.
Cell count in PD-associated peritonitis is usually WBC >100 with >50% neutrophils.
Both gram-positive and gram-negative organisms are involved with PD-associated peritonitis . Keep both MRSA and Pseudomonas in mind.
In the ED, empiric therapy should cover both gram-positive and gram-negative organisms. Initiate antibiotic therapy with vancomycin and either a third-generation cephalosporin (ceftazidime) or aminoglycoside, respectively.
For PD-associated peritonitis, intraperitoneal (IP) administration of antibiotics is preferred over IV.
1. Li PK, et al. Peritoneal Dialysis-Related Infections Recommendations: 2010 Update. Peritoneal Dialysis International, Vol. 30, pp. 393–423.
2. Fadrowski JJ, et al. Children on long-term dialysis in the United States: findings from the 2005 ESRD clinical performance measures project. Am J Kidney Dis. 2007;50(6):958.
Category: Pediatrics
Keywords: Concussion, sports injury, TBI, return to play (PubMed Search)
Posted: 9/30/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
You are seeing a high school football player following a head injury. After your exam or head CT, you determine the child to have had a mild traumatic brain injury (aka concussion). You are ready to discharge him home when the parents or coach ask you when he can return to playing football.
A concussion is a form of functional, rather than structural, brain injury that displays no evidence of injury on structural neuroimaging. Symptoms include transient loss of consciousness, amnesia, vomiting, headache, poor school work, sleep changes, and emotional lability. Remember that children’s brains (even adolescents) are still developing, and are more prone to prolonged recovery following injury.
Recovery of symptoms usually follows a sequential course. Current guidelines recommend a stepwise return to play (aka concussion rehabilitation) involving both physical and cognitive rest (e.g. no texting, video games, limited school work). Once asymptomatic, the patient goes through each stage with at least 24 hours between stages. If symptoms return during a stage, then the patient is expected to return to the previous stage for 24 hours before attempting the higher stage again.
Return to Play Guidelines:
| Rehabilitation stage | Functional Exercise |
| Complete physical and cognitive rest |
| Walking, swimming, stationary cycling at 70% maximal heart rate, no resistance exercise |
| Specific sport related drills but no head impact |
| More complex drills, may start light resistance training |
| After medical clearance, participate in normal training |
| Normal game play |
References:
Category: Pediatrics
Keywords: ultrasound, intra-abdominal injury, free fluid, blunt trauma (PubMed Search)
Posted: 9/23/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Posted: 9/9/2011 by Rose Chasm, MD
(Updated: 5/13/2026)
Click here to contact Rose Chasm, MD
MedStudy Pedatrics Board Review, Core Curriculum, Book 3 2004
Category: Pediatrics
Keywords: severe asthma, decreased hospitalization (PubMed Search)
Posted: 8/26/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: weakness, constipation (PubMed Search)
Posted: 8/20/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Infantile botulism
Category: Pediatrics
Posted: 8/5/2011 by Vikramjit Gill, MD
(Updated: 5/13/2026)
Click here to contact Vikramjit Gill, MD
1) C-A-B for CPR. Now recommended to start compressions immediately instead of the conventional rescue breaths.
2) Capnography during CPR. Continuous capnography recommended during CPR to guide the resuscitation, especially the effectiveness of chest compressions.
a. If ETCo2 is less than 10 to 15 mm Hg consistently, focus your efforts on improving chest compressions.
3) Etomidate for RSI induction. Okay to use in infants and children, BUT not recommended for pediatric patients in septic shock. Etomidate was not addressed in 2005 guidelines.
4) Cuffed ET tubes. Acceptable to use in infants and children.
5) Limit FiO2 after resuscitation. Keep O2 sats ≥94%. Avoid hyperoxia.
6) Therapeutic hypothermia after cardiac arrest. Recommendation based off of adult data, no pediatric prospective RCT done on this. This is beneficial in adolescents with out-of-hospital VF arrest.
a. Consider therapeutic hypothermia for infants and children.
b. Cool to 32oC-34oC
1. Kleinman ME, Chameides L, Schexnayder SM, et al. Part 14: pediatric advanced life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122:S876 –S908.
