Category: Pediatrics
Keywords: Kawasaki, vasculitis, fever, (PubMed Search)
Posted: 11/25/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Classic Kawasaki is diagnosed by fever for greater than 5 days plus 4 out of 5 classic signs.
But what about an 8 month-old with 6 days of fever plus nonexudative conjunctivitis, unilateral cervical adenopathy and a diffuse maculopapular rash? Send some labs!
Incomplete Kawasaki is defined as fever for >5 days with 2 or more of the classic findings plus elevated ESR (>40mm/hr) and CRP (>3.0mg/dL). It is most common in infants under 12 months of age.
Disposition for the 8 month-old?
If the echo is normal, follow up in 24-48 hours and will need a repeat echo if fever persists.
TREAT kids with IVIG and aspirin (which generally means admission) if echo is positive, or with normal echo and the presence of 3 or more supplemental criteria:
Category: Pediatrics
Keywords: Passenger Safety (PubMed Search)
Posted: 11/18/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Child Passenger Safety.
Perhaps one of the greatest contributions emergency physicians can provide to society comes in the form of anticipatory guidance. It is important to take the opportunity during the ED encounter to provide information to parents to prevent future injuries. Child passenger safety is one clear example. With over 330,000 pediatric visits to EDs across the US annually attributed to motor vehicle collisions, the need to provide clear recommendations to parents on how to restrain their children in their vehicle is paramount. Despite a recent survey of over 1000 EPs in which 85% of respondents indicated child passenger safety should routinely be a part of pediatric MVC discharge instructions, only 36% of EPs knew the latest guidelines on child passenger safety. The American Academy of Pediatrics provides such guidelines. These recommendations were recently adjusted in 2011.
(1) Infants up to 2 years must be in REAR-facing car seats
(2) Children through 4 years in forward-facing car safety seats
(3) Belt-positioning booster seat for children through at least 8 years old
(4) Lap-and-shoulder seat belts for those who have outgrown booster seats. How does one know when the child has outgrown the booster seat?
a. Can the child sit with his/her knees bent at the edge of the seat?
b. Does the shoulder belt lie across the middle of the chest/shoulder?
c. Does the lap belt lie across the upper thighs and not the abdomen?
(5) Children younger than 13 should sit in the rear seats
Special Thanks to JV Nable, MD, EMT-P for writing this pearl.
1. Zonfrillo MR, Nelson KA, Durbin DR. Emergency physician's knowledge and provision of child passenger safety information. Acad Emerg Med 2011;18:145-151.
2. Durbin DR. Child passenger safety. Pediatrics 2011;127:788-793
Category: Pediatrics
Keywords: dermabond, glue, foreign body, (PubMed Search)
Posted: 10/21/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
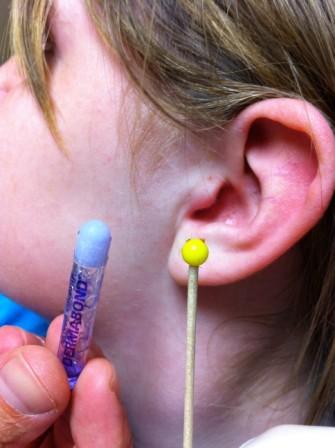
Category: Pediatrics
Keywords: Concussion, sports injury, TBI, return to play (PubMed Search)
Posted: 9/30/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
You are seeing a high school football player following a head injury. After your exam or head CT, you determine the child to have had a mild traumatic brain injury (aka concussion). You are ready to discharge him home when the parents or coach ask you when he can return to playing football.
A concussion is a form of functional, rather than structural, brain injury that displays no evidence of injury on structural neuroimaging. Symptoms include transient loss of consciousness, amnesia, vomiting, headache, poor school work, sleep changes, and emotional lability. Remember that children’s brains (even adolescents) are still developing, and are more prone to prolonged recovery following injury.
Recovery of symptoms usually follows a sequential course. Current guidelines recommend a stepwise return to play (aka concussion rehabilitation) involving both physical and cognitive rest (e.g. no texting, video games, limited school work). Once asymptomatic, the patient goes through each stage with at least 24 hours between stages. If symptoms return during a stage, then the patient is expected to return to the previous stage for 24 hours before attempting the higher stage again.
Return to Play Guidelines:
| Rehabilitation stage | Functional Exercise |
| Complete physical and cognitive rest |
| Walking, swimming, stationary cycling at 70% maximal heart rate, no resistance exercise |
| Specific sport related drills but no head impact |
| More complex drills, may start light resistance training |
| After medical clearance, participate in normal training |
| Normal game play |
References:
Category: Pediatrics
Keywords: ultrasound, intra-abdominal injury, free fluid, blunt trauma (PubMed Search)
Posted: 9/23/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: severe asthma, decreased hospitalization (PubMed Search)
Posted: 8/26/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Category: Pediatrics
Keywords: weakness, constipation (PubMed Search)
Posted: 8/20/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Infantile botulism
Category: Pediatrics
Posted: 7/29/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
Acute Poststreptococcal Glomerulonephritis (APSGN) is a sequela of group A beta-hemolytic streptococci (GAS) infection of the skin or pharynx with nephrogenic strains of GAS. Damage to the kidneys is due to deposition of antigen-antibody complexes in the glomeruli.
Presentation:
Testing:
Treatment:
Prognosis (favorable):
Reference:
Kit, Brian. Assess the volume status and electrolytes in children with poststreptococcal glomerulonephritis. Avoiding Common Pediatric Errors. 2008. p356-57.
Category: Pediatrics
Posted: 7/22/2011 by Mimi Lu, MD
Click here to contact Mimi Lu, MD
You're called to bedside to evaluate a "lethargic" infant. You wisely ask for a POCT glucose which returns at 35. How much dextrose do you give (since you know it's not just "an amp" of D50?
Here's a simple mnemonic:
Rule of 50-100 = multiply type of dextrose solution by ____ factor (ml/kg) to total 50-100
D10 (neonate) x 5-10 ml/kg = 50-100
D25 (infant) x 2-4 ml/kg = 50-100
D50 (child/adolescent) x 1-2 ml/kg = 50-100
Category: Pediatrics
Keywords: Enterovirus, infant, CSF (PubMed Search)
Posted: 7/15/2011 by Mimi Lu, MD
(Updated: 7/22/2011)
Click here to contact Mimi Lu, MD
Now that summer is in full swing, the question is: Should the evaluation of the febrile young infant change during the summer and fall months? And can that affect length of hospitalization and antibiotic use?
Two retrospective cohort studies from the Children’s Hospital of Philadelphia (CHOP) suggest yes! The addition of enterovirus polymerase chain reaction (PCR) testing to cerebrospinal fluid (CSF) may improve the care of infants with fever during enterovirus season (early June through late October).
Of note, at CHOP: 1) infants 56 days or younger routinely undergo lumbar puncture during evaluation for fever. 2) Most CSF enterovirus PCR test results (90%) were available within 36 hours; 95% of results were available within 48 hours.
In the King study, having positive enterovirus PCR CSF results decreased the length of hospitalization and the duration of antibiotic use for young infants less than 90 days, supporting the routine use of this test during periods of peak enterovirus season. In multivariate
analysis, a positive CSF enterovirus PCR result was associated with a 1.54-day decrease in the length of stay and a 33.7% shorter duration of antibiotic use.
Bottom line: Consider adding enterovirus PCR testing to CSF obtained during the evaluation of febrile young infants during enterovirus season, as this may reduce length of hospitalization and duration of antibiotic use. The effects, however, may be limited at institutions with slower lab turnaround times.
References:
1) King RL, Lorch SA, Cohen DM, Hodinka RL, Cohn KA, Shah SS. Routine cerebrospinal fluid enterovirus polymerase chain reaction testing reduces hospitalization and antibiotic use for infants 90 days or younger. Pediatrics. 2007 Sep;120(3):489-96. http://pediatrics.aappublications.org/content/120/3/489.full.pdf
2) Dewan M, Zorc JJ, Hodinka RL, Shah SS. Cerebrospinal fluid enterovirus testing in infants 56 days or younger. Arch Pediatr Adolesc Med. 2010 Sep;164(9):824-30.
Category: Pediatrics
Posted: 4/22/2011 by Mimi Lu, MD
(Updated: 5/6/2011)
Click here to contact Mimi Lu, MD
Continuing the theme of endotracheal tube size pearls... You get a box call for a pre-term baby delivered precipitously by mom at home and baby is blue. EMS is bagging but unable to secure a definitive airway. What size ETT do you reach for? If you try to apply the formula "uncuffed ETT = (age/4) + 4", how much smaller than size 4 can you go?
Category: Pediatrics
Posted: 4/22/2011 by Mimi Lu, MD
(Updated: 4/30/2011)
Click here to contact Mimi Lu, MD
You decided to intubate a child and wisely remembered that you should also follow with an NG/ OG after intubation to decompress the stomach. In order to avoid the blank stare when asked "what size"? Here's a nice mneumonic about Pediatric "tube" sizes... easy as 1-2-3-4!!! Please note ETT = endotracheal tube size.
So for example, a 4-year-old child would get intubated with a 5-0 ETT inserted to depth of 15 cm (3x ETT), a 10Fr NG/OG/foley (2x ETT), and a 20Fr chest tube (4x ETT).
Also, remember that you can use cuffed tubes in any child except neonates but the formula needs to be adjusted as follows: cuffed endotracheal tube ID (mm) = (age/4) + 3.5
Category: Pediatrics
Keywords: Influenza (PubMed Search)
Posted: 3/2/2011 by Mimi Lu, MD
(Updated: 3/5/2011)
Click here to contact Mimi Lu, MD
Now that influenza season is in full swing, remember that early antiviral treatment can reduce the risk of complications in high-risk individuals. One of those high-risk groups is children <2 years, with the highest hospitalizations and mortality in infants <6 months.
According to the CDC website:
Recommended antiviral medications (neuraminidase inhibitors) are not FDA-approved for treatment of children aged <1 year (oseltamivir) or those aged <7 years (zanamivir). Oseltamivir was used for treatment of 2009 pandemic influenza A (H1N1) virus infection in children aged <1 year under an Emergency Use Authorization, which expired on June 23, 2010. Nevertheless,
Current CDC guidance on treatment of influenza should be consulted; updated recommendations from CDC are available at http://www.cdc.gov/flu
.
